Plaster of paris in orthopedics procedure and types
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Searching Images
plaster of paris cast orthopedic application types
I now have comprehensive information to write a thorough answer. Let me compile it.
Plaster of Paris (POP) in Orthopedics
What Is Plaster of Paris?
Plaster of Paris gets its name from the gypsum deposits of Paris, France, where it was first prepared. When gypsum (calcium sulfate dihydrate) is heated to approximately 128°C, most of the water of crystallization is driven off, leaving a fine white powder — plaster of Paris. When water is re-added, the reaction reverses: the plaster recrystallizes by incorporating water molecules back into the calcium sulfate dihydrate crystalline lattice, causing it to "set" and harden. This exothermic setting reaction is why warm water must be avoided during application — water hotter than 24°C (75°F) can cause thermal injury to the patient.
Today, plaster is impregnated into rolls or strips of a crinoline-type material (fabric mesh) that allows easy application, maintains mold during setting, and adds structural support to the finished splint or cast.
— Roberts and Hedges' Clinical Procedures in Emergency Medicine, p. 1180
Historical Context
- Fracture immobilization dates to 2498–2345 BCE in Egypt (bark splints for forearm fractures).
- Gypsum was used in the 16th century Ottoman Empire for immobilization.
- In 1927, hard-coated plaster of Paris rolls were developed with a binder to improve plaster-to-cloth adherence.
- Salicylic acid, zinc, or aluminum can accelerate setting; gums or glue can slow it.
- Gradually, plaster replaced splintage as the standard method, with Hugh Owen Thomas and Lorenz Böhler of Vienna being notable early proponents.
— Pfenninger and Fowler's Procedures for Primary Care, p. 1285
Indications for POP Immobilization
| Indication | Examples |
|---|---|
| Fractures | Stable/undisplaced fractures of radius, ulna, phalanges, metacarpals, metatarsals, malleoli |
| Reduced dislocations | Shoulder, elbow, ankle |
| Soft tissue injuries | Tendon lacerations, severe ligament sprains (grade III) |
| Inflammatory conditions | Acute gout, tenosynovitis, refractory tendonitis |
| Infections | Deep space hand/foot infections, cellulitis over joints |
| Wounds | Lacerations crossing joints, deep abrasions over joints |
| Post-surgical protection | After vascular, nerve, or tendon repair |
| Congenital deformities | Clubfoot correction (Ponseti method), talipes equinovarus |
| Multiple trauma | Temporary stabilization while other procedures are completed |
— Roberts and Hedges' Clinical Procedures in Emergency Medicine, p. 1308–1310
POP vs. Fiberglass: Comparison
| Feature | Plaster of Paris | Fiberglass |
|---|---|---|
| Cost | Inexpensive | More expensive (gap narrowing) |
| Weight | Heavier | ~2–3× lighter |
| Strength | Standard | ~2–3× stronger for same thickness |
| Moldability | Excellent (preferred for complex molding) | More difficult to mold |
| Radiolucency | Less radiolucent | More radiolucent |
| Setting time | Slower (~24–72 hrs full strength) | ~3 minutes to set, 20 min to cure |
| Heat generation | More exothermic | Less heat during application |
| Waterproofing | Not waterproof | Can be paired with Gore-Tex liner for waterproofing |
— Pfenninger and Fowler's Procedures for Primary Care, p. 1286; Rockwood & Green's Fractures in Adults, p. 321
Types of POP Casts and Splints
By Completeness
1. Circumferential (Full) Cast
A continuous cast wrapping completely around the limb. Applied using plaster or fiberglass bandages wrapped over stockinette and wool padding. Provides maximum rigidity. Contraindicated acutely when significant swelling is anticipated (risk of compartment syndrome).
2. Slab (Back Slab / Posterior Splint)
A non-circumferential slab applied on one surface (usually posterior) and held in place with a bandage. Preferred when swelling is anticipated, as it allows expansion. Used as a temporary measure before conversion to a full cast.
— Rockwood & Green's Fractures in Adults, p. 329 (Fig. 10-10: forearm back slab for undisplaced distal radial fracture)
By Anatomical Region & Design
Upper Limb Splints
| Splint Type | Construction | Position | Indications |
|---|---|---|---|
| Long Arm Posterior Splint | 8–10 layers of 4–6 inch plaster; posterior arm → ulnar forearm → MCP joints | Elbow 90°, forearm neutral, wrist neutral/10–20° extension | Elbow and forearm injuries |
| Long Arm Anterior Splint | Mirrors posterior splint along anterior arm and radial forearm | Same as above | Used only as adjunct to posterior splint; prevents pronation/supination |
| Double Sugar-Tong Splint | Two plaster pieces: forearm runs dorsum of hand → around elbow → volar forearm; arm portion wraps around shoulder | Elbow 90°, forearm neutral | Distal forearm/elbow fractures; prevents pronation/supination |
| Volar Wrist Splint | 8–10 layers; runs from palmar hand crease to mid-forearm | Wrist slightly extended | Wrist sprains, carpal fractures (non-scaphoid), carpal tunnel |
| Ulnar Gutter Splint | Along ulnar aspect of forearm from DIP of little finger to mid-forearm | Wrist 10–20° extension, MCP 50° flexion, IP joints slight flexion (90° MCP for metacarpal neck fractures) | 4th/5th metacarpal fractures, ring/little finger injuries |
| Radial Gutter Splint | Along radial aspect | Similar position | 2nd/3rd metacarpal fractures, index/middle finger injuries |
| Thumb Spica | Incorporates thumb | Wrist extended, thumb in "beer can grip" position | Scaphoid fractures, De Quervain's, thumb UCL injuries |
Lower Limb Casts
| Cast Type | Extent | Indications |
|---|---|---|
| Short Leg Cast | Foot to just below knee | Ankle fractures, foot fractures, stable tibial injuries |
| Long Leg Cast | Foot to mid-thigh | Patellar fractures, tibial plateau fractures, tibial/fibular shaft fractures, knee ligament avulsions |
| Walking Cast | Short leg with rubber heel incorporated | Stable fractures requiring mobilization |
| Cylinder Cast | Knee to ankle, no foot | Patellar injuries, knee ligament injuries |
— Pfenninger and Fowler's, p. 1287 (Fig. 187-7); Roberts and Hedges', p. 1189–1195
Long Arm Cast with Thumb Spica
Used for navicular (scaphoid) fractures, complicated Colles' fractures, and nondisplaced radius/ulnar shaft fractures.
Application Procedure (Step-by-Step)
Based on the standard protocol from Rockwood & Green's Fractures in Adults (Table 10-4):
- Reduce the fracture (if displaced)
- Assistant holds the fracture in the reduced position
- Measure and apply stockinette (~10 cm beyond cast ends)
- Apply wool/Webril padding distal to proximal, 50% overlap; extra padding over bony prominences
- Submerge plaster in cool water (≤24°C) until bubbling stops; squeeze out excess
- If swelling anticipated → use slab; if minimal swelling → full cast
- Apply plaster/fiberglass, smoothing with palms (not fingertips — to avoid pressure point indentations)
- Hold fracture in reduced position until cast hardens
- Fold stockinette and wool padding back; apply second cast bandage to secure edges
- Ensure adequate proximal and distal joint mobility
- Obtain radiographs to confirm acceptable fracture position
- If swelling occurs post-application → bivalve or split the cast
Layers recommended:
- Upper extremity: 8 layers
- Lower extremity: 12–15 layers
Key Application Tips
- Use cool water only — warm water accelerates setting and increases thermal injury risk
- Mold with palms, not fingers — finger indentations become pressure points
- Avoid tight wrapping with elastic bandages
- Leave fingertips/toes exposed to monitor circulation and sensation
- Post-application check: FACTS — Function, Arterial pulse, Capillary refill, Temperature, Sensation
- Instruct patient on elevation and not to insert objects or get cast wet
Complications of POP Casts
| Complication | Mechanism |
|---|---|
| Compartment syndrome | Circumferential cast prevents expansion as swelling increases → ↑ intracompartmental pressure |
| Pressure sores / ulcers | Inadequate padding, finger-tip indentations, wrinkled padding |
| Plaster blisters | Skin reaction under cast |
| Peripheral nerve injury | Pressure on superficial nerves |
| Muscle wasting | Disuse under prolonged immobilization |
| Thermal burns | Hot water used to activate plaster; exothermic reaction |
| Contact/allergic dermatitis | Reaction to benzalkonium chloride or resin in cast material |
| Joint stiffness | Unnecessary inclusion of joints; prolonged immobilization |
| Fat embolism | From improperly immobilized long bone fractures |
| Secondary fracture displacement | Excessive padding permitting movement in unstable fractures |
— Rockwood & Green's Fractures in Adults, p. 329–330
Clinical Images
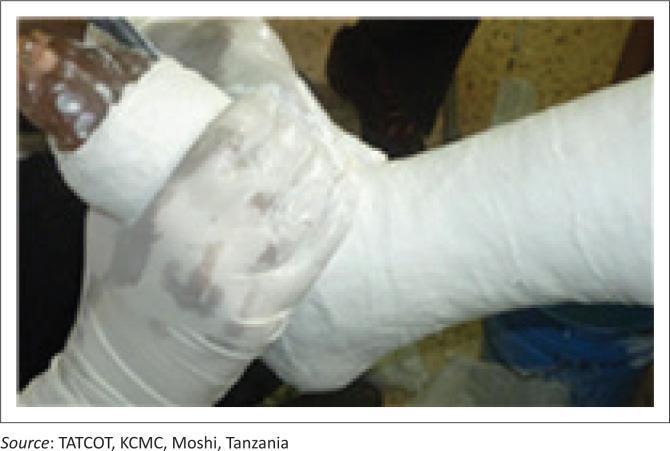

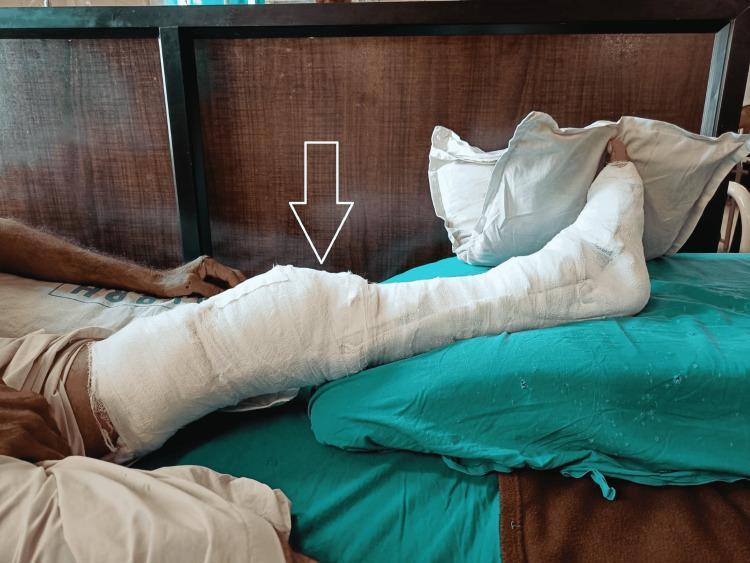
Sources:
- Roberts and Hedges' Clinical Procedures in Emergency Medicine, Chapter 50 (Splinting)
- Rockwood and Green's Fractures in Adults, 10th ed. 2025, Chapter 10 (Nonoperative Management)
- Pfenninger and Fowler's Procedures for Primary Care, Chapter 187 (Cast Immobilization)
- Gray's Anatomy for Students — Bone Fractures section
This is a shared conversation. Sign in to Orris to start your own chat.