18 y old female with pain and rashes as shown on multiple sites 18-year-old female with pain and scratches or rashes on multiple sites, as seen in neck, abdomen, chest, and lower thighs of right leg. No history of itching present. No history of fever.
Reading File
Finding Sources
Finding Sources
Searching the Web
cutaneous larva migrans serpiginous track multiple sites treatment 2024
Reading File
Reading File
Searching Images
cutaneous larva migrans serpiginous track creeping eruption leg
Loading Image
Clinical Assessment
Most Likely Diagnosis: Cutaneous Larva Migrans (CLM) — "Creeping Eruption"
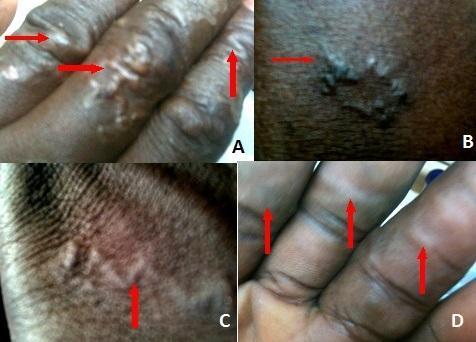
Image Findings
The photographs show the pathognomonic features of CLM:
- Right thigh/leg: A raised, serpiginous (serpentine/winding), erythematous track with white thread-like raised edges — this is the classic creeping eruption representing the migratory path of hookworm larvae within the epidermis
- Chest/upper chest area: Linear erythematous scratch-like marks consistent with additional larval tracks
- Multiple-site involvement suggests the patient may have had prolonged contact with contaminated soil/sand (e.g., lying on ground)
For comparison, the reference image below shows the same morphology:
Key Clinical Features (Confirmed by Textbooks)
| Feature | This Patient |
|---|---|
| Serpiginous/linear raised track | ✅ Present (thigh, chest) |
| Erythema at lesion site | ✅ Present |
| Multiple body sites | ✅ Neck, abdomen, chest, thigh |
| No fever | ✅ Consistent (CLM is localized, no systemic involvement) |
| No itching | ⚠️ Atypical — CLM classically causes intense pruritus (see note below) |
Note on absent itching: CLM typically causes intense pruritus. The absence of itching in this patient is atypical but does not exclude the diagnosis — early presentations, individual variation, or recent topical application could explain this. The morphology is otherwise classic. Gnathostomiasis (another migratory larval infection) should also be considered as it often causes less pruritus and deeper tracks.
Causative Organism
Animal hookworm larvae — most commonly:
- Ancylostoma braziliense (dog/cat hookworm) — most frequent
- Ancylostoma caninum
Transmission: Skin contact with soil or sand contaminated by dog/cat feces — walking barefoot, sitting or lying on contaminated ground. Ask about recent outdoor exposure, sandy areas, animal contact, or rural/beach environments.
Differential Diagnosis
| Condition | Features that differ |
|---|---|
| Gnathostomiasis | Deeper, faster-moving tracks (1 cm/hour vs 1-2 cm/day); trunk/upper body more common; less pruritus — consider this given absent itching |
| Tinea corporis | Ring-shaped, not serpiginous; fungal in origin |
| Contact dermatitis | No track formation; associated with allergen exposure |
| Scabies | Burrows in web spaces, more diffuse; intense itch |
| Self-inflicted excoriations | Important to consider given the pattern — however, the serpiginous raised track is too characteristic to be excoriation |
Management
First-line treatment — both are effective:
| Drug | Dose | Duration | Cure Rate |
|---|---|---|---|
| Ivermectin (preferred) | 200 µg/kg single oral dose | Single dose | 81–100% |
| Albendazole | 400 mg orally once daily | 3–7 days | 46–100% |
- Ivermectin single-dose is preferred for its high efficacy and low relapse rate
- For multiple lesions or widespread involvement as in this patient, albendazole for 5–7 days may be more reliable
- Apply topical antiseptic to prevent secondary bacterial infection of excoriated tracks
- Do NOT perform skin biopsy — larvae are rarely found histologically and biopsy provokes further inflammation
Work-Up
- Diagnosis is clinical — no labs required in typical presentations
- If atypical: stool examination for hookworm eggs/larvae
- Eosinophil count (CBC) — mild eosinophilia may be present
- If deep/rapidly migrating lesion: consider serology for Gnathostoma
Epidemiological Enquiry
Ask about:
- Walking barefoot on soil, sand, or grass recently
- Contact with dogs/cats or their feces
- History of travel to tropical/subtropical regions
- Outdoor activities (gardening, farming, playing on ground)
Sources: Dermatology 2-Volume Set 5e; Harrison's Principles of Internal Medicine 22E, p. 1856; BMJ Best Practice — Cutaneous Larva Migrans
Is it not herpes?
Finding Sources
Finding Sources
Searching the Web
herpes zoster vs cutaneous larva migrans serpiginous track differentiation
Finding Sources
Reading Web Page
CLM mimicking herpes zoster differences diagnosis
Herpes vs. Cutaneous Larva Migrans — Direct Comparison
This is a well-documented diagnostic pitfall — extensive CLM has been reported in literature to mimic herpes zoster, and patients are sometimes misdiagnosed and treated with aciclovir (ineffectively). Let's go through each distinguishing point:
Feature-by-Feature Comparison
| Feature | Herpes Zoster | Cutaneous Larva Migrans (this patient) |
|---|---|---|
| Lesion morphology | Grouped vesicles/pustules on an erythematous base, becoming crusted | Raised, winding/serpiginous thread-like track — the hallmark |
| Distribution | Strictly dermatomal (follows one nerve root, usually unilateral) | Random, following larval migration path — not dermatomal |
| Sides affected | Almost always unilateral — does not cross midline | Can affect multiple sites on any part of the body |
| Track shape | Clusters of vesicles in a band/strip | Serpiginous, snake-like, advancing track |
| Progression | Vesicles appear in crops, then crust; does not actively "move" | Track advances 1–2 cm per day — actively migrating |
| Pain | Prodromal burning/neuralgic pain before rash appears | Local discomfort/pain at lesion — no prodromal neuralgia |
| Itching | Burning/pain more than itch | Classic intense itch (though absent here) |
| Fever | Often present, especially in immunocompromised | Absent ✅ (consistent with CLM) |
| Age | More common in elderly/immunocompromised; unusual in healthy 18-yr-old | Common in young, healthy individuals with outdoor exposure |
| Vesicle content | Clear then turbid/pustular fluid — discrete grouped vesicles | Thread-like raised whitish track (seen in thigh image), not grouped vesicles |
Why This is NOT Herpes
Looking at the images directly:
-
The thigh lesion shows a single serpiginous, winding, raised white track — this is not how herpes looks. Herpes produces clustered vesicles (like a bunch of bubbles) on red skin, not a continuous crawling thread.
-
The distribution is not dermatomal — neck, abdomen, chest, and thigh simultaneously suggests multiple contact points with contaminated ground, not a single nerve root activation.
-
No grouped vesicles or pustules visible in any of the images.
-
No fever — herpes zoster in a young immunocompetent person typically causes prodromal symptoms.
-
18 years old, healthy — herpes zoster (shingles) is rare in young healthy individuals. Herpes simplex would be clustered in one site (lips, genitals), not dispersed like this.
The Published Precedent
A published case report describes a 42-year-old with extensive CLM at multiple sites who was incorrectly treated with aciclovir (herpes medication) without improvement. He was subsequently cured by a single dose of ivermectin 12 mg. This underscores why correct diagnosis matters here.
Bottom Line
The morphology — specifically the serpiginous, thread-like advancing track on the thigh — is not consistent with herpes by any standard. Herpes does not produce a crawling linear thread; it produces clustered fluid-filled blisters. The clinical picture here is classic for Cutaneous Larva Migrans.
Treat with: Ivermectin 200 µg/kg single oral dose, or Albendazole 400 mg once daily × 5–7 days (preferred given multiple sites).
This is a shared conversation. Sign in to Orris to start your own chat.