One health concept in community medicine
Reading File
Finding Sources
Searching PubMed
"One Health" community medicine
Finding Sources
Searching the Web
One Health concept community medicine definition pillars zoonosis
Finding Sources
Reading Web Page
One Health concept definition pillars community medicine history
Finding Sources
Reading Web Page
One Health pillars applications examples community medicine public health
Reading File
Reading File
Here is a comprehensive overview of the One Health Concept as it applies to community medicine:
One Health Concept in Community Medicine
Definition
One Health is a global collaborative, multisectoral, and transdisciplinary approach that recognizes the interconnection between people, animals, plants, and their shared environment. It aims to balance and optimize the health of humans, animals, and ecosystems by integrating these fields rather than keeping them separate.
"One Health is a global collaborative, multisectoral, and transdisciplinary approach to disease that recognizes the interconnection between people, animals, plants, and their shared environment." — Fishman's Pulmonary Diseases and Disorders
The WHO and CDC jointly define it as: an approach that integrates multiple sectors, disciplines, and communities to achieve optimal health outcomes across humans, animals, plants, and the environment.
Historical Background
| Period | Development |
|---|---|
| Mid-20th century | Calvin Schwabe (US veterinary surgeon) proposed "One Medicine" — comparing human and animal health to advocate cross-disciplinary work |
| Early 21st century | Concept expanded to encompass wider ecosystem health (wild animals, plants, geography) |
| 2004 | Manhattan Principles of Conservation called for integrated view of human–animal interactions; term "One Health" first coined |
| 2002–2004 | SARS-CoV-1 global outbreak sharply highlighted zoonotic risks — accelerated One Health adoption |
| 2020–present | COVID-19 pandemic and climate change effects renewed urgency; UN Sustainable Development Goals incorporated One Health targets |
| 2022 | Dedicated journal "Science in One Health" established |
The Three Pillars (Interconnected Spheres)
HUMAN HEALTH
↕
ANIMAL HEALTH
↕
ENVIRONMENTAL HEALTH
A newer relational model nests these: human health ⊂ animal health ⊂ ecosystem health, all sharing common social, cultural, economic, biophysical, political, and historical dimensions.
Governing Bodies — The One Health Quadripartite
Four international organizations lead global One Health strategy:
- WHO (World Health Organization) — human health dimensions
- WOAH/OIE (World Organisation for Animal Health) — animal health
- FAO (UN Food and Agriculture Organization) — food systems & agriculture
- UNEP (UN Environment Programme) — environmental dimensions (newest member)
Six Focus Areas (WHO/Quadripartite Framework)
| Focus Area | Key Issues |
|---|---|
| 1. Laboratory Services | Diagnostic protocols for humans, animals, and environment; Point-of-Care Tests |
| 2. Zoonotic Disease Control | Diseases transmissible between animals and humans (rabies, Ebola, avian influenza, leptospirosis) |
| 3. Neglected Tropical Diseases (NTDs) | Often have animal reservoirs; require integrated control |
| 4. Antimicrobial Resistance (AMR) | Antibiotic use in agriculture amplifies resistance; One Health approach monitors all reservoirs |
| 5. Food Safety | Foodborne pathogens (Salmonella, Listeria, norovirus) at every stage of production |
| 6. Environmental Health | Climate change, ecosystem degradation, pollution, land use |
Why It Matters — Key Statistics
- ~60% of emerging infectious diseases globally originate from animals (wild or domestic)
- Over 30 new human pathogens detected in the last 3 decades — 75% originated in animals
- Factors driving emergence: deforestation, climate change, global travel/trade, ecotourism, intensive agriculture, urbanization
Applications in Community Medicine
1. Zoonosis Prevention & Control
Direct animal-to-human transmission (rabies, brucellosis, anthrax, Q fever), vector-borne (malaria, dengue, Lyme disease), and environmental routes (leptospirosis from contaminated water). Community medicine applies One Health by coordinating human surveillance with veterinary and environmental monitoring.
2. Antimicrobial Resistance (AMR)
AMR reservoirs exist in agriculture, food production, and domestic animals. Antibiotic use in livestock amplifies resistance genes which transfer to humans. A One Health approach addresses:
- Antimicrobial stewardship in hospitals and outpatient settings
- Regulation of antibiotic use in food animals
- Environmental surveillance of resistance genes
(Harrison's Principles of Internal Medicine, 22E, 2025)
3. Pandemic Preparedness
COVID-19, SARS, MERS, influenza H5N1 — all have animal origins. One Health frameworks enable early-warning surveillance at the human-animal-environment interface.
4. Food Safety
Community-level foodborne disease investigations link contamination at the farm level (e.g., Campylobacter on poultry farms) to human illness clusters — a classic One Health investigation.
5. Environmental Health
Land use changes → altered vector habitats → changes in malaria, dengue distribution. Climate change affects both invertebrate vectors and vertebrate hosts differently, requiring ecological modeling alongside clinical surveillance.
One Health vs. Traditional Approaches
| Feature | Traditional (Siloed) | One Health |
|---|---|---|
| Focus | Human OR animal OR environment | All three simultaneously |
| Disciplines | Medicine, veterinary, ecology separately | Integrated, transdisciplinary |
| Response | Sector-specific | Cross-sectoral coordination |
| Surveillance | Separate systems | Shared data and governance |
Relevance to Public Health Practice
One Health operates at every level:
- Community level: local zoonosis surveillance, food safety inspections, vector control
- National level: integrated disease reporting systems, agricultural policy
- Global level: WHO/FAO/WOAH joint outbreak investigations, pandemic preparedness frameworks
Key message: "Collaboration across sectors achieves together what no sector can achieve alone." — WHO
Summary
The One Health concept is central to 21st-century community medicine because:
- Most emerging infections are zoonotic in origin
- AMR is a cross-species, cross-environment problem
- Climate and ecological change continuously reshape disease geography
- Effective prevention requires breaking down silos between human medicine, veterinary science, and environmental science
The framework is not a discipline itself, but a way of working — collaborative, multisectoral, and transdisciplinary — already embedded in public health activities like vector surveillance, outbreak investigation, and environmental monitoring.
One health approach in leptospirosis
Finding Sources
Finding Sources
Searching PubMed
"leptospirosis" AND "One Health"
Finding Sources
Reading File
Reading File
Finding Sources
Searching the Web
One Health approach leptospirosis control prevention human animal environment surveillance
Reading File
Reading Web Page
One Health leptospirosis human animal environment prevention control surveillance
Reading File
Loading Image
Here is a comprehensive account of the One Health Approach in Leptospirosis:
One Health Approach in Leptospirosis
Why Leptospirosis is a Model One Health Disease
Leptospirosis is widely described as the world's most widespread zoonosis — the perfect case study for the One Health framework because it sits precisely at the intersection of human health, animal health, and the environment. No single sector can address it alone.
"Leptospirosis is a clear example of why we need collaboration between clinicians, veterinarians, environmental authorities and communities. Only a truly integrated approach can reduce the risk of outbreaks." — Dr Jane Sykes, WSAVA / WOAH (2025)
The Pathogen — Quick Background
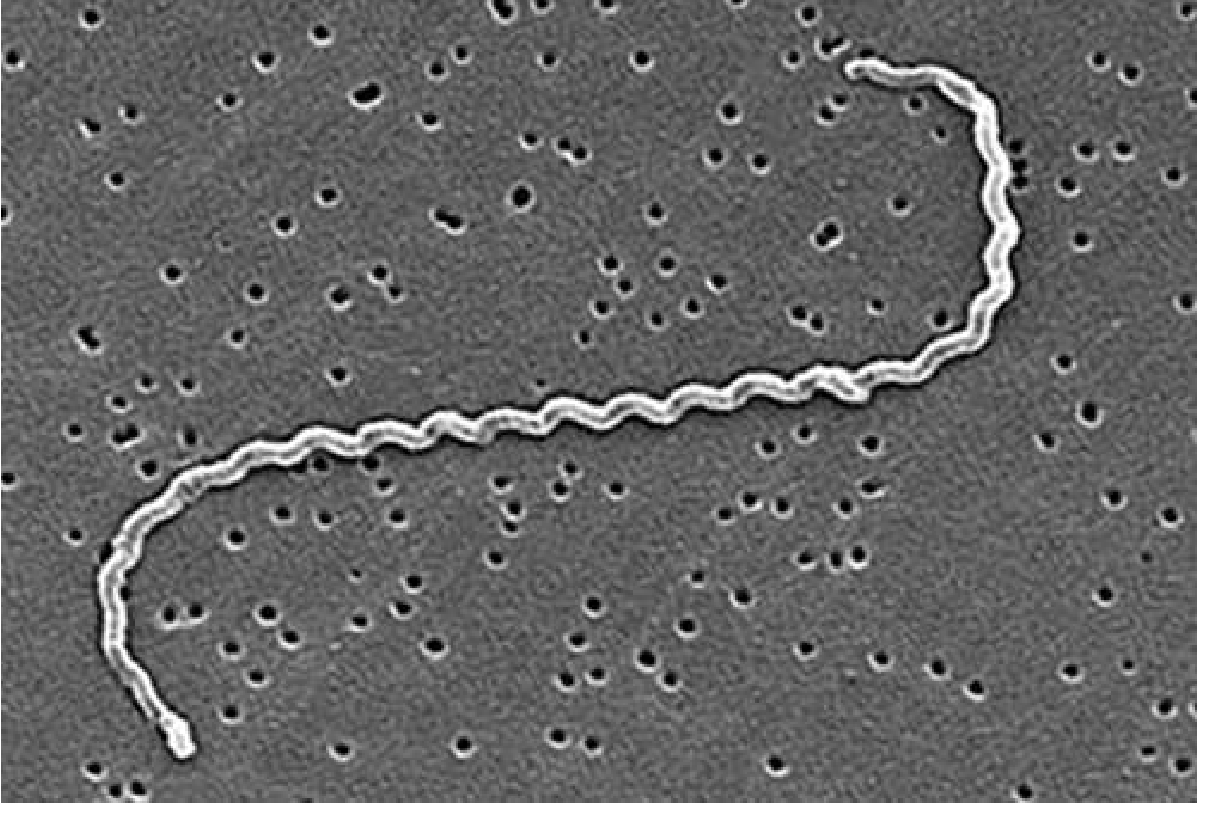
Causative agent: Pathogenic spirochetes of the genus Leptospira (most commonly L. interrogans)
- Over 25 serogroups and 250 serovars with different geographic distribution and host specificity
- Organisms colonize the renal tubules of reservoir animals → persistent urinary shedding for months to years
- Survive in humid soil and water for many months → environmental reservoir
The Three Dimensions of Leptospirosis (One Health Lens)
1. HUMAN DIMENSION
| Feature | Details |
|---|---|
| Global burden | ~1 million severe cases/year; ~60,000 deaths/year |
| Case fatality rate | ~10% in severe disease |
| Underdiagnosis | Frequently misdiagnosed as dengue, malaria, or influenza |
| At-risk occupations | Veterinarians, farmers, sewage workers, slaughterhouse workers, fishermen, rice paddy workers |
| At-risk activities | Adventure sports, flood exposure, swimming in contaminated water |
| Severe form (Weil's disease) | Jaundice + acute kidney injury + hemorrhage ± pulmonary hemorrhage (ARDS) |
(Harrison's Principles of Internal Medicine, 22E, 2025; Goldman-Cecil Medicine)
2. ANIMAL DIMENSION
| Reservoir Animal | Main Serovar |
|---|---|
| Rats (Rattus norvegicus) — most important | Icterohaemorrhagiae, Copenhageni |
| Voles | Grippotyphosa |
| Cattle | Hardjo |
| Dogs | Canicola |
| Pigs | Pomona |
| Wild boar, foxes, hedgehogs, horses | Various |
Key point: Animals are asymptomatic reservoir hosts — even asymptomatic animals shed >10¹⁰ organisms/gram of kidney tissue in their urine for years. This makes source detection and control critical for the animal sector.
(Harrison's Principles of Internal Medicine, 22E, 2025)
3. ENVIRONMENTAL DIMENSION
- Leptospira survives in warm, moist soil and stagnant/slow-moving freshwater (pH 6.0–8.0)
- Some strains form biofilms on surfaces, resisting antibiotics and environmental degradation — explaining outbreaks months after flooding
- Flooding is the major environmental trigger: washes leptospires from rodent burrows into water supplies
- Climate change → more extreme rainfall events → increasing leptospirosis incidence projected
- Land use: deforestation, agriculture, urbanization increase human–animal–environment contact
(Goldman-Cecil Medicine; WOAH 2025)
One Health Framework Applied to Leptospirosis
HUMAN SECTOR ANIMAL SECTOR
(clinicians, public (veterinarians, farmers,
health, epidemiology) animal health workers)
\ /
\ /
ONE HEALTH APPROACH
/ \
/ \
ENVIRONMENTAL SECTOR LABORATORY SERVICES
(ecologists, urban (shared surveillance,
planners, WASH) diagnostics, serovars)
One Health Interventions — Structured by Sector
A. Human Health Sector
- Clinical awareness: Recognizing leptospirosis in febrile illness, especially in at-risk occupational groups and after floods
- Chemoprophylaxis: Doxycycline 200 mg/week for high-risk short-term exposures (military, adventure travelers)
- Treatment: Penicillin G or doxycycline (mild–moderate); ceftriaxone/penicillin IV for severe disease
- Personal protection: Waterproof boots/gloves for occupational exposure; avoid wading in floodwaters; cover cuts before water exposure
- Public health messaging: Community education about flood risk, animal contact, and safe water practices
- Integrated surveillance: Mandatory reporting, standardized case definitions, data sharing with animal and environmental sectors
B. Animal Health Sector
- Vaccination of companion animals: Dogs — annual leptospirosis vaccines (bivalent/quadrivalent) are effective; all dogs at risk regardless of urban/rural setting
- Vaccination of livestock: Cattle vaccination (Hardjo serovar) reduces urinary shedding on farms
- Veterinary surveillance: Monitoring serovar distribution in animal populations; linking animal serovar data to human case serogroups
- Rodent control (vector control):
- Reduction of rodent habitats in urban areas
- Rodent sentinel surveillance programs — identifying Leptospira-positive rodent populations
- Rodent baiting and trapping in high-risk areas
- Farm hygiene: Restricting livestock access to water sources; keeping livestock areas clean to reduce urine contamination
C. Environmental Sector
- WASH (Water, Sanitation, Hygiene): Clean water supply; sewage management; reduce human contact with contaminated water
- Flood control infrastructure: Urban drainage systems, early flood warning — critical in slums/informal settlements where rodent access to homes is high
- Land use planning: Buffer zones between wildlife habitats and human settlements; slaughterhouse siting
- Environmental monitoring: Testing water sources (rivers, canals, floodwater) for Leptospira DNA using PCR
- Climate adaptation: Planning for increased flood frequency and leptospirosis risk under climate change models
D. Laboratory and Surveillance (Cross-Sector)
- Integrated sentinel surveillance: Indonesia's pilot program (WHO/Ministry of Health + Agriculture + Environment) monitors rodents, water, and human cases simultaneously
- Shared diagnostics: MAT (Microscopic Agglutination Test — gold standard), PCR, IgM ELISA used across human and veterinary labs
- Molecular typing: Linking human outbreak serovars to animal reservoirs via genomic methods
- Data systems: One integrated platform for human, animal, and environmental leptospirosis data (operationalized in Brazil, Malaysia, Chile as models)
Real-World One Health Case Studies
| Country | One Health Action |
|---|---|
| Indonesia | Pilot rodent sentinel surveillance in 10 districts; integrated human-animal-wildlife surveillance (WHO 2022) |
| Brazil | Integrated rodent surveillance + human case mapping during flooding; linked to animal serovar studies |
| Australia | One Health framework post-2018–2019 outbreaks; multi-agency response involving physicians, vets, epidemiologists, ecologists |
| Tanzania | Ministry of Health incorporating leptospirosis into national One Health strategy aligned with agriculture and flooding |
| Bangladesh/India | Occupational exposure in rice paddy farmers addressed through coordinated human + veterinary + environmental programs |
One Health Duties in Leptospirosis — Ethical Dimension
The duty of care principle expands under One Health:
- Physicians: Prevent contagion, treat the infected
- Veterinarians: Immunize animal reservoir hosts; reduce urinary shedding
- Environmental authorities: Maintain safe water; control rodent populations; mitigate flood damage
- Policymakers/planners: WASH infrastructure, urban design, climate preparedness
Key Message for Community Medicine
Leptospirosis cannot be controlled by the medical sector alone. Its cycle involves:
Rat urine → contaminated water/soil → human skin/mucosa → illness
Breaking this cycle at any point requires veterinary, environmental, and public health action simultaneously. This is why leptospirosis is used as a model disease for teaching and implementing the One Health concept in community medicine — it perfectly illustrates how human health is embedded within animal and ecosystem health.
Sources:
- Goldman-Cecil Medicine, International Edition (Chapter 298 — Leptospirosis)
- Harrison's Principles of Internal Medicine, 22E (2025) (Chapter 189 — Leptospirosis)
- Fishman's Pulmonary Diseases and Disorders
- WHO Integrated Leptospirosis Surveillance (2022)
- WOAH World Zoonoses Day Report (2025)
- PMC9696530 — One Health: An Effective and Ethical Approach to Leptospirosis Control in Australia
This is a shared conversation. Sign in to Orris to start your own chat.