Tonge discoloration
Reading File
Finding Sources
Finding Sources
Searching the Web
tongue discoloration causes clinical significance
Reading File
Finding Sources
Searching Images
tongue discoloration black hairy tongue geographic tongue strawberry tongue
Reading File
Searching Images
strawberry tongue scarlet fever Kawasaki geographic tongue red
I now have comprehensive information. Let me compile a thorough clinical answer on tongue discoloration.
Tongue Discoloration — Clinical Overview
Tongue discoloration is classified by color, mechanism (intrinsic vs. extrinsic), and underlying cause. Below is a systematic breakdown.
Normal Tongue
A healthy tongue is light pink with moist, velvety surface papillae (filiform, fungiform, circumvallate).
By Color
🖤 Black / Brown Tongue
Black Hairy Tongue (Lingua Villosa Nigra)
The most characteristic black discoloration. Results from reduced desquamation and keratin accumulation on filiform papillae, which then trap chromogenic bacteria, food debris, and tobacco pigments.
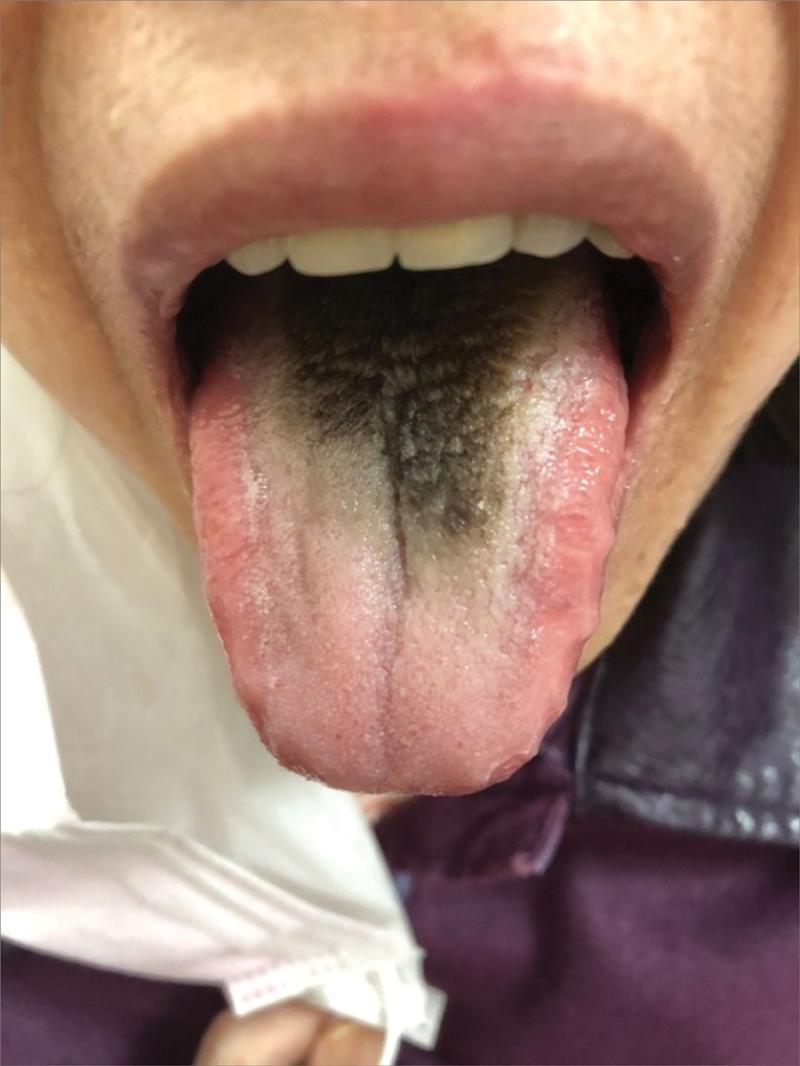
| Feature | Detail |
|---|---|
| Prevalence | 0.5–11.3% (higher in elderly, institutionalized) |
| Location | Midportion of dorsal tongue; tip and lateral borders spared |
| Color range | Yellow → brown → black (depends on staining source) |
| Risk factors | Smoking, poor oral hygiene, antibiotics (linezolid, minocycline), oxidizing mouthwashes, dehydration, soft/liquid diet, HIV |
| Mechanism | Impaired desquamation + porphyrin production by colonizing bacteria |
| Treatment | Self-limiting; tongue scraper, better hydration, coarse diet, smoking cessation; fresh pineapple (bromelain) anecdotally helpful |
Pseudo-Black Hairy Tongue: Black discoloration from bismuth (e.g., Pepto-Bismol) — extrinsic, reversible with brushing. — Dermatology 2-Volume Set 5e
Amalgam tattoo: Small, focal blue-black patch on the ventral tongue or gingiva from embedded dental amalgam fragments. Stable, requires no treatment. — Harrison's, Table 38-2
🔴 Red / Strawberry Tongue
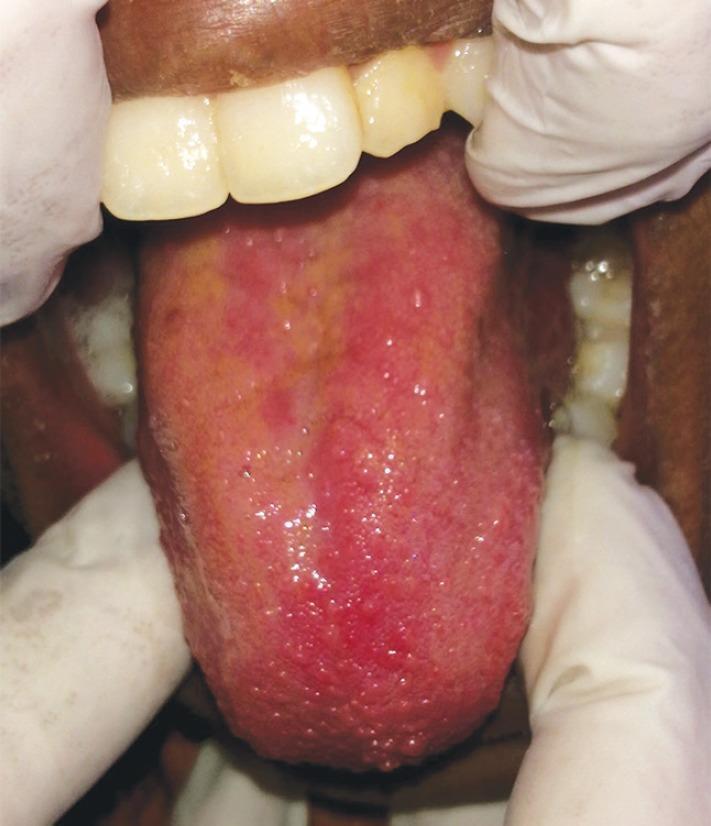
| Color Pattern | Cause | Key Association |
|---|---|---|
| Strawberry red (prominent red papillae through white coat → then beefy red) | Strep pyogenes toxin | Scarlet fever |
| Strawberry red in child | Mucocutaneous inflammation | Kawasaki disease (+ MIS-C, COVID-19 complication) |
| Beefy red / magenta | B12 / folate deficiency → atrophic glossitis | Pernicious anemia |
| Smooth red + painful | Niacin (B3) deficiency | Pellagra |
| Central red rhomboid patch | Erythematous candidiasis | Median rhomboid glossitis |
Scarlet fever progression: white strawberry tongue (day 1–2) → sloughing of white coat → red strawberry tongue (day 3+). — Tintinalli's Emergency Medicine
⬜ White / Pale Tongue
| Appearance | Cause |
|---|---|
| Pale, smooth, atrophic | Iron deficiency anemia / pernicious anemia (B12 deficiency) — atrophic glossitis |
| White removable plaques | Oral candidiasis (thrush) — pseudomembranous type |
| White non-removable patch | Leukoplakia (premalignant), lichen planus, secondary syphilis |
| White hairy patches on lateral tongue | Hairy leukoplakia — EBV-associated, marker of immunodeficiency (HIV) |
| White + red patches (migratory) | Geographic tongue (benign migratory glossitis) |
Geographic tongue: Asymmetric red denuded patches surrounded by white borders; shifts over days; associated with fissured tongue; usually asymptomatic. — Harrison's Principles of Internal Medicine 22E
🟡 Yellow Tongue
Often represents an intermediate stage before black hairy tongue. Causes:
- Early hairy tongue (bacterial overgrowth + dead cell accumulation)
- Jaundice (systemic bilirubin excess — yellowish hue from intrinsic pigmentation)
- Poor oral hygiene, dry mouth, smoking
🔵 Blue / Cyanotic Tongue
- Central cyanosis (hypoxemia) — bluish discoloration of tongue and mucous membranes
- Dark blue-black focal patch — amalgam tattoo or vascular lesion
- Noma (cancrum oris): Gangrenous stomatitis — produces dark blue-black necrotic discoloration (seen in Andrews' Clinical Atlas)
🟤 Brown / Dark Pigmented Patches
From Harrison's Table 38-2 (Pigmented Lesions of the Oral Mucosa):
| Condition | Features |
|---|---|
| Oral melanotic macule | Discrete brown-black macule; stable |
| Addison's disease | Bluish-black blotches (any oral area) + diffuse skin pigmentation + adrenal insufficiency |
| Peutz-Jeghers syndrome | Dark spots on lips + buccal mucosa + perioral/perinasal skin; concomitant intestinal polyposis |
| Drugs (minocycline, zidovudine, neuroleptics, antimalarials, oral contraceptives) | Brown/black/gray areas; resolves after drug cessation |
| Malignant melanoma | Flat diffuse or raised nodular; brown-black; expands and metastasizes early |
Mechanisms: Intrinsic vs. Extrinsic
| Type | Mechanism | Examples |
|---|---|---|
| Intrinsic | Systemic absorption alters tongue tissue | Jaundice, B12 deficiency, Addison's, Peutz-Jeghers, drug pigmentation |
| Extrinsic | Surface deposition of chromogenic material | Food stains, tobacco, bismuth, chromogenic bacteria (hairy tongue) |
Diagnostic Approach
- Color + distribution: uniform vs. patchy, dorsal vs. lateral/ventral
- Removable vs. non-removable: white coat that scrapes off → candidiasis; non-removable → leukoplakia, lichen planus
- Associated symptoms: pain, fever, lymphadenopathy, skin changes
- Medications and habits: bismuth, antibiotics, minocycline, smoking, alcohol
- Systemic signs: jaundice, anemia, immunodeficiency, adrenal insufficiency
- Age: strawberry tongue in a child → Kawasaki disease until proven otherwise
Sources: Dermatology 2-Volume Set 5e; Harrison's Principles of Internal Medicine 22E; Andrews' Diseases of the Skin Clinical Atlas 2e; Tintinalli's Emergency Medicine; K.J. Lee's Essential Otolaryngology; MSD Manuals; PMC literature on drug-associated tongue discoloration.
This is a shared conversation. Sign in to Orris to start your own chat.