Prosthetic eye types
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Loading Image
Here is a comprehensive overview of prosthetic eye types, drawn from Kanski's Clinical Ophthalmology and Cummings Otolaryngology.
Prosthetic Eye Types
A prosthetic eye (ocular prosthesis) is a cosmetic shell placed in the socket after enucleation (removal of the entire globe) or evisceration (removal of intraocular contents with sclera retained). It does not restore vision.
1. Conformer
The first device placed after surgery. Made of silicone or acrylic, it is a clear shell that:
- Supports the conjunctival fornices while healing occurs
- Maintains socket volume and shape
- Remains in place until the socket is ready for a definitive prosthesis (typically 6–8 weeks post-op)
2. Temporary Artificial Eye
A pre-made, non-customized prosthesis placed after the initial socket impression mould is taken (~6–8 weeks post-op). Used while the custom prosthesis is being manufactured.
3. Custom Ocular Prosthesis
The definitive prosthesis — individually crafted to match:
- The shape of the patient's socket (via impression mould)
- The appearance of the fellow (opposite) eye — iris colour, pupil size, vein pattern
Materials:
- Polymethylmethacrylate (PMMA) / Acrylic — the modern standard; durable, polishable, lightweight, and tissue-compatible
- Glass — historically used (German glass eyes), largely replaced by acrylic; more fragile and less customizable
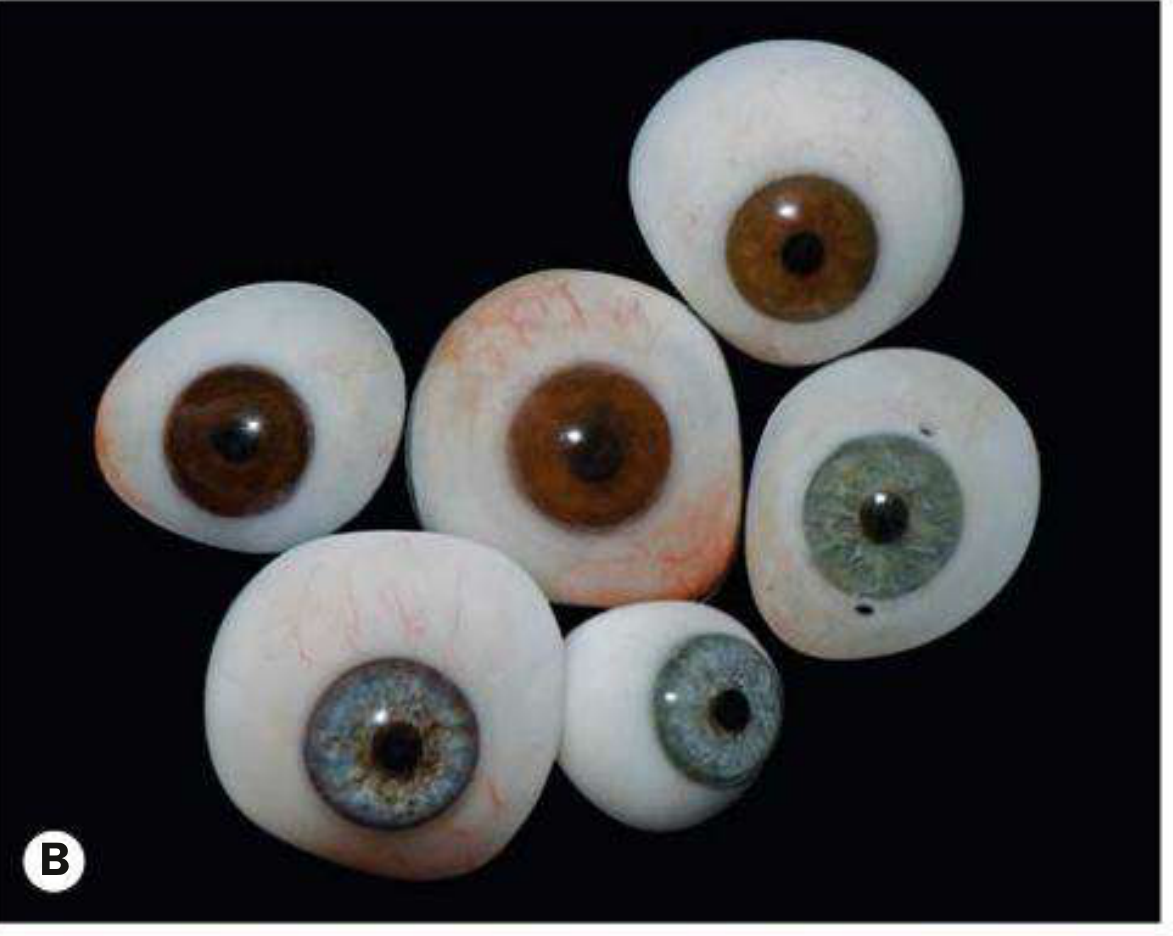
Custom PMMA ocular prostheses in various iris colours — Kanski's Clinical Ophthalmology
4. Orbital Implants (the underlying volume-replacement component)
An orbital implant is placed inside the socket at the time of enucleation to restore volume. The ocular prosthesis shell sits over it. Two main categories:
| Type | Material | Property |
|---|---|---|
| Non-integrated (solid) | Silicone, acrylic (PMMA) | No fibrovascular ingrowth; no direct attachment to prosthesis |
| Integrated (porous) | Hydroxyapatite, porous polyethylene (Medpor) | Fibrovascular ingrowth into pores; improves prosthesis motility |
- Porous implants can receive a peg (a coupling post) inserted into the implant to mechanically link it to the prosthesis, further improving motility — though peg complications (discharge, extrusion) are not uncommon.
- Extrusion is a risk with all implants; deep placement with good vascularized tissue cover is the most important preventive measure.
5. Orbital Prosthesis
Used when the entire orbit is absent or exenterated (e.g. after radical tumour surgery). This is a larger maxillofacial prosthetic device that:
- Incorporates an ocular component (a PMMA globe painted to match the contralateral eye)
- Is fabricated from silicone (for a skin-like appearance and texture)
- Is retained by adhesive, osseointegrated implants, or spectacle frames
- Includes painted eyelids, lashes, and sometimes an eyebrow
The ocular component is oriented using rulers and light reflection to match the gaze direction of the opposite eye.
Post-enucleation Socket Syndrome (PESS)
If an orbital implant is not used, volume deficit leads to:
- Enophthalmos
- Upper lid ptosis
- Superior sulcus hollowing
- Sagging lower lid (prosthesis tilts backward and exerts forward pressure on lower lid)
Correction: secondary implant insertion, silicone block in the inferior orbit, or dermis-fat graft.
Summary table:
| Type | Purpose | Material |
|---|---|---|
| Conformer | Immediate post-op socket support | Silicone or acrylic |
| Temporary prosthesis | Bridge until custom fitting | PMMA |
| Custom ocular prosthesis | Definitive cosmetic restoration | PMMA (acrylic); historically glass |
| Non-integrated implant | Orbital volume replacement | Solid silicone, acrylic |
| Integrated (porous) implant | Volume replacement + motility | Hydroxyapatite, porous polyethylene |
| Orbital prosthesis | Full orbital reconstruction | Silicone body + PMMA ocular component |
— Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed. | Cummings Otolaryngology: Head and Neck Surgery
This is a shared conversation. Sign in to Orris to start your own chat.