Give a diagramatic or interpreted overview of Prevention of CHD according to Park's Preventive medicine book
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching the Web
Park's Preventive and Social Medicine CHD prevention levels primary secondary tertiary
Generating Image
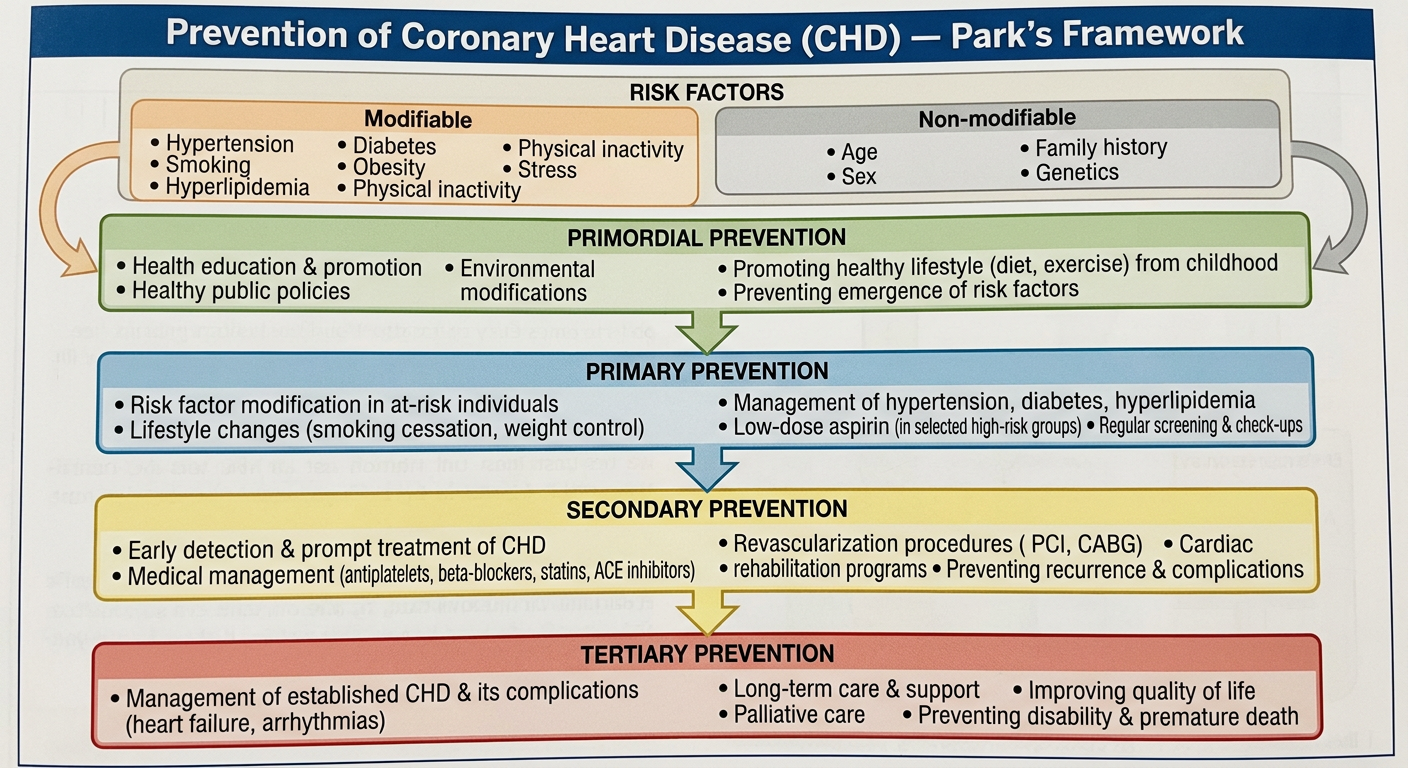
Prevention of Coronary Heart Disease (CHD) — Park's Framework
Park's Textbook of Preventive and Social Medicine approaches CHD prevention using the natural history of disease model, intercepting at multiple levels across the disease continuum. CHD prevention is organized into 4 levels, preceded by identification of risk factors.
Risk Factors for CHD
Non-Modifiable
| Factor | Details |
|---|---|
| Age | Risk rises after 45 (men), 55 (women) |
| Sex | Males at higher risk; women's risk rises post-menopause |
| Family history | First-degree relatives with premature CHD |
| Genetic factors | Familial hypercholesterolaemia, etc. |
Modifiable (Major)
| Factor | Target |
|---|---|
| Hypertension | BP < 130/80 mmHg |
| Hyperlipidaemia | LDL-C reduction; total cholesterol < 200 mg/dL |
| Cigarette smoking | Complete cessation |
| Diabetes mellitus | HbA1c < 7%; glycaemic control |
| Obesity | BMI 18.5–24.9; waist < 90 cm (M), < 80 cm (F) |
| Physical inactivity | ≥150 min/week moderate activity |
| Psychosocial stress | Type A behaviour, depression |
Modifiable (Minor/Emerging)
- Hypertriglyceridaemia, Low HDL, Homocysteinaemia, CRP elevation, Fibrinogen, Lipoprotein(a), Oral contraceptive use
The Four Levels of Prevention
🔵 Primordial Prevention
Targets the pre-risk stage — preventing the emergence of risk factors themselves in the population
Target group: Entire healthy population, especially children & youth
Measures:
- National/Community level policies: food labelling, salt reduction in processed foods, tobacco control legislation (FCTC), trans-fat bans
- Health education: promotion of healthy diet, physical activity, non-smoking habits from childhood
- School-based programmes: nutrition education, physical fitness curricula
- Urban planning: creating environments conducive to walking, cycling
- Social/economic development to reduce poverty and improve living standards
Concept: Prevention is directed at social, environmental, and economic conditions that allow risk factors to arise — not at the individual risk factors themselves.
🟢 Primary Prevention
Targets individuals at risk (risk factors present, no disease yet) — preventing CHD from ever occurring
Target group: Individuals with identified risk factors
Measures:
A. Health Promotion
- Health education about CHD risk factors
- Promote balanced diet low in saturated fats, trans fats, salt, and refined sugars
- Encourage regular aerobic exercise (brisk walking, cycling, swimming)
- Weight management & avoidance of central obesity
- Stress management; work–life balance
B. Specific Protection
- Anti-tobacco programmes; smoking cessation support (NRT, counselling)
- Control of hypertension (lifestyle + pharmacotherapy where indicated)
- Control of hyperlipidaemia (statins in high-risk individuals, diet)
- Glycaemic control in diabetes
- Aspirin in selected high-risk individuals (as per guidelines)
- Screening and referral programmes for risk factor detection
Key principle: Even a modest reduction in population-wide risk factor levels produces large absolute reductions in CHD incidence (Rose's strategy).
🟡 Secondary Prevention
Targets those with established CHD — halting progression, preventing recurrence and complications
Target group: Patients with angina, post-MI, post-revascularisation
Measures:
A. Early Diagnosis
- ECG, stress testing, coronary angiography
- Screening of high-risk asymptomatic individuals
B. Prompt Treatment
- Thrombolysis/primary PTCA/CABG for acute MI
- Antiplatelet therapy (aspirin + clopidogrel)
- Beta-blockers (post-MI cardioprotection)
- ACE inhibitors/ARBs (post-MI, HF with reduced EF)
- High-intensity statins (LDL-C ≥ 50% reduction)
- Nitrates for angina
- Rehabilitation post-MI
C. Disability Limitation
- Prevent heart failure progression
- Prevent arrhythmias (ICD implantation where indicated)
- Prevent re-infarction through strict risk factor control
🔴 Tertiary Prevention
Targets those with severe/complicated CHD — restoring maximal function and preventing further disability
Target group: Post-MI patients with heart failure, disability, or post-revascularisation
Measures:
A. Rehabilitation
- Cardiac rehabilitation programme (Phase I–III):
- Phase I: In-hospital mobilisation
- Phase II: Supervised outpatient exercise
- Phase III: Long-term community maintenance
- Psychosocial rehabilitation; management of depression and anxiety
- Vocational rehabilitation — return to work
B. Prevention of Recurrence
- Continued pharmacotherapy adherence (statins, antiplatelets, beta-blockers, ACEi)
- Lifestyle modification reinforcement
- Regular follow-up and monitoring
C. Palliative / End-Stage Care
- Management of end-stage heart failure (diuretics, device therapy, transplant evaluation)
- Palliative care for irreversible cardiac disability
Summary Diagram (Textual)
NATURAL HISTORY OF CHD
━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━
No risk Risk factors Subclinical Clinical Complications
factors emerging CHD CHD / Death
│ │ │ │ │
▼ ▼ ▼ ▼ ▼
┌──────────┐ ┌───────────┐ ┌───────────┐ ┌────────────┐ ┌──────────┐
│PRIMORDIAL│ │ PRIMARY │ │ SECONDARY │ │ SECONDARY │ │TERTIARY │
│Prevention│ │Prevention │ │Prevention │ │Prevention │ │Prevention│
│(pop-level│ │(risk factor│ │(early Dx &│ │(treatment) │ │(rehab & │
│ policies)│ │ control) │ │ screening)│ │ │ │ palliate)│
└──────────┘ └───────────┘ └───────────┘ └────────────┘ └──────────┘
↑ ↑ ↑ ↑ ↑
Leavell & Leavell & Leavell & Leavell & Leavell &
Clark Level Clark Level 1 Clark Level 2 Clark Level 3 Clark Level 4/5
(added (Health (Early diag. (Treatment (Rehab)
by WHO) Promo + + Rx) + Disab.
Specific limit.)
Protection)
━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━
Key Park's Concepts in CHD Prevention
| Concept | Relevance |
|---|---|
| Leavell & Clark's levels | 5 levels mapped to natural history of disease |
| Primordial prevention | Added specifically for NCDs like CHD by WHO/Park |
| Rose's Population Strategy | Small shift in population BP/cholesterol = large CHD reduction |
| High-Risk Strategy | Target intensive prevention at those with most risk |
| Epidemiological triad | Host (genetics, age) + Agent (atherogenic factors) + Environment (diet, stress, smoking culture) |
| Web of causation | CHD is multi-factorial; no single cause — prevention must be multi-pronged |
Note: Park's Textbook of Preventive and Social Medicine (24th ed.) places CHD prevention within the broader framework of non-communicable disease (NCD) control, emphasising that primordial prevention — absent from earlier Leavell & Clark schemas — is the most impactful level for population-wide CHD burden reduction, as it prevents the very emergence of risk factors.
This is a shared conversation. Sign in to Orris to start your own chat.