Caushing syndrome
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Searching Images
Cushing syndrome clinical features signs
Loading Image
Loading Image
Here is a comprehensive overview of Cushing Syndrome based on authoritative medical textbooks.
Cushing Syndrome
Definition & Terminology
Cushing syndrome refers to the clinical state caused by chronic exposure to excess glucocorticoids — from any source. Cushing disease is a specific subtype: excess cortisol driven by an ACTH-secreting pituitary corticotroph adenoma. The term "Cushing disease" should not be used interchangeably with "Cushing syndrome."
"Cushing syndrome reflects excessive tissue exposure to glucocorticoids... the most common cause is when excess cortisol is produced by the unmitigated release of ACTH from a pituitary adenoma; the term Cushing disease is reserved for this specific cause." — Goldman-Cecil Medicine
Causes (Classification)
1. Exogenous (most common overall)
- Iatrogenic glucocorticoid administration (the #1 cause worldwide)
2. ACTH-Dependent (endogenous, ~80–85%)
| Cause | Proportion |
|---|---|
| Cushing disease (pituitary corticotroph adenoma) | ~80% of ACTH-dependent cases |
| Ectopic ACTH secretion (lung carcinoid, SCLC, thymic tumors) | ~20% of ACTH-dependent cases |
3. ACTH-Independent (~15–20%)
- Adrenocortical adenoma
- Adrenocortical carcinoma
- Bilateral adrenal nodular hyperplasia (primary pigmented nodular adrenocortical disease, PPNAD)
"ACTH-dependent hypercortisolism accounts for 80% to 85% of endogenous Cushing syndrome. Approximately 80% of ACTH-dependent disease results from primary pituitary pathology and is known as Cushing disease." — Campbell-Walsh-Wein Urology
Pathophysiology
The hypothalamic-pituitary-adrenal (HPA) axis normally operates via negative feedback:
- Hypothalamus secretes CRH → stimulates anterior pituitary
- Pituitary secretes ACTH (cleaved from POMC) → stimulates adrenal zona fasciculata
- Adrenal produces cortisol → feeds back to suppress CRH and ACTH
- Cortisol follows a circadian rhythm (peak in morning, nadir ~11 PM)
In Cushing syndrome, this feedback loop is disrupted, producing sustained hypercortisolism without the normal diurnal variation.
Clinical Features
Classic Physical Signs
Central / Fat redistribution:
- Centripetal (truncal) obesity — sparing of limbs
- Moon facies — rounded face from fat deposition
- Buffalo hump — dorsocervical fat pad between scapulae
- Supraclavicular fat pads
- Facial plethora (ruddy cheeks from increased hematocrit)
Skin:
- Wide violaceous striae — >1 fingerbreadth wide, purple; distinguishable from pregnancy striae by their width and color
- Easy bruising / ecchymoses — from capillary fragility and thin skin
- Hyperpigmentation — particularly in ectopic ACTH syndrome (excess ACTH binds MC1R)
- Hirsutism, acne, thin skin, impaired wound healing, edema
Musculoskeletal:
- Proximal muscle weakness — difficulty rising from chairs, climbing stairs
- Osteoporosis, vertebral fractures, back pain
Metabolic:
- Glucose intolerance / diabetes mellitus
- Hypokalemia and metabolic alkalosis (particularly in ectopic ACTH)
- Hypercalciuria and nephrolithiasis
Reproductive:
- Oligomenorrhea / amenorrhea in women
- Decreased libido in both sexes
- Female-pattern baldness in women
Neuropsychiatric:
- Depression (common; suicidal ideation in severe cases)
- Emotional lability, irritability
- Psychosis
- Sleep disruption
Cardiovascular:
- Hypertension — from direct mineralocorticoid effects of ACTH and glucocorticoid excess
- Hypercoagulability → DVT and pulmonary embolism risk
Clinical Photos
Truncal obesity with violaceous striae:
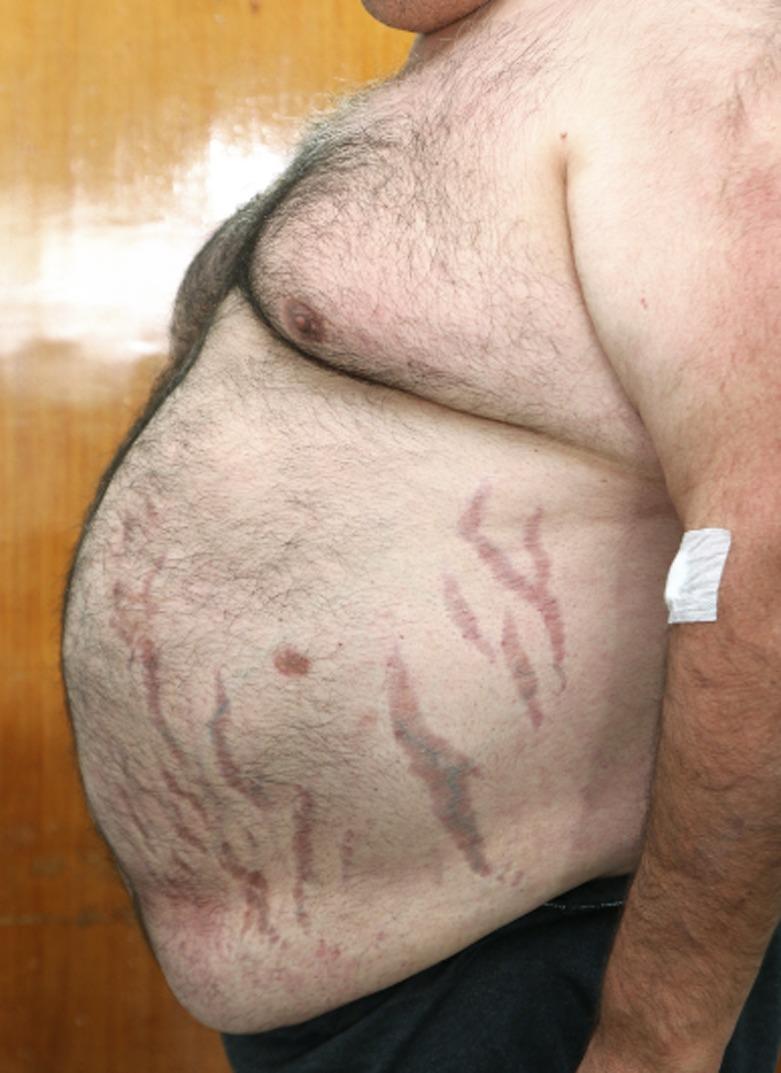
Moon facies and facial plethora:
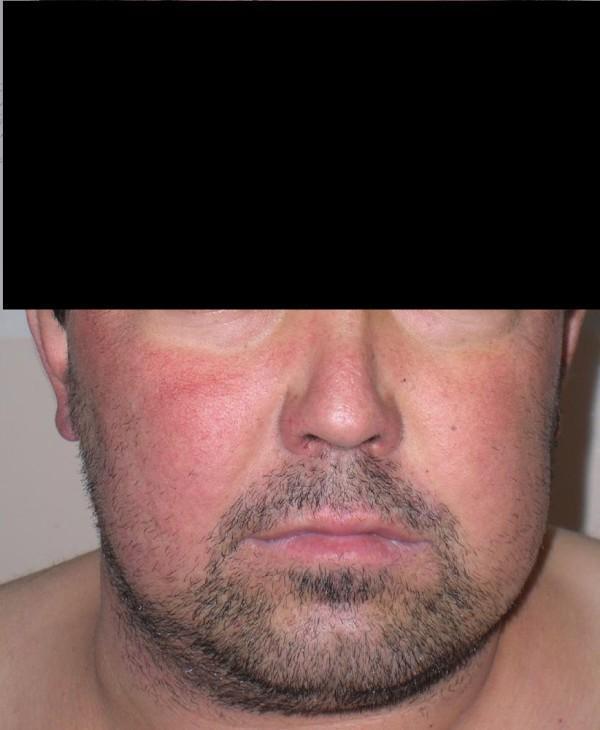
Diagnosis
Diagnosis is a two-step process: confirm hypercortisolism, then determine the cause.
Step 1 — Confirm Cortisol Excess (Screening Tests)
| Test | Details |
|---|---|
| 24-hour urinary free cortisol (UFC) | Elevated in Cushing syndrome; must be ≥2× ULN to be meaningful |
| Late-night salivary cortisol | Exploits loss of circadian rhythm; highly sensitive |
| Overnight 1-mg dexamethasone suppression test (DST) | Normal: cortisol <1.8 µg/dL; failure to suppress suggests hypercortisolism |
| Low-dose DST (2-day, 0.5 mg q6h) | More specific; failure to suppress confirms Cushing |
Step 2 — Determine the Cause
| Test | Purpose |
|---|---|
| Plasma ACTH level | Suppressed (<5 pg/mL) = ACTH-independent (adrenal source); elevated/normal = ACTH-dependent |
| High-dose DST (8 mg overnight) | Suppression to <50% baseline suggests pituitary origin (Cushing disease); no suppression suggests ectopic or adrenal |
| Pituitary MRI | Detects corticotroph adenoma (often <6 mm microadenoma) |
| CRH stimulation test | Pituitary adenoma responds (ACTH rises ≥35%, cortisol ≥20%); ectopic source does not |
| Inferior petrosal sinus sampling (IPSS) | Gold standard for confirming pituitary origin; central-to-peripheral ACTH ratio >2 (basal) or >3 (post-CRH) indicates Cushing disease |
| CT adrenals / chest imaging | For adrenal or ectopic source localization |
"The high-dose DST is used to answer the question, 'Is Cushing syndrome caused by a pituitary corticotroph adenoma (Cushing disease), or from an ectopic source?'" — Quick Compendium of Clinical Pathology
Treatment
Cushing Disease (Pituitary)
- Transsphenoidal surgery (TSS) — first-line; remission in 65–90% for microadenomas
- Radiotherapy — for persistent/recurrent disease or surgical failures
- Bilateral adrenalectomy — definitive but risks Nelson syndrome (enlarging pituitary tumor + hyperpigmentation)
- Medical therapy (second-line or bridge): ketoconazole, metyrapone, mitotane, osilodrostat, pasireotide (somatostatin analog)
Adrenal Cushing (ACTH-independent)
- Unilateral adrenalectomy for adenoma/carcinoma
- Bilateral adrenalectomy for bilateral disease
Ectopic ACTH Syndrome
- Remove the primary tumor when possible
- Medical adrenal-blocking therapy while awaiting surgery
Exogenous Cushing
- Gradual tapering of glucocorticoids (the HPA axis will be suppressed and requires time to recover)
Epidemiology
- Endogenous Cushing syndrome: 2–5 cases/million/year
- Cushing disease specifically: 1.2–2.4/million/year
- Female predominance (8–10:1 in Cushing disease)
- Most pituitary tumors are microadenomas (<10 mm); 10–15% are macroadenomas
Key Sources:
- Goldman-Cecil Medicine, International Edition
- Campbell-Walsh-Wein Urology, 3-Volume Set
- Fitzpatrick's Dermatology
- Quick Compendium of Clinical Pathology, 5th ed.
- Washington Manual of Medical Therapeutics
This is a shared conversation. Sign in to Orris to start your own chat.