a 34 year old female suffers from hair thinning hairfall and hair breakage
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
I now have comprehensive information to provide a thorough, well-cited answer. Let me compose the response.
Hair Thinning, Hairfall & Breakage in a 34-Year-Old Female
In a woman of this age, these three symptoms together most commonly point to one or more of the following conditions, which often co-exist:
1. Androgenetic Alopecia (AGA) — Female Pattern Hair Loss
The most common cause of progressive hair thinning in women.
Presentation
- Diffuse thinning over the centroparietal (crown) region with preservation of the frontal hairline — the Ludwig pattern
- Alternatively, a "Christmas tree" pattern: centroparietal thinning with additional breaching of the frontal hairline
- Slowly progressive; patients often notice reduced hair density rather than dramatic shedding
- Hair shaft miniaturization occurs — follicles produce progressively thinner, shorter hairs
Classification (Ludwig scale)
| Grade | Description |
|---|---|
| I | Minimal thinning of crown |
| II | Moderate, visible widening of part |
| III | Severe, near-complete loss at crown |
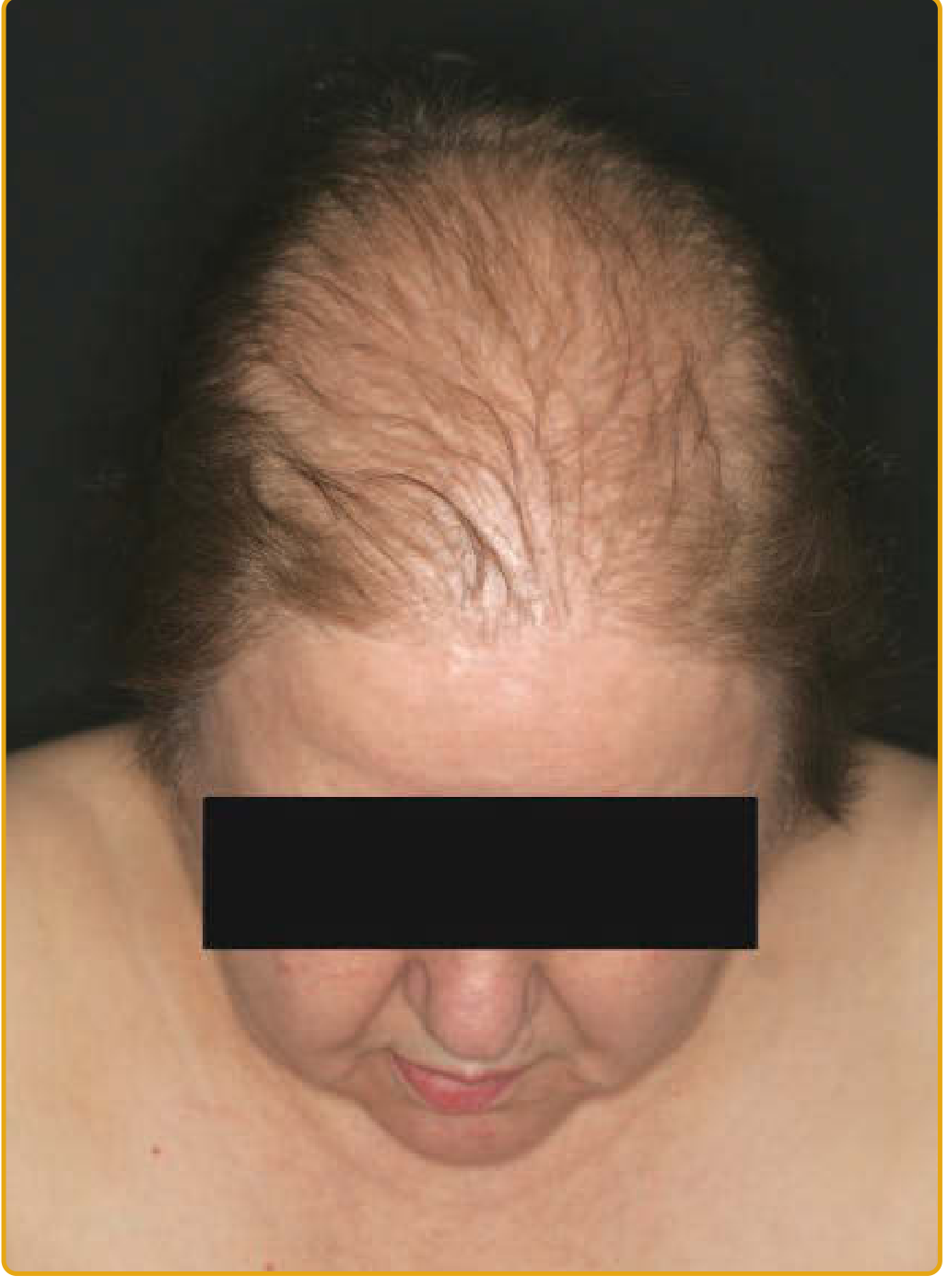
Pathogenesis
- Multifactorial and polygenic
- In women, the role of androgens is less certain than in men; there is a subset with associated hormonal dysregulation (e.g., PCOS, hyperandrogenism)
- Weak association with the androgen receptor (AR/EDA2) locus and estrogen receptor 2 (ESR2) gene
- DHT-driven follicular miniaturization (same mechanism as in men, but less dominant in females)
— Fitzpatrick's Dermatology, Vol. 1 & 2, p. 1526–1527
2. Telogen Effluvium (TE)
The most common cause of diffuse hair shedding (hairfall).
Presentation
- Excessive shedding of telogen club hairs (hair lost "at the root," with a visible depigmented bulb)
- Typically occurs 3–5 months after a trigger
- Can be acute (resolves in months) or chronic (>6 months)
- Normal daily loss: ~100–150 hairs/day; TE significantly exceeds this
Common Triggers in Young Women
| Category | Examples |
|---|---|
| Physiological | Postpartum, hormonal changes |
| Nutritional | Iron deficiency, ferritin <70 µg/L, protein deficiency, crash dieting, zinc deficiency |
| Endocrine | Hypothyroidism, hyperthyroidism, PCOS |
| Psychological | Severe stress, anxiety |
| Medications | OCP discontinuation, retinoids, anticoagulants |
| Systemic illness | Fever, surgery, chronic illness |
Diagnosis
- Pull test: >4–6 club hairs from 40-hair grasp = abnormal
- Trichogram: anagen/telogen ratio
- Hairfall is characterized by telogen hairs with nonpigmented, club-shaped bulbs
— Andrews' Diseases of the Skin, p. 870
3. Hair Breakage (Structural Hair Damage)
Hair breakage is distinct from hair loss — the hair shaft breaks mid-length rather than falling from the root.
Causes
- Nutritional deficiencies: Iron, zinc, biotin, protein malnutrition
- Chemical damage: Bleaching, perming, relaxing
- Mechanical/thermal: Excessive heat styling, tight hairstyles (traction), over-brushing
- Underlying scalp disease: Seborrheic dermatitis, tinea capitis
Workup / Investigations
For a 34-year-old woman presenting with all three symptoms, the following baseline investigations are recommended:
| Investigation | Rationale |
|---|---|
| Serum ferritin | Most sensitive marker of iron deficiency in TE |
| CBC | Anemia |
| TSH, free T4 | Thyroid disease (very common cause in women) |
| Fasting glucose / insulin | PCOS screening |
| Free & total testosterone, DHEAS | Hyperandrogenism |
| LH:FSH ratio | PCOS |
| Serum zinc, vitamin D, B12 | Nutritional deficiencies |
| ANA | If lupus suspected |
| Trichoscopy / dermoscopy | Peripilar signs, hair diameter variability, yellow dots |
| Scalp biopsy | If diagnosis unclear after clinical workup |
Treatment
Androgenetic Alopecia (Female)
1. Topical Minoxidil — First-line, evidence-based
- 2% solution: 1 mL twice daily
- 5% foam: Half a cap once daily
- Assess response at 6 months; treatment must be continued indefinitely to maintain benefit
- Warn patient about transient increased shedding in the first 8 weeks (telogen release)
- Side effects: hypertrichosis (local), irritant/allergic contact dermatitis
- Pause during pregnancy and lactation
2. Anti-androgens (in women with hormonal dysregulation)
- Spironolactone 100–200 mg/day (off-label; effective in hyperandrogenic women)
- Oral contraceptives with anti-androgenic progestins (e.g., cyproterone acetate, drospirenone)
- Finasteride 5 mg/day: may be effective in normoandrogenic pre- and postmenopausal women, but contraindicated in women of childbearing potential unless reliable contraception is used (risk of feminization of male fetus)
3. Low-Level Laser Therapy (LLLT): Evidence-based adjunct for AGA in women
4. Platelet-Rich Plasma (PRP): Increasingly used; evidence growing
5. Hair Transplantation: For stable, advanced AGA
Telogen Effluvium
- Address and correct the underlying trigger
- Iron supplementation if ferritin is low (target ferritin >70 µg/L)
- Most acute TE resolves spontaneously within 3–6 months once the trigger is removed
- Topical minoxidil can be used in chronic TE
Hair Breakage
- Correct nutritional deficiencies
- Reduce chemical and mechanical trauma
- Protein/biotin supplementation if deficient
Key Points for This Patient
- At 34 years old, hormonal evaluation for PCOS and thyroid disease is especially important
- Ferritin and thyroid function should be checked before attributing hair loss to AGA
- Hair thinning + shedding + breakage together often suggests a combined picture of AGA + TE + nutritional deficiency
- Topical minoxidil 2% is the single most evidence-supported intervention for female AGA
- Psychosocial impact is often underestimated — address patient concerns and set realistic expectations (months to see benefit)
— Fitzpatrick's Dermatology, Vol. 1 & 2, p. 1527–1530; Andrews' Diseases of the Skin, p. 870
This is a shared conversation. Sign in to Orris to start your own chat.