Layer of digestive system Mucosa submucosa Teeth and tounge
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Loading Image
Loading Image
Searching Images
tooth anatomy enamel dentin pulp cementum structure
I now have everything I need. Let me compile a comprehensive, well-organized answer.
Layers of the Digestive System
The wall of the gastrointestinal tract is organized into four concentric layers from lumen to outer surface. The diagram below shows this beautifully:
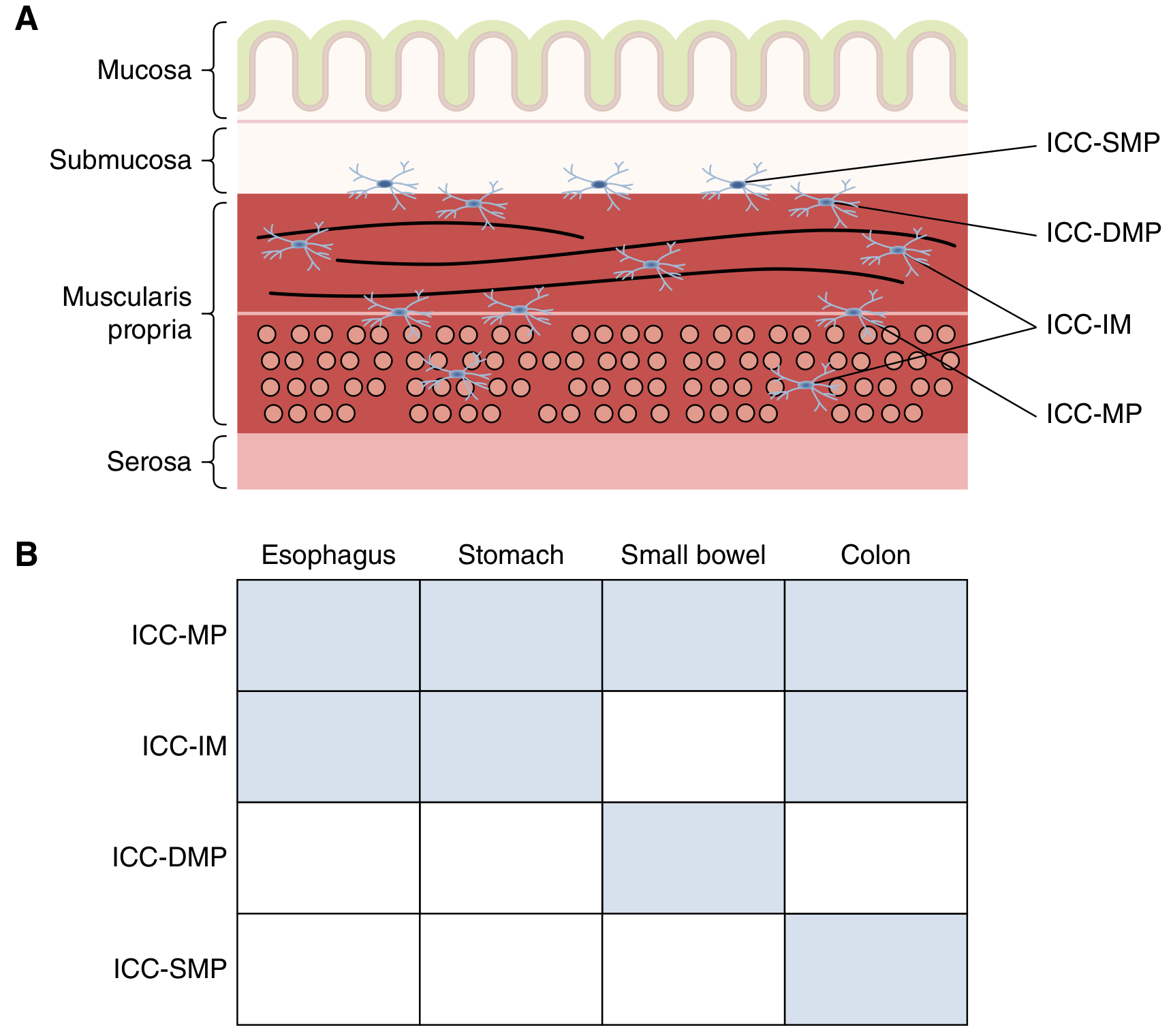
1. Mucosa (Innermost Layer)
The mucosa is the innermost layer lining the lumen. It has three sublayers:
a) Epithelium
- Lines the lumen and is adapted to the region:
- Esophagus: stratified squamous epithelium (protection from abrasion)
- Stomach to large intestine: simple columnar epithelium (absorption + secretion)
- Tight junctions form a selectively permeable barrier against antigens and pathogens
- Secretes antibodies (IgA) received from the underlying connective tissue
b) Lamina Propria
- Loose connective tissue beneath the epithelium
- Contains:
- Mucosal glands (secrete mucus, enzymes, hormones)
- Fenestrated blood capillaries for absorbing nutrients
- Lymphatic capillaries (especially important for lipid absorption in small intestine)
- Diffuse lymphatic tissue + lymphatic nodules — collectively called GALT (gut-associated lymphoid tissue)
- Peyer's patches in the ileum; lymphoid nodules in the appendix
c) Muscularis Mucosae
- Deepest sublayer of the mucosa
- Thin layer of inner circular + outer longitudinal smooth muscle
- Contraction creates local ridges and valleys → facilitates absorption and secretion
- This localized movement is independent of peristalsis
Functions of the mucosa: protection, absorption, secretion
2. Submucosa
- Dense irregular connective tissue layer external to the mucosa
- Contains:
- Larger blood vessels (send branches to mucosa, muscularis, and serosa)
- Lymphatic vessels
- Submucosal (Meissner's) plexus — unmyelinated nerve fibers and parasympathetic ganglion cells; part of the enteric nervous system; regulates mucosal secretion and blood flow
- Submucosal glands in specific regions (esophagus and proximal duodenum — Brunner's glands)
- Surface folds of the mucosa + submucosa form plicae circulares in the small intestine, greatly increasing surface area for absorption
3. Muscularis Externa (Muscularis Propria)
- Two concentric thick layers of smooth muscle:
- Inner circular layer — constricts the lumen, compresses and mixes contents
- Outer longitudinal layer — shortens the tube, propels contents
- Between the two layers lies the myenteric (Auerbach's) plexus — postganglionic parasympathetic neurons + enteric nervous system neurons that control peristalsis
- Peristalsis = rhythmic contraction waves that propel luminal contents distally
Regional variations:
| Region | Variation |
|---|---|
| Proximal esophagus | Striated muscle (voluntary) |
| Stomach | Extra oblique layer (innermost), allowing churning |
| Pylorus, LES, ileocecal valve | Thickened circular layer → sphincters |
| Anal canal | Striated muscle in external anal sphincter |
4. Serosa / Adventitia (Outermost Layer)
- Serosa: simple squamous epithelium (mesothelium) + thin connective tissue = visceral peritoneum. Present where the gut is suspended in the peritoneal cavity (stomach, small intestine, transverse colon, etc.)
- Adventitia: loose connective tissue without a mesothelial covering. Present where the gut is retroperitoneal or fixed to the body wall (thoracic esophagus, descending/ascending duodenum, ascending/descending colon, rectum, anal canal)
- Large blood vessels, lymphatics, and nerve trunks travel through the serosa from the mesentery
Teeth
Structure of a Tooth
A tooth has three specialized calcified tissues and a central cavity:
| Tissue | Location | Key Features |
|---|---|---|
| Enamel | Crown (visible part) | Hardest substance in the body; made of enamel rods produced by ameloblasts during development; regulated by amelogenins, ameloblastins, enamelins; mostly hydroxyapatite |
| Dentin | Deep to enamel (crown) and under cementum (root) | Deposited by odontoblasts as predentin → mineralized to dentin by dentin phosphoprotein (DPP) and dentin sialoprotein (DSP); contains odontoblast tubules |
| Cementum | Root surface | Bone-like tissue; anchors the periodontal ligaments that connect tooth to alveolar socket |
| Dental Pulp | Central pulp cavity (pulp chamber + root canals) | Soft connective tissue; richly vascularized and innervated; odontoblasts line the pulp–dentin junction |
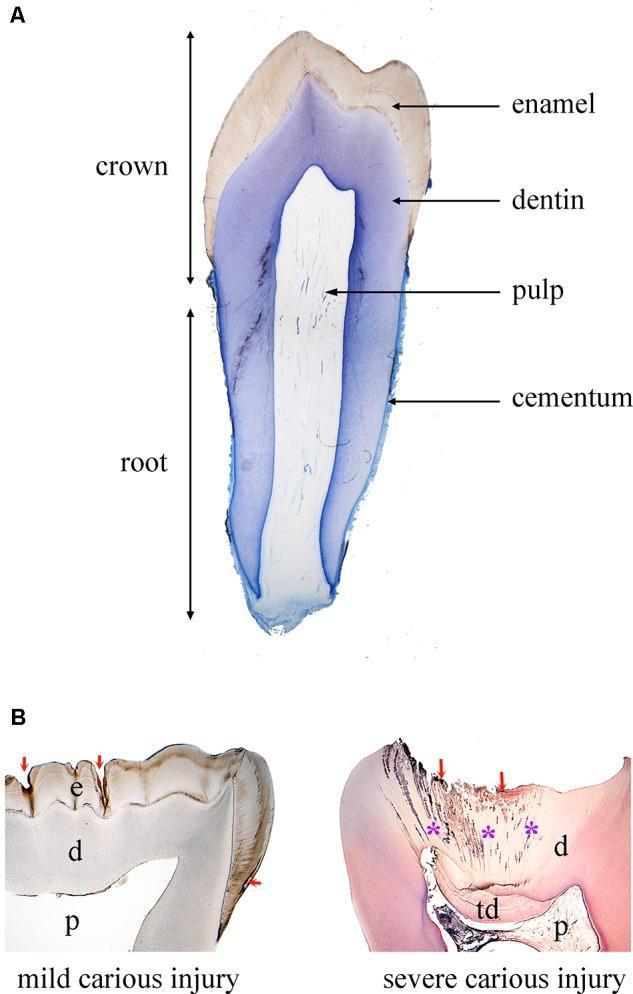
Supporting Structures
- Periodontal ligament: collagen fibers from cementum anchoring tooth to alveolar bone
- Alveolar bone: the socket
- Gingiva (gum): mucosal covering of the alveolar process
Tongue
The tongue is a mass of striated (voluntary) muscle covered by mucous membrane. Fascicles run in all directions, giving it exceptional mobility.
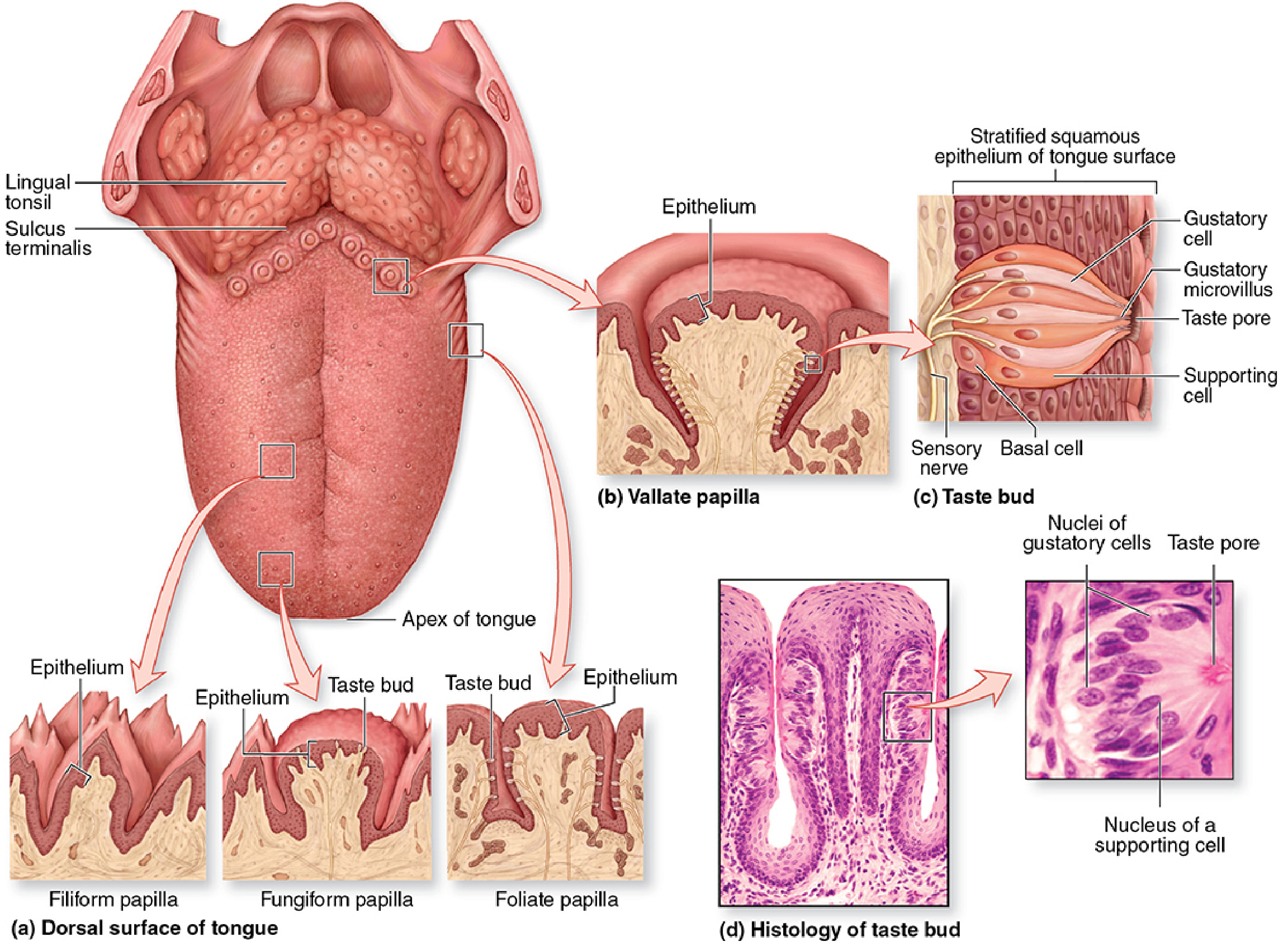
Surfaces
| Surface | Features |
|---|---|
| Ventral (inferior) | Smooth lining mucosa |
| Dorsal (superior) | Anterior 2/3: lingual papillae; Posterior 1/3: lingual tonsils |
The sulcus terminalis (V-shaped groove) separates the anterior papillary area from the posterior tonsillar area.
Four Types of Lingual Papillae
| Type | Description | Taste Buds? |
|---|---|---|
| Filiform | Most numerous; elongated, conical, heavily keratinized; whitish; provide friction for food movement | No |
| Fungiform | Mushroom-shaped, lightly keratinized; scattered among filiform; well-vascularized | Yes (a few) |
| Foliate | Parallel ridges on lateral tongue; rudimentary in adults | Yes |
| Vallate (Circumvallate) | Largest (1–3 mm diameter); 8–12 papillae in a V-line just anterior to sulcus terminalis; surrounded by a moat with serous salivary gland (Ebner's gland) ducts | Most abundant |
Taste Buds
Each taste bud contains:
- Gustatory (taste) cells — neuroepithelial sensory cells; microvilli project through the taste pore
- Supporting cells
- Basal stem cells — renew the other cell types
Five basic tastes detected: sweet, salty, bitter, sour, and umami
- Sweet, bitter, umami → G-protein-coupled receptors
- Sour, salty → ion channels (Na⁺ and K⁺)
Lingual Tonsil
- Posterior 1/3 of tongue
- Aggregation of diffuse lymphatic tissue and lymphatic nodules
- Part of Waldeyer's tonsillar ring (immune defense)
Sources: Histology: A Text and Atlas with Correlated Cell and Molecular Biology, p. 1521–1526; Junqueira's Basic Histology, p. 738–740, 1491–1492
This is a shared conversation. Sign in to Orris to start your own chat.