arrhythmias-definition,etiology, classification, symptoms, diagnosis, treatment
Reading File
Finding Sources
Finding Sources
Searching PubMed
"cardiac arrhythmia"[MeSH Terms] AND "classification"[MeSH Terms]
Reading File
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Searching Images
cardiac arrhythmia classification ECG diagram
Reading File
Searching Images
antiarrhythmic drugs Vaughan Williams classification mechanism
I now have comprehensive data from Braunwald's Heart Disease. Let me compile the full, authoritative answer.
Cardiac Arrhythmias
1. Definition
An arrhythmia (or dysrhythmia) is any disturbance in the normal rate, rhythm, site of origin, or conduction pattern of the cardiac impulse. Normal sinus rhythm originates in the sinoatrial (SA) node and results in a regular sequence of atrial and ventricular depolarizations at 60–100 beats/min. Any deviation — whether in automaticity, conduction velocity, or refractoriness — constitutes an arrhythmia.
Sinus arrhythmia specifically refers to a phasic variation in sinus cycle length in which the maximum minus minimum sinus cycle length exceeds 120 msec (or >10% of the minimum cycle length). It is the most frequent form of arrhythmia and is physiologically normal.
2. Etiology & Predisposing Factors
Arrhythmias arise from three broad categories of cause:
Structural / Cardiac Disease
- Coronary artery disease / MI — sinus bradycardia occurs in 10–15% of acute MI patients; ventricular arrhythmias arise from ischemic scars; reentrant VT is strongly associated with myocardial fibrosis
- Heart failure / Cardiomyopathy — structural remodeling (fibrosis), electrophysiologic remodeling, and neural (autonomic) remodeling all contribute
- Valvular disease, myocarditis, pericarditis, congenital heart disease
- Hypertrophy — increased wall stress and ionic remodeling raise arrhythmic risk
Systemic / Extra-Cardiac
- Electrolyte disturbances — hypokalemia, hypomagnesemia, hypocalcemia
- Metabolic — hypoxia, hypothyroidism (myxedema), hypothermia, sepsis
- Autonomic — excessive vagal tone (vasovagal syncope, carotid sinus hypersensitivity), sympathetic activation (catecholamine excess, emotional stress)
- Elevated intracranial pressure, meningitis, intracranial tumors, cervical/mediastinal tumors
- Neurally mediated — eye surgery, coronary arteriography, vomiting reflex
Drug / Toxic
- Antiarrhythmics themselves — proarrhythmia (e.g., class IA/IC agents, TdP from QT-prolonging drugs)
- Beta-blockers, calcium channel blockers, digoxin, amiodarone — can cause bradyarrhythmias
- Sympathomimetics — catecholamines, cocaine, thyroid hormone excess
- Other — lithium, clonidine, propafenone, parasympathomimetic drugs; even ophthalmic beta-blocker drops can cause SA/AV nodal abnormalities in elderly patients
Genetic / Channelopathies
- Long QT syndrome (LQTS) — mutations in K⁺ or Na⁺ channel genes → prolonged APD → EADs → TdP
- Short QT syndrome, Brugada syndrome, CPVT, HCM, ARVC
- Remodeling through autonomic remodeling (nerve sprouting, denervation) amplifies dispersion of refractoriness
3. Mechanisms
Three fundamental electrophysiologic mechanisms underlie arrhythmias:
A. Abnormal Automaticity
- Normal automaticity: SA node fires spontaneously due to pacemaker current (I_f — "funny current") via HCN channels
- Enhanced automaticity: ectopic foci in atria, AV junction, or ventricles discharge faster than the SA node
- Antiarrhythmic drugs suppress ectopic firing by depressing diastolic depolarization slope, shifting threshold voltage, or hyperpolarizing resting membrane potential
B. Triggered Activity
- Early afterdepolarizations (EADs): occur during phases 2–3 of the action potential, caused by APD prolongation (e.g., LQTS, hypokalemia, QT-prolonging drugs); mediated by reactivation of L-type Ca²⁺ or late Na⁺ currents → TdP
- Delayed afterdepolarizations (DADs): occur after full repolarization (phase 4), caused by cytosolic Ca²⁺ overload (digitalis toxicity, catecholamine excess, heart failure) via SR Ca²⁺ release → transient inward current
C. Reentry
The most common mechanism for sustained tachyarrhythmias. Requires:
- Two anatomically or functionally distinct pathways
- Unidirectional block in one pathway
- Sufficient conduction slowing in the other to allow the blocked pathway to recover
Fibrosis and gap junction remodeling (lateralization of Cx43, annular gap junctions in failing hearts) exacerbate anisotropic conduction and facilitate reentry. Acute MI reduces side-to-side electrical coupling, exaggerating anisotropy.
4. Classification
Arrhythmias are classified by rate, origin, and mechanism:
By Rate
| Type | Heart Rate |
|---|---|
| Bradyarrhythmia | < 60 bpm |
| Normorhythmia | 60–100 bpm |
| Tachyarrhythmia | > 100 bpm |
By Site of Origin
Supraventricular Arrhythmias (SVA)
- Sinus node: Sinus bradycardia, sinus tachycardia, sinus arrhythmia, sick sinus syndrome (SSS), sinoatrial block
- Atrial: Atrial premature complexes (APCs), atrial tachycardia (AT), atrial flutter, atrial fibrillation (AF)
- AV junctional: Junctional rhythm, AV nodal reentrant tachycardia (AVNRT), AV reentrant tachycardia (AVRT — e.g., WPW syndrome)
Ventricular Arrhythmias
- Premature ventricular complexes (PVCs)
- Ventricular tachycardia (VT): monomorphic, polymorphic
- Ventricular flutter and ventricular fibrillation (VF)
- Torsades de pointes (TdP) — polymorphic VT in setting of prolonged QT
Conduction Disturbances
- SA block: first-, second-, third-degree
- AV block:
- First-degree (prolonged PR > 200 ms)
- Second-degree Mobitz type I (Wenckebach — AV nodal)
- Second-degree Mobitz type II (infranodal — His-Purkinje)
- Third-degree (complete heart block)
- Bundle branch blocks (LBBB, RBBB), fascicular blocks
By Duration
- Paroxysmal (self-terminating)
- Persistent (requires cardioversion)
- Permanent (cardioversion not feasible or elected)
5. Clinical Features / Symptoms
Symptoms depend on the type, rate, duration of arrhythmia, and the underlying cardiac substrate:
| Symptom | Common Causes |
|---|---|
| Palpitations | APCs, PVCs, any tachyarrhythmia |
| Dizziness / presyncope | Bradyarrhythmias, VT, rapid SVT |
| Syncope | High-degree AV block, VT/VF, SSS, vasovagal |
| Dyspnea / fatigue | AF, VT, tachycardia-induced cardiomyopathy |
| Chest pain / angina | Rapid VT, AF in CAD patients |
| Sudden cardiac death | VF, polymorphic VT, complete AV block |
| Near-SCD / cardiac arrest | VF from any structural disease |
- Sinus bradycardia is asymptomatic in healthy young adults and athletes (HR may fall to 35–40 bpm during sleep); symptomatic only when cardiac output is inadequate
- Tachyarrhythmia-induced cardiomyopathy can develop from persistent, untreated tachycardia — with potential normalization of LV function after successful treatment
- Second-degree AV nodal block (proximal to His) without structural disease follows a benign course in younger patients but carries poor prognosis in structural heart disease
6. Diagnosis
History & Physical
- Onset, duration, associated symptoms (syncope, chest pain)
- Drug history (QT-prolonging agents, digoxin, stimulants)
- Family history (LQTS, SCD, HCM, ARVC)
12-Lead ECG
The cornerstone of arrhythmia diagnosis:
- P wave morphology and PR interval → SA/AV node function
- QRS duration and morphology → bundle branch block, VT vs. SVT with aberrancy
- QT interval → LQTS risk
- Delta waves → pre-excitation (WPW)
- ST-T changes → ischemic substrate
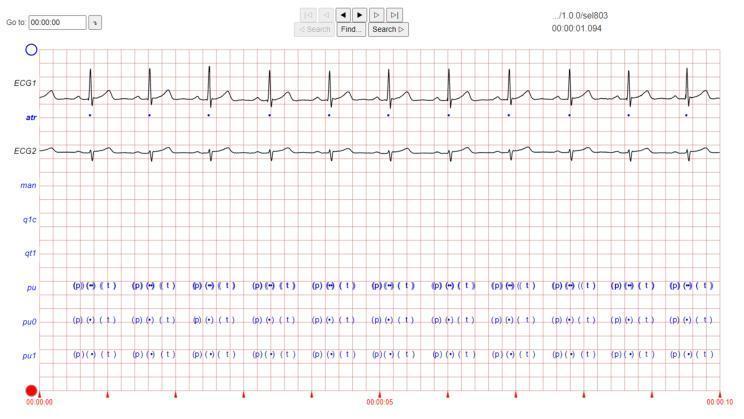
Ambulatory Monitoring
- Holter monitor (24–48 h) — for frequent arrhythmias
- Event recorder / loop recorder — for infrequent paroxysmal events
- Implantable loop recorder (ILR) — for cryptogenic syncope, long-term monitoring
- Smartwatch/wearable — emerging tool; validated for AF detection (Apple Heart Study)
Electrophysiology Study (EPS)
- Invasive catheter-based mapping of intracardiac electrograms (A, H, V)
- Distinguishes site of AV block (AV node vs. His-Purkinje)
- Assesses inducibility of VT, identifies mechanism (reentry vs. triggered)
- Guides radiofrequency (RF) catheter ablation
Additional Studies
- Echocardiogram — structural substrate (EF, wall motion, LVH, ARVC)
- Cardiac MRI — fibrosis (late gadolinium enhancement) → reentrant VT substrate
- Stress testing — CPVT, catecholaminergic VT, ischemia-related arrhythmias
- Tilt-table test — neurally mediated (vasovagal) syncope
- Carotid sinus massage — carotid sinus hypersensitivity
- Labs — electrolytes (K⁺, Mg²⁺, Ca²⁺), thyroid function, drug levels
AV Block Localization Clues
- Type I (Wenckebach): response to vagal stimulation/atropine → suggests AV nodal site; generally benign
- Type II (Mobitz): carotid sinus massage improves, atropine worsens → suggests His-Purkinje site; more ominous, higher risk of progression to complete block
- Very long PR intervals (>200 ms) are more likely from AV nodal delay
7. Treatment
Pharmacologic — Antiarrhythmic Drugs (AADs)
The Vaughan Williams classification remains the standard framework:
| Class | Mechanism | Agents | Key Uses |
|---|---|---|---|
| 0 | HCN (I_f) channel blocker | Ivabradine | Inappropriate sinus tachycardia, heart failure |
| IA | Na⁺ channel block (↓V_max, ↑APD) | Quinidine, Procainamide, Disopyramide | AF, VT |
| IB | Na⁺ channel block (minimal ↑APD) | Lidocaine, Mexiletine | Ventricular arrhythmias, post-MI |
| IC | Strong Na⁺ channel block (no APD change) | Flecainide, Propafenone | AF, SVT (avoid in structural heart disease) |
| II | Beta-adrenoceptor blockade | Metoprolol, Atenolol, Carvedilol | Rate control in AF, VT storm, CPVT |
| III | K⁺ channel block (↑APD, ↑refractoriness) | Amiodarone, Sotalol, Dronedarone, Ibutilide, Dofetilide | AF, VT/VF |
| IV | L-type Ca²⁺ channel block | Verapamil, Diltiazem | Rate control AF, AVNRT, AVRT |
| V–VII | Mechanosensitive channels, gap junctions, upstream targets | Investigational | — |
A modified Vaughan Williams classification (2018+) encompasses classes 0–VII including connexin modulators and upstream targets (atrial structural remodeling). No new agents have been FDA-approved in the US since dronedarone (2009).
Key AAD principles:
- Drug effects depend on tissue type, heart rate (use-dependence), membrane potential, autonomic tone, genetics, and age
- Reverse use dependence (class III agents): QT prolongation is greater at slow rates → TdP risk
- AADs suppress arrhythmias by: (a) reducing automatic pacemaker rate, (b) eliminating afterdepolarizations, or (c) converting unidirectional block to bidirectional block or increasing conduction velocity to eliminate reentry
Non-Pharmacologic
Cardioversion / Defibrillation
- Electrical cardioversion (DC): synchronized shock for AF, flutter, hemodynamically unstable VT
- Defibrillation: unsynchronized shock for VF/pulseless VT
- Chemical cardioversion: ibutilide (IV) or dofetilide for AF/flutter
Cardiac Pacing
- Temporary pacing: hemodynamically significant bradycardia, post-arrest bradycardia, complete AV block
- Permanent pacemaker (PPM): SSS, symptomatic bradycardia, Mobitz II or third-degree AV block, chronotropic incompetence
- Atropine: 0.5 mg IV initially for acute sinus bradycardia; ineffective for His-Purkinje block
- Cardiac resynchronization therapy (CRT): HF with LBBB and reduced EF
Implantable Cardioverter-Defibrillator (ICD)
- Primary prevention: EF ≤35% despite optimal therapy (NYHA II–III)
- Secondary prevention: survivors of VF/hemodynamically unstable VT
- Delivers anti-tachycardia pacing (ATP) and/or high-energy shocks
- ICD with CRT (CRT-D) for HF with ventricular dyssynchrony
Catheter Ablation (Radiofrequency / Cryoablation)
- AVNRT / AVRT / WPW: success rate ~95%; first-line in symptomatic patients
- Atrial flutter: isthmus ablation, >95% success
- AF: pulmonary vein isolation (PVI); increasingly first-line in paroxysmal AF
- Idiopathic VT (structurally normal heart): ~85% success
- Post-infarction VT: >70% free from recurrence; guided by 3D electroanatomic mapping (CARTO, EnSite NavX)
- Complications (up to 3%): vascular injury, heart block, tamponade, stroke, valve damage
Surgical
- Maze procedure (surgical AF ablation)
- Left cardiac sympathetic denervation (LCSD) for refractory CPVT/LQTS
- Left atrial appendage occlusion (WATCHMAN) for AF + CHA₂DS₂-VASc ≥ 2 with anticoagulation contraindication
Specific Arrhythmia Syndromes — Targeted Management
| Arrhythmia | First-Line Treatment |
|---|---|
| Sinus bradycardia (asymptomatic) | None |
| Sinus bradycardia (symptomatic) | Atropine IV → PPM |
| AF (rate control) | Beta-blocker or CCB (diltiazem/verapamil) |
| AF (rhythm control) | Flecainide/propafenone (no SHD) or amiodarone; PVI ablation |
| AVNRT | Vagal maneuvers → adenosine IV; ablation for recurrent cases |
| WPW / AVRT | Avoid AV nodal blockers in pre-excited AF; ablation curative |
| Monomorphic VT (stable) | Amiodarone IV, procainamide IV; ablation |
| VF / Unstable VT | Immediate defibrillation; ACLS protocol |
| Torsades de pointes | IV Mg²⁺ sulfate, correct electrolytes, overdrive pacing; discontinue offending drugs |
| Complete AV block | Temporary then permanent pacemaker |
| LQTS/CPVT | Beta-blockers; ICD; LCSD if refractory |
Summary
Arrhythmias encompass a broad spectrum of disorders unified by disrupted cardiac impulse formation or conduction. The cornerstone of workup is the 12-lead ECG, supplemented by ambulatory monitoring and invasive EPS where indicated. Treatment is directed at the arrhythmia mechanism — pharmacologic (Vaughan Williams classes 0–VII), electrical (cardioversion, defibrillation, pacing), or interventional (catheter ablation, ICD) — with the goal of restoring or maintaining hemodynamic stability and preventing sudden cardiac death.
Sources: Braunwald's Heart Disease, 12th Edition (Chapters 62, 64, 68); Fuster and Hurst's The Heart, 15th Edition (Chapter 34).
This is a shared conversation. Sign in to Orris to start your own chat.