what viva can be asked check in detailed nd give it with answers
Reading File
Finding Sources
Finding Sources
Finding Sources
The library doesn't have specific physiotherapy textbooks. I'll now provide a comprehensive viva Q&A from my own expert knowledge covering all the topics in your BPT syllabus image.
BPT Viva Questions & Answers
Obstetrics, Gynaecology & Paediatric Physiotherapy
PART A — OBSTETRICS & GYNAECOLOGY PHYSIOTHERAPY
🔹 TOPIC 1: Treatment of Incontinence & Pelvic Floor Dysfunction
Q1. What is stress urinary incontinence (SUI)?
A: Involuntary leakage of urine on effort, exertion, sneezing, or coughing due to increased intra-abdominal pressure in the absence of detrusor contraction. It occurs due to weakness of the urethral sphincter and pelvic floor muscles.
Q2. What is the difference between stress, urge, and mixed urinary incontinence?
A:
- Stress incontinence – leakage with physical exertion (weak sphincter/pelvic floor)
- Urge incontinence – sudden, strong urge to void followed by leakage (detrusor overactivity)
- Mixed incontinence – combination of both
Q3. What are Kegel exercises? How are they performed?
A: Kegel exercises are voluntary contractions of the pelvic floor muscles (levator ani group). Technique:
- Patient contracts pelvic floor as if stopping urine flow
- Hold for 5–10 seconds, then relax
- Perform 10–15 repetitions, 3 sets/day
- Both fast (quick flicks) and slow sustained contractions are included
Q4. What is pelvic floor dysfunction?
A: A broad term encompassing conditions caused by weakened, overactive, or poorly coordinated pelvic floor muscles — including incontinence, pelvic organ prolapse, pelvic pain, and dyspareunia.
Q5. What are the layers of the pelvic floor?
A:
- Endopelvic fascia – deepest supportive layer
- Levator ani muscle group – pubococcygeus, iliococcygeus, puborectalis
- Coccygeus muscle
- Perineal membrane (urogenital diaphragm)
- Superficial perineal muscles – ischiocavernosus, bulbospongiosus, superficial transverse perinei
Q6. What physiotherapy modalities are used for pelvic floor dysfunction?
A:
- Kegel / PFMT (Pelvic Floor Muscle Training)
- Biofeedback
- Electrical stimulation (NMES / TENS)
- Bladder retraining
- Vaginal cones
- Behavioural modification and fluid management
🔹 TOPIC 2: Postnatal Physiotherapy Management
Q7. What postnatal complications does physiotherapy address?
A:
- Bladder incontinence
- Bowel incontinence / constipation
- Pelvic floor muscle weakness
- Postpartum depression
- Low back pain
- Diastasis recti
- Perineal pain / episiotomy healing
- Deep vein thrombosis prevention
Q8. When is postnatal physiotherapy started?
A:
- Pelvic floor exercises begin within 24 hours of delivery (vaginal or caesarean)
- Gentle walking and breathing exercises start from day 1
- Core strengthening (transversus abdominis) can begin after 6–8 weeks post-delivery
- Full exercise resumption after 12 weeks, depending on healing
Q9. What is diastasis recti and how is it managed by physiotherapy?
A: Diastasis recti is the separation (>2–2.5 cm) of the two rectus abdominis bellies along the linea alba due to stretching in pregnancy.
- Managed by transversus abdominis activation
- Avoid sit-ups, crunches, and heavy lifting initially
- Abdominal splinting, gentle progressive core strengthening
Q10. How does physiotherapy help postnatal depression?
A:
- Aerobic exercise increases serotonin and endorphins
- Group-based exercises improve social support
- Yoga and relaxation techniques reduce cortisol
- Breathing exercises reduce anxiety
🔹 TOPIC 3: Electrotherapy Modalities for Pelvic Floor
Q11. What is Neuromuscular Electrical Stimulation (NMES) and how is it used in pelvic floor rehabilitation?
A: NMES uses electrical current to stimulate motor nerves, causing involuntary pelvic floor muscle contractions in patients unable to voluntarily contract.
- Frequency: 35–50 Hz for stress incontinence (muscle strengthening)
- Frequency: 5–10 Hz for urge incontinence (detrusor inhibition)
- Applied via intravaginal/intrarectal probe or surface electrodes
- Improves muscle tone and sphincter activity
Q12. What is the role of TENS in pelvic floor dysfunction?
A: TENS (Transcutaneous Electrical Nerve Stimulation) at low frequencies inhibits detrusor overactivity and reduces urgency. It works via the pudendal nerve reflex arc to suppress involuntary bladder contractions.
Q13. What is interferential therapy (IFT) in pelvic floor rehabilitation?
A: IFT uses two medium-frequency AC currents that interfere to produce a low-frequency beat frequency deep in tissues. Used for:
- Detrusor muscle inhibition
- Pelvic pain relief
- Improved blood circulation in perineal region
Q14. What are the contraindications of electrotherapy in the pelvic floor?
A:
- Pregnancy
- Cardiac pacemaker
- Active infection or UTI
- Malignancy in the region
- Prolapse (Grade III/IV)
- Sensory impairment in the area
🔹 TOPIC 4: Therapeutic Electrical Stimulation & Biofeedback
Q15. What is biofeedback and how is it used in pelvic floor therapy?
A: Biofeedback converts physiological signals (muscle EMG or pressure) into visual/auditory feedback so the patient can learn to consciously control pelvic floor muscle activity.
- Types: EMG biofeedback (muscle electrical activity) and manometric biofeedback (pressure)
- Helps patients identify correct muscles, improve coordination, and increase strength
- Especially useful when voluntary contraction is poor
Q16. What is the difference between biofeedback and electrical stimulation?
A:
| Feature | Biofeedback | Electrical Stimulation |
|---|---|---|
| Principle | Teaches voluntary control | Causes involuntary contraction |
| Patient participation | Active | Passive |
| Used when | Patient can identify muscles | Patient cannot contract muscles |
| Feedback | Visual/auditory | None |
Q17. What is vaginal manometry?
A: A pressure-based measurement technique using a vaginal probe to assess pelvic floor muscle strength (squeeze pressure in cmH₂O). Used to quantify baseline strength and monitor progress.
🔹 TOPIC 5: Osteoporosis — Prevention & Physiotherapy
Q18. Define osteoporosis and state its WHO diagnostic criterion.
A: Osteoporosis is a metabolic bone disease characterized by reduced bone mineral density (BMD) and microarchitectural deterioration, leading to increased fracture risk.
- WHO criterion: T-score ≤ −2.5 on DEXA scan
- Osteopenia: T-score between −1.0 and −2.5
Q19. What are the physiotherapy goals in osteoporosis?
A:
- Prevent further bone loss through weight-bearing exercise
- Improve muscle strength (especially back extensors, hip abductors)
- Improve balance and reduce fall risk
- Correct posture (reduce thoracic kyphosis)
- Pain management
- Patient education
Q20. What type of exercises are recommended in osteoporosis?
A:
- Weight-bearing aerobic – walking, low-impact aerobics, dancing
- Resistance training – progressive strengthening of back extensors and hips
- Balance training – Tai Chi, single-leg stance
- Postural exercises – thoracic extension, chin tucks
- AVOID – high-impact, spinal flexion exercises (forward bending), twisting
Q21. What precautions must a physiotherapist take while treating osteoporotic patients?
A:
- Avoid spinal flexion (increases vertebral fracture risk)
- No high-impact activities
- Monitor fall risk (use fall prevention protocols)
- Ensure adequate footwear and environment modification
- Work in conjunction with medical management (calcium, vitamin D, bisphosphonates)
🔹 TOPIC 6: Breast Cancer Rehabilitation & Lymphedema after Mastectomy
Q22. What is lymphedema and why does it occur after mastectomy?
A: Lymphedema is the accumulation of protein-rich fluid in tissues due to impaired lymphatic drainage. After mastectomy with axillary lymph node dissection (ALND) or radiation, the lymphatic channels are disrupted, causing upper limb lymphedema.
Q23. What are the four stages of lymphedema?
A:
- Stage 0 (Latent) – No visible swelling, subclinical damage
- Stage I (Reversible) – Pitting edema, reduces with elevation
- Stage II (Irreversible) – Non-pitting edema, fibrosis begins
- Stage III (Elephantiasis) – Severe, skin changes, fibrosis
Q24. What is Complete Decongestive Therapy (CDT)?
A: CDT is the gold standard for lymphedema management, consisting of:
- Manual Lymphatic Drainage (MLD) – gentle massage to redirect lymph to functioning vessels
- Compression bandaging – multi-layer short-stretch bandages
- Therapeutic exercises – active movement with compression
- Skin & nail care – hygiene to prevent infection
Q25. What is the role of exercise after mastectomy?
A:
- Prevent shoulder contracture and frozen shoulder
- Restore shoulder range of motion (pendulum, pulley, wall-climbing exercises)
- Reduce lymphedema risk
- Improve upper limb function and strength
- Psychosocial benefit — improves quality of life and reduces fatigue
Q26. What precautions are taken in breast cancer rehabilitation?
A:
- Avoid blood pressure measurements on the affected arm
- No venepuncture or IV lines on affected side
- Avoid tight clothing or jewellery on affected arm
- Protect from cuts/infections (risk of cellulitis)
- Avoid heavy lifting initially
🔹 TOPIC 7: Physiotherapy after Gynaecological Surgeries
Q27. What surgeries require post-operative physiotherapy in gynaecology?
A:
- Hysterectomy (abdominal/vaginal/laparoscopic)
- Prolapse repair (anterior/posterior colporrhaphy)
- Incontinence procedures (TVT, TOT slings)
- Myomectomy
- Pelvic floor repair surgeries
Q28. What is the physiotherapy protocol after a hysterectomy?
A:
- Day 1–2: Breathing exercises (ACBT), ankle pumps, bed mobility, early ambulation
- Week 1–4: Pelvic floor exercises, gentle walking, posture correction
- Week 4–6: Progressive core strengthening (transversus abdominis)
- After 6–8 weeks: Gradual return to full activity
- Avoid: Heavy lifting, high-impact activity for 3 months
PART B — PAEDIATRIC PHYSIOTHERAPY
🔹 TOPIC 8: Developmental Milestones
Q29. State the major gross motor developmental milestones.
A:
| Age | Milestone |
|---|---|
| 1 month | Lifts head briefly in prone |
| 3 months | Head control in prone, social smile |
| 5 months | Rolls prone to supine |
| 6 months | Sits with support |
| 9 months | Stands with support, creeps |
| 12 months | Walks independently |
| 18 months | Runs, climbs stairs with support |
| 2 years | Runs well, up-down stairs |
| 3 years | Rides tricycle, stands on one foot |
Q30. What are primitive reflexes and developmental reflexes? Give examples.
A:
- Primitive reflexes – Present at birth, disappear by 4–6 months. Persistence = CNS pathology.
- Moro reflex (disappears ~4 months)
- Rooting reflex (~4 months)
- Palmar grasp (~6 months)
- ATNR – Asymmetric Tonic Neck Reflex (~6 months)
- STNR – Symmetric Tonic Neck Reflex (~8–10 months)
- Stepping reflex (~2 months)
- Postural/righting reflexes – Emerge as primitive reflexes disappear (head righting, parachute reaction — appears ~8–9 months)
Q31. What is the ATNR and its clinical significance?
A: ATNR (Asymmetric Tonic Neck Reflex) — When the head is turned to one side, the limbs on the face side extend and the limbs on the skull side flex ("fencer posture"). Normally disappears by 6 months. Persistence in cerebral palsy interferes with midline hand use and feeding.
🔹 TOPIC 9: Cerebral Palsy (CP)
Q32. Define cerebral palsy.
A: Cerebral palsy is a group of permanent, non-progressive disorders of movement and posture, caused by an injury or malformation in the developing fetal or infant brain, often accompanied by disturbances of sensation, cognition, communication, perception, and behaviour.
Q33. What are the types of cerebral palsy?
A:
- Spastic CP (most common, ~75%) – Upper motor neuron lesion, hypertonicity, clasp-knife rigidity
- Hemiplegia, Diplegia, Quadriplegia/Tetraplegia
- Dyskinetic/Athetoid CP – Basal ganglia lesion, involuntary movements
- Ataxic CP – Cerebellar lesion, incoordination, balance problems
- Mixed type
Q34. What is NDT (Neurodevelopmental Therapy)? Who developed it?
A: NDT was developed by Karel and Bertha Bobath in the 1940s. It focuses on:
- Inhibition of abnormal tonal patterns and primitive reflexes
- Facilitation of normal postural reactions and movement patterns
- Handling techniques to promote quality of movement
- Used primarily in CP, stroke, and developmental disorders
Q35. What is Vojta therapy?
A: Developed by Václav Vojta, this neurophysiological technique activates innate locomotor patterns (reflex creeping and reflex rolling) through specific pressure points on the body.
- Stimulates the CNS to produce coordinated movement patterns
- Used in infants at risk (preterm, birth asphyxia) and children with CP
- Works by activating the spinal cord locomotor centres
Q36. What is Constraint-Induced Movement Therapy (CIMT)?
A: CIMT involves restraining the unaffected (stronger) limb to force use of the affected (weaker) limb in children with hemiplegic CP.
- Encourages cortical reorganization (neuroplasticity)
- Constraint worn for 6+ hours/day
- Intensive task-specific training of the affected limb
- Evidence shows improved hand function in hemiplegic CP
Q37. What is Sensory Integration (SI) therapy?
A: Developed by A. Jean Ayres, SI therapy addresses the brain's ability to organize and process sensory information (tactile, vestibular, proprioceptive) to produce adaptive responses.
- Used in children with autism, developmental coordination disorder, sensory processing disorder
- Activities include swings, balance boards, textured surfaces, deep pressure
🔹 TOPIC 10: Down Syndrome
Q38. What is Down syndrome and its cause?
A: Trisomy 21 — presence of an extra chromosome 21 (total 47 chromosomes). Most common chromosomal disorder. Caused by non-disjunction during meiosis, translocation, or mosaicism.
Q39. What are the physiotherapy concerns in Down syndrome?
A:
- Hypotonia (low muscle tone) — primary physiotherapy concern
- Joint hypermobility and ligament laxity
- Atlantoaxial instability (C1–C2) — must be screened before exercise
- Delayed motor milestones
- Feeding difficulties
- Obesity risk
- Congenital heart disease (in ~40%)
Q40. What physiotherapy interventions are used in Down syndrome?
A:
- Strengthening and tone-building exercises
- Postural control and balance training
- Developmental milestone facilitation (NDT approach)
- Hydrotherapy
- Sensory integration
- Oral motor therapy for feeding
- Orthotics if needed (flat feet, genu valgum)
🔹 TOPIC 11: Autism Spectrum Disorder (ASD)
Q41. What is the role of physiotherapy in autism?
A:
- Improve motor coordination and praxis
- Sensory integration therapy (tactile, vestibular, proprioceptive input)
- Reduce stereotyped motor behaviors
- Improve social participation through play-based therapy
- Aquatic therapy for sensory modulation
- CIMT if motor asymmetry present
🔹 TOPIC 12: Spina Bifida
Q42. What is spina bifida and its types?
A: Spina bifida is a neural tube defect with incomplete closure of the vertebral arch.
- Spina bifida occulta – Bony defect only, cord intact, usually asymptomatic
- Meningocele – Meninges protrude, cord intact, mild neurological deficit
- Myelomeningocele – Most severe; cord and meninges protrude, significant neurological deficit (paralysis, incontinence)
Q43. What is the physiotherapy role in myelomeningocele?
A:
- Prevent deformity (hip dislocation, clubfoot, scoliosis)
- Strengthen remaining functional muscles
- Mobility aids (orthotics, wheelchairs, crutches)
- Bladder/bowel program (in coordination with team)
- Pressure ulcer prevention
- Family and caregiver education
🔹 TOPIC 13: Hydrocephalus
Q44. What is hydrocephalus and its relevance to paediatric physiotherapy?
A: Accumulation of CSF in the cerebral ventricles, causing increased intracranial pressure and head enlargement. Associated with:
- Motor delays, spasticity, visual problems
- Often co-exists with myelomeningocele
- Managed medically with VP shunt (ventriculoperitoneal shunt)
- Physiotherapy: developmental facilitation, postural control, caution regarding shunt function
🔹 TOPIC 14: Early Intervention
Q45. What is early intervention and why is it important?
A: Early intervention refers to therapeutic services provided to infants and toddlers (0–3 years) at risk of or diagnosed with developmental delays/disabilities.
- Rationale: Brain plasticity is greatest in early years; early stimulation maximizes functional outcomes
- Includes physiotherapy, occupational therapy, speech therapy, and family education
- Programs target motor, cognitive, communication, and social development
Q46. What tools are used for developmental screening in paediatrics?
A:
- Denver Developmental Screening Test (DDST II) — ages 0–6 years, screens gross motor, fine motor, language, social
- Bayley Scales of Infant Development (BSID III) — comprehensive assessment
- Gross Motor Function Classification System (GMFCS) — classifies CP severity (I–V)
- Hammersmith Infant Neurological Examination (HINE) — for infants
- Peabody Developmental Motor Scales (PDMS-2) — motor skills 0–5 years
🔹 TOPIC 15: Neurophysiological Approaches Summary
Q47. Compare NDT, Vojta, and Sensory Integration approaches.
A:
| Feature | NDT (Bobath) | Vojta | Sensory Integration (Ayres) |
|---|---|---|---|
| Developer | Karel & Bertha Bobath | Václav Vojta | A. Jean Ayres |
| Mechanism | Inhibit abnormal patterns, facilitate normal movement | Activate innate locomotor patterns via pressure points | Organize sensory input for adaptive response |
| Age group | All ages | Mainly infants | Children, esp. ASD |
| Handling | Therapist-guided | Specific pressure point stimulation | Sensory-rich environment |
| Primary use | CP, stroke | At-risk infants, CP | ASD, sensory processing disorder |
🔹 QUICK-FIRE VIVA QUESTIONS
Q: What nerve supplies the pelvic floor? → Pudendal nerve (S2, S3, S4)
Q: What is the T-score for osteoporosis? → T-score ≤ −2.5 on DEXA
Q: When does the Moro reflex disappear? → By 4 months
Q: What is the most common type of cerebral palsy? → Spastic (75%)
Q: What is GMFCS? → Gross Motor Function Classification System — 5 levels classifying motor function in cerebral palsy
Q: What chromosome is affected in Down syndrome? → Chromosome 21 (Trisomy 21)
Q: What is the gold standard for lymphedema? → Complete Decongestive Therapy (CDT)
Q: Name the muscles of levator ani. → Pubococcygeus, iliococcygeus, puborectalis
Q: What frequency of NMES is used for stress incontinence? → 35–50 Hz
Q: What is the parachute reaction? → Protective extension of arms when the child is tilted forward; appears at ~8–9 months; absent in CP
Q: What is CIMT? → Constraint-Induced Movement Therapy — restraining stronger limb to force use of weaker limb
Q: What precaution is essential in Down syndrome before vigorous exercise? → Screen for atlantoaxial instability (risk of spinal cord injury)
This covers all the topics listed in your BPT syllabus image in a viva-ready format. Let me know if you want any topic expanded further or want MCQ-format questions on any section!
i want only peadistric in depth questions
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Excellent — rich content from Bradley and Daroff's Neurology. Now I have all I need to compile a deeply detailed, textbook-backed viva set.
🧒 PAEDIATRIC PHYSIOTHERAPY — IN-DEPTH VIVA Q&A
BPT Examination Preparation (All Syllabus Topics Covered)
SECTION 1: PAEDIATRIC NEUROLOGY & DEVELOPMENTAL MILESTONES
Q1. What is paediatric neurology from a physiotherapy perspective?
A: Paediatric neurology deals with neurological conditions affecting infants and children — including disorders of movement, posture, tone, reflexes, coordination, and development. From a physiotherapy standpoint, it involves:
- Assessment of neuromotor function
- Identification of abnormal tone, reflexes, and movement patterns
- Facilitating normal developmental progression
- Managing conditions like CP, spina bifida, Down syndrome, hydrocephalus
Q2. What are developmental milestones? Why are they important in physiotherapy?
A: Developmental milestones are age-specific skills that most children achieve within a predictable time window, reflecting progressive maturation of the CNS.
Importance in physiotherapy:
- Help identify developmental delay early
- Guide goal setting in rehabilitation
- Assist in monitoring treatment progress
- Form the basis of developmental facilitation programs
Key domains assessed:
- Gross motor
- Fine motor / adaptive
- Language / communication
- Personal-social
Q3. State all major gross motor milestones with ages.
A:
| Age | Gross Motor Milestone |
|---|---|
| 1 month | Lifts chin in prone |
| 3 months | Head control in prone on elbows, no head lag |
| 5 months | Rolls prone to supine |
| 6 months | Sits with support, rolls both ways |
| 8–9 months | Sits independently, crawls |
| 9–10 months | Pulls to stand, cruises along furniture |
| 12 months | Walks independently (range: 9–15 months) |
| 15 months | Walks well, stoops and recovers |
| 18 months | Runs (stiff), climbs stairs with support |
| 2 years | Runs well, up and down stairs, kicks ball |
| 3 years | Stands on one foot, rides tricycle |
| 4 years | Hops on one foot, skips |
| 5 years | Skips on alternate feet, balances on one foot for 10 seconds |
Q4. What are primitive reflexes? Name them and state when they disappear.
A: Primitive reflexes are automatic, involuntary movements present at birth controlled by the brainstem and spinal cord. As the cortex matures, they become integrated (suppressed). Persistence beyond expected age = CNS pathology (e.g., cerebral palsy).
| Reflex | Appears | Disappears |
|---|---|---|
| Moro reflex | Birth | 4–5 months |
| Rooting reflex | Birth | 4 months |
| Sucking reflex | Birth | 4 months |
| Palmar grasp | Birth | 5–6 months |
| Plantar grasp | Birth | 9–10 months |
| ATNR (Asymmetric Tonic Neck Reflex) | Birth | 5–6 months |
| STNR (Symmetric Tonic Neck Reflex) | 4–6 months | 8–10 months |
| TLR (Tonic Labyrinthine Reflex) | Birth | 6 months |
| Stepping/walking reflex | Birth | 2–3 months |
| Parachute reaction | 8–9 months | Persists for life |
Q5. Describe the ATNR and its clinical significance.
A: ATNR = Asymmetric Tonic Neck Reflex ("Fencer Posture")
- Stimulus: Turning the head to one side
- Response: Limbs on the face side extend, limbs on the skull side flex
- Normal disappearance: 5–6 months
Clinical significance:
- Persistence beyond 6 months → sign of cerebral palsy
- Interferes with midline hand use (bimanual tasks), feeding, and hand-to-mouth activity
- Child cannot look at what they are holding
- Affects rolling and early locomotion
Q6. Describe the Moro reflex and its clinical significance.
A: The Moro (startle) reflex is elicited by a sudden drop of the head or loud sound.
- Response: Arms abduct and extend (Phase 1), then adduct and flex as if embracing (Phase 2)
- Normal disappearance: 4–5 months
- Absent Moro at birth → bilateral brachial plexus injury, severe hypotonia, or birth asphyxia
- Asymmetric Moro → unilateral brachial plexus injury (Erb's palsy) or hemiplegia
- Persistent Moro beyond 5 months → cerebral palsy
Q7. What is the STNR and how does it affect development?
A: STNR = Symmetric Tonic Neck Reflex
- Stimulus: Neck flexion or extension
- Neck flexion → arms flex, legs extend
- Neck extension → arms extend, legs flex
Clinical significance:
- Normally integrates by 8–10 months
- Persistence prevents reciprocal crawling on hands and knees
- Children may "bunny hop" or W-sit instead
- A sign of abnormal neurological development
Q8. What is the Tonic Labyrinthine Reflex (TLR) and its significance?
A:
- Mediated by the labyrinth (otolith organs)
- Supine position → extensor tone increases (opisthotonus-like)
- Prone position → flexor tone increases
- Normal disappearance: ~6 months
- Persistence → child cannot lift head in prone, cannot come to sitting, increased extensor spasticity in supine (common in spastic CP)
Q9. What are postural reactions and when do they appear?
A: Postural reactions are automatic responses that maintain body alignment and equilibrium as the cortex matures and replaces primitive reflexes.
| Reaction | Age of Appearance |
|---|---|
| Head righting (labyrinthine) | 2 months |
| Body righting | 4–6 months |
| Landau reflex | 3–4 months (disappears ~2 years) |
| Protective extension (forwards) | 6–7 months |
| Protective extension (sideways) | 7–8 months |
| Protective extension (backwards) | 9–10 months |
| Equilibrium reactions (prone) | 6 months |
| Equilibrium reactions (sitting) | 7–8 months |
| Equilibrium reactions (standing) | 12–18 months |
Q10. What is the Landau reflex?
A: When the infant is held in horizontal suspension (prone in the air), the head and legs extend — the body forms an arc. If the head is then forcibly flexed, the legs and hips also flex. Appears at 3–4 months, disappears by 2–2.5 years. Absent in hypotonic infants (floppy baby).
SECTION 2: ASSESSMENT IN PAEDIATRIC PHYSIOTHERAPY
Q11. What are the components of paediatric physiotherapy assessment?
A:
- History – Birth history, APGAR, gestational age, prenatal/perinatal insults, developmental history, family history
- Observation – Posture, spontaneous movement, symmetry, head control, play
- Palpation – Muscle tone, muscle bulk, joint range
- Milestone examination – Gross motor, fine motor, speech, social
- Developmental reflex examination – Primitive and postural reflexes
- Higher mental functions – Cognition, attention, behavior
- Cranial nerve examination – Facial symmetry, eye movements, swallowing
- Motor & Sensory examination – Tone, power, coordination, sensation
- Reflex testing – Tendon reflexes (hyporeflexia / hyperreflexia), Babinski
- Differential diagnosis – Based on findings
- Balance & Coordination examination – Romberg, tandem walking
- Gait analysis – Scissor gait, toe walking, Trendelenburg
- Functional analysis – ADL performance, transfers, mobility
Q12. What is the GMFCS and how is it used?
A: Gross Motor Function Classification System (GMFCS) classifies the severity of motor function in children with cerebral palsy across 5 levels:
| Level | Description |
|---|---|
| I | Walks without restrictions; limitations in advanced gross motor skills |
| II | Walks with limitations (uneven surfaces, inclines, crowds) |
| III | Walks with assistive mobility device indoors; wheelchair outdoors |
| IV | Self-mobility limited; transported or uses powered wheelchair |
| V | Transported in manual wheelchair; minimal voluntary control |
Age bands: < 2 years, 2–4 years, 4–6 years, 6–12 years, 12–18 years
Use: Sets realistic goals, guides intervention intensity, predicts outcomes
Q13. What tools are used for developmental screening?
A:
| Tool | Age Range | What It Assesses |
|---|---|---|
| Denver DDST-II | 0–6 years | Gross motor, fine motor, language, personal-social |
| Bayley Scales (BSID-III) | 0–42 months | Motor, cognitive, language, social-emotional |
| Peabody Developmental Motor Scales (PDMS-2) | 0–5 years | Gross and fine motor in detail |
| Hammersmith Infant Neurological Exam (HINE) | 2–24 months | Neurological function in at-risk infants |
| Alberta Infant Motor Scale (AIMS) | 0–18 months | Gross motor from birth to independent walking |
| Gross Motor Function Measure (GMFM) | CP children | Outcome measure for CP rehabilitation (88 or 66 items) |
Q14. What is gait analysis in paediatrics and what abnormal patterns are seen?
A: Gait analysis evaluates the child's walking pattern — stride length, cadence, joint angles, and muscle activity.
Abnormal gait patterns:
- Scissor gait – Hip adduction + internal rotation (spastic diplegia in CP)
- Toe walking (equinus gait) – Plantarflexion, no heel strike (spastic CP, idiopathic toe walking)
- Trendelenburg gait – Pelvis drops on unaffected side (hip abductor weakness — MMC, CDH)
- Crouch gait – Excessive knee and hip flexion (CP)
- Steppage gait – High stepping due to foot drop (peripheral nerve problem)
- Hemiplegic gait – Circumduction of affected leg (CP hemiplegia)
SECTION 3: CEREBRAL PALSY (CP)
Q15. Give the current definition of cerebral palsy.
A: Cerebral palsy is defined as "a group of permanent disorders of the development of movement and posture, causing activity limitation, that are attributed to non-progressive disturbances that occurred in the developing fetal or infant brain."
(Rosenbaum et al., 2007 — International Consensus Panel)
To diagnose CP, ALL of the following must be present:
- Disorder of movement and posture (onset before 1–2 years of age)
- Evidence of disturbance in the fetal or infant brain
- Non-progressive (no evidence of worsening)
- Significant functional limitation
- Expected to persist throughout life
Although non-progressive, CP should be viewed as a dynamic disorder — its clinical expression evolves with growth and development. — Bradley and Daroff's Neurology in Clinical Practice
Q16. What is the incidence of cerebral palsy?
A: Approximately 2–3 per 1000 live births in developed countries. Spastic CP accounts for ~80% of all cases; extrapyramidal forms make up ~20% (15% dyskinetic, 5% ataxic).
Q17. What are the causes (etiology) of cerebral palsy?
A:
Prenatal (most common — ~80%):
- Periventricular leukomalacia (PVL) in preterm infants
- Congenital brain malformations
- Intrauterine infections (TORCH)
- Genetic/chromosomal disorders
- Maternal vascular disease
Perinatal (~10%):
- Hypoxic-ischaemic encephalopathy (HIE) — birth asphyxia
- Neonatal stroke
- Prematurity, very low birth weight
Postnatal (~10%):
- Meningitis/encephalitis
- Traumatic brain injury (shaken baby)
- Prolonged seizures / status epilepticus
Q18. Classify cerebral palsy in detail.
A:
By motor type:
| Type | Lesion Site | Features |
|---|---|---|
| Spastic (~80%) | Cortex/corticospinal tract (UMN) | Hypertonicity, hyperreflexia, clasp-knife rigidity, clonus, Babinski positive |
| Dyskinetic/Athetoid (~15%) | Basal ganglia | Involuntary slow writhing (athetosis) or rapid (chorea), fluctuating tone |
| Ataxic (~5%) | Cerebellum | Hypotonia, incoordination, intention tremor, wide-based gait |
| Mixed | Multiple sites | Combination of above |
By topographical distribution (Spastic CP):
| Type | Distribution | Common Cause |
|---|---|---|
| Hemiplegia | One side (arm > leg) | Periventricular infarction, term baby |
| Diplegia | Legs > arms | PVL in preterm babies (most common) |
| Quadriplegia/Tetraplegia | All 4 limbs, severe | Severe HIE, cortical dysgenesis |
| Monoplegia | Single limb | Rare |
Q19. What are the associated impairments in cerebral palsy?
A: CP is NOT just a motor disorder. Associated conditions are extremely common:
- Intellectual disability – 50–60%
- Epilepsy – 25–45%
- Speech and language disorders – 38–60%
- Visual impairment – strabismus, nystagmus, cortical visual impairment
- Hearing impairment – especially in athetoid CP (kernicterus)
- Feeding difficulties/dysphagia – 43–99%
- Behavioural problems – ADHD, autism features
- Sleep disturbance
- Drooling (sialorrhoea)
- Pain (often under-recognized)
Q20. What are the short-term and long-term goals of physiotherapy in CP?
A:
Short-term goals:
- Reduce spasticity and abnormal tone
- Inhibit persistent primitive reflexes
- Facilitate head control, rolling, sitting
- Improve joint range of motion
- Prevent contractures and deformities
- Improve functional mobility and transfers
Long-term goals:
- Maximize independent ambulation
- Maintain musculoskeletal integrity (prevent scoliosis, hip dislocation)
- Achieve age-appropriate ADL function
- Improve quality of life and social participation
- Educate caregivers in handling techniques
Q21. What mechanical complications occur in CP and how does physiotherapy manage them?
A:
| Complication | Cause | Physiotherapy Management |
|---|---|---|
| Hip dislocation | Spastic hip adductors/flexors | Abduction positioning, stretching, orthotics |
| Equinus foot (toe walking) | Spastic gastrocnemius/soleus | Stretching, ankle-foot orthosis (AFO), serial casting |
| Knee flexion contracture | Hamstring spasticity | Stretching, splinting |
| Scoliosis | Asymmetric tone, poor sitting | Postural support, seating systems, trunk strengthening |
| Shoulder internal rotation | Spastic subscapularis | Stretching, strengthening, positioning |
| Wrist/hand deformity | Spastic wrist flexors | Resting splints, functional training |
Q22. What is spasticity and how is it graded?
A: Spasticity is a velocity-dependent increase in tonic stretch reflexes (muscle tone) with exaggerated tendon jerks, resulting from UMN lesion. It is graded by the Modified Ashworth Scale:
| Grade | Description |
|---|---|
| 0 | No increase in tone |
| 1 | Slight increase — catch and release |
| 1+ | Slight increase — catch, then minimal resistance |
| 2 | Marked increase in tone, but limb easily moved |
| 3 | Considerable increase — passive movement difficult |
| 4 | Limb rigid in flexion or extension |
SECTION 4: NDT, VOJTA & NEUROPHYSIOLOGICAL TECHNIQUES
Q23. What is Neurodevelopmental Therapy (NDT / Bobath Concept)?
A: NDT was developed by Karel Bobath (neurologist) and Bertha Bobath (physiotherapist) in London in the 1940s.
Principles:
- The brain has plasticity — it can learn and reorganize
- Abnormal movement patterns are learned and can be changed
- Inhibit abnormal tonal patterns and primitive reflexes
- Facilitate normal postural reactions and movement patterns
- Use specific handling techniques at key points of control (head, shoulder girdle, pelvis)
Key points of control:
- Proximal: head, trunk, shoulder girdle, pelvic girdle
- Distal: hands, feet
Techniques:
- Inhibition – Reflex Inhibiting Postures/Patterns (RIP) to reduce spasticity
- Facilitation – Guide patient through normal movement sequences
- Weight bearing and weight shifting – Promote postural reactions
- Sensory stimulation – Normalize sensory input
Used in: CP, stroke, traumatic brain injury, developmental delay
Q24. What is Vojta Therapy? Explain its principles.
A: Developed by Czech neurologist Václav Vojta in the 1960s.
Principle: Specific pressure point stimulation activates the spinal cord locomotion centres, triggering two innate locomotor patterns:
- Reflex Creeping (Reflex Kriechen) – From the prone position
- Reflex Rolling (Reflex Umdrehen) – From supine and lateral positions
Key concepts:
- These movement patterns are genetically encoded in the CNS
- In children with neurological impairment, normal locomotor patterns are blocked
- Pressure on specific body zones unlocks these patterns
- With repeated activation, the CNS reorganizes and voluntary movement improves
Zones of stimulation (examples):
- Medial epicondyle of humerus
- Lateral third of clavicle
- Heel
- Inside of knee
Used in: At-risk neonates (preterm, birth asphyxia), CP, MMC, scoliosis, spinal cord injury
Advantage over NDT: Can be started in early infancy (even newborns), teaches parents to do home therapy
Q25. What is Constraint-Induced Movement Therapy (CIMT)?
A: CIMT is based on the concept of learned non-use — after brain injury, the child stops using the weaker limb because it is easier to use the stronger one. The weaker limb becomes progressively more neglected.
Principle: By restraining the stronger limb (cast, splint, or mitt), the child is forced to use the weaker limb, driving cortical reorganization.
Protocol:
- Constraint worn for 6+ hours/day on the unaffected limb
- Intensive task-specific training of affected limb simultaneously (2–6 hours/day)
- Duration: typically 2–3 weeks intensive program
Evidence: Strong evidence for improved hand function in hemiplegic CP.
Modified CIMT (mCIMT): Less intense, constraint worn for 2 hours, used for younger children or lower severity.
Q26. What is Sensory Integration (SI) Therapy? Who developed it?
A: Developed by Dr. A. Jean Ayres (occupational therapist and neuroscientist) in the 1970s.
Principle: The brain must receive, organize, and integrate multiple sensory inputs (tactile, vestibular, proprioceptive) to produce adaptive, purposeful responses. When this process is disordered (Sensory Processing Disorder), the child has difficulty with movement, learning, and behaviour.
Three foundational senses in SI:
- Tactile – Touch discrimination
- Vestibular – Balance and spatial orientation (inner ear)
- Proprioceptive – Body position and movement (muscles, joints)
Common SI-based activities:
- Swings (linear and rotary) — vestibular input
- Textured surfaces, vibration — tactile input
- Heavy work (pushing, pulling, carrying) — proprioceptive input
- Balance boards, trampolines
- Brushing protocol (Wilbarger protocol) — deep pressure/tactile
Used in: Autism Spectrum Disorder (ASD), Developmental Coordination Disorder (DCD), Sensory Processing Disorder, ADHD
Q27. Compare NDT, Vojta, and CIMT approaches.
A:
| Feature | NDT (Bobath) | Vojta | CIMT |
|---|---|---|---|
| Developer | Karel & Bertha Bobath | Václav Vojta | Edward Taub |
| Mechanism | Inhibit abnormal patterns, facilitate normal movement | Activate innate locomotor patterns via pressure zones | Force use of weaker limb by restraining stronger limb |
| Age group | All ages, mainly children and adults | Primarily infants (even newborns) | Children with hemiplegia, usually >18 months |
| Child's role | Active (guided by therapist) | Passive (involuntary reflex response) | Active (intensive task practice) |
| Parent involvement | High | Very high (home program) | Moderate |
| Evidence base | Good for tone, handling | Good for at-risk infants | Strongest evidence for hand function in hemiplegia |
| Primary use | All CP types, stroke | At-risk neonates, CP | Hemiplegic CP |
SECTION 5: DEVELOPMENTAL DELAY & EARLY INTERVENTION
Q28. What is developmental delay? Differentiate global and specific developmental delay.
A:
- Developmental Delay – Performance significantly below average (>2 SD) in one or more developmental domains for age
- Specific Developmental Delay – Delay in only ONE domain (e.g., only motor, only language)
- Global Developmental Delay (GDD) – Significant delay in TWO or more developmental domains; used in children <5 years (after 5 years termed Intellectual Disability)
Q29. What is early intervention? Why is the first 3 years critical?
A: Early intervention = therapeutic services for children 0–3 years at risk of or diagnosed with developmental disability.
Why first 3 years are critical:
- Neuroplasticity is at its peak during this period — the brain forms ~1 million new neural connections per second in early infancy
- Myelination progresses rapidly in the first 2 years
- Abnormal sensorimotor experiences entrench abnormal patterns; early correction prevents this
- Early intervention is dramatically more effective than later treatment for outcomes in CP, Down syndrome, autism, and preterm infants
Components of early intervention:
- Physiotherapy (motor development, tone management)
- Occupational therapy (fine motor, feeding, ADL)
- Speech and language therapy
- Special education and family training
- Psychological support
Q30. What is the physiotherapy management of a child with global developmental delay?
A:
- Assessment first — Identify which milestones are delayed and by how much
- SMART goal setting — Short and long-term goals aligned with GMFCS level
- Postural management — Appropriate seating, sleeping positioning
- Developmental milestone facilitation — Progress through head control → sitting → standing → walking
- Handling and movement facilitation (NDT-based)
- Tone management — Stretching, positioning, splinting
- Sensory stimulation — Vestibular, proprioceptive, tactile input
- Family and caregiver training — Home exercise program (HEP)
- Multidisciplinary team approach — Paediatrician, OT, speech therapist, psychologist
SECTION 6: CONDITIONS — DETAILED
Q31. What is Down syndrome? State its physiotherapy assessment and management.
A: Trisomy 21 — extra chromosome 21 (47 chromosomes total). Most common chromosomal disorder (~1 in 700 births). Causes: Non-disjunction (~95%), Translocation (~4%), Mosaicism (~1%).
Key features relevant to physiotherapy:
- Hypotonia — Primary concern; affects all muscles from birth
- Joint hypermobility — Ligamentous laxity
- Atlantoaxial instability — Excess laxity at C1–C2; present in ~15% → must SCREEN before any vigorous exercise (risk of spinal cord injury)
- Delayed motor milestones (walk avg. ~24 months vs. 12 months)
- Flat feet (pes planus), genu valgum
- Congenital heart disease (~40–50%)
- Intellectual disability
- Obesity risk
Physiotherapy management:
- Strengthening exercises to combat hypotonia
- Balance and postural control training
- Gait training and orthotics (AFO for flat feet)
- Developmental milestone facilitation (NDT approach)
- Hydrotherapy — excellent for tone, strength, confidence
- Oral motor therapy for feeding difficulties
- Pre-sport screen for atlantoaxial instability
- Family education and home program
Q32. What is autism spectrum disorder (ASD) and what is the physiotherapy role?
A: ASD is a neurodevelopmental disorder characterized by:
- Impaired social communication and interaction
- Restricted, repetitive behaviours and interests
- Sensory processing differences
Physiotherapy role:
- Sensory integration therapy — Most significant PT contribution; addresses tactile hypersensitivity, vestibular dysfunction, proprioceptive seeking
- Motor coordination training — Children with ASD often have DCD (Developmental Coordination Disorder)
- Aquatic therapy — Calming, excellent for proprioceptive and vestibular input
- CIMT if motor asymmetry is present
- Social play-based therapy — Structured physical play to improve interaction
- Core strengthening — Many children with ASD have core hypotonia
- Manage stereotyped motor behaviors (hand flapping, rocking) with sensory substitution
Q33. What is spina bifida? Classify and explain physiotherapy management.
A:
Classification:
| Type | Features |
|---|---|
| Spina bifida occulta | Bony defect only; spinal cord intact; often asymptomatic; hairy patch/dimple over spine |
| Meningocele | Meninges protrude through defect; cord intact; mild/no neurological deficit |
| Myelomeningocele | Cord AND meninges protrude; most severe; significant paralysis, sensory loss, bladder/bowel dysfunction |
| Rachischisis | Completely open cord; most severe, incompatible with life |
Neurological level determines function:
- L1–L2: Hip flexors intact, no knee extension → needs KAFO, limited ambulation
- L3–L4: Knee extension intact → KAFO or AFO, community ambulation
- L4–L5: Dorsiflexion intact → AFO, functional ambulation
- S1–S2: Near-normal ambulation; mild bladder/bowel issues
Physiotherapy management:
- Prevent deformity — Hip dislocation, knee contractures, clubfoot (serial casting), scoliosis
- Strengthen available muscles — Progressive resistive exercises within neurological capacity
- Mobility — Orthotic prescription (KAFO, AFO), crutches, wheelchair as needed
- Pressure ulcer prevention — Sensation absent below level; regular skin inspection, pressure relief
- Bladder/bowel program — In collaboration with nursing/urology team
- Hydrotherapy — Supports body weight, facilitates movement
- Family education — Handling, positioning, skin care
Q34. What is hydrocephalus and how does it affect paediatric physiotherapy?
A: Hydrocephalus = accumulation of CSF in the cerebral ventricles due to obstruction, impaired absorption, or overproduction → increased intracranial pressure.
Features:
- Enlarged head circumference (macrocephaly)
- Sunset sign (eyes deviated downward)
- Prominent scalp veins
- Irritability, vomiting, bulging fontanelle
Causes in children:
- Aqueductal stenosis (most common congenital cause)
- Post-meningitis
- Intraventricular haemorrhage (in preterm)
- Associated with myelomeningocele (Arnold-Chiari malformation)
Management: VP shunt (Ventriculoperitoneal shunt) insertion
Physiotherapy considerations:
- Delayed motor milestones → developmental facilitation
- Spasticity of lower limbs (spastic diplegia pattern)
- Visual problems — therapist uses large, high-contrast materials
- VP shunt precautions — No neck compression, no contact sports, report any signs of shunt malfunction (vomiting, irritability, headache) immediately
- Positioning to avoid pressure on shunt site
Q35. What is Chorea and what is its physiotherapy management in children?
A: Chorea = rapid, involuntary, irregular, flowing dance-like movements due to basal ganglia dysfunction.
Causes in children:
- Sydenham's chorea (post-streptococcal, rheumatic fever) — most common in children
- Huntington's disease (juvenile form)
- Kernicterus
- Metabolic disorders
Physiotherapy management:
- Stability training — Proximal stabilization exercises
- Coordination and balance training
- Weight and resistance — Proprioceptive input helps dampen involuntary movements
- Adaptive strategies — Weighted utensils, clothing adaptations
- Functional task training — Writing, feeding, dressing
- Speech and swallowing therapy (oropharyngeal chorea)
Q36. What is syringomyelia and its physiotherapy management?
A: Syringomyelia = formation of a fluid-filled cavity (syrinx) within the spinal cord → progressive central cord compression.
Features:
- Cape-like dissociated sensory loss (pain/temperature lost, touch preserved) — "cape distribution"
- UMN signs below lesion
- LMN signs at lesion level (weakness, wasting)
- Autonomic dysfunction
Physiotherapy management:
- Joint protection — Avoid positions that cause shunt expansion
- Strengthening — Available muscles, avoiding Valsalva manoeuvre
- Hydrotherapy — Low-resistance environment
- Splinting and orthotics — Prevent deformity
- Sensory compensation strategies — Visual monitoring of insensate limbs
- Post-surgical rehabilitation (after syrinx drainage)
SECTION 7: MINIMUM BRAIN DAMAGE & RISK BABIES
Q37. What is Minimum Brain Damage (Minimal Brain Dysfunction — MBD)?
A: MBD refers to a cluster of mild, subtle neurological impairments in children of average or near-average intelligence who have mild motor, cognitive, or behavioural difficulties not severe enough to classify as CP or intellectual disability.
Features:
- Mild motor incoordination (clumsiness)
- Learning disabilities (reading, writing, arithmetic)
- Attention deficit (ADHD features)
- Soft neurological signs (mild hyperreflexia, mild tremor, dysdiadochokinesia)
- Normal intelligence
Physiotherapy role:
- Coordination and balance training
- Fine and gross motor skill development
- Sensory integration therapy
- School-based physiotherapy for handwriting, physical education participation
Q38. What is a "risk baby" and what neurophysiological approaches are used?
A: A risk baby is an infant with identified risk factors for neurological/developmental impairment:
Risk factors:
- Preterm birth (<32 weeks gestation)
- Very low birth weight (<1500g)
- Birth asphyxia / HIE
- Neonatal seizures
- Intraventricular haemorrhage (IVH)
- Congenital infections
- Hyperbilirubinemia (kernicterus risk)
Neurophysiological approaches used:
- Vojta therapy — Activates innate locomotion patterns; started from first weeks of life
- NDT/Bobath handling — Correct positioning, facilitate normal postures
- NIDCAP (Newborn Individualized Developmental Care and Assessment Program) — Minimize stimulation in NICU, positional support
- Kangaroo mother care — Skin-to-skin; improves neurodevelopmental outcomes
- Developmental follow-up programs — Regular milestone monitoring, early detection of CP
SECTION 8: QUICK-FIRE VIVA (HIGH-YIELD)
Q: What nerve supplies the pelvic floor in context of paediatric voiding dysfunction?
→ Pudendal nerve (S2, S3, S4)
Q: At what age does independent walking typically occur?
→ 12 months (normal range: 9–15 months)
Q: What is the most common type of CP?
→ Spastic CP (~80%); most common distribution is diplegia (in preterm) and hemiplegia (in term)
Q: Who developed NDT?
→ Karel and Bertha Bobath (1940s)
Q: Who developed Vojta therapy?
→ Václav Vojta
Q: Who developed Sensory Integration therapy?
→ Dr. A. Jean Ayres
Q: What is GMFCS?
→ Gross Motor Function Classification System — 5 levels, classifies CP motor severity
Q: What chromosome is affected in Down syndrome?
→ Chromosome 21 (Trisomy 21)
Q: What must be screened before vigorous exercise in Down syndrome?
→ Atlantoaxial instability (X-ray of C1–C2)
Q: What is the parachute reaction?
→ Protective arm extension when child tilted forward; appears ~8–9 months; persists for life; ABSENT in CP
Q: What is the Babinski sign?
→ Upgoing plantar response (big toe dorsiflexes, other toes fan out) — NORMAL up to 18–24 months; ABNORMAL after this (UMN lesion)
Q: What is CIMT and for which CP type is it most used?
→ Constraint-Induced Movement Therapy; most used in hemiplegic CP
Q: What is PVL and which CP type is it associated with?
→ Periventricular Leukomalacia — white matter damage around ventricles in preterm infants → spastic diplegia
Q: What is HIE and which CP type does it cause?
→ Hypoxic-Ischaemic Encephalopathy (birth asphyxia) → spastic quadriplegia or dyskinetic CP
Q: What is the Modified Ashworth Scale used for?
→ Grading spasticity (0–4)
Q: What does GMFM stand for?
→ Gross Motor Function Measure — outcome measurement tool for CP (88 items across 5 dimensions)
Q: What is learned non-use?
→ The principle underlying CIMT — the weaker limb is progressively abandoned as the stronger limb compensates
Q: What is the stepping reflex and when does it disappear?
→ Automatic stepping when infant is held upright with feet on surface; disappears by 2–3 months
Q: What gait pattern is seen in spastic diplegia?
→ Scissor gait (hip adduction + internal rotation, toe walking)
Q: What is the AIMS scale?
→ Alberta Infant Motor Scale — assesses gross motor development from birth to 18 months (independent walking)
This covers every single topic from your paediatric physiotherapy syllabus in detail, structured for viva answers. Ask if you want any specific condition, technique, or topic expanded even further!
demonstare sit to stand uding ndt principles
Reading File
Finding Sources
Searching Images
sit to stand transfer NDT Bobath cerebral palsy physiotherapy
Loading Image
Loading Image
Sit to Stand Using NDT (Bobath) Principles
📸 Clinical Demonstration — Actual NDT Session
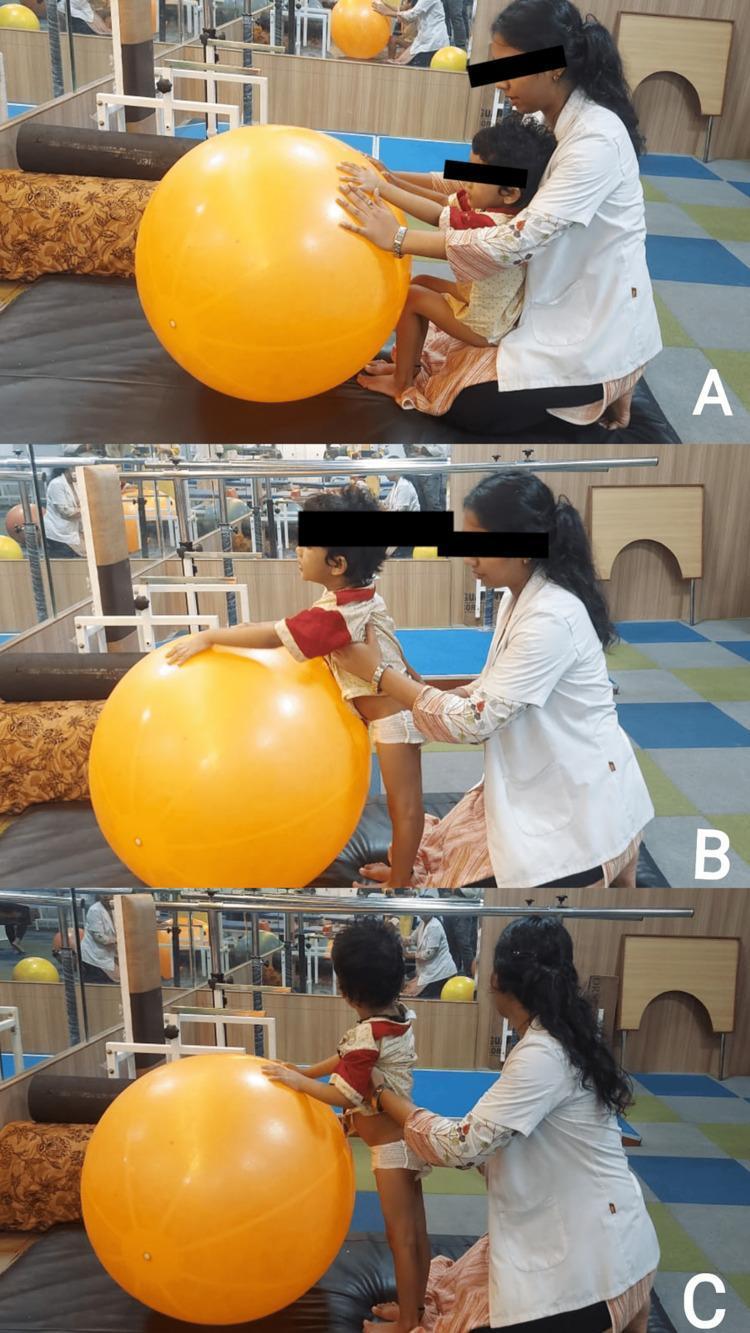
Image A → Seated position with trunk support at pelvis/hips, hands on ball for upper limb loading Image B → Transition/mid-phase — therapist facilitates at hips & trunk, child pushing through arms Image C → Full standing — therapist shifts hands to lower trunk/thighs to maintain pelvic stability
What is Sit to Stand (STS) in NDT?
In NDT (Bobath concept), sit to stand is NOT just a functional transfer — it is used as a therapeutic movement sequence to:
- Inhibit abnormal tone and spasticity
- Facilitate normal weight shift and postural reactions
- Promote symmetrical lower limb loading
- Build antigravity muscle activation (quads, glutes, trunk extensors)
- Develop standing postural control and equilibrium reactions
NDT Principles Applied to Sit to Stand
| NDT Principle | Application in STS |
|---|---|
| Inhibition of abnormal tone | Break up flexor/extensor synergies before initiating movement |
| Key points of control | Therapist handles at pelvis, shoulder girdle, or knees |
| Facilitation of normal patterns | Guide through the biomechanically correct movement arc |
| Weight shift | Anterior shift of trunk over feet before rising |
| Symmetry | Equal loading through both lower limbs |
| Postural reactions | Stimulate equilibrium and righting reactions in standing |
| Sensory input | Use of ball, surface textures, weight bearing for proprioception |
Step-by-Step: Sit to Stand Using NDT
🟡 PHASE 0 — Preparation (Before Movement Begins)
Goal: Normalize tone, position optimally, achieve active sitting posture
Child's position:
- Sitting at the edge of a plinth or stool
- Hips at 90° flexion, feet flat on the floor, hip-width apart
- Trunk erect, head in midline
Therapist's role:
- Assess tone — if high extensor tone or ATNR pattern, inhibit first
- For spastic child: perform slow rotational trunk movements (trunk rotation RIP) to reduce spasticity before initiating STS
- Ensure symmetrical pelvis — no posterior pelvic tilt or lateral lean
- Position feet BEHIND the knees (ankles dorsiflexed) to prepare for weight acceptance
🟡 PHASE 1 — Anterior Weight Shift ("Nose Over Toes")
Goal: Shift the child's centre of gravity forward over the base of support
What happens biomechanically:
- Trunk inclines forward (hip flexion) — "nose over toes"
- Body weight moves from ischial tuberosities → onto feet
- Ankle dorsiflexion occurs
- Eccentric quad activity prepares for push-off
NDT handling — Key Points of Control:
Option A: Pelvic control (most common)
- Therapist kneels/sits in front of or behind child
- Both hands on the anterior superior iliac spine (ASIS) or lateral pelvis
- Facilitate anterior pelvic tilt + forward trunk lean
- Prevent posterior pelvic tilt (which causes the child to fall back)
Option B: Shoulder girdle control
- Hands on shoulder girdle
- Guide trunk forward and slightly down (inhibiting scapular retraction in spastic child)
Verbal cue: "Lean forward — bring your nose to your knees"
Visual cue: Place a toy/target in front and slightly above eye level to encourage forward lean
🟡 PHASE 2 — Momentum Phase (Initiation of Rise)
Goal: Transfer forward momentum into upward movement — the "push-off"
What happens biomechanically:
- Continued forward trunk lean generates momentum
- Hip and knee extensors (gluteus maximus, quadriceps) begin concentric contraction
- The child rises from the seat — hips and knees extend simultaneously
- Arms may assist by pushing off thighs or a surface
NDT handling:
- Therapist facilitates upward and forward direction of movement at the pelvis
- Prevent the child's hips from shooting backward (common in extensor spasticity)
- If scissoring (hip adduction) occurs — guide hips apart with thumbs on medial thighs
- For a child with poor initiation — use tapping (quick stretch) on quads just before rise to activate muscle spindles
Ball technique (as shown in image):
- Child places hands on a Swiss ball placed in front
- Ball provides proprioceptive input through upper limbs
- Prevents forward fall and gives confidence
- Therapist handles at trunk/pelvis from behind
🟡 PHASE 3 — Full Extension & Standing
Goal: Achieve full upright standing with symmetrical weight bearing and active postural reactions
What happens biomechanically:
- Hips, knees, and ankles fully extend
- Trunk aligns over lower limbs
- Postural tone activates in trunk extensors, hip abductors, and ankles
NDT handling:
- Therapist's hands move to lower trunk / greater trochanter area to support upright pelvis
- Check for:
- Hip hyperextension (common in hypotonic child) — facilitate slight hip flexion, engage glutes
- Knee hyperextension (back-knee) — press gently behind knee to encourage slight flexion/co-contraction
- Equinus (toe standing) — guide heel contact with floor, provide firm input through calcaneus
- Lateral lean — facilitate midline through pelvic handling
Equilibrium reactions:
- Once standing is achieved, introduce gentle weight shifts side-to-side and forward-backward to stimulate standing equilibrium and righting reactions
- This is a core NDT principle — postural reactions must be facilitated, not just achieved
🟡 PHASE 4 — Consolidation in Standing
Goal: The child maintains active, independent standing as long as possible
- Progress from maximum assistance → minimum assistance → hands-off
- Use graded withdrawal of therapist support (reduce handling gradually)
- Introduce reaching tasks while standing (activates anticipatory postural adjustments)
- Use mirrors for visual biofeedback of upright posture
Common Problems & NDT Solutions
| Problem Seen | NDT Solution |
|---|---|
| Posterior pelvic tilt when rising | Facilitate anterior pelvic tilt at ASIS; cue trunk lean forward |
| Scissoring (hip adduction) during rise | Guide knees apart; abduction facilitation at medial thighs |
| One-sided weight bearing (hemiplegia) | Weight shift onto affected side; load the affected lower limb |
| Toe standing / equinus | Press through heel; AFO before session; facilitate dorsiflexion |
| Trunk collapsed in flexion | Key point at shoulder girdle, facilitate trunk extension |
| Child pushes back into extension (total extensor pattern) | Trunk rotation / flexion RIP before initiating STS |
| Fear / poor confidence | Use Swiss ball or parallel bars as forearm support initially |
| Hyperextended knees in standing | Gentle posterior knee pressure to activate knee flexors |
NDT Handling Images — Trunk & Pelvis Facilitation
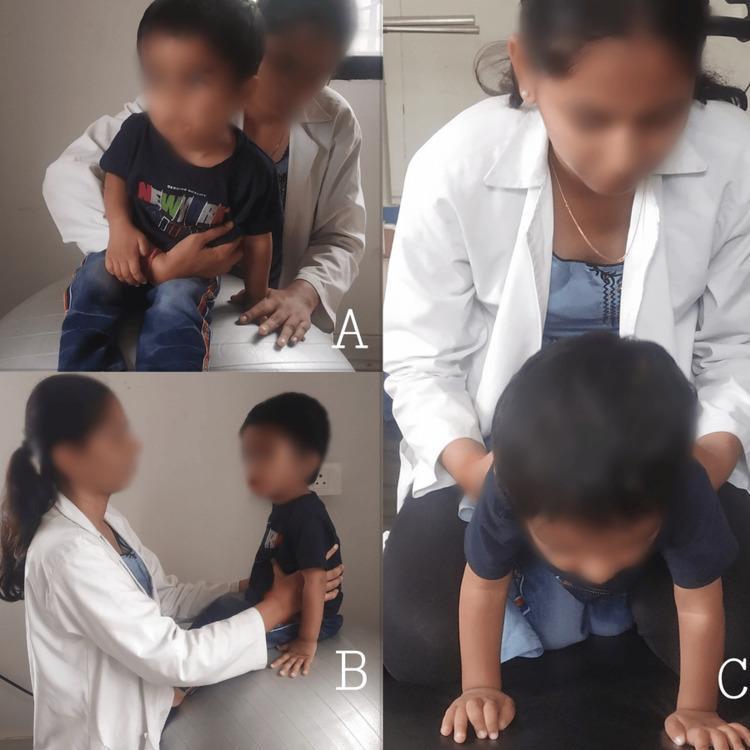
Panel A — Therapist facilitates at pelvis and lower trunk from behind (seated) Panel B — Swiss ball used to challenge dynamic core stability Panel C — Quadruped facilitation for trunk co-contraction and weight bearing
Grading the Activity (Progression Levels)
| Level | How to Progress |
|---|---|
| Maximum assist | Therapist fully guides at pelvis, child's arms on ball/rail |
| Moderate assist | Therapist at pelvis only, arms free |
| Minimal assist | Therapist touches thighs only as cue |
| Supervision | Therapist stands by, verbal cues only |
| Independent | No support, varied surfaces (pillow, incline) |
| Advanced | STS without hands, from low surface, carrying an object |
Summary — NDT Sit to Stand Checklist
✅ Normalize tone BEFORE initiating movement
✅ Symmetrical base — feet flat, hip-width, behind knees
✅ Anterior pelvic tilt + trunk forward lean ("nose over toes")
✅ Weight shift forward onto feet
✅ Facilitate rise with upward-forward direction at pelvis
✅ Correct scissoring, equinus, or lateral lean during transition
✅ Achieve full upright standing — aligned trunk, hips, knees, ankles
✅ Stimulate standing equilibrium reactions
✅ Withdraw support gradually — aim for independence
✅ Functional task immediately after standing (reach, step, play)
This is the complete NDT-based sit to stand demonstration framework. Ask if you want the stand to sit, standing balance, or gait facilitation using NDT next!
This is a shared conversation. Sign in to Orris to start your own chat.