Tell me brief treatment of pancreatitis with serum amylase 3000 and nausea vomiting with core concept and diagram
Reading File
Finding Sources
Finding Sources
Searching Images
acute pancreatitis pathophysiology diagram treatment
Reading File
Reading File
Loading Image
Reading File
I have sufficient information. Let me now deliver a comprehensive, well-structured answer.
Acute Pancreatitis — Brief Treatment Overview
Serum Amylase 3000 U/L (normal <100–300 U/L) = ~10× elevation → strongly confirms acute pancreatitis when paired with nausea, vomiting, and epigastric pain. Note: lipase is more specific; amylase is also elevated in renal failure, intestinal obstruction, and perforated ulcer.
Core Concept
Acute pancreatitis is premature activation of pancreatic enzymes (trypsinogen → trypsin) within acinar cells, causing autodigestion of the gland and surrounding tissues. The classic triggers are:
- Gallstones (most common overall)
- Alcohol (most common in chronic/recurrent)
- Hypertriglyceridemia, ERCP, trauma, drugs
Pathophysiology at a Glance
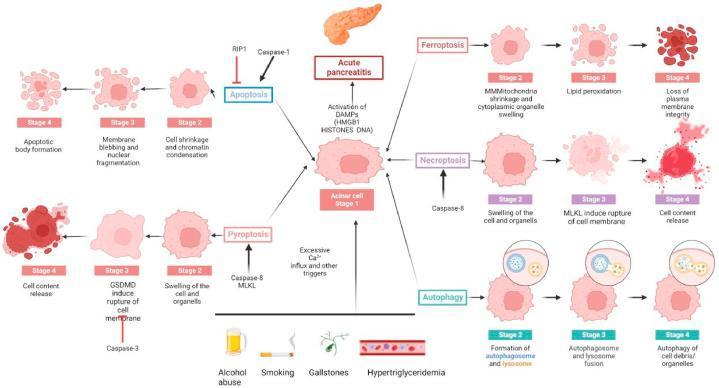
Triggers (alcohol, gallstones, smoking, hypertriglyceridemia) activate DAMPs in pancreatic acinar cells, initiating apoptosis, necroptosis, ferroptosis, pyroptosis, and autophagy — all contributing to pancreatic inflammation and systemic injury.
Treatment — Pillars of Management
1. Aggressive IV Fluid Resuscitation (Most Critical Step)
- Lactated Ringer's is preferred over normal saline (reduces systemic inflammation)
- Rate: 250–500 mL/hr initially; titrate to urine output >0.5 mL/kg/hr
- Goal: correct hypovolemia caused by third-spacing and vomiting
2. NPO (Nil Per Os) + GI Rest
- Keep the patient NPO initially to reduce pancreatic secretion stimulation
- Insert nasogastric tube if vomiting is intractable (decompresses the stomach, reduces aspiraton risk)
- Restart oral feeds as soon as tolerated — early enteral feeding (within 24–48 hrs if mild) is now preferred over prolonged fasting
3. Analgesia
- Opioids (morphine, fentanyl, hydromorphone) — first-line for pain control
- Old teaching that morphine causes sphincter of Oddi spasm is not clinically significant
- IV route preferred initially given nausea/vomiting
4. Antiemetics
- Ondansetron (5-HT₃ antagonist) — first-line
- Metoclopramide or promethazine as alternatives
5. Monitor & Manage Complications
| Parameter | Target |
|---|---|
| Urine output | >0.5 mL/kg/hr |
| Heart rate | <100 bpm |
| Hematocrit | 35–44% |
| BUN | Trending down |
| Calcium | Monitor (hypocalcemia in severe disease) |
| Blood glucose | Control hyperglycemia |
6. Antibiotics — NOT routine
- Only if infected pancreatic necrosis is suspected (fever, rising WBC after 72 hrs, CT showing >30% pancreatic necrosis with gas)
- Drug of choice: Imipenem/meropenem or piperacillin-tazobactam
7. Treat the Cause
- Gallstone pancreatitis with cholangitis or biliary obstruction → urgent ERCP within 24–48 hrs
- Alcohol-related → abstinence counseling
- Hypertriglyceridemia (>1000 mg/dL) → insulin drip + consider plasmapheresis
Severity Assessment (Revised Atlanta Classification)
| Severity | Features |
|---|---|
| Mild | No organ failure, no local complications; resolves in 1 week |
| Moderately severe | Transient organ failure (<48 hrs) or local complications |
| Severe | Persistent organ failure (>48 hrs); mortality up to 30% |
Bedside index (BISAP Score) — BUN >25, impaired mental status, SIRS, age >60, pleural effusion → score ≥3 predicts mortality.
Summary Algorithm
Acute Pancreatitis (Amylase >3× normal + symptoms)
│
▼
IV Fluids (LR, aggressive)
+ NPO + Analgesia (opioids)
+ Antiemetics (ondansetron)
│
▼
Severity Assessment (BISAP, APACHE-II)
│
┌────┴────┐
Mild Severe/Necrotizing
│ │
Early oral ICU admission
re-feeding Monitor organs
Treat cause CT abdomen
± ERCP
± Antibiotics (if infected necrosis)
Key Points to Remember
| Concept | Detail |
|---|---|
| Amylase 3000 U/L | ~10× normal → confirms pancreatitis, but lipase is more specific |
| Best fluid | Lactated Ringer's (not NS) |
| Pain control | IV opioids are safe and appropriate |
| Feeding | Early oral/enteral feeding preferred over prolonged NPO |
| Antibiotics | NOT prophylactic; only for infected necrosis |
| ERCP | Only if gallstone pancreatitis with obstruction/cholangitis |
| Avoid | NSAIDs (worsen GI; not adequate alone), prolonged fasting |
Sources: Tintinalli's Emergency Medicine, p. 600; Goodman & Gilman's Pharmacological Basis of Therapeutics, Pancreas section
a 1.5 year old boy having fever 104 degree and having history of sand eating and loose stool what was the perfect diagnose and treatment for the child
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching Images
pica geophagia intestinal parasites child diagnosis
Loading Image
Loading Image
Now I have all the information needed. Here is a comprehensive clinical answer:
Clinical Case: 1.5-Year-Old Boy | Fever 104°F + Sand Eating + Loose Stool
Primary Diagnosis: Intestinal Parasitosis secondary to Geophagia (Pica)
This triad — pica (sand/soil eating) + high fever (104°F / 40°C) + loose stools in a toddler — is a classic presentation of intestinal parasitic infection, most likely:
| Most Likely | Also Consider |
|---|---|
| Giardia lamblia (giardiasis) | Entamoeba histolytica (amoebiasis) |
| Ascaris lumbricoides (roundworm) | Toxocara canis (Visceral Larva Migrans) |
| Trichuris trichiura (whipworm) | Strongyloides stercoralis |
Understanding the Clinical Picture
🔵 Why Sand/Soil Eating (Geophagia / Pica)?
Pica is the compulsive ingestion of non-food substances. In toddlers (12–36 months), it is commonly driven by:
- Iron deficiency anemia (most common underlying cause)
- Zinc deficiency
- Developmental/behavioral factors
Sand/soil ingestion directly introduces helminth eggs and protozoa into the GI tract → infection → fever + diarrhea.

🔴 High Fever (104°F = 40°C)
Fever this high in a toddler with parasitosis suggests:
- Active tissue invasion (Toxocara, Ascaris larval migration)
- Systemic inflammatory response to parasitic antigens
- Secondary bacterial superinfection from gut mucosal damage
- Concurrent viral illness (always rule out)
🟡 Loose Stools
- Disruption of intestinal mucosa by parasites → malabsorption diarrhea
- Giardia causes fatty, foul-smelling, pale loose stools
- Amoeba causes bloody/mucoid diarrhea (dysentery)
- Ascaris/Trichuris → watery or mucoid loose stools
Endoscopic Appearance of Intestinal Parasites
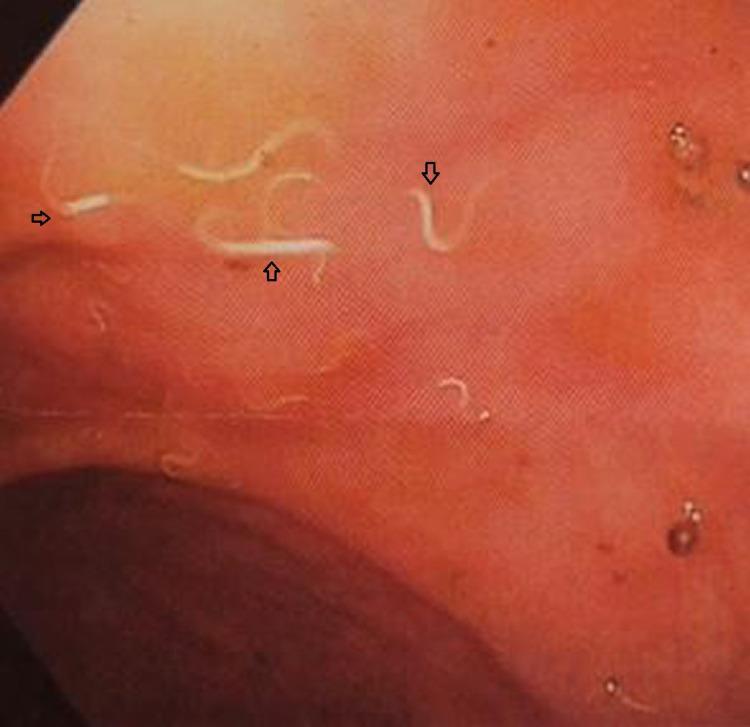
Investigations to Order
| Test | Purpose |
|---|---|
| Stool microscopy (×3 samples) | Detect ova, cysts, trophozoites |
| Stool antigen test | Rapid detection of Giardia/Cryptosporidium |
| CBC with differential | Eosinophilia → helminth infection; anemia |
| Serum ferritin + iron studies | Confirm iron deficiency (driving pica) |
| Blood film | Rule out malaria (high fever in endemic areas) |
| LFT, serology (Toxocara ELISA) | If visceral larva migrans suspected |
| Abdominal X-ray | If heavy worm burden (Ascaris bolus) suspected |
Treatment
Step 1: Control High Fever
- Paracetamol (Acetaminophen): 15 mg/kg/dose every 4–6 hrs PO/PR
- Tepid sponging
- Ensure adequate oral hydration (ORS if dehydrated)
- If fever >48 hrs or child appears toxic → hospitalize, rule out malaria/sepsis
Step 2: Antiparasitic Treatment
| Parasite | Drug of Choice | Dose (Pediatric) |
|---|---|---|
| Giardia lamblia | Metronidazole | 15 mg/kg/day ÷ 3 doses × 5–7 days |
| Entamoeba histolytica | Metronidazole | 30–40 mg/kg/day ÷ 3 doses × 10 days |
| Ascaris / Trichuris / Hookworm | Albendazole | 400 mg single dose (≥2 yrs); 200 mg (<2 yrs) |
| Ascaris / hookworm | Mebendazole | 100 mg BD × 3 days OR 500 mg single dose |
| Toxocara (VLM) | Albendazole | 15 mg/kg/day × 5 days + oral prednisolone |
⚠️ Child is 1.5 yrs (18 months) — Albendazole dose = 200 mg (half of standard) for children 12–24 months per WHO guidelines.
Step 3: Treat Underlying Iron Deficiency (Driving Pica)
- Elemental iron: 3–6 mg/kg/day in 2 divided doses for 3 months
- Zinc supplementation: 10 mg/day × 14 days (also reduces diarrhea duration per WHO/UNICEF)
Step 4: Manage Diarrhea / Dehydration
- ORS (Oral Rehydration Solution) — give 75 mL/kg over 4 hrs if mild-moderate dehydration
- Zinc: 10 mg/day × 14 days — proven to shorten diarrhea duration and reduce severity in children <5 yrs
- Continue breastfeeding/normal feeding
- Avoid antidiarrheals (loperamide) — contraindicated in children <2 yrs
Summary Algorithm
1.5-yr Boy: Fever 104°F + Sand Eating + Loose Stools
│
▼
PICA → Intestinal Parasitosis
│
┌──────────┼──────────┐
▼ ▼ ▼
Giardia Amoebiasis Helminths
(watery (bloody (loose ±
stool) mucoid) mucoid)
│
┌──────────┼──────────┐
▼ ▼ ▼
Stool MC&S CBC Iron/Zinc
Antigen (eosinophilia) studies
│
▼
TREAT:
► Antipyretic (Paracetamol)
► Metronidazole (Giardia/Amoeba)
► Albendazole 200 mg (Helminths)
► ORS + Zinc (diarrhea)
► Iron supplementation (pica)
► Nutritional counseling
Preventive Advice for Parents
| Action | Reason |
|---|---|
| Wash hands before feeding child | Break fecal-oral transmission cycle |
| Keep child away from soil/sand play unsupervised | Prevent reinfection |
| Cook food thoroughly, wash vegetables | Destroy parasite eggs |
| Treat iron deficiency fully | Eliminates the drive to eat non-food items |
| Deworm all household contacts | Household transmission is common |
| Follow-up stool test at 2 weeks | Confirm treatment success |
Bottom line: This child most likely has Giardiasis or Ascariasis acquired through geophagia, driven by iron deficiency anemia. First-line treatment is Metronidazole + Albendazole 200 mg, combined with ORS + Zinc for diarrhea, Paracetamol for fever, and iron supplementation to address the root cause of pica. Investigate for malaria if the child lives in or has traveled to an endemic area.
This is a shared conversation. Sign in to Orris to start your own chat.