Forces acting on shoulder during anterior dislocation
Reading File
Finding Sources
Finding Sources
Searching Images
anterior shoulder dislocation forces mechanism
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Loading Image
Now I have comprehensive information to provide a thorough answer. Let me compile it.
Forces Acting on the Shoulder During Anterior Dislocation
Mechanism Overview
Anterior dislocation accounts for ~96–98% of all glenohumeral dislocations. The humeral head is forced anteriorly past the glenoid rim, most commonly to a subcoracoid position (>99% of cases).
Primary Force Vectors
1. Abduction + External Rotation (Most Common)
The classic mechanism involves the arm in abduction (~90°) and external rotation — common in throwing, tackling, or falling on an outstretched arm. The forces at play:
- External rotation torque winds up the anterior capsule and inferior glenohumeral ligament (IGHL), which act as a cam.
- Once the IGHL is maximally stretched, continued external rotation levers the humeral head anteriorly over the glenoid rim.
- The subscapularis (primary anterior dynamic stabilizer) is overcome by the external rotation force.
- The humeral head translates anteroinferiorly, avulsing the anteroinferior labrum (Bankart lesion).
"This is the subcoracoid, anterior shoulder dislocation, usually occurring when an abducted, extended, and externally rotated upper extremity takes a major jolt. The resulting lever forces the proximal humerus anteriorly." — Pfenninger & Fowler's Procedures for Primary Care
2. Posterolateral Direct Force
A direct blow applied posterolaterally to the humeral head (e.g., tackling in collision sports with the arm extended):
- Drives the humeral head anteriorly across the glenoid rim.
- The glenoid rim acts as a fulcrum, and the posterior force vector translates to anterior displacement.
- Creates a Hill-Sachs lesion: impaction fracture of the posterolateral humeral head against the anterior glenoid rim.
3. Fall on Outstretched Hand (FOOSH) — Older Patients
- Ground reaction force travels up the long axis of the humerus.
- With the arm forward-flexed and externally rotated, this axial load is converted into an anterior shear force at the glenohumeral joint.
- More common in patients >40 years and associated with rotator cuff tears (up to 80% incidence in patients >60 years).
The Mechanism Illustrated
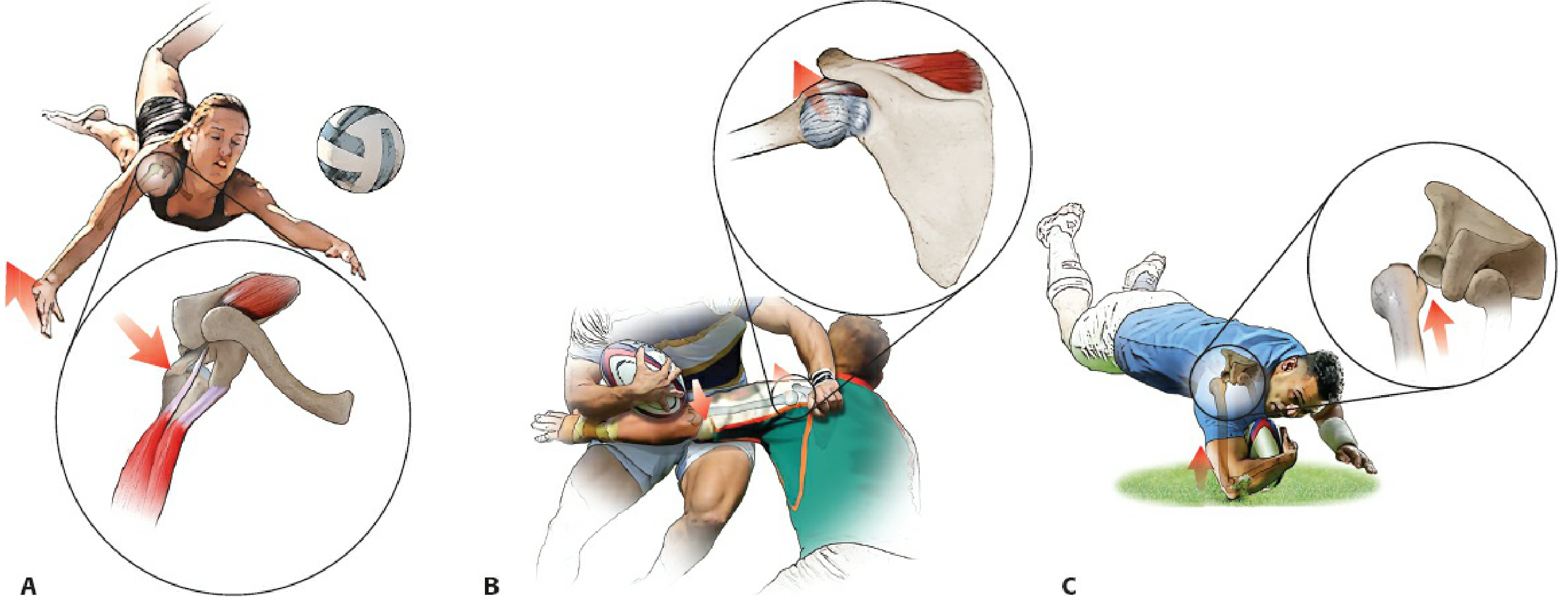
Figure: A — Fall onto forward-flexed, externally rotated arm → anterior dislocation. B — Tackling with arm extended + posteriorly directed force → anterior dislocation. C — Fall onto forward-flexed, internally rotated arm → posterior dislocation. (Rockwood & Green's Fractures in Adults, 10th ed.)
Force Summary Table
| Force Component | Direction | Effect |
|---|---|---|
| External rotation torque | Lateral → anterior spin | Overcomes IGHL, levers humeral head anteriorly |
| Abduction | Superolateral | Tightens inferior capsule; positions humeral head at glenoid rim edge |
| Direct posterolateral blow | Posterior → anterior | Directly translates head forward over rim |
| Axial load (FOOSH) | Distal → proximal | Converted to anterior shear at glenohumeral joint |
| Extension force | Posterior | Stretches anterior capsule, reduces anterior restraint |
Structures Resisting These Forces (and Failing)
| Stabilizer | Type | Failure Pattern |
|---|---|---|
| Inferior glenohumeral ligament complex (IGHLC) | Static | Avulsion from glenoid rim → Bankart lesion |
| Anterior labrum | Static | Tear/detachment (Bankart lesion) |
| Subscapularis | Dynamic | Overpowered by external rotation force |
| Anterior capsule | Static | Stretching, rupture, or HAGL lesion (humeral avulsion) |
| Glenoid rim bone | Static | Bony Bankart fracture (high-energy mechanisms) |
Associated Injuries by Force Magnitude
- Low-energy: Capsulolabral avulsion only (Bankart lesion)
- Moderate: Hill-Sachs lesion (posterolateral humeral head impaction fracture)
- High-energy: Bony Bankart, greater tuberosity fracture, axillary nerve injury (≤13.5%), axillary artery injury (rare), rotator cuff tear
- Subclavicular/intrathoracic dislocation: Requires additional strong lateral-to-medial force vector — extremely rare
"Subclavicular and intrathoracic dislocations are extremely rare and involve the addition of strong lateral to medial forces." — Rosen's Emergency Medicine, 10th ed.
Sources:
- Rockwood & Green's Fractures in Adults, 10th ed., p. 1248–1249
- Rosen's Emergency Medicine, 10th ed., p. 654
- Pfenninger & Fowler's Procedures for Primary Care, 3rd ed.
This is a shared conversation. Sign in to Orris to start your own chat.