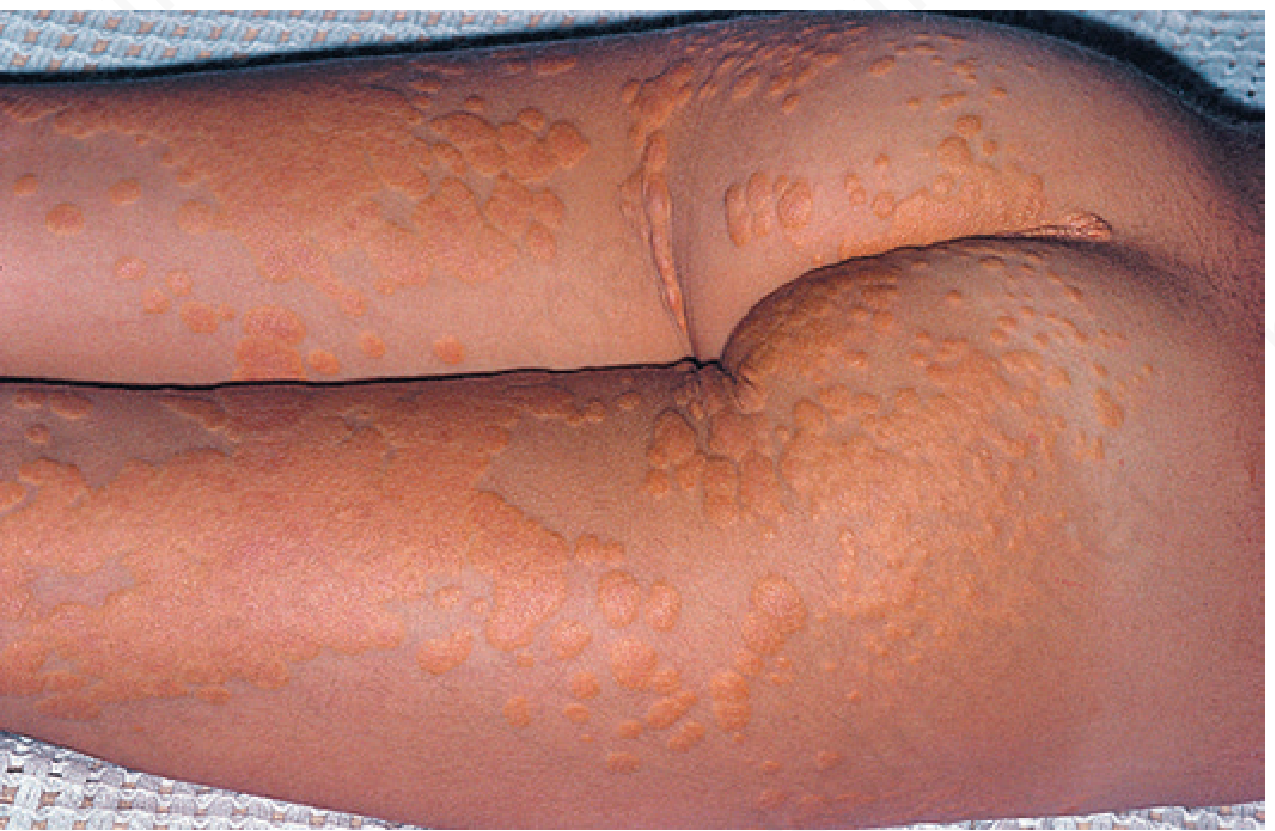
9 yrs old female multiple cholesterol diposition in skin total cholesterol 750 mg/dl
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Based on the clinical scenario — a 9-year-old girl with multiple cholesterol deposits in the skin and a total cholesterol of 750 mg/dL — this is a classic presentation of Homozygous Familial Hypercholesterolemia (HoFH).
Diagnosis: Homozygous Familial Hypercholesterolemia (HoFH)
Pathogenesis
FH is a "receptor disease" caused in 80–85% of cases by loss-of-function mutations in the LDL receptor gene, which impairs transport and catabolism of LDL cholesterol. Additional causative mutations include:
- ApoB-100 mutations (5–10%) — defective LDL ligand
- Gain-of-function PCSK9 mutations (1–2%) — increased degradation of LDL receptors
Without functional LDL receptors:
- LDL cannot be cleared from circulation
- IDL is not taken up by the liver → more is converted to LDL
- Excess LDL is taken up by macrophages and monocytes via scavenger receptors → deposits as xanthomas
- Accelerated atherosclerosis ensues
— Robbins & Kumar Basic Pathology, p. 111–112
Why Homozygous (not Heterozygous)?
| Feature | Heterozygous FH | Homozygous FH |
|---|---|---|
| Cholesterol | 2–3× elevated (~300–500 mg/dL) | >5× elevated (600–1200 mg/dL) |
| Xanthomas | Tendon xanthomas in adulthood | Cutaneous xanthomas in childhood |
| Cardiac events | Middle age | MI before age 20 |
This child's presentation — xanthomas appearing at age 9 with cholesterol 750 mg/dL — is textbook homozygous FH.
— Robbins & Kumar Basic Pathology, p. 112 | Fitzpatrick's Dermatology, p. 2311
LDL Receptor Mutation Classes (5 Classes)
| Class | Defect |
|---|---|
| I | Complete absence of LDL receptor synthesis |
| II | Defective transport from ER to Golgi |
| III | Abnormal LDL-receptor binding (receptor or ApoB mutation) |
| IV | Correct binding, defective endocytosis |
| V | Defective receptor recycling |
Types of Xanthomas in FH
- Tendinous xanthomas — most common in heterozygotes; over Achilles tendon, extensor tendons of hands
- Tuberous/tuberoeruptive xanthomas — over elbows, knees
- Planar/cutaneous xanthomas — flat deposits in skin folds (interdigital, palmar)
- Xanthelasma — periorbital cholesterol deposits
- In HoFH, xanthomas appear in childhood and may be widespread
Cardiovascular Risk
Premature, accelerated atherosclerosis is the major cause of morbidity and mortality. Children with HoFH can develop:
- Coronary artery disease
- Aortic valve stenosis (lipid infiltration)
- Death from MI before age 20 if untreated
Management
1. Statins (first-line)
- Inhibit HMG-CoA reductase → reduce cholesterol synthesis → upregulate LDL receptor expression
- Note: In true HoFH (no functional LDL receptors), statins have limited efficacy
2. PCSK9 Inhibitors (e.g., evolocumab, alirocumab)
- Monoclonal antibodies that block PCSK9 → prevent degradation of LDL receptors
- Also: inclisiran (siRNA targeting PCSK9 transcription)
3. Ezetimibe
- Inhibits intestinal cholesterol absorption (NPC1L1 transporter)
4. Lomitapide / Mipomersen
- Used specifically for HoFH; reduce hepatic VLDL production or ApoB synthesis
5. LDL Apheresis
- Mechanical removal of LDL from blood; recommended every 1–2 weeks in HoFH
6. Liver Transplantation
- Provides functional LDL receptors; considered in severe refractory HoFH
- Also: portacaval shunt and ileal bypass (older, less favored options)
— Fitzpatrick's Dermatology; Robbins & Kumar Basic Pathology, p. 112
Key Takeaway
A 9-year-old with multiple cutaneous xanthomas + total cholesterol ~750 mg/dL = Homozygous Familial Hypercholesterolemia (autosomal dominant, LDL receptor mutation). This child is at high risk of fatal MI in the second decade of life without aggressive lipid-lowering therapy, ideally including LDL apheresis and PCSK9 inhibition.
This is a shared conversation. Sign in to Orris to start your own chat.