Patient Education & Counselling Disease Awareness Glomerulonephritis
Reading File
Finding Sources
Finding Sources
Searching Images
glomerulonephritis kidney anatomy pathology
Reading File
Reading File
Reading File
Finding Sources
Searching Images
glomerulonephritis nephritic syndrome hematuria red cell casts urine microscopy
Reading File
Reading File
I now have comprehensive information from authoritative nephrology textbooks to produce a thorough patient education and counselling document on Glomerulonephritis. Let me compile this.
🫘 Patient Education & Counselling — Glomerulonephritis (GN)
What is Glomerulonephritis?
Your kidneys contain millions of tiny filtering units called glomeruli. Each glomerulus is a small ball of blood vessels that cleans your blood by removing waste, excess salt, and water. Glomerulonephritis (GN) means these filters are inflamed. When inflamed, the glomeruli cannot filter blood properly — they allow blood and protein to leak into the urine and fail to remove waste from the body efficiently.
GN can be acute (sudden onset) or chronic (slow and progressive over months to years). It is one of the leading causes of kidney failure worldwide.
How the Kidneys Are Affected — What Goes Wrong?
In GN, the immune system mistakenly attacks the glomeruli. This can happen in several ways:
| Mechanism | Example |
|---|---|
| Antibodies attack the glomerular basement membrane directly | Anti-GBM disease / Goodpasture's syndrome |
| Immune complexes deposited after infection | Post-streptococcal GN |
| Immune complexes from a systemic disease | Lupus nephritis, Hepatitis C |
| Antibodies against white blood cell proteins | ANCA-associated vasculitis |
| IgA deposits in the mesangium | IgA nephropathy (most common worldwide) |
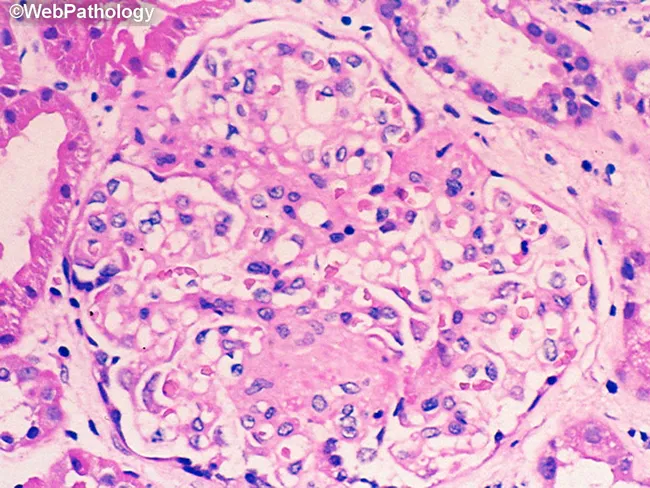
What Causes Glomerulonephritis?
GN has many possible triggers:
🦠 Infections
- Streptococcal throat infection or skin infection (impetigo) — the most classic cause in children (post-streptococcal GN)
- Hepatitis B → membranous or membranoproliferative GN
- Hepatitis C → cryoglobulinemic GN, membranoproliferative GN
- Bacterial endocarditis (infection of heart valves)
- HIV, malaria, schistosomiasis
🔁 Autoimmune / Systemic Diseases
- Systemic Lupus Erythematosus (SLE)
- IgA vasculitis (Henoch-Schönlein purpura)
- Granulomatosis with polyangiitis (Wegener's)
- Microscopic polyangiitis
- Goodpasture's disease
💊 Drugs and Toxins
- Hydralazine, levamisole-adulterated cocaine, penicillamine, gold therapy
🧬 Inherited/Other
- Alport syndrome (genetic disorder of collagen IV in the glomerular basement membrane)
- IgG4-related kidney disease
- C3 glomerulopathy (complement-driven)
Who Gets Glomerulonephritis?
- Post-streptococcal GN is most common in children aged 3–10 years, though it can affect all ages
- About 10–15% of people with nephritogenic streptococcal infection develop GN
- In younger children, the trigger is often skin infection (impetigo); in older children and adults, it is more commonly throat infection (pharyngitis)
- Autoimmune and IgA-related forms are more common in adults
Symptoms — What You Might Notice
The clinical features of GN result from the damaged glomeruli leaking blood and protein and failing to remove waste:
| Symptom | Why It Happens |
|---|---|
| Dark, tea-coloured, or red urine (hematuria) | Blood leaking through damaged glomerular filters |
| Foamy or frothy urine (proteinuria) | Protein leaking into urine |
| Puffiness / swelling (oedema) — especially face, ankles, legs | Low blood protein + fluid retention |
| High blood pressure (hypertension) | Kidneys retaining salt and water |
| Decreased or no urine output | Severely impaired kidney filtration |
| Fatigue and malaise | Build-up of waste products in the blood |
| Headache | Often related to high blood pressure |
| Low-grade fever, anorexia | Associated inflammation |
⚠️ Warning signs: If you develop sudden, severe reduction in urine output, or urine that looks like cola/blood — seek immediate medical attention. Some forms of GN can progress to kidney failure within days to weeks if untreated.
How is it Diagnosed?
Your doctor will use several tests to confirm GN and identify the cause:
Blood Tests
- Serum creatinine & urea — to assess kidney function
- Complement levels (C3, C4) — low in post-streptococcal GN, lupus, MPGN
- Anti-streptolysin O (ASO) titre — elevated after streptococcal infection
- ANA, anti-dsDNA — for lupus
- ANCA (MPO / PR3) — for vasculitis-associated GN
- Anti-GBM antibodies — for Goodpasture's disease
- Immunoglobulins — IgA, IgG levels
Urine Tests
- Urine microscopy — reveals red blood cell (RBC) casts (the hallmark of GN), granular casts, white cells
- Urine protein-to-creatinine ratio — quantifies protein loss
- 24-hour urine protein collection
Kidney Biopsy
- Often essential for definitive diagnosis
- A small needle removes a tiny piece of kidney tissue, which is examined under light microscopy, immunofluorescence, and electron microscopy to identify the exact type of GN
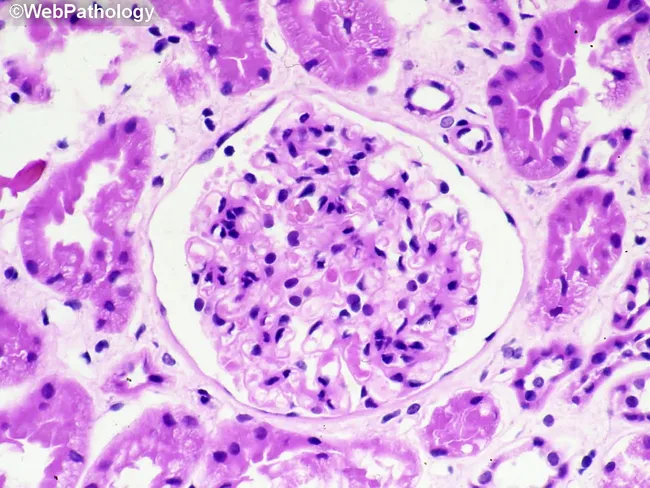
Types of Glomerulonephritis
| Type | Key Feature | Typical Cause |
|---|---|---|
| Post-streptococcal GN | Follows throat/skin strep infection, self-limiting | Group A β-haemolytic streptococcus |
| IgA Nephropathy (Berger's disease) | Mesangial IgA deposits; episodic haematuria | Unknown trigger; most common GN globally |
| Membranous Nephropathy | Subepithelial deposits; nephrotic syndrome | Idiopathic, lupus, hepatitis B, cancer |
| Membranoproliferative GN (MPGN) | Thickened basement membrane + proliferation | Hepatitis C, complement dysregulation |
| Rapidly Progressive GN (RPGN) | Crescents on biopsy; rapid kidney failure | Anti-GBM, ANCA vasculitis, immune complex |
| Lupus Nephritis | Subendothelial deposits | Systemic lupus erythematosus |
| ANCA-Associated GN | Pauci-immune (few deposits) | Granulomatosis with polyangiitis, MPA |
| Anti-GBM Disease / Goodpasture's | Linear IgG on basement membrane | Autoantibodies to α3(IV) collagen |
Treatment
Treatment depends on the type and severity of GN. There is no single treatment for all forms.
🔵 General Supportive Measures (for most types)
- Low-salt diet — reduces fluid retention and blood pressure
- Fluid restriction — if significant oedema or reduced urine output
- Protein restriction — reduces load on damaged kidneys
- Loop diuretics (e.g., furosemide) — to remove excess fluid
- ACE inhibitors or ARBs — lower blood pressure AND reduce protein leakage; protect the kidneys long-term
- Blood pressure control — critical to slow progression
🔴 Specific Immunosuppressive Therapy
- Corticosteroids (prednisolone) — cornerstone for autoimmune and inflammatory GN types
- Cyclophosphamide — used for severe lupus nephritis, ANCA vasculitis, anti-GBM disease
- Rituximab — increasingly used for ANCA vasculitis and membranous nephropathy
- Mycophenolate mofetil (MMF) — used in lupus nephritis and other immune GN
- Plasma exchange (plasmapheresis) — urgently removes harmful antibodies in Goodpasture's disease and severe ANCA vasculitis
🟡 Anticoagulation
- If heavy protein loss (nephrotic range) occurs, clotting risk rises — anticoagulant therapy may be prescribed
Prognosis — What to Expect
| Type | Outlook |
|---|---|
| Post-streptococcal GN | Excellent — ~95% of patients regain normal kidney function within 8–12 weeks |
| Minimal change disease | Excellent response to steroids |
| IgA nephropathy | Variable — up to 30–40% progress to chronic kidney disease over 20–25 years |
| Membranoproliferative GN | >70% develop chronic kidney failure over time |
| Rapidly progressive GN (untreated) | Can progress to dialysis-dependent kidney failure within weeks |
| Anti-GBM (Goodpasture's) | Better outcomes with early treatment (dialysis can often be avoided if treated promptly) |
Living With Glomerulonephritis — Patient Guidance
🍽️ Diet
- Reduce salt — aim for < 2 g sodium/day; avoid processed foods, canned soups, pickles
- Limit potassium (bananas, oranges, potatoes) if kidney function is reduced
- Limit phosphate (dairy, cola drinks) if creatinine is elevated
- Adequate calories to prevent muscle wasting — work with a renal dietitian
💊 Medications
- Take all prescribed medications as directed
- Avoid NSAIDs (ibuprofen, naproxen, diclofenac) — these can worsen kidney function
- Avoid contrast dyes for imaging if possible without pre-hydration — inform your radiologist
- Report any new medications (even herbal/OTC) to your nephrologist
🩺 Monitoring
- Regular blood pressure checks (target usually < 130/80 mmHg)
- Routine blood tests: creatinine, electrolytes, urine protein
- Follow-up urine microscopy — improvement in RBC casts signals response to treatment
🚫 Lifestyle
- Stop smoking — smoking worsens kidney and cardiovascular disease
- Limit alcohol
- Exercise moderately — as tolerated; avoid strenuous activity during acute flares
- Avoid unnecessary infections — infections can trigger GN flares (especially in IgA nephropathy)
🤰 Pregnancy
- GN can worsen during pregnancy and increase risks to mother and baby
- Discuss with your nephrologist before planning a pregnancy
- Some immunosuppressants are contraindicated in pregnancy
When to Seek Urgent Medical Help
Contact your doctor or go to the emergency department if you notice:
- 🔴 Sudden dramatic decrease in urine output
- 🔴 Urine that appears bright red or very dark (cola-coloured)
- 🔴 Severe, rapidly worsening swelling
- 🔴 Severe headache with vision changes (hypertensive emergency)
- 🔴 Breathlessness (especially in Goodpasture's — may indicate lung haemorrhage)
- 🔴 Confusion or extreme fatigue (signs of uraemia)
Key Takeaways
- Glomerulonephritis is inflammation of the kidney's filtering units, most often immune-mediated
- Causes range from strep infections to autoimmune diseases to medications
- Cardinal signs are blood and protein in the urine, swelling, and raised blood pressure
- A kidney biopsy is often needed to confirm the exact type and guide treatment
- Treatment ranges from supportive measures to powerful immunosuppression, depending on type
- Post-streptococcal GN in children has an excellent prognosis; other forms need long-term follow-up
- Protect your kidneys: control blood pressure, avoid NSAIDs, follow your prescribed plan, and attend regular check-ups
Sources: Smith & Tanagho's General Urology, 19th Ed. | Comprehensive Clinical Nephrology, 7th Ed. | National Kidney Foundation Primer on Kidney Diseases, 8th Ed. | Swanson's Family Medicine Review
I want Patient Education & Counselling for this disease
Asking for Preferences
The full Patient Education & Counselling material for Glomerulonephritis is already detailed in my previous response above. Here's a quick reference summary you can share directly with patients:
📋 Patient Education Sheet — Glomerulonephritis (GN)
What is it?
Glomerulonephritis is inflammation of the tiny filtering units (glomeruli) in your kidneys. It causes these filters to leak blood and protein into urine and reduces the kidneys' ability to clean the blood.
What Causes It?
- Infections — strep throat, skin infections, hepatitis B or C
- Autoimmune diseases — lupus, IgA vasculitis, Goodpasture's disease
- Antibody-mediated injury — anti-GBM disease, ANCA vasculitis
- Drugs — hydralazine, certain others
Symptoms to Watch For
| Symptom | What It Looks Like |
|---|---|
| Blood in urine | Dark, tea-coloured, or red urine |
| Protein in urine | Foamy or frothy urine |
| Fluid retention | Puffy face, swollen ankles/legs |
| High blood pressure | Headaches, dizziness |
| Reduced urine | Less urine than usual |
| Fatigue | Tiredness, low energy |
How is it Diagnosed?
- Urine test — checks for blood, protein, and RBC casts
- Blood tests — kidney function, complement, antibodies (ASO, ANCA, ANA, anti-GBM)
- Kidney biopsy — the definitive test to identify the exact type
Treatment
Supportive (all types):
- Low-salt, low-fluid diet
- Blood pressure control (ACE inhibitors / ARBs)
- Loop diuretics for swelling
Specific (immune-type GN):
- Corticosteroids (prednisolone)
- Cyclophosphamide, Rituximab, or Mycophenolate
- Plasma exchange (for Goodpasture's / severe ANCA)
Prognosis
- Post-strep GN in children → 95% fully recover within 8–12 weeks ✅
- IgA nephropathy → variable; needs long-term follow-up
- Rapidly progressive GN → medical emergency; requires urgent treatment
- Membranoproliferative GN → >70% risk of chronic kidney failure over time
Daily Life Tips
| Do ✅ | Avoid ❌ |
|---|---|
| Take all medications as prescribed | NSAIDs (ibuprofen, diclofenac) |
| Follow low-salt diet | Smoking |
| Monitor blood pressure daily | Excess protein intake if creatinine is high |
| Attend all follow-up appointments | Unnecessary contrast dyes / nephrotoxic drugs |
| Stay hydrated (unless fluid-restricted) | Over-the-counter herbal supplements without asking your doctor |
🚨 Go to Emergency Immediately If:
- Urine is bright red or you stop urinating
- Severe facial/body swelling develops suddenly
- You develop breathlessness (may suggest lung involvement)
- Severe headache with visual changes
- Confusion or extreme fatigue
Questions to Ask Your Doctor
- What type of GN do I have?
- Do I need a kidney biopsy?
- Which medications should I avoid?
- How often do I need blood/urine monitoring?
- Can my kidney function recover fully?
- Is my condition hereditary — should my family be tested?
This material is for education purposes. Always follow the advice of your treating nephrologist.
This is a shared conversation. Sign in to Orris to start your own chat.