Cellulitis treatment
Reading File
Finding Sources
Searching PubMed
cellulitis treatment management
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive overview of cellulitis treatment based on multiple authoritative sources.
Cellulitis Treatment
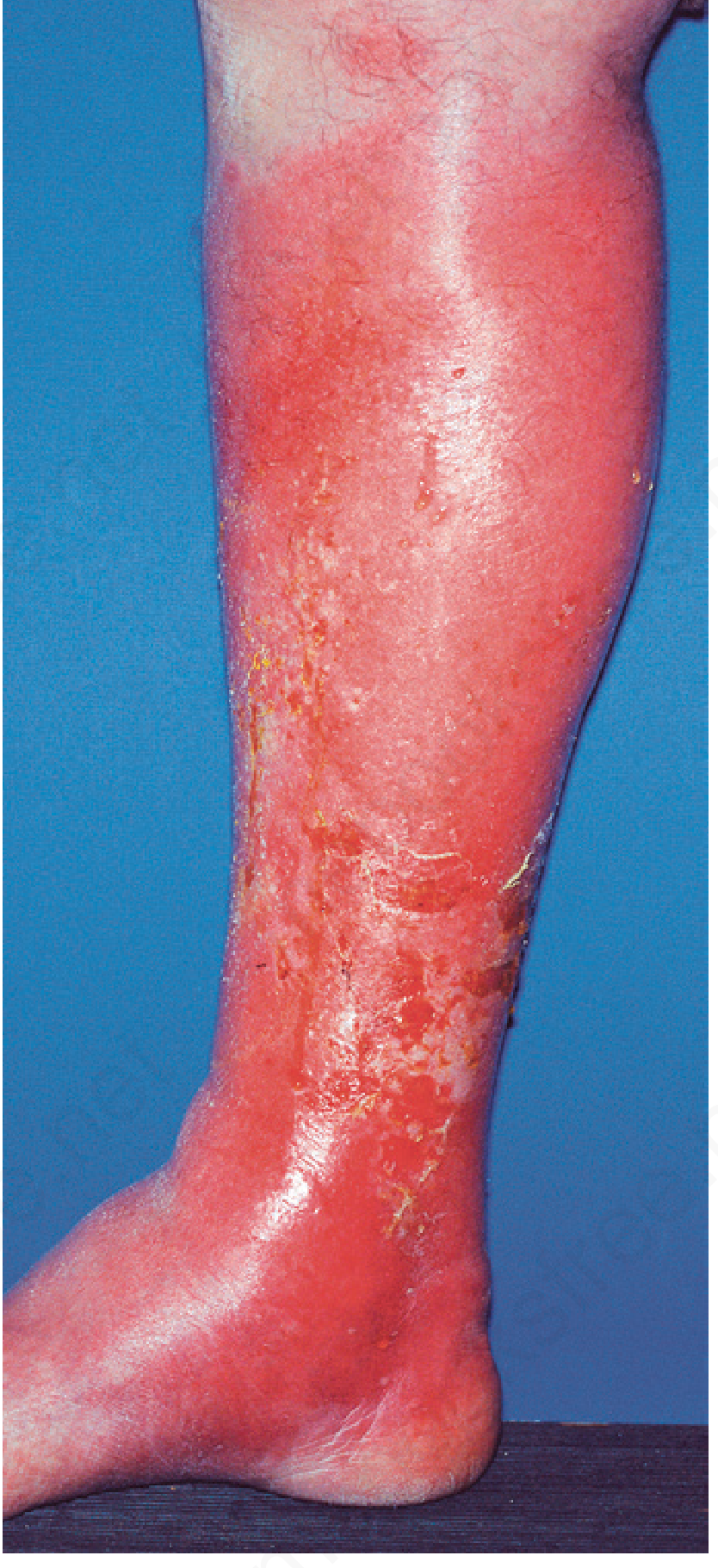
Background
Cellulitis is an acute infection of the dermis and subcutaneous tissue. The predominant pathogens are:
- Streptococcus (Group A, ~75% of cases) — typically causes nonpurulent cellulitis
- Staphylococcus aureus (including MRSA) — predominant cause of purulent cellulitis
Common portals of entry: tinea pedis, wounds, abrasions, IV drug use.
Risk factors for treatment failure: fever, lymphedema/chronic edema, chronic leg ulcers, prior cellulitis at the same site, diabetes, immunosuppression, and obesity.
Treatment Framework: Nonpurulent vs. Purulent
Treatment is guided by whether cellulitis is purulent (pus-producing) and by severity.
1. Nonpurulent Cellulitis / Erysipelas
Target organism: Streptococci
| Severity | Antibiotic | Duration |
|---|---|---|
| Mild (outpatient) | Cephalexin or dicloxacillin PO | 5–7 days |
| Moderate (non-responsive or early systemic signs) | Cephalexin PO or transition to IV | 5–7 days |
| Severe (systemic toxicity, sepsis) | Penicillin G IV, or cefazolin IV, or clindamycin IV | Admit; IV until improved, then oral step-down |
| Penicillin allergy | Clindamycin or fluoroquinolone | — |
2. Purulent Cellulitis / Soft Tissue Abscess
Target organism: Staphylococcus aureus / MRSA
| Severity | Antibiotic | Duration |
|---|---|---|
| Mild (drainable abscess, no systemic infection) | Incision & drainage alone; antibiotics often not required in healthy immunocompetent patients | — |
| Moderate (purulent cellulitis, mild-moderate systemic signs) | TMP-SMX DS 1–2 tabs PO BID, or doxycycline 100 mg PO BID, or clindamycin 300–450 mg PO QID | 7–10 days |
| Severe (systemic infection, sepsis, or immunocompromised) | Vancomycin 15 mg/kg IV q12h (MRSA coverage), or linezolid 600 mg IV q12h, or daptomycin 4 mg/kg IV q24h | Admit to hospital |
Note: Wound cultures are recommended whenever antibiotics are given. For all severe cases, rule out necrotizing fasciitis.
3. General Management Principles
- Mark the skin with an indelible marker at the perimeter of erythema to track progression or regression after starting treatment.
- Elevate the affected limb.
- Immobilize if on the hand or extremity.
- If an abscess is present, drain it — this is the primary treatment.
- Do not use the affected limb for venipuncture (risk of proximal seeding).
- POCUS (point-of-care ultrasound) is useful to distinguish deep abscess from cellulitis and guide drainage.
4. Admission Criteria
Admit patients with:
- Signs of systemic toxicity (fever, tachycardia, hypotension)
- Comorbidities: diabetes, immunosuppression, alcoholism
- Failure of outpatient oral antibiotics
- Unable to tolerate oral antibiotics
- Sepsis → consider ICU
Healthy patients without systemic toxicity can be discharged with close follow-up in 2–3 days.
5. Recurrent Cellulitis
Predisposing factors: lymphedema, venous stasis, tinea pedis, obesity, diabetes, prior saphenous vein harvest, irradiation.
- Treat active episodes with antibiotics at full doses
- Long-term suppressive antibiotics (e.g., penicillin V or erythromycin) may be used to prevent recurrence in chronic/recurrent cases
- Compression therapy to reduce lymphedema can help prevent recurrence
Recent Evidence
A 2024 network meta-analysis (PMID: 39240378) evaluated first- and second-line antibiotics for cellulitis/erysipelas across RCTs. The findings support beta-lactams as effective first-line agents for nonpurulent disease, consistent with current guidelines.
Sources:
- Tintinalli's Emergency Medicine: A Comprehensive Study, Block 13
- Andrews' Diseases of the Skin: Clinical Dermatology, Block 4
- Current Surgical Therapy 14e, Block 10
- Goldman-Cecil Medicine, Block 44
Non purulent , swelling, pain redness for 15 days , known diabetic type 2. Stenting done twice age 68
Checking Date & Time
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
This is a complex, high-risk clinical scenario. Here is a structured assessment and management plan:
Clinical Assessment
Patient profile: 68-year-old male | Type 2 DM | Prior coronary stenting ×2 | Non-purulent cellulitis ×15 days
Why This Is High-Risk
| Risk Factor | Clinical Implication |
|---|---|
| Type 2 Diabetes | Impaired leukocyte chemotaxis, phagocytosis, and bactericidal function; hyperglycemia promotes bacterial proliferation; poor wound healing |
| Age 68 + stenting ×2 | Likely peripheral vascular disease (PVD) / atherosclerosis → reduced limb perfusion → poor antibiotic delivery and tissue oxygenation |
| 15 days duration | Chronic/non-resolving course → suggests either inadequate treatment, resistant organism, or underlying deep infection (osteomyelitis, abscess, DVT) |
| Non-purulent | Primary pathogens: Group A Streptococcus; S. aureus also possible |
This patient almost certainly requires hospital admission and IV antibiotics. The combination of T2DM + 15 days no improvement = meets criteria for inpatient treatment.
Immediate Workup Required
Before finalizing antibiotics, rule out complications:
- CBC with differential — leukocytosis, left shift
- CRP / ESR — elevated in active infection and osteomyelitis
- HbA1c + fasting glucose — assess glycemic control; hyperglycemia must be corrected
- BMP/CMP — renal function (critical for vancomycin and antibiotic dosing)
- Blood cultures × 2 — yield ~5% in cellulitis, but mandatory in diabetic/immunocompromised patients
- Plain X-ray of affected area — rule out gas in soft tissue (necrotizing fasciitis), cortical erosion (osteomyelitis)
- MRI — if osteomyelitis or deep tissue involvement is suspected (probing to bone, non-healing ulcer)
- Doppler ultrasound — rule out DVT, which can mimic or co-exist with cellulitis
- ESR >70 mm/h → 11-fold higher risk of osteomyelitis in diabetic patients
Antibiotic Treatment
First-line (Admit + IV)
Nonpurulent cellulitis in a diabetic patient with comorbidity = broad-spectrum IV coverage:
| Scenario | Drug of Choice | Dose |
|---|---|---|
| Standard (no MRSA risk, no penicillin allergy) | Cefazolin IV | 1–2 g IV q8h |
| If MRSA risk factors present | Vancomycin IV | 15 mg/kg IV q12h (renal-adjusted) |
| Diabetic ulcer + cellulitis (polymicrobial concern) | Piperacillin/tazobactam IV | 3.375–4.5 g IV q6–8h |
| Penicillin-allergic | Metronidazole + ciprofloxacin | Standard dosing |
Per Dermatology 2-Volume Set 5e: "Diabetic or decubitus ulcers complicated by cellulitis require broad-spectrum coverage such as piperacillin/tazobactam, or in penicillin-allergic patients, metronidazole plus ciprofloxacin."
Coverage for MRSA does not improve outcomes for simple non-purulent cellulitis in healthy patients — but this patient is diabetic with vascular disease, changing the risk calculus.
Step-Down to Oral (when improving after 48–72h)
- Cephalexin 500 mg PO QID × 7–10 days total, OR
- Amoxicillin-clavulanate 875/125 mg PO BID (broader, good for diabetic patients)
Critical Considerations in This Patient
1. Glycemic Control
Hyperglycemia directly impairs immune function. Target glucose 140–180 mg/dL inpatient. Coordinate with endocrinology or medicine if HbA1c is high.
2. Coronary Stenting / Antiplatelet Drugs
- Patient is likely on aspirin ± clopidogrel/ticagrelor — this does NOT contraindicate treatment but:
- Avoid NSAIDs (mask fever and signs of necrotizing fasciitis, and interact with antiplatelet agents)
- Be cautious with fluoroquinolones if on anticoagulants (drug interactions)
- Monitor renal function closely if starting vancomycin (nephrotoxic)
3. Rule Out Necrotizing Fasciitis
15 days of progressive or non-resolving cellulitis in a diabetic → always exclude:
- Triad: severe pain + swelling + fever
- Pain out of proportion to exam
- Gas / crepitus on imaging
- Hemorrhagic or dark bullae → If suspected: urgent surgical consult; do NOT delay for imaging
4. Rule Out Osteomyelitis
- Probe-to-bone test if wound/ulcer present
- MRI is the gold standard
- If confirmed: prolonged antibiotic course (IV → oral, 6+ weeks)
Adjunctive Measures
- Elevate affected limb above heart level (reduces edema, improves venous return)
- Mark the erythema border daily with a skin marker to track progression or regression
- Wound care if any skin breakdown present
- No venipuncture in the affected limb
- Compression therapy once acute infection resolves, to manage underlying edema
Disposition
| Criterion | Recommendation |
|---|---|
| 15-day non-resolving course | ✅ Admit |
| Type 2 DM | ✅ Admit |
| Age + PVD (stenting ×2) | ✅ Admit |
| No systemic toxicity documented | Monitor closely; if stable, IV antibiotics + observe 24–48h |
Follow-up if outpatient is considered (not recommended here): mandatory reassessment within 24–48 hours with clear return precautions.
Sources: Tintinalli's Emergency Medicine, Block 12–13 | Dermatology 2-Volume Set 5e, Block 16 | Rosen's Emergency Medicine, Block 25 | Tintinalli's, Block 18 (Diabetic Foot)
This is a shared conversation. Sign in to Orris to start your own chat.