Glaucoma
Reading File
Asking for Preferences
Finding Sources
Searching PubMed
"glaucoma"[MeSH Terms] AND "treatment"[MeSH Terms]
Finding Sources
Searching PubMed
"glaucoma" AND "intraocular pressure" AND "therapy"
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
I now have comprehensive content from multiple authoritative sources. Here is a structured clinical overview of glaucoma treatment and management:
Glaucoma: Treatment & Management
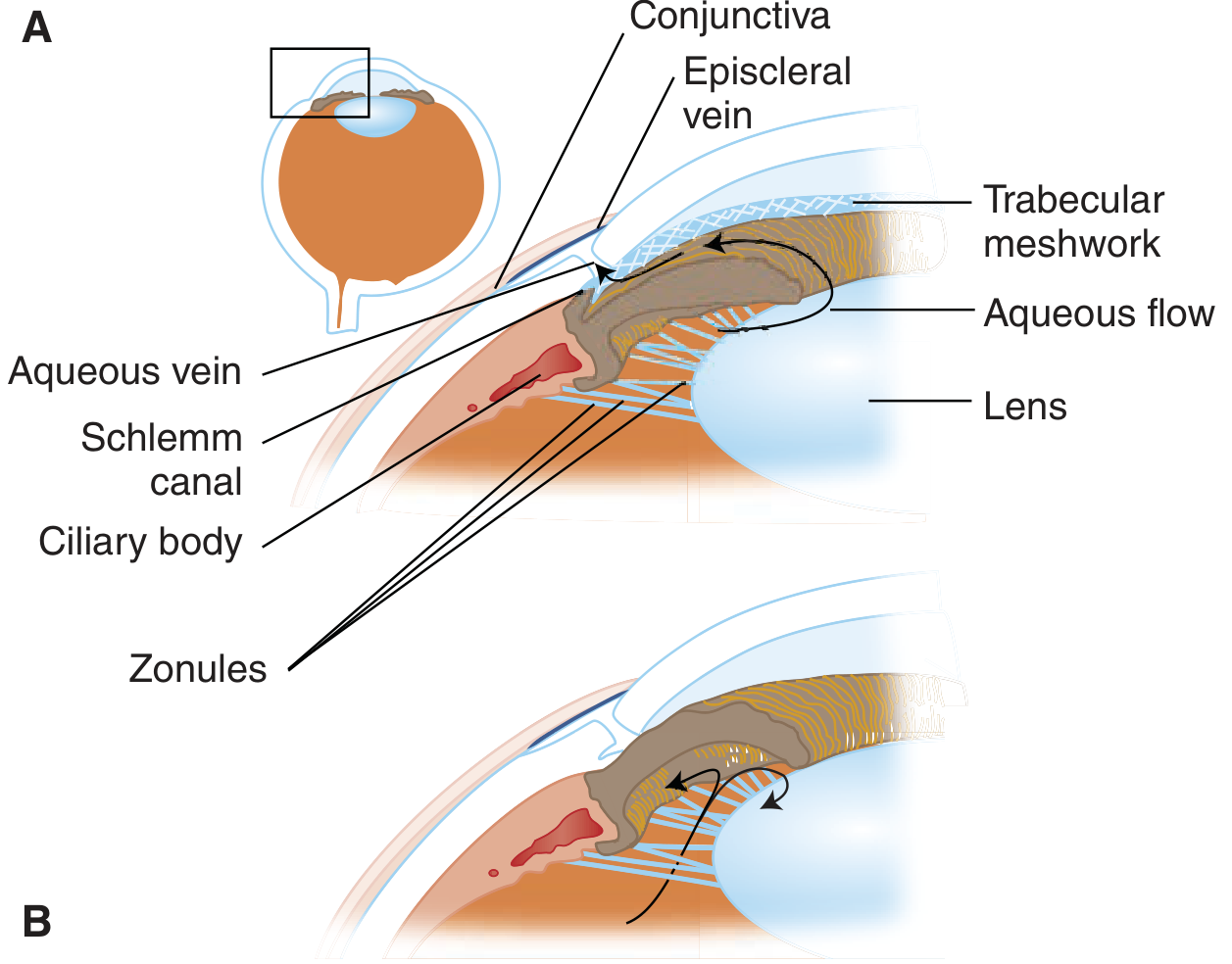
Core Principle
The sole proven intervention for all types of glaucoma is reducing intraocular pressure (IOP). Even in normal-tension glaucoma, lowering IOP delays progression. There is no pressure that is absolutely "safe" — the target is individualized. — Goldman-Cecil Medicine
1. Primary Open-Angle Glaucoma (POAG) — The Most Common Form
POAG is typically asymptomatic until late and identified on routine examination. Peripheral visual fields can be severely damaged before the patient notices.
Medical Therapy (First Line)
Drops are generally taken for life:
| Drug Class | Example | Mechanism | Dosing |
|---|---|---|---|
| Prostaglandin analogues | Latanoprost 0.005%, Travoprost 0.004%, Bimatoprost, Tafluprost | Increase uveoscleral outflow (FP receptor agonists) | Once daily |
| β-blockers (topical) | Timolol 0.5%, Betaxolol, Levobunolol, Carteolol | Reduce aqueous humor production (↓ cAMP in ciliary body) | Twice daily |
| α₂-agonists | Brimonidine 0.2% | Reduce aqueous production + increase uveoscleral outflow | 2–3× daily |
| Carbonic anhydrase inhibitors (topical) | Dorzolamide 2%, Brinzolamide | Inhibit carbonic anhydrase → ↓ aqueous production | 3× daily |
| Rho-kinase (ROCK) inhibitors | Netarsudil 0.02% | Increase trabecular outflow | Once daily |
Prostaglandin analogues are generally the preferred first-line agent due to once-daily dosing and efficacy. Adverse effects include irreversible iris/eyelash pigmentation. — Katzung's Basic & Clinical Pharmacology
Timolol warning: systemic absorption can cause bradycardia, bronchospasm, and heart block (especially when combined with verapamil). Use with caution in asthma and heart block. — Katzung's
Laser Therapy (First-Line Alternative)
- Selective Laser Trabeculoplasty (SLT) or Argon Laser Trabeculoplasty (ALT): apply energy to trabecular meshwork, improving aqueous outflow. Can maintain normal IOP for years without medications. The American Academy of Ophthalmology now considers this a first-line option. — Goldman-Cecil Medicine
Surgical Therapy (For Refractory Cases)
- Trabeculectomy — creates a fistula between anterior chamber and episcleral tissue, bypassing the trabecular meshwork
- Tube-shunt implants (glaucoma drainage devices) — anterior chamber tube drained to a reservoir behind the equator of the eye
- Both are reserved for cases not controlled with medications or laser
2. Acute Angle-Closure Glaucoma (AACG) — Ophthalmic Emergency
IOP can exceed 60–80 mmHg (normal: 10–20 mmHg). Presents with sudden severe eye pain, nausea/vomiting, halos around lights, foggy vision, fixed mid-dilated pupil, and rock-hard globe with hazy cornea.
Triggers
Anything causing pupillary dilation: anticholinergics, antihistamines, sympathomimetics (pseudoephedrine, cocaine), dim lighting, emotional stress, nebulized ipratropium + albuterol in ICU patients.
Immediate Medical Treatment (Stepwise)
| Step | Agent | Dose |
|---|---|---|
| 1st | Acetazolamide (CAI) | 500 mg IV (or 2×250 mg PO); max 1000 mg/day |
| 1st | Timolol 0.5% (topical β-blocker) | 1 drop affected eye |
| 1st | Apraclonidine 1% or Brimonidine 0.2% (α₂-agonist) | 1 drop affected eye |
| If IOP >40 after 1 hour | Mannitol 15–20% (hyperosmotic) | 1.5–2 g/kg IV over 30 min |
Pilocarpine is no longer recommended in the acute setting — cholinergic agents can paradoxically worsen angle closure. — Tintinalli's Emergency Medicine
Pain management: Fentanyl lowers IOP; ondansetron is safe for vomiting (does not affect IOP).
Definitive Treatment
- Peripheral laser iridotomy (iridectomy): creates a hole through the peripheral iris to bypass the pupillary block — definitive cure
- Prophylactic iridotomy in the fellow eye is standard practice
- Lens extraction: an alternative especially in elderly patients where lens enlargement drives angle closure
3. Secondary Glaucomas
- Post-traumatic / inflammatory (uveitic): treat underlying cause; steroids may paradoxically raise IOP
- Neovascular: treat underlying ischemia (diabetic retinopathy, CRVO); anti-VEGF + glaucoma surgery
- Sturge-Weber syndrome: Medical therapy alone may suffice; goniotomy or trabeculectomy if needed
- Aniridia-associated: Glaucoma drainage devices offer best long-term IOP control; medical treatment usually inadequate — Kanski's Clinical Ophthalmology
- Post-hemorrhage / post-surgery: observation and IOP-lowering drops first; surgical washout if needed
4. Normal-Tension Glaucoma (NTG)
IOP is within normal range but glaucomatous damage still occurs. Treatment is still IOP reduction — a 30% reduction from baseline has been shown to slow progression. Brimonidine may offer additional neuroprotection beyond IOP lowering.
Treatment Targets & Monitoring
- Target IOP is individualized based on degree of damage, age, life expectancy, and rate of progression — typically 20–30% below baseline, or even lower in advanced disease
- Monitoring with automated visual field testing (perimetry) and OCT of the retinal nerve fiber layer (RNFL) is essential for tracking progression
- Cup-to-disc ratio on fundoscopy tracks structural damage (high ratio >0.6 is suspicious)
Recent Evidence (2024–2025)
- A 2025 review (Mai et al., PMID 39787001) in Current Opinion in Ophthalmology highlights emerging glaucoma treatments including sustained-release drug delivery systems, novel ROCK inhibitors, and cell-based neuroprotection strategies
- Metformin has been proposed as a potential adjunct neuroprotectant in glaucoma (Daka et al., PMID 38536124) though this remains investigational
Sources: Goldman-Cecil Medicine 22E, Kanski's Clinical Ophthalmology 10th Ed, Katzung's Basic & Clinical Pharmacology 16th Ed, Goodman & Gilman's Pharmacological Basis of Therapeutics, Tintinalli's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.