Is weight loss beneficial to pcod
Reading File
Finding Sources
Searching PubMed
"polycystic ovary syndrome"[MeSH Terms] AND "weight loss"[MeSH Terms]
Finding Sources
Reading Article
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching the Web
weight loss benefits PCOS polycystic ovary syndrome insulin resistance hormones menstruation
Reading File
Reading File
I now have comprehensive information from authoritative textbooks and recent meta-analyses. Here's a thorough answer:
Weight Loss and PCOS (Polycystic Ovary Syndrome)
Yes — weight loss is one of the most beneficial and recommended first-line interventions for PCOS, particularly in women with overweight or obesity. Here's a breakdown of the evidence:
Why Obesity Worsens PCOS
Excess adipose tissue drives insulin resistance (IR) and hyperinsulinemia, which in turn stimulates ovarian androgen production and disrupts the hypothalamic-pituitary-ovarian (HPO) axis. This creates a cycle of worsening anovulation, elevated androgens, and irregular periods.
"The insulin resistance associated with obesity may trigger the development of polycystic ovary syndrome in susceptible individuals." — Goldman-Cecil Medicine
Benefits of Weight Loss in PCOS
Even a modest 5–10% weight loss over 6 months produces meaningful clinical improvements:
| Benefit | Details |
|---|---|
| Reduced insulin resistance | Lowers fasting insulin and HOMA-IR |
| Lower androgen levels | Reduces free testosterone and free androgen index (FAI) |
| Restored ovulation | >75% of women regain ovulatory cycles; menstrual frequency significantly improves |
| Improved fertility | Weight loss improves response to ovulation induction (clomiphene, letrozole) and ART |
| Reduced hirsutism | Lower androgens can reduce unwanted hair growth |
| Improved SHBG | Weight loss reduces SHBG suppression, further lowering free testosterone |
"Weight loss of as little as 5% to 7% over a 6-month period can reduce the bioavailable or calculated free testosterone level significantly and restore ovulation and fertility in more than 75% of women." — Berek & Novak's Gynecology
"A percentage of PCOS patients will respond to weight loss alone with spontaneous ovulation." — Berek & Novak's Gynecology
Exercise Also Plays a Role
Exercise targeting large muscle groups (e.g., thigh/lower body exercises) independently reduces insulin resistance and is an important part of lifestyle management — separate from caloric restriction.
Weight Loss as Part of a Broader Treatment Plan
Weight loss is the first step, but not always sufficient alone. For patients who don't respond to lifestyle changes, the treatment ladder includes:
- Weight loss + lifestyle modification (first-line)
- Insulin sensitizers (e.g., Metformin) — especially for anovulatory infertility and IR
- Oral contraceptives — for hirsutism and cycle regulation (if pregnancy not desired)
- Ovulation induction (letrozole or clomiphene) — for fertility
- Bariatric surgery — can even resolve PCOS in morbidly obese women
What the Latest Evidence Says (2024 Meta-Analysis)
A 2024 systematic review and meta-analysis in Annals of Internal Medicine (PMID: 39496172) — the highest-quality evidence available — analyzed 29 RCTs with 1,529 participants and found:
- Insulin resistance (HOMA-IR): Significantly improved (mean difference −0.45)
- Free androgen index: Significantly reduced (mean difference −2.03)
- Menstrual frequency: Significantly improved (+2.64 cycles)
- Hirsutism and quality of life: Not significantly improved (possibly due to underpowered studies)
Conclusion: "Weight loss interventions were associated with improvements in some important features of PCOS and should be considered as a routine treatment option."
Key Takeaway
Weight loss is beneficial, evidence-backed, and officially recommended as first-line management for PCOS in women with overweight or obesity. Even a 5–10% reduction in body weight can trigger hormonal re-balancing, restore menstrual regularity, and improve fertility — sometimes without any medication. It works primarily by reducing insulin resistance and lowering androgen levels.
The same patient have recurring blister medial to the eyes
Reading File
Finding Sources
Finding Sources
Searching the Web
recurring blister medial canthus eye inner corner differential diagnosis PCOS
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Searching Images
milia periorbital eyelid white cyst
Finding Sources
Loading Image
Loading Image
Finding Sources
Searching the Web
syringoma PCOS insulin resistance hyperandrogenism association eyelid
Reading File
Reading File
Loading Image
Reading File
I now have comprehensive information. Here is the full clinical answer:
Recurring Blister/Papule Medial to the Eye in a PCOS Patient
The location medial to the eye (inner canthal / periorbital region) with recurring lesions in a young woman with PCOS points strongly to two top diagnoses. Here's the full differential:
🥇 Most Likely: Syringoma
Syringomas are benign neoplasms arising from eccrine sweat duct proliferation. They are the most classic periorbital "blister-like" papule in young women and have a specific link to PCOS through insulin resistance.
Clinical features:
- Small (1–3 mm), firm, skin-colored to yellowish papules
- Virtually always multiple and bilateral
- Characteristically periorbital — especially lower eyelids and medial canthal area
- Female predominance; more common in Asian women
- Develop slowly, persist indefinitely, and recur after removal (hence the "recurring" pattern)
"Syringomas may occur at any site on the body but are prone to occur in the periorbital area, especially the eyelids." — Dermatology 2-Volume Set 5e
"The lesions are removed from women more commonly than men... Clear cell syringomas are associated with diabetes mellitus." — Dermatology 2-Volume Set 5e
PCOS connection: The insulin resistance and hyperinsulinemia seen in PCOS drives excessive eccrine gland stimulation and ductal proliferation. Clear-cell syringoma variant is specifically linked to metabolic/insulin dysregulation.
Classic appearance:
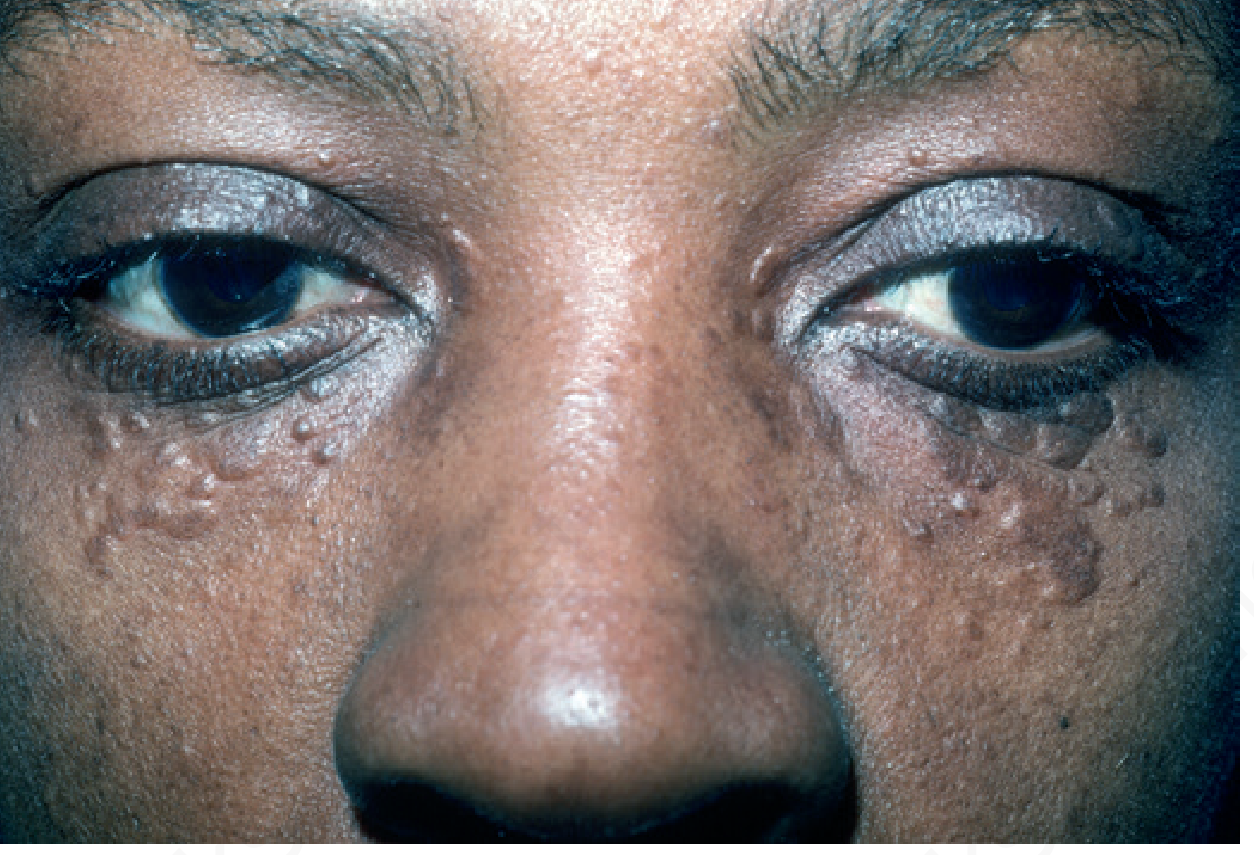
🥈 Second Most Likely: Milia
Milia are tiny keratin-filled epidermal inclusion cysts — white, 1–2 mm, dome-shaped.
Clinical features:
- Pearly white, superficial, 1–2 mm papules
- Common on the periorbital face
- Often appear after trauma, topical steroids, or cosmetic procedures
- Can recur if the underlying pilosebaceous unit keeps forming keratin plugs
"Milia. Tiny (1-2 mm), white, dome-shaped papules on the face." — Dermatology 2-Volume Set 5e
Histology: Small epidermoid cyst lined by stratified squamous epithelium with laminated keratin content.

Differential Diagnosis Table
| Feature | Syringoma | Milia | Xanthelasma |
|---|---|---|---|
| Color | Skin-colored / yellow | Pearly white | Yellow-orange plaques |
| Size | 1–3 mm | 1–2 mm | Larger, flat plaques |
| Location | Periorbital, esp. lower lid & medial | Face, periorbital | Medial canthal area |
| Texture | Firm papule | Soft, fluctuant | Flat, soft |
| PCOS link | Strong (insulin resistance) | Indirect | Yes (dyslipidemia) |
| Recurrence | Yes — persists indefinitely | Can recur | Can recur |
| Histology | Eccrine duct proliferation ("tadpole" pattern) | Keratin-filled cyst | Lipid-laden macrophages |
Kanski's Ophthalmology (definitive entry):
"Syringomas are benign proliferations arising from eccrine sweat glands. They are characterized by small papules that are often multiple and bilateral." — Kanski's Clinical Ophthalmology 10th ed.
Management
| Treatment | Notes |
|---|---|
| Light electrodessication | Most commonly used; may need repeat sessions |
| CO₂ laser ablation | Effective but recurrence possible |
| Shave removal | For larger lesions |
| Topical retinoids | For milia — reduces new lesion formation |
| Manual expression | For milia — needle incision + comedo extractor |
| Address underlying PCOS | Weight loss + insulin sensitization may reduce recurrence rate of metabolically-driven syringomas |
Key Takeaway
In a PCOS patient, recurring periorbital papules medial to the eye are most likely syringomas — driven by insulin resistance and eccrine duct hyperactivity. The "blister-like" appearance reflects the small, dome-shaped, fluid-appearing (but actually solid) nature of these lesions. Treating the underlying PCOS (weight loss, metformin) may slow new lesion formation, though existing ones require local destruction.
This is a shared conversation. Sign in to Orris to start your own chat.