oNH evaluation
Reading File
Asking for Preferences
Finding Sources
Searching the Web
optic nerve head ONH evaluation clinical assessment ophthalmology
Reading File
Finding Sources
Searching Images
optic nerve head evaluation cup disc ratio neuroretinal rim
Reading File
Searching PubMed
optic nerve head evaluation glaucoma
Reading File
Here is a comprehensive overview of Optic Nerve Head (ONH) Evaluation, drawn from Kanski's Clinical Ophthalmology (10th ed.).
Optic Nerve Head (ONH) Evaluation
1. Normal ONH Anatomy
The key structures assessed during ONH evaluation are:
| Structure | Description |
|---|---|
| Neuroretinal Rim (NRR) | Orange-pink tissue between the cup edge and disc margin |
| Optic Cup | Central pale depression within the disc |
| Optic Disc | The visible head of the optic nerve |
| Peripapillary Retina | Surrounding tissue that may show atrophic changes |
2. The ISNT Rule
The normal NRR follows a predictable width hierarchy:
Inferior > Superior > Nasal > Temporal
- Sensitivity for glaucoma: 81%, but low specificity (32%)
- Eyes without glaucoma often do not respect this rule
- A 2026 meta-analysis (PMID: 41212675) is the most recent evidence on ISNT rule diagnostic accuracy
3. Cup/Disc (C/D) Ratio
- Vertical C/D ratio is preferred over horizontal
- Only 2% of the population has a C/D ratio >0.7
- Asymmetry ≥0.2 between eyes raises suspicion for glaucoma — but always exclude a genuine difference in disc size first
- Small discs → small cups (may be normal); Large discs → large cups (may also be normal)
💡 Tip: Any cupping in a small disc may be pathological; a large disc with a large cup may be entirely healthy.
4. Optic Disc Size
- Measured by vertical diameter; normal median: 1.5–1.7 mm (white population)
- Large discs may be more susceptible to IOP-induced lamina cribrosa displacement (relevant in normal tension glaucoma, NTG)
- Disc size varies by racial group — largest in those of African descent
- Measured clinically using a slit beam + correction factor (Table 11.3 in Kanski)
5. Glaucomatous Changes at the ONH
Structural signs of glaucomatous damage:
| Sign | Description |
|---|---|
| NRR notching | Focal loss, most often inferior or superior |
| Cup enlargement | Concentric or polar |
| Disc haemorrhage | Risk factor for development and progression; requires magnification to detect |
| Baring of circumlinear vessels | Space between NRR and superficial vessel → early NRR thinning |
| Bayoneting | Double angulation of vessels due to NRR loss |
| Laminar dot sign | Exposed lamina cribrosa fenestrations in advancing glaucoma |
| Sharpened rim/edge | Sharper disc margin angle as NRR recedes |
| Loss of nasal NRR | Sign of moderately advanced damage |
| Collateral vessels | Uncommon; caused by chronic low-grade circulatory obstruction |
Classic glaucomatous subtypes (Fig. 11.9):
- Focal ischaemic — inferior notch
- Myopic — temporal crescent + inferior NRR loss
- Sclerotic — superior shelving, inferior notching
- Concentrically enlarged — deep, uniform cup enlargement
6. Peripapillary Atrophy (PPA)
Two zones surround the disc:
- Alpha zone (outer): Superficial RPE changes; larger/more common in glaucomatous eyes
- Beta zone (inner): Chorioretinal atrophy; larger, more common in glaucoma; risk factor for progression; its location predicts the orientation of visual field loss
7. Retinal Nerve Fibre Layer (RNFL)
- Arcuate fibres (superotemporal and inferotemporal) are most vulnerable to glaucomatous damage
- Papillomacular bundle fibres are most resistant
- RNFL defects (wedge-shaped or diffuse) precede detectable disc and visual field changes
- Assessed using:
- Red-free (green) light on slit lamp / fundus photography
- OCT (optical coherence tomography)
- Scanning laser polarimetry
⚠️ RNFL defects are not specific to glaucoma — they can occur in neurological disease and in apparently normal individuals.
Key Images
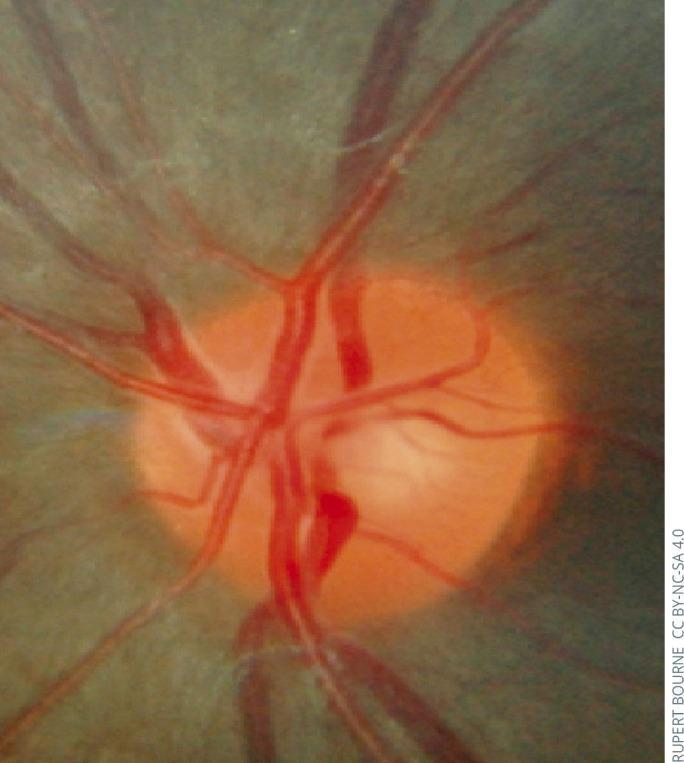
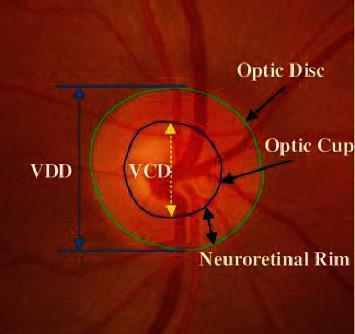
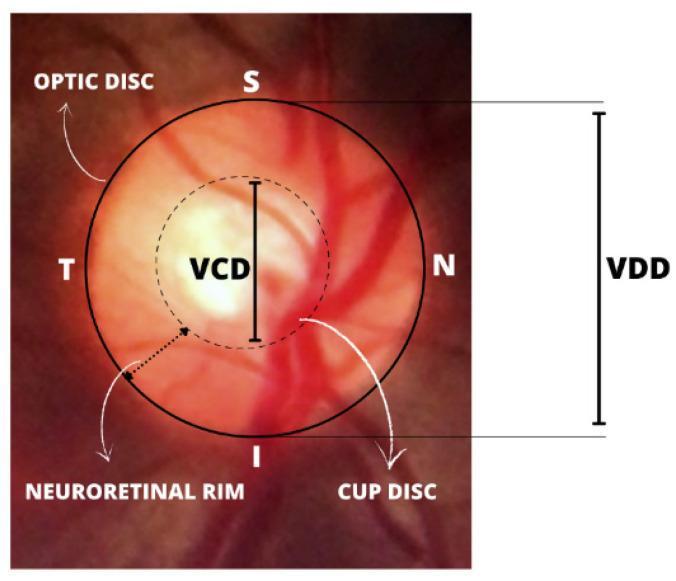
Recent Evidence Update
- PMID 41212675 (Eur J Ophthalmol, 2026): Systematic review/meta-analysis on ISNT rule — most current evidence on its diagnostic accuracy for glaucoma
- PMID 39392516 (Int Ophthalmol, 2024): Comprehensive review of ONH/RNFL imaging modalities in high myopia with glaucoma
Source: Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed., Chapter 11
Trabecu
Asking for Preferences
Finding Sources
Searching the Web
trabeculectomy surgical procedure steps indications complications ophthalmology
Reading File
Reading File
Searching PubMed
trabeculectomy outcomes complications glaucoma
Reading File
Searching Images
trabeculectomy surgical technique scleral flap bleb glaucoma
Reading File
Reading File
Here is a comprehensive overview of Trabeculectomy, based on Kanski's Clinical Ophthalmology (10th ed.).
Trabeculectomy
Trabeculectomy is glaucoma filtration surgery that lowers IOP by creating a fistula — protected by a superficial scleral flap — to allow aqueous outflow from the anterior chamber to the sub-Tenon space, forming a filtering bleb.
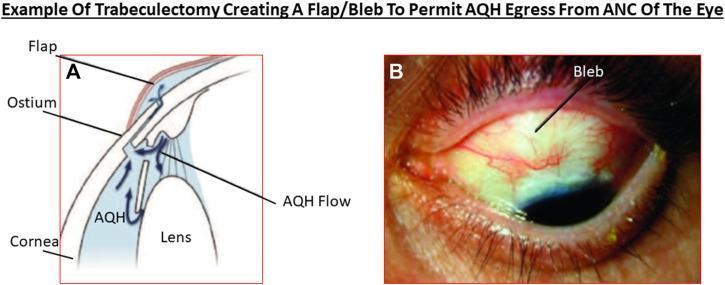
Indications
- Failure of conservative (medical) therapy to achieve adequate IOP control
- Progressive deterioration despite seemingly adequate IOP control (including poor adherence)
- Primary therapy in advanced disease requiring very low target pressure — early surgery may give superior long-term outcomes, particularly in younger patients
- Patient preference — desire to be free of chronic medication
Surgical Technique (Classical Procedure)
| Step | Detail |
|---|---|
| Preoperative | Pupil constricted with pilocarpine 2% |
| Bridle suture | Inserted at superior cornea or superior rectus |
| Conjunctival flap | Limbal or fornix-based flap fashioned superiorly (12 o'clock incision to reduce bleb dysaesthesia) |
| Episcleral prep | Episcleral tissue cleared, major vessels cauterized |
| Scleral trapdoor | Lamellar scleral flap (50% depth) created — rectangular 3×3–4 mm, trapezoidal, or triangular |
| Flap dissection | Dissected anteriorly into clear cornea |
| Paracentesis | Made in temporal peripheral clear cornea |
| AC entry | Along most of the trapdoor base width |
| Sclerectomy | Block of deep sclera excised, usually with a Kelly punch |
| Peripheral iridectomy | Created to prevent blockage of the internal sclerostomy (may be omitted in pseudophakic eyes, with caution) |
| Flap suturing | Posterior corners sutured — releasable or lysable sutures to control postoperative leakage |
| AC reformation | BSS injected through paracentesis to test fistula patency |
| Conjunctival closure | Sutured; irrigation repeated to produce a bleb, checked for leakage |
| Postoperative drops | Atropine 1%; steroids + antibiotics 4×/day for 2 weeks, then steroids alone for 8–12 weeks |
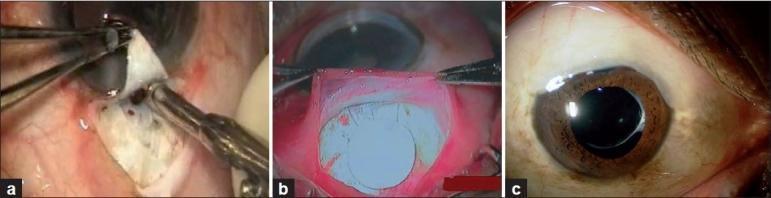
Ex-Press Mini-Shunt
A small stainless steel device inserted beneath the scleral flap as an alternative to a Kelly punch. It standardizes the size of the sclerostomy and may reduce early postoperative hypotony.
Antimetabolites in Filtration Surgery
Used to reduce subconjunctival fibrosis and improve long-term IOP control. Used with caution — only with risk factors for failure or in uncomplicated glaucoma at low doses.
Risk Factors for Surgical Failure:
- Previous failed trabeculectomy or MIGS
- Previous conjunctival or cataract surgery
- Secondary glaucoma (inflammatory, neovascular, post-traumatic)
- Black race, age <65 years
- Topical medication >3 years (especially sympathomimetics)
5-Fluorouracil (5-FU)
- Inhibits fibroblast proliferation by retarding DNA synthesis
- Intraoperative: sponge soaked in 50 mg/ml applied under Tenon flap for 5 minutes
- Postoperative: subconjunctival injection of 25–50 mg/ml solution
- Complications: persistent corneal epithelial defects, bleb leakage
Mitomycin C (MMC)
- Alkylating agent — more potent than 5-FU
- Typical: 0.2 mg/ml for 2 minutes intraoperatively; up to 0.4 mg/ml for high-risk patients
- Sponges placed away from the limbus to improve bleb profile
- Risk: cystic thin-walled bleb → chronic hypotony, late bleb leak, endophthalmitis
Bevacizumab (anti-VEGF)
- More effective than placebo, but increases risk of bleb encapsulation
- Not superior to MMC alone; combining with MMC shows no benefit
Complications
1. Shallow Anterior Chamber
Causes: pupillary block, overfiltration, or malignant glaucoma
| Cause | Management |
|---|---|
| Pupillary block | Mydriatics; Nd:YAG laser iridectomy |
| Overfiltration | Conservative; pressure dressing; AC reformation; suture tightening |
| Malignant glaucoma | Mydriatics + IV mannitol → Nd:YAG anterior hyaloid disruption → pars plana vitrectomy |
2. Failure of Filtration
Diagnosis — bleb appearances indicating failure:
- Flat, avascular bleb
- Vascularized bleb — episcleral fibrosis
- Encapsulated bleb (Tenon cyst) — localized, dome-shaped, fluid-filled, engorged vessels
Causes by site:
- Extrascleral: Subconjunctival/episcleral fibrosis; bleb encapsulation
- Scleral: Over-tight flap suturing; scleral bed scarring
- Intraocular: Sclerostomy blockage (vitreous, blood, uveal tissue, membranes)
A healthy functioning bleb is slightly elevated, relatively avascular, and shows superficial microcysts.
3. Bleb-Associated Infection
| Condition | Description |
|---|---|
| Blebitis | Infection without vitreous involvement |
| Endophthalmitis | Infection with vitreous involvement |
Blebitis symptoms: painful, red, photophobic, sticky eye
Signs: white bleb with inflammatory material, possible anterior uveitis/hypopyon; normal red reflex
Treatment (urgent):
- Conjunctival swab (do NOT aspirate from within bleb)
- Topical broad-spectrum antibiotics hourly (e.g. ofloxacin + cephalosporin)
- Oral co-amoxiclav 500/125 mg TDS + ciprofloxacin 750 mg BD for ≥5 days (or azithromycin 500 mg/day)
- Steroids only after definite antibiotic response
4. Late Bleb Leakage
- Positive Seidel test confirms aqueous leak through bleb
- Risks: thin-walled or MMC blebs
- Management: pressure dressing, bandage contact lens, surgical revision, or bleb needling with 5-FU
5. Bleb Dysaesthesia
- Discomfort from a large or anteriorly placed bleb contacting the lid
- Reduced by placing incisions at 12 o'clock
Recent Evidence
- PMID 39394492 (Graefe's, 2025): Meta-analysis — PreserFlo MicroShunt vs. trabeculectomy: comparable IOP reduction with a different complication profile
- PMID 39670502 (Dtsch Arztebl Int, 2025): MIGS vs. trabeculectomy — trabeculectomy remains the gold standard for advanced glaucoma
Source: Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed., Chapter 11
This is a shared conversation. Sign in to Orris to start your own chat.