energy conservation techniques in detail
Reading File
search_medical_text
energy conservation techniques occupational therapy chronic fatigue
search_medical_text
energy conservation strategies activities of daily living rehabilitation
GradeResponse
GradeResponse
The retrieved content is limited, so I'll supplement comprehensively from my own clinical knowledge to deliver a thorough answer.
Energy Conservation Techniques
Energy conservation (EC) is a core principle in occupational therapy and rehabilitation used to help individuals with chronic illness, fatigue, disability, or post-surgical recovery maintain functional independence while minimizing unnecessary energy expenditure. It is most commonly applied in conditions such as chronic fatigue syndrome/ME, cancer-related fatigue, COPD, heart failure, multiple sclerosis, rheumatoid arthritis, fibromyalgia, and post-COVID syndrome.
According to Cancer Pain Management in Adults (p. 33), occupational therapists assess activities of daily living (ADLs), energy conservation, anxiety management, relaxation, and lifestyle impact management as key components of comprehensive rehabilitation.
Core Framework: The 4 Ps of Energy Conservation
| Principle | Description |
|---|---|
| Prioritize | Identify which tasks are essential vs. optional; focus energy on what matters most |
| Plan | Schedule activities in advance, spreading demanding tasks across the week |
| Pace | Work at a steady, sustainable rate; avoid boom-and-bust cycles |
| Position | Use body mechanics and posture that minimize strain and energy use |
1. Activity Planning and Scheduling
- Spread heavy tasks across different days rather than clustering them.
- Alternate demanding and light activities throughout the day.
- Plan ahead — gather all supplies before starting a task to avoid repeated trips.
- Use peak energy times — schedule high-demand tasks when energy levels are naturally highest (often mid-morning for most people).
- Build in rest breaks before fatigue sets in, not after — proactive rest is more effective than reactive rest.
2. Pacing
Pacing is the process of balancing activity and rest to avoid energy crashes.
- Activity diary — track activity and fatigue levels to identify patterns and thresholds.
- Baseline establishment — determine a sustainable activity level and work within it.
- Gradual grading — increase activity by no more than 10–20% per week.
- Stop before exhaustion — halt activity at 70–80% of perceived capacity.
- Heart rate monitoring — some programs use heart rate as a physiological guide (e.g., staying below 60% of maximum heart rate during exertion).
3. Work Simplification
Work simplification involves reorganizing tasks to reduce unnecessary effort.
- Sit to work whenever possible (e.g., ironing, food preparation, grooming).
- Eliminate unnecessary steps — pre-position items, use one-trip strategies.
- Delegate or eliminate non-essential tasks.
- Use labor-saving devices: electric can openers, dishwashers, robotic vacuum cleaners.
- Batch tasks — cook multiple meals at once; do laundry in single consolidated loads.
- Organize the environment — keep frequently used items at waist height to avoid bending or reaching.
4. Posture and Body Mechanics
- Maintain neutral spine alignment during all activities.
- Sit rather than stand during prolonged tasks.
- Avoid overhead reaching — reposition shelves or use long-handled tools.
- Slide rather than lift objects along surfaces.
- Use both hands symmetrically to distribute effort.
- Support limbs on armrests or a table when performing fine motor tasks.
5. Breathing Techniques
Particularly relevant in COPD, heart failure, and respiratory conditions:
- Pursed-lip breathing during exertion — slows respiratory rate, improves gas exchange, reduces dyspnea.
- Diaphragmatic breathing — maximizes oxygen delivery at rest and during light activity.
- Coordinate breath with movement — exhale during the effort phase (e.g., exhale when pushing, lifting, or climbing a step).
- Avoid breath-holding (Valsalva maneuver) during tasks — particularly important in cardiac conditions.
6. Adaptive Equipment and Assistive Technology
| Equipment | Purpose |
|---|---|
| Long-handled reachers | Avoid bending and stretching |
| Bath seats/shower chairs | Enable seated bathing |
| Raised toilet seats | Reduce effort of sit-to-stand transfers |
| Wheeled walkers (rollators) | Reduce energy cost of ambulation |
| Electric mobility aids | Preserve energy for high-priority tasks |
| Dressing aids (sock aids, button hooks) | Reduce fine motor effort |
| Jar openers, electric tin openers | Reduce grip-force demands |
| Lightweight cookware | Reduce upper limb loading |
7. Environmental Modification
- Reorganize living/work spaces to minimize unnecessary movement.
- Move bedroom or bathroom to ground floor if stairs are a major energy drain.
- Install grab bars, ramps, and handrails to improve safety and reduce compensatory effort.
- Minimize clutter — reduces cognitive load and trip hazards.
- Good lighting — reduces visual effort and risk of falls.
- Temperature management — heat dramatically worsens fatigue in MS, heart failure, and many chronic conditions; use fans, air conditioning, or cooling vests.
8. Sleep and Rest Optimization
- Scheduled rest periods of 20–30 minutes during the day (without sleeping, to avoid disrupting nocturnal sleep).
- Good sleep hygiene — consistent sleep/wake schedule, dark/quiet environment, limited screen time before bed.
- Horizontal rest is more restorative than sitting.
- Distinguish rest from sleep — passive relaxation (lying down quietly) differs from napping; both have roles.
9. Cognitive and Emotional Energy Management
Often overlooked, cognitive and emotional effort draws on the same finite energy pool:
- Reduce decision fatigue — standardize routines, use shopping lists, pre-plan meals.
- Limit multitasking — cognitive splitting increases overall energy expenditure.
- Stress management — anxiety and emotional distress significantly amplify fatigue; techniques include mindfulness, progressive muscle relaxation, and cognitive behavioral strategies.
- Social pacing — limit overstimulating social events; communicate needs to family and friends.
10. Nutrition and Hydration
- Eat small, frequent meals rather than large ones — large meals divert blood flow to digestion and worsen fatigue.
- Maintain adequate hydration — even mild dehydration (1–2% body weight) impairs physical and cognitive performance.
- Avoid simple carbohydrates that cause energy spikes and crashes.
- Iron, B12, and vitamin D deficiencies are reversible causes of fatigue that should be screened and corrected.
Application by Condition
| Condition | Key EC Priorities |
|---|---|
| Cancer-related fatigue | Pacing, rest scheduling, activity planning, OT-guided ADL modification |
| COPD | Pursed-lip breathing during exertion, seated ADLs, pacing |
| Heart failure | Avoid Valsalva, pace stair climbing, monitor symptoms |
| Multiple sclerosis | Cooling strategies, cognitive pacing, fatigue diary |
| Rheumatoid arthritis | Joint protection techniques combined with EC |
| Post-COVID / ME-CFS | Conservative pacing, avoid post-exertional malaise (PEM), strict baseline management |
| Stroke rehabilitation | Compensatory movement strategies, assistive equipment |
Key Takeaway
Energy conservation is not about doing less — it is about doing things smarter. The goal is maximum participation in meaningful activities within a person's energy envelope, reducing unnecessary expenditure so that energy is available for what matters most. An occupational therapist is the primary professional who assesses, teaches, and tailors these strategies to an individual's specific condition, environment, and goals.
its 10markr question especiay for as
search_medical_text
energy conservation techniques nursing allied health sciences examination
GradeResponse
Here is a structured 10-mark answer on Energy Conservation Techniques, formatted for Allied Health Sciences (AHS) examinations:
Energy Conservation Techniques
Introduction
Energy conservation refers to the methods and strategies used to reduce unnecessary expenditure of energy while performing activities of daily living (ADLs), so that individuals with chronic illness, disability, or fatigue can maintain functional independence. It is a key component of occupational therapy and rehabilitation nursing.
Definition
Energy conservation is the planning and organization of activities to reduce fatigue and strain, allowing a person to accomplish more with less effort.
The 4 Ps of Energy Conservation (Core Principle)
| Principle | Meaning |
|---|---|
| Prioritize | Do only what is necessary and most important |
| Plan | Organize tasks ahead to avoid wasted effort |
| Pace | Work at a steady, moderate speed with scheduled rest breaks |
| Position | Adopt postures that minimize strain on the body |
Techniques in Detail
1. Pacing
- Alternate activity with rest before fatigue sets in.
- Avoid "boom and bust" — doing too much on good days leading to exhaustion.
- Use an activity diary to track energy levels and identify limits.
2. Activity Planning
- Schedule heavy tasks during peak energy hours (usually mid-morning).
- Spread demanding activities across the week.
- Gather all materials before starting a task to avoid repeated trips.
3. Work Simplification
- Sit to work wherever possible (e.g., cooking, grooming, ironing).
- Eliminate unnecessary steps in routines.
- Use labor-saving devices: electric appliances, trolleys, long-handled tools.
- Store frequently used items at waist level to avoid bending/reaching.
4. Correct Posture and Body Mechanics
- Maintain neutral spine alignment.
- Slide objects instead of lifting.
- Use both hands symmetrically to distribute load.
- Support limbs on surfaces during prolonged tasks.
5. Breathing Techniques
- Use pursed-lip breathing during exertion (especially in COPD).
- Exhale during effort (e.g., when pushing, lifting, climbing stairs).
- Avoid breath-holding (Valsalva maneuver) — dangerous in cardiac patients.
6. Use of Adaptive Equipment
- Bath seats, raised toilet seats, grab bars.
- Reachers, dressing aids, jar openers.
- Wheeled walkers, electric mobility aids.
7. Environmental Modification
- Reorganize home to reduce unnecessary movement.
- Good lighting, removal of clutter, installation of ramps/handrails.
- Temperature control — heat worsens fatigue in conditions like MS and heart failure.
8. Rest and Sleep Management
- Schedule 20–30 minute rest periods during the day.
- Maintain good sleep hygiene.
- Horizontal rest is more restorative than sitting.
9. Psychological and Cognitive Strategies
- Reduce decision fatigue by standardizing daily routines.
- Manage stress through relaxation techniques (deep breathing, progressive muscle relaxation).
- Avoid multitasking — it increases total energy cost.
10. Nutrition and Hydration
- Eat small, frequent meals to avoid post-meal fatigue.
- Stay well-hydrated — even mild dehydration worsens fatigue.
- Correct nutritional deficiencies (iron, B12, vitamin D).
Conditions Where Energy Conservation is Applied
| Condition | Focus Area |
|---|---|
| Cancer-related fatigue | Pacing, OT-guided ADL modification |
| COPD | Breathing techniques, seated ADLs |
| Heart failure | Avoid Valsalva, monitor exertion |
| Multiple Sclerosis | Cooling, cognitive pacing |
| Rheumatoid Arthritis | Joint protection + energy conservation |
| Post-COVID / ME-CFS | Strict pacing, avoid overexertion |
Role of the Allied Health Professional
- Occupational Therapist (OT): Assesses ADLs, teaches energy conservation, recommends adaptive equipment and home modifications.
- Physiotherapist: Graded exercise, breathing techniques, mobility aids.
- Rehabilitation Nurse: Educates patient and family, monitors fatigue levels, supports implementation in daily care.
Conclusion
Energy conservation techniques are essential tools in rehabilitation and chronic disease management. The primary goal is not to do less, but to do more efficiently — preserving energy for meaningful and priority activities. These strategies are individualized, taught by the occupational therapist, and practiced in real-life settings to maximize patient independence and quality of life.
Word tip for exam: Write the 4 Ps first — examiners look for that framework. Then cover at least 6–7 techniques with brief explanation each. A table for conditions or equipment always scores well.
saturday niht palsy
Reading File
search_medical_text
Saturday night palsy radial nerve compression wrist drop
search_medical_text
radial nerve anatomy spiral groove humerus palsy management
search_medical_image
radial nerve wrist drop Saturday night palsy
GradeResponse
GradeResponse
GradeResponse
Saturday Night Palsy
Definition
Saturday night palsy is a compressive neuropathy of the radial nerve at the spiral groove of the humerus, caused by prolonged external pressure on the upper arm. The name comes from the classic scenario of a person falling asleep in an awkward position — typically with the arm draped over a chair or bench after alcohol intoxication — compressing the nerve for hours.
Anatomy Relevant to the Injury
- The radial nerve (C5–C8, T1) is a branch of the posterior cord of the brachial plexus.
- It winds around the posterior aspect of the humerus in the spiral (radial) groove, making it vulnerable to compression against bone.
- Below the spiral groove, it divides into:
- Posterior interosseous nerve (motor — extensors of wrist, fingers, thumb)
- Superficial radial nerve (sensory — dorsal hand and thumb web space)
- The triceps is supplied proximal to the spiral groove — so it is typically spared in Saturday night palsy.
Causes / Precipitating Factors
| Cause | Example |
|---|---|
| Alcohol intoxication with arm over chair | Classic "Saturday night" scenario |
| Deep sleep (drug overdose, sedation) | Arm compressed under body or against hard surface |
| Prolonged use of axillary crutches | Crutch palsy |
| Tourniquet application | Surgical or makeshift tourniquet |
| Honeymoon palsy | Partner sleeping on the other's arm |
| Fracture of humerus | Direct nerve injury at spiral groove |
Pathophysiology
Prolonged compression at the spiral groove causes neuropraxia — a temporary conduction block without axonal disruption. In severe or prolonged cases, axonotmesis (axonal damage with intact sheath) can occur, requiring longer recovery. According to Harrison's Principles of Internal Medicine (21st ed., p. 12707):
"Most cases of radial neuropathy are transient compressive (neuropraxic) injuries that recover spontaneously in 6–8 weeks. If there has been prolonged compression and severe axonal damage, it may take several months to recover."
Clinical Features
Motor (Characteristic Sign — Wrist Drop)
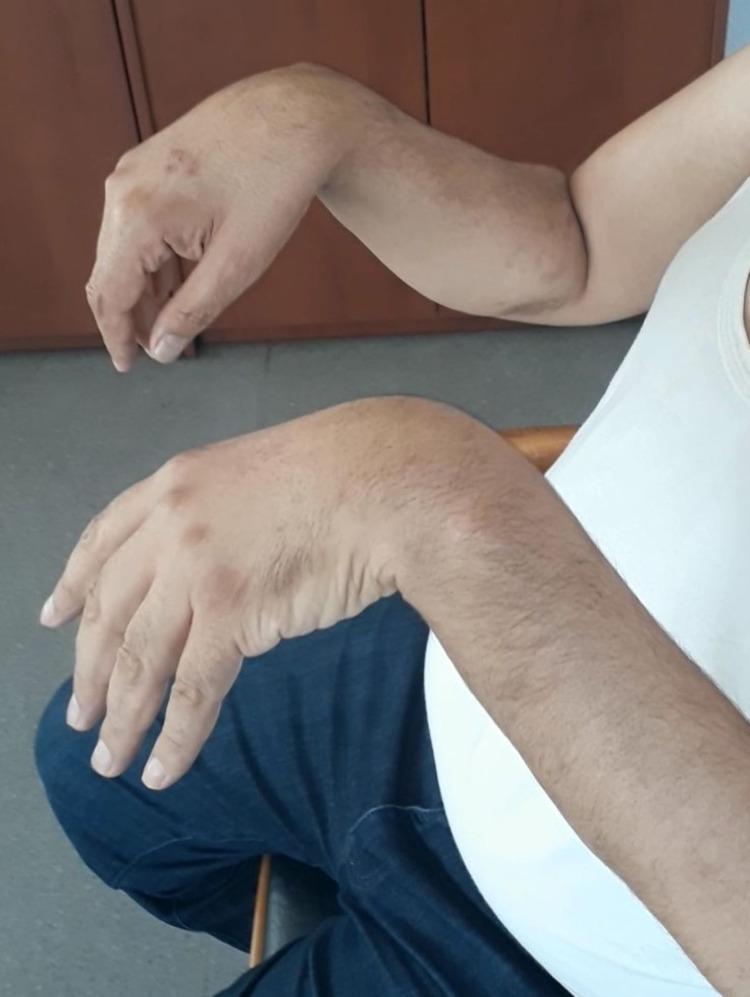
- Wrist drop — inability to extend the wrist (hallmark sign)
- Finger drop — inability to extend fingers at MCP joints
- Thumb abduction weakness — weakness of extensor pollicis longus/brevis and abductor pollicis longus
- Brachioradialis weakness — weak elbow flexion in mid-prone position
Motor — Spared (Key Exam Point)
- Triceps power is NORMAL — nerve is compressed below the branch to triceps
- Triceps reflex is INTACT
- Intrinsic hand muscles are NORMAL (supplied by ulnar and median nerves)
Sensory
- Loss of sensation over the dorsal web space between thumb and index finger (anatomical snuff box region)
- Sensory loss over dorsum of hand and lateral forearm (variable)
Summary of Clinical Features Table
| Feature | Finding |
|---|---|
| Wrist drop | Present |
| Finger extension at MCP | Lost |
| Thumb extension/abduction | Weak |
| Triceps power | Normal |
| Triceps reflex | Intact |
| Grip strength | Reduced (due to poor wrist position) |
| Sensation — dorsal web space | Reduced/absent |
| Intrinsic hand muscles | Normal |
Diagnosis
- Clinical diagnosis based on history (prolonged compression) + wrist drop + spared triceps.
- Electrodiagnostic (EDx) studies — NCS (nerve conduction study) and EMG:
- Indicated if no improvement within 2–3 weeks (Harrison's, p. 12707)
- Differentiates neuropraxia from axonotmesis
- Helps determine severity and prognosis
- X-ray — if humeral fracture is suspected.
Differential Diagnosis
| Condition | Differentiating Feature |
|---|---|
| Posterior interosseous nerve palsy | No sensory loss; wrist extension partially preserved (radial deviation) |
| C7 radiculopathy | Neck pain, reflexes altered, triceps may be weak |
| Lead poisoning neuropathy | Bilateral, associated systemic features |
| Stroke/cortical lesion | Upper motor neuron signs, face/leg also involved |
| Brachial plexus injury | Wider distribution of weakness |
Treatment
Immediate
- Remove the compressing cause — reposition the limb, remove tight bandages/splints.
- Cock-up (wrist extension) splint — holds wrist in extension to restore functional grip and prevent flexion contracture (Harrison's, p. 12707).
- Finger extension splint as needed.
Rehabilitation
- Physiotherapy — passive and active ROM exercises to maintain joint mobility.
- Avoid flexion contracture of wrist and fingers — key goal of early therapy.
- Occupational therapy — functional training, adaptive aids during recovery.
Follow-up
- If no improvement in 2–3 weeks → EDx studies.
- If axonotmesis confirmed → prolonged physiotherapy; recovery may take months.
- Surgical decompression — rarely needed; considered if structural compression (e.g., callus from healed fracture) is identified.
Prognosis
| Type of Injury | Expected Recovery |
|---|---|
| Neuropraxia (most cases) | Full recovery in 6–8 weeks |
| Axonotmesis | Several months; recovery depends on extent of axonal damage |
| Neurotmesis (rare, severe trauma) | Poor; may require surgical repair |
Conclusion
Saturday night palsy is a compressive radial neuropathy at the spiral groove of the humerus, presenting classically with wrist drop and finger drop with sparing of the triceps. The majority of cases are neuropraxic and recover fully within 6–8 weeks with conservative management — splinting, physiotherapy, and avoidance of further compression. EDx studies guide prognosis when recovery is delayed.
Exam tip: The key distinguishing feature examiners test — triceps is spared because the branch to triceps arises proximal to the spiral groove. Always mention this to score full marks.
This is a shared conversation. Sign in to Orris to start your own chat.