Bishops score and it's indications regarding delivery and induction
Reading File
Finding Sources
Finding Sources
Searching PubMed
"Bishop score" AND "labor induction"
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive overview of the Bishop Score and its role in delivery and induction of labor.
Bishop Score (Pelvic Scoring for Elective Induction of Labor)
The Bishop score, introduced by Dr. Edward H. Bishop in 1964 (Obstet Gynecol. 1964;24:266), is a standardized pre-labor cervical assessment tool used to predict the likelihood of successful labor induction and vaginal delivery.
The Scoring System
Five cervical parameters are assessed digitally. Each is assigned 0–3 points:
| Parameter | 0 | 1 | 2 | 3 |
|---|---|---|---|---|
| Dilation | Closed | 1–2 cm | 3–4 cm | ≥5 cm |
| Effacement | 0–30% | 40–50% | 60–70% | ≥80% |
| Station | −3 | −2 | −1/0 | +1/+2 |
| Consistency | Firm | Moderate | Soft | — |
| Position | Posterior | Mid | Anterior | — |
Maximum score: 13
Dilation is considered the single most predictive component; Lange et al. (808 patients) recommended scoring it at twice its assigned value. — Creasy & Resnik's Maternal-Fetal Medicine
Score Modifiers
Add 1 point for:
- Preeclampsia
- Each prior vaginal delivery
Subtract 1 point for:
- Postdates pregnancy
- Nulliparity
- Premature or prolonged rupture of membranes (PROM)
Interpretation & Clinical Thresholds
| Score | Cervical Status | Clinical Implication |
|---|---|---|
| ≥9 | Favorable/Ripe | Induction success approaches spontaneous labor; average labor ~4 hours in multiparas. No failed inductions in Bishop's original multipara series |
| >8 | Favorable | Likelihood of successful vaginal delivery with oxytocin approximates spontaneous labor |
| 6–8 | Intermediate | Induction may succeed; cervical ripening may be considered |
| <6 | Unfavorable | Correlates with prolonged labor or failed induction; cervical ripening strongly recommended before oxytocin |
| ≤5 | Unfavorable | 50% risk of failed induction in nulliparous women at term |
— Pfenninger & Fowler's Procedures for Primary Care; Creasy & Resnik's MFM
Indications for Induction of Labor (where Bishop Score guides management)
Induction is indicated when benefits of delivery outweigh risks of continuing pregnancy:
Maternal indications:
- Pregnancy-induced hypertension, preeclampsia, eclampsia (>80% of inductions)
- Prolonged/post-term pregnancy (>40–42 weeks)
- Maternal medical complications: diabetes mellitus, renal disease, chronic pulmonary disease, chronic hypertension
Obstetric/fetal indications:
- Abruptio placentae
- Chorioamnionitis
- Abnormal antepartum testing requiring delivery
- Premature rupture of membranes (PROM)
- Fetal demise
- Isoimmunization
Elective/logistic indications (not routinely recommended but acceptable):
- Distance from hospital
- History of rapid labor/precipitous delivery
- Psychosocial factors
- To ensure presence of familiar physician/staff
Contraindications to Induction
Absolute
- Placenta previa or vasa previa
- Transverse fetal lie
- Prolapsed umbilical cord
- Previous classical (vertical) uterine incision
- Severe hydrocephalus
- Active genital herpes
- Invasive cervical carcinoma
- Non-reassuring fetal status
- Known hypersensitivity to prostaglandins
Relative
- Multiple gestation
- Polyhydramnios
- Appreciable macrosomia
- Maternal cardiac disease
- Previous uterine surgery (non-classical)
Management Based on Bishop Score
Bishop Score ≥8–9
→ Proceed directly with oxytocin or amniotomy
Bishop Score <6
→ Cervical ripening first:
Mechanical: Foley balloon catheter, laminaria
Pharmacologic: Dinoprostone (PGE₂), Misoprostol (PGE₁)
→ Then reassess → oxytocin if appropriate
Key points:
- Amniotomy alone is effective when the cervix is favorable (Bishop ≥8); only 3.4% require additional oxytocin in such patients (Keettel series)
- If oxytocin is needed, a minimum of 12 hours of stimulation after membrane rupture should be required before diagnosing failed induction
- Elective induction carries a ~2× increased cesarean risk in nulliparas with an unfavorable cervix — this risk is nearly eliminated with a favorable cervix
Simplified Bishop Score
Laughton et al. (using the Consortium on Safe Labor database, 5610 nulliparas) validated a simplified 3-component score using only dilation, effacement, and station (range 0–9). This had better positive and negative predictive values than the traditional 5-component score.
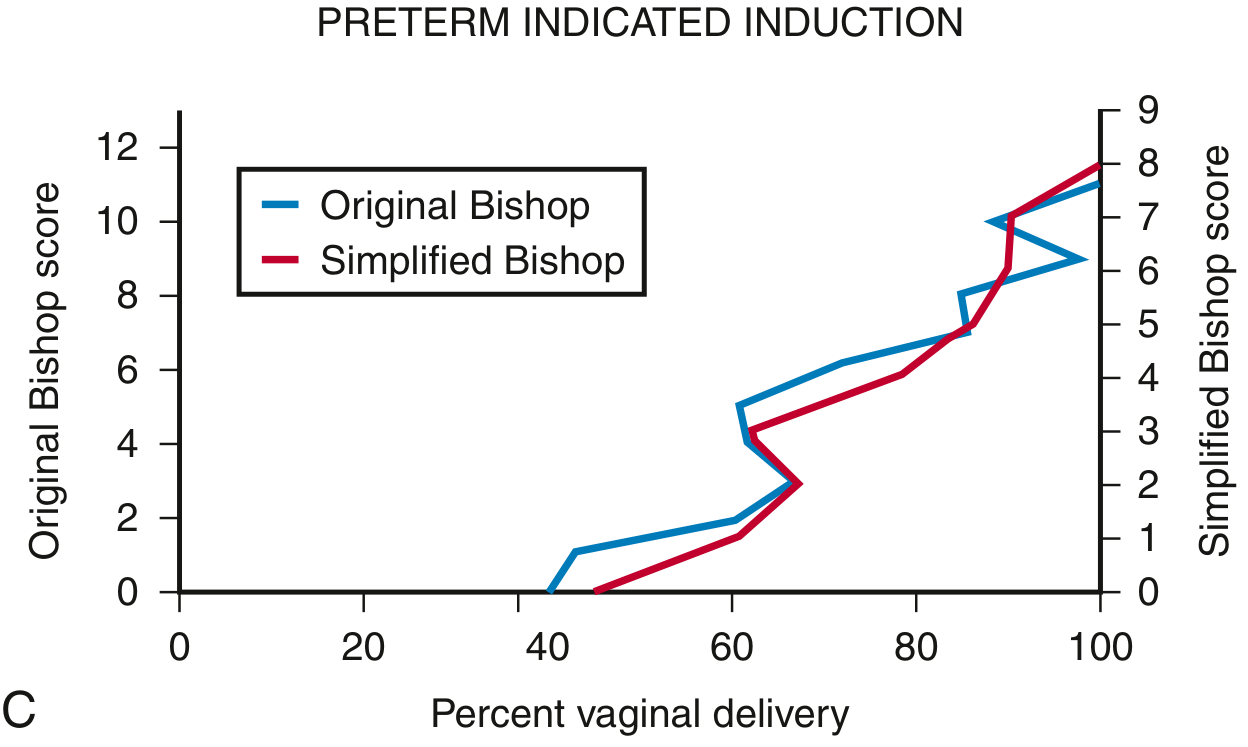
Figure: Original Bishop score (left y-axis, 0–13) vs Simplified Bishop score (right y-axis, 0–9) correlated with percent vaginal delivery in preterm indicated inductions. Both systems track closely, validating the simplified approach. — Creasy & Resnik's MFM
Bishop Score & Prediction of Preterm Birth
Beyond induction planning, the Bishop score (via digital cervical examination) has also been studied as a predictor of spontaneous preterm birth, though transvaginal ultrasound cervical length measurement is generally superior for this purpose. — Creasy & Resnik's MFM
Recent Evidence
A 2026 global systematic review and meta-analysis (PMID: 41485908) assessed the accuracy of both preinduction transvaginal sonography and Bishop scores in predicting successful labor induction, confirming ongoing clinical relevance of the Bishop score alongside ultrasound-based cervical assessment. The traditional Bishop score remains the standard clinical tool despite newer modalities.
Sources: Textbook of Family Medicine 9e; Pfenninger & Fowler's Procedures for Primary Care; Creasy & Resnik's Maternal-Fetal Medicine (Principles and Practice)
This is a shared conversation. Sign in to Orris to start your own chat.