Intervertebral disk anatomy blood supply embryology full details for 10 marks
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
I now have all the information needed for a comprehensive 10-mark answer. Here is the full structured response:
Intervertebral Disc — Anatomy, Blood Supply & Embryology
1. Overview
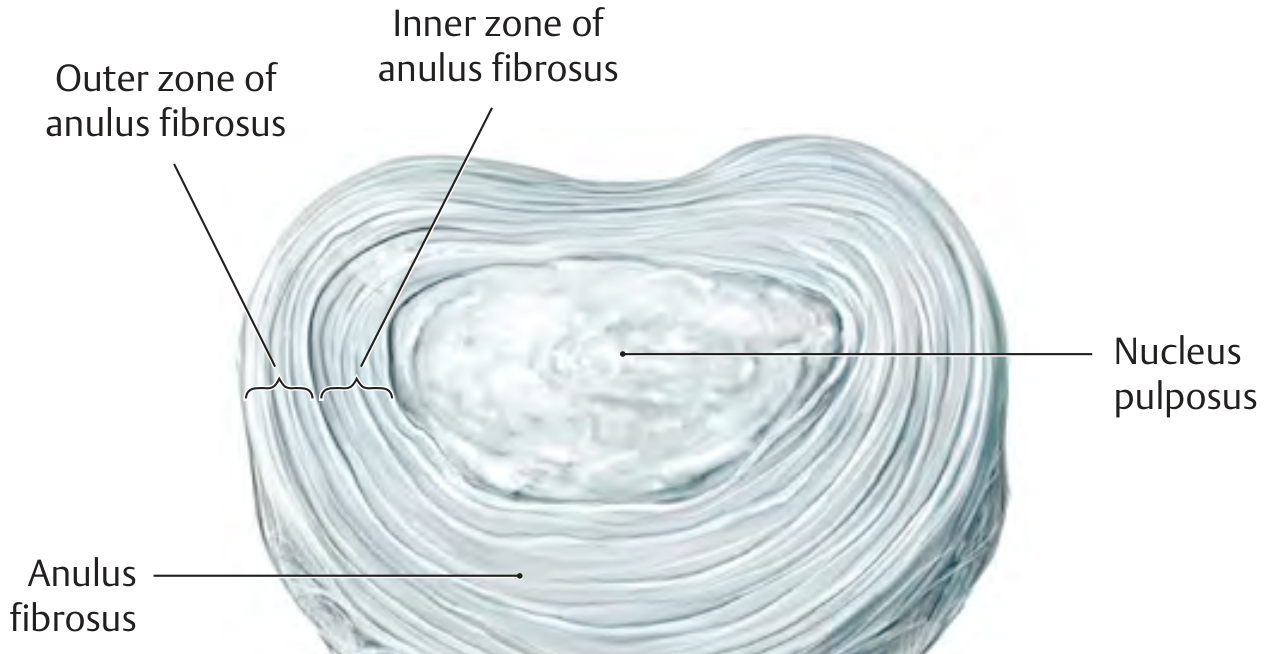
The intervertebral disc (IVD) is a fibrocartilaginous joint (symphysis) located between adjacent vertebral bodies from C2–C3 to L5–S1 (23 discs total). It functions as a shock absorber, load distributor, and permits spinal motion. It has two principal structural components: the annulus fibrosus and the nucleus pulposus, both resting on hyaline cartilage end plates superiorly and inferiorly.
2. Anatomy
A. Annulus Fibrosus
- The outer, tough ring encircling the disc.
- Composed of 15–25 concentric lamellae of collagen fibers arranged obliquely, with adjacent lamellae oriented in opposing directions (~30° to the disc plane). This crisscross arrangement confers high tensile strength in multiple directions.
Two zones:
| Feature | Outer Zone | Inner Zone |
|---|---|---|
| Collagen type | Type I (high) | Type II |
| Tissue | Dense fibrous | Fibrocartilaginous |
| Attachment | Marginal bony ridges (Sharpey's fibers into epiphyseal ring) | Hyaline cartilage end plates |
| Blood supply | Present (some) | Avascular |
| Nerve supply | Sinuvertebral nerve (outer 1/3) | None |
- The outer zone is a fibrous sheath with high tensile strength; its fiber bundles interconnect the marginal ridges of two adjacent vertebrae.
- At the junction with the inner zone, the tough fibrous tissue blends with fibrocartilaginous tissue whose type II collagen fibers attach to the hyaline cartilage end plates.
- The superficial layer of the annulus fibrosus contains nerve fibers (nociceptive — source of discogenic pain).
B. Nucleus Pulposus
-
The central, gelatinous, hydrophilic core of the disc.
-
Composition:
- Water: 80–85% (highest in children; decreases with age)
- Proteoglycans (aggrecan, chondroitin sulfate, keratan sulfate — responsible for the high osmotic pressure and water-binding capacity via glycosaminoglycans/GAGs)
- Type II collagen (~20% of dry weight)
- Scattered notochordal/vacuolated cells (the only remnant of the embryonic notochord to persist postnatally — relatively large in children, diminishes with age)
- Hyaluronan
-
Acts as a hydraulic press / water cushion: the high hydrostatic pressure within the nucleus redistributes compressive axial loads radially, which the annulus converts into tensile (hoop) stress.
-
Under sustained load, fluid slowly exits through the end plates → disc height decreases (~1–1.5 cm diurnal height loss). When pressure is released, fluid re-enters from subchondral bone marrow vessels.
C. Cartilage End Plates
- Thin (~0.6 mm) layers of hyaline cartilage covering the superior and inferior surfaces of each vertebral body.
- Interface between vertebral body and disc.
- The subchondral bony portion of the end plate is permeated by myriad pores (vascular channels) through which bone marrow vessels supply nutrients to the disc by diffusion.
- Type II collagen fibers of the inner annulus attach to these end plates.
D. Functional Biomechanics
- The nucleus pulposus + annulus fibrosus act together as an effective shock absorber, uniformly distributing pressures over adjacent end plates.
- The annulus fibrosus transforms compressive forces into tensile forces (hoop stress), resisting radial bulging of the nucleus.
- Mechanically, the disc is a hydrostatic system: resilient under pressure due to its tension-resistant sheath (annulus) and incompressible watery core (nucleus).
3. Blood Supply
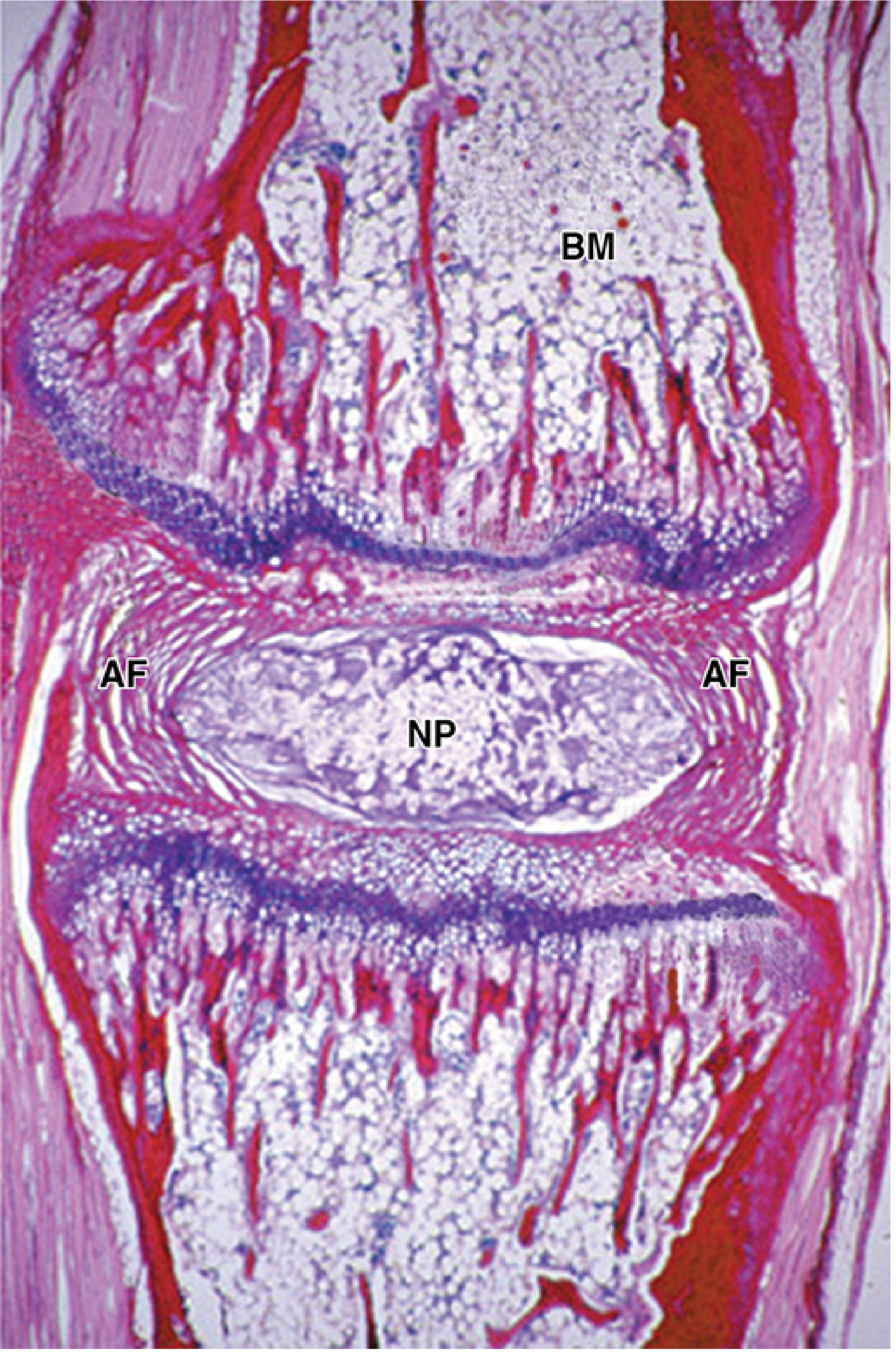
The IVD is one of the largest avascular structures in the body. Its nutrition depends entirely on diffusion rather than direct vascular supply.
In Adults:
| Region | Vascularity |
|---|---|
| Nucleus pulposus | Completely avascular |
| Inner annulus fibrosus | Avascular |
| Outer annulus fibrosus | Receives some blood supply from small radial capillary loops |
Route of Nutrient Supply:
- Vertebral end plate route (primary): Subchondral capillaries in the bone marrow spaces of adjacent vertebral bodies penetrate the porous bony end plate and supply nutrients (glucose, oxygen) and remove metabolic waste (lactate) by diffusion through the cartilage end plate into the disc. This is the dominant pathway.
- Peripheral annular route (secondary): Small blood vessels from the perivertebral plexus penetrate the outermost lamellae of the annulus fibrosus.
Key Points:
- Pressure-dependent convection (fluid shifts during loading/unloading) augments passive diffusion by creating a "pumping" mechanism that drives solute transport.
- The avascular nature of the nucleus pulposus renders it immunologically privileged and makes it vulnerable to degeneration when diffusion is compromised (e.g., end plate calcification, smoking, atherosclerosis of segmental arteries).
- With age, loss of proteoglycans → loss of hydration → desiccation and disc degeneration.
In Fetuses/Neonates:
- Vascular channels extend into the disc tissue (especially the end plate region) in early life.
- These vessels regress by the 2nd decade, leaving the disc avascular.
4. Embryology
Overview of Vertebral Column Development
| Stage | Timing | Events |
|---|---|---|
| Mesenchymal | Week 4 | Sclerotome migration; notochord present |
| Cartilaginous | Week 6 | Chondrification centers appear |
| Bony/Ossification | Week 8 onwards | Primary ossification centers |
Step-by-Step Development:
Week 3 — Notochord Formation:
- The notochord forms as a midline axial structure derived from epiblast cells that pass through the primitive node (Hensen's node). It is a defining chordate characteristic and serves as the initial axial skeleton and inducer of the neural plate.
Week 4 — Somite Differentiation and Sclerotome Migration:
- Paraxial mesoderm segments into somites, which differentiate into:
- Myotome (muscles)
- Dermatome (skin)
- Sclerotome (vertebrae and ribs)
- Sclerotome cells separate and migrate medially toward the notochord, forming paired condensations of mesenchymal cells around it — the anlage of the future spinal column.
- Each sclerotome consists of loosely arranged cranial cells and densely packed caudal cells.
Intervertebral Disc Formation (Resegmentation):
- Some densely packed cells from the caudal portion of each sclerotome migrate cranially (opposite the center of the adjacent myotome) → these form the intervertebral disc primordium.
- The remaining densely packed cells fuse with the loosely arranged cells of the immediately caudal sclerotome → form the mesenchymal centrum (body of a vertebra).
- Thus, each vertebral body forms from parts of two adjacent sclerotomes (intersegmental structure), while the IVD forms at the level of the original segment.
- This resegmentation ensures that segmental nerves lie next to intervertebral discs (and thus adjacent to the intervertebral foramina), while intersegmental arteries lie on each side of the vertebral bodies → these become the nutrient vessels of the vertebral bodies by week 10.
Nucleus Pulposus — from Notochord:
- As vertebral bodies develop, the notochord is surrounded and degenerates within the centra.
- Between the vertebrae, the notochord expands to form the gelatinous, hydrophilic nucleus pulposus.
- Notochordal remnant cells persist within the nucleus pulposus postnatally (vacuolated notochordal cells), but are gradually replaced by fibrocartilaginous cells with aging.
Annulus Fibrosus — from Mesoderm (Sclerotome):
- The densely arranged mesenchymal cells surrounding the expanding notochord become circularly arranged fibers → the annulus fibrosus.
- Derived from mesoderm (sclerotome), not notochord.
- Chondrification of the vertebral centra begins in week 6, displacing notochordal material into the future disc spaces.
- Ossification of vertebral bodies begins in week 8.
Summary Table: Embryological Origins
| Component | Embryological Origin |
|---|---|
| Nucleus pulposus | Notochord (ectoderm of notochordal process) |
| Annulus fibrosus | Mesoderm (sclerotome of paraxial mesoderm) |
| Cartilage end plates | Mesoderm (sclerotome) |
| Vertebral body | Mesoderm (two adjacent sclerotomes — resegmentation) |
Clinical Correlate — Chordoma:
Remnants of the notochord that fail to regress may persist and form a chordoma — a rare, slow-growing malignant tumor. ~1/3 occur at the base of cranium (clivus, extending to nasopharynx); others occur in the lumbosacral region. They infiltrate bone and are difficult to resect.
Clinical Correlate — Disc Herniation:
Loss of or degenerative changes in annulus fibrosus collagen allow the nucleus pulposus to herniate, most commonly posterolaterally (where fewer collagen bundles are present). Compression of adjacent nerve roots produces radiculopathy. — Junqueira's Basic Histology, p. 393
Quick-Recall Summary for Exams
| Point | Key Fact |
|---|---|
| Type of joint | Secondary cartilaginous (symphysis) |
| Annulus collagen | Outer = Type I; Inner = Type II |
| Nucleus water content | 80–85% |
| Nucleus collagen | Type II (20% dry weight) |
| Blood supply (adult) | Avascular (NP); some supply to outer AF only |
| Nutrient route | Diffusion via cartilage end plates (primary) |
| NP embryological origin | Notochord |
| AF embryological origin | Mesoderm (sclerotome) |
| Nerve supply | Outer 1/3 of AF (sinuvertebral nerve) |
| Tumour of notochord remnant | Chordoma |
Sources:
- THIEME Atlas of General Anatomy and Musculoskeletal System — Section 1.9
- The Developing Human: Clinically Oriented Embryology — Chapter 14 (Moore & Persaud)
- Junqueira's Basic Histology, 17e — Chapter 8 (Joints)
- Miller's Review of Orthopaedics, 9e — Neural Tissue & IVD
- Goldman-Cecil Medicine — Pathobiology of the Spine (Ch. 369)
This is a shared conversation. Sign in to Orris to start your own chat.