Case presentation history , examination, negative history of tb lymph node swelling
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
I now have comprehensive content to construct a detailed case presentation. Let me compile everything.
Case Presentation: Tuberculous Lymphadenitis (TB Lymph Node Swelling)
📋 Presenting Complaint
A young woman (or adolescent/young adult) presents with a painless, progressively enlarging swelling in the neck of several weeks' duration.
🗒️ History of Presenting Illness
- Painless neck swelling — gradual onset over weeks to months
- Located in the posterior cervical chain or supraclavicular fossa (most common); may be bilateral
- The swelling has been slowly increasing in size
- No acute pain over the swelling initially; skin overlying the node appears normal early on
- Later: node may become matted, firmer, with overlying skin becoming inflamed
- If advanced: fluctuance, abscess formation, or sinus tract discharging through the skin
Systemic (Constitutional) Symptoms
- Low-grade fever, often diurnal (worse in afternoons/evenings)
- Night sweats
- Weight loss / anorexia
- General malaise and weakness
- Systemic symptoms are often absent or mild in isolated lymphadenitis
⛔ Negative History (Pertinent Negatives)
This is essential to document in TB lymphadenitis:
| Feature | Absent (Negative) |
|---|---|
| Cough | No cough or minimal dry cough |
| Hemoptysis | None |
| Chest pain / dyspnea | None |
| Painful lymph node | Node is characteristically painless |
| Rapid growth | Swelling is slow/gradual, not acute |
| Sore throat / odynophagia | None (rules out tonsillitis/peritonsillar) |
| Preceding URTI | No recent upper respiratory tract infection |
| Animal contact / cat scratch | None (rules out cat-scratch disease) |
| Skin rash / joint pains | None (rules out sarcoid, lymphoma) |
| Contact with known TB patient | May be negative — isolated TB lymphadenitis is often not associated with active pulmonary TB |
| Prior TB diagnosis or treatment | None |
| Immunocompromise / HIV | No known HIV or immunosuppressive therapy (if immunocompetent) |
| Malignancy / weight loss with drenching night sweats | Absence of B-symptoms strongly suggestive of lymphoma helps; but mild constitutional symptoms may overlap |
Pulmonary infection is present in only a minority of TB lymphadenitis cases — the negative respiratory history does NOT exclude TB. — Rosen's Emergency Medicine, p. 2711
🔍 Past Medical & Social History
- BCG vaccination status (may reduce severity but does not prevent all forms)
- Travel to or origin from TB-endemic region (Sub-Saharan Africa, South/Southeast Asia)
- Living conditions: overcrowding, poor ventilation
- HIV status: HIV-negative in this case (or note if positive — HIV increases risk of generalized lymphadenopathy)
- No prior TB treatment
- No known contact with confirmed TB case (TB lymphadenitis can occur without known exposure)
🩺 Physical Examination
General
- Appears well or mildly unwell; may be afebrile or have low-grade fever
- No acute distress
Head & Neck
- Solitary or multiple enlarged lymph nodes in the posterior cervical chain / supraclavicular region
- Early stage: discrete, rubbery, firm, freely mobile; overlying skin normal
- Later stage: nodes become matted (adherent to each other and underlying structures); skin becomes erythematous and warm
- Advanced: fluctuant mass (cold abscess); may have an open sinus tract draining caseous material
- No tenderness on palpation (key feature)
Respiratory
- Chest clear to auscultation bilaterally (absence of crackles, bronchial breathing)
- No signs of pleural effusion
- Percussion note normal
Abdomen
- No hepatosplenomegaly
- No abdominal lymphadenopathy palpable
Other
- No axillary or inguinal lymphadenopathy (in isolated cervical disease)
- No clubbing, no jaundice, no skin lesions
🔬 Investigations
Bedside / Routine
- Tuberculin Skin Test (Mantoux): often positive (induration ≥10 mm)
- IGRA (Interferon-Gamma Release Assay): positive in TB infection
- Full Blood Count: mild normocytic anaemia, leukocytosis, thrombocytosis
- ESR / CRP: mildly elevated (non-specific)
- CXR: may be normal (pulmonary TB absent in majority) — no active parenchymal lesion, no hilar adenopathy in isolated disease
Diagnostic (Confirmatory)
- Fine-Needle Aspiration Cytology (FNAC) — first-line diagnostic procedure
- AFB smear positive in ~20–50% of cases
- Shows caseating granulomas (epithelioid histiocytes + Langhans giant cells + central necrosis) in nearly all immunocompetent patients
- Sensitivity 77%, specificity 93% for TB
- Mycobacterial culture of aspirate — M. tuberculosis isolated in ~70% of confirmed cases; gold standard
- Xpert MTB/RIF assay (GeneXpert): rapid molecular diagnosis; sensitivity 81%, specificity 99%
- Excisional lymph node biopsy: if FNAC inconclusive
Caseating granulomas are seen in nearly all biopsy specimens from immunocompetent patients. In immunodeficiency states, granulomas may be poorly formed or absent. — Murray & Nadel's Textbook of Respiratory Medicine, p. 1198
🩻 Clinical Image
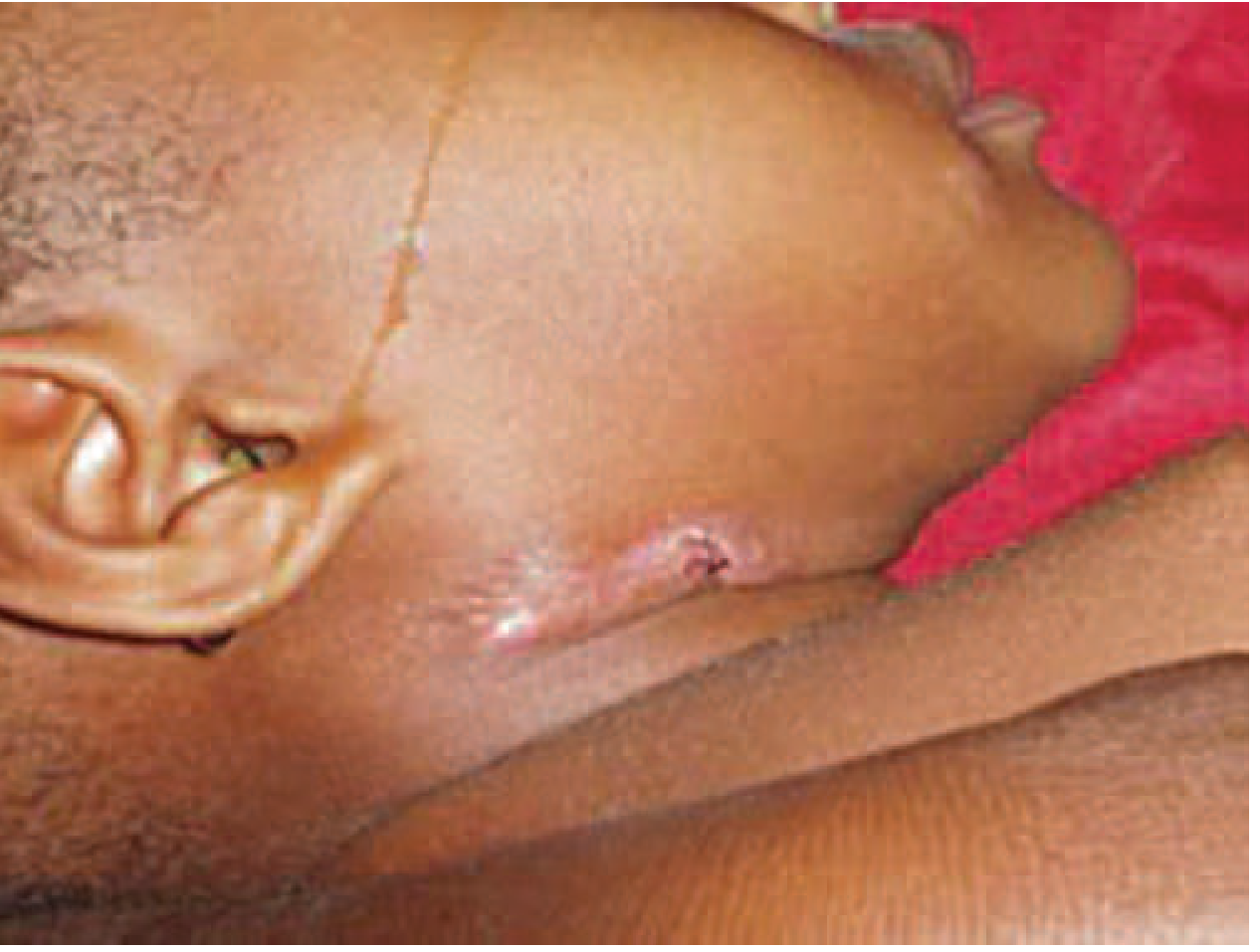
🧾 Differential Diagnosis
| Diagnosis | Distinguishing Features |
|---|---|
| Reactive lymphadenitis | Tender, often following URTI; resolves spontaneously |
| Lymphoma | Firm, rubbery, may be painless; B-symptoms (drenching sweats, fever >38°C, weight loss >10%); biopsy shows Reed-Sternberg cells |
| Metastatic carcinoma | Hard, fixed nodes; primary malignancy usually identifiable |
| Non-tuberculous mycobacteria (NTM) | Common in developed countries; in children especially; Mantoux weakly positive |
| Cat-scratch disease | History of cat contact; Bartonella henselae serology positive |
| Bacterial adenitis | Tender, warm, rapid onset; fever; responds to antibiotics |
| Sarcoidosis | Bilateral hilar adenopathy on CXR; non-caseating granulomas; ACE elevated |
| Toxoplasmosis | Serology positive; often self-limiting |
| Kikuchi / Kimura / Castleman disease | Rare; biopsy required |
The differential diagnosis includes lymphoma, metastatic cancer, fungal disease, cat-scratch disease, sarcoid, toxoplasmosis, reactive adenitis, and bacterial adenitis. — Rosen's Emergency Medicine
💊 Management
Anti-TB Chemotherapy (First-Line)
- 2RHZE / 4RH (2 months Rifampicin + Isoniazid + Pyrazinamide + Ethambutol, followed by 4 months Rifampicin + Isoniazid)
- A 6-month regimen is adequate for drug-susceptible TB lymphadenitis
- Responses may be slower than pulmonary TB
- Paradoxical upgrading reactions (nodes enlarge or new nodes appear during treatment) can occur — do not indicate treatment failure; represent immune reconstitution
Surgical
- Incision and drainage should NOT be performed — leads to permanent sinuses and prolonged drainage
- Surgical excision is reserved for: failure of medical therapy, diagnostic uncertainty
- FNAC preferred over excision biopsy as initial diagnostic step
Key Teaching Points
- TB lymphadenitis is the most common form of extrapulmonary TB worldwide (~35% of extrapulmonary cases)
- It predominantly affects women, adolescents, and young adults; also common in children and HIV-positive individuals
- The characteristic node is painless, non-tender, posterior cervical or supraclavicular
- Pulmonary TB is absent in the majority — a negative chest examination and normal CXR do NOT rule it out
- FNAC is the cornerstone of diagnosis; culture remains the gold standard
- Nodes may mature, suppurate, and form sinus tracts if untreated
- Treatment is medical, not surgical — incision and drainage is contraindicated
Sources: Harrison's Principles of Internal Medicine 22e; Murray & Nadel's Textbook of Respiratory Medicine; Goldman-Cecil Medicine; Rosen's Emergency Medicine
Case presentation history , examination, negative history of tb lymph node swelling
I already have comprehensive textbook data from the previous session. Here is the complete structured case presentation:
Case Presentation: Tuberculous Lymphadenitis (Scrofula)
Presenting Complaint
"I have had a painless swelling on the side of my neck for the past 2 months."
Patient: 24-year-old female | Setting: Outpatient clinic
History of Presenting Illness
- Painless, slowly progressive swelling in the right side of the neck for 8 weeks
- Initially a single small lump; now appears to have two or three lumps matting together
- No redness over the skin initially; recently the overlying skin has become slightly indurated
- No pus discharge or sinus tract at this stage
- Reports mild evening fever and night sweats over the past 3–4 weeks
- Weight loss of approximately 3–4 kg over 2 months
- Appetite reduced; general fatigue and malaise
Negative History (Pertinent Negatives — Critically Important)
These must be explicitly documented:
Respiratory Negatives
| Symptom | Status |
|---|---|
| Cough (productive or dry) | Absent |
| Haemoptysis | Absent |
| Chest pain or pleuritic pain | Absent |
| Breathlessness / dyspnoea | Absent |
Pulmonary TB is absent in the majority of TB lymphadenitis cases — a negative respiratory history does NOT rule out TB lymphadenitis. — Goldman-Cecil Medicine
Local / Neck Negatives
| Symptom | Status |
|---|---|
| Pain over the swelling | Absent (characteristically painless) |
| Rapid or sudden increase in size | Absent (slow, gradual growth) |
| Sore throat / odynophagia | Absent |
| Difficulty swallowing | Absent |
| Hoarseness of voice | Absent |
| Preceding upper respiratory tract infection | Absent |
Systemic / Other Negatives
| Feature | Status |
|---|---|
| Drenching night sweats with >10% weight loss + high fever (lymphoma B-symptoms) | Absent in classic pattern |
| Skin rash | Absent |
| Joint pains | Absent |
| Pruritus | Absent |
| Previous TB diagnosis or anti-TB treatment | None |
| Known contact with confirmed TB patient | None documented |
| HIV diagnosis or risk factors | None |
| Immunosuppressive medication / steroids | None |
| Animal contact (cats) / cat scratch | None (excludes cat-scratch disease) |
| Foreign travel recently | Lives in endemic region |
| Alcohol / substance use | None |
Past Medical History
- No prior TB or other chronic illness
- No previous surgeries or hospitalisations
- BCG vaccination in childhood (scar present)
Drug History
- No regular medications
- No known drug allergies
Family & Social History
- Lives in a densely populated household (4–5 people, 2-room dwelling)
- No known family member with TB (but may still be a source)
- Non-smoker, no alcohol
Review of Systems
- No haematuria, dysuria (rules out genitourinary TB as co-presentation)
- No back pain or limb weakness (rules out Pott's disease)
- No headache or neck stiffness (rules out TB meningitis)
- No abdominal distension (rules out TB peritonitis)
Physical Examination
General Appearance
- Young woman, alert and oriented, looks mildly unwell
- No acute distress; not pale, not jaundiced, not cyanosed
- Low-grade fever: Temp 37.8°C | PR 88 bpm | BP 110/70 mmHg | RR 18/min | SpO₂ 98% on air
Head & Neck (Most Important)
- Right posterior cervical chain: 3 enlarged lymph nodes, largest ~3 × 2.5 cm
- Nodes are firm, non-tender, partially matted
- Overlying skin: slightly erythematous and thickened; no fluctuance yet; no sinus tract
- No transillumination
- Left cervical nodes: 1 mildly enlarged, soft, non-tender node (~1 cm)
- No supraclavicular, axillary, or inguinal lymphadenopathy
Respiratory System
- Chest expansion: equal bilaterally
- Percussion: resonant throughout; no dullness
- Auscultation: vesicular breath sounds, air entry equal bilaterally; no crackles, no wheeze, no bronchial breathing
- No signs of pleural effusion
Cardiovascular
- Heart sounds I and II heard; no murmurs
- No raised JVP, no ankle oedema
Abdomen
- Soft, non-tender
- No hepatomegaly, no splenomegaly
- No palpable abdominal masses
Musculoskeletal
- Normal spine — no gibbus deformity, no kyphosis (excludes Pott's disease)
Neurological
- No focal deficits; no neck stiffness
Skin
- BCG scar present (left deltoid)
- No skin lesions, erythema nodosum, or lupus vulgaris
Clinical Image

Summary / Clinical Impression
A 24-year-old woman from an endemic area presenting with an 8-week history of painless, progressive, matted right-sided cervical lymphadenopathy with constitutional symptoms (low-grade fever, night sweats, weight loss), in the absence of any respiratory symptoms, and no clinical evidence of pulmonary disease.
Most likely diagnosis: Tuberculous lymphadenitis (Scrofula)
Differential Diagnosis
| Diagnosis | Key Distinguishing Feature |
|---|---|
| Tuberculous lymphadenitis | Painless, matted, cervical; constitutional symptoms; endemic setting |
| Reactive lymphadenitis | Tender; preceded by URTI; self-limiting |
| Lymphoma (Hodgkin's) | Rubbery, painless but with drenching sweats, pruritus, mediastinal widening on CXR |
| Metastatic carcinoma | Hard, fixed; identifiable primary; older patient |
| Non-tuberculous mycobacteria | Similar picture; more common in children in developed countries |
| Cat-scratch disease (Bartonella) | History of cat contact; serology positive |
| Bacterial lymphadenitis | Acutely tender, hot, erythematous; responds to antibiotics |
| Sarcoidosis | Bilateral hilar adenopathy on CXR; non-caseating granulomas; ACE elevated |
Investigations
| Investigation | Expected Finding |
|---|---|
| Mantoux / TST | Induration ≥10 mm (positive) |
| IGRA | Positive |
| CXR (PA) | Often normal — no parenchymal lesion |
| FBC | Mild anaemia, leukocytosis, thrombocytosis |
| ESR / CRP | Mildly elevated (non-specific) |
| FNAC of node | Caseating granulomas; AFB smear positive in ~20–50%; sensitivity 77%, specificity 93% |
| Culture (Lowenstein-Jensen) | M. tuberculosis isolated in ~70% confirmed cases (gold standard; 6–8 weeks) |
| GeneXpert MTB/RIF | Rapid molecular diagnosis; sensitivity 81%, specificity 99% |
| HIV test | Perform in all cases |
Caseating granulomas are seen in nearly all biopsy specimens from immunocompetent patients. In immunodeficiency states, granulomas may be poorly formed or absent. — Murray & Nadel's Textbook of Respiratory Medicine
Note: Incision and drainage is contraindicated — causes permanent sinus tracts. FNAC is preferred over open biopsy as the initial diagnostic step.
Management
Anti-TB Chemotherapy
- Intensive phase (2 months): Rifampicin (R) + Isoniazid (H) + Pyrazinamide (Z) + Ethambutol (E) → 2RHZE
- Continuation phase (4 months): Rifampicin + Isoniazid → 4RH
- Total: 6 months — adequate for drug-susceptible TB lymphadenitis
- Responses may be slower than pulmonary TB
- Paradoxical reactions (nodes temporarily enlarge during treatment) can occur — indicate immune reconstitution, not treatment failure
Surgical
- Reserved for: failed medical therapy, diagnostic uncertainty
- Do NOT incise and drain — permanent sinuses result
Sources: Harrison's Principles of Internal Medicine 22e · Murray & Nadel's Textbook of Respiratory Medicine · Goldman-Cecil Medicine · Rosen's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.