Acne
Reading File
Asking for Preferences
Finding Sources
Finding Sources
Reading File
Reading File
Loading Image
Reading File
I now have comprehensive content from Harrison's to synthesize a thorough answer. Here is a full clinical overview of acne:
Acne Vulgaris
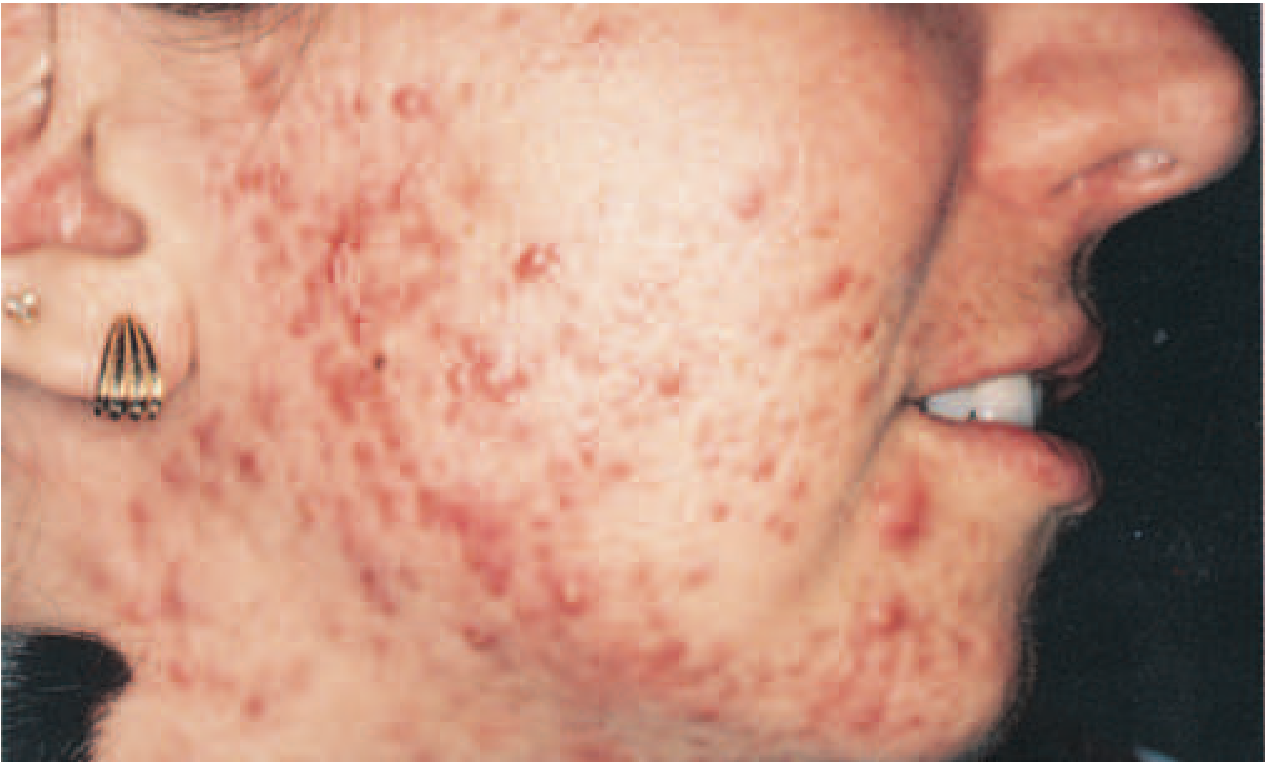
Pathophysiology
Acne vulgaris is a self-limited disorder primarily of teenagers and young adults, though 10–20% of adults may continue to experience it. Four key factors drive the disease:
- Sebum overproduction — puberty-driven androgenic stimulation of sebaceous glands is the permissive factor
- Follicular hyperkeratinization — abnormal differentiation and proliferation of follicular epithelium causes retention of keratinous material, blocking the pilosebaceous unit
- Cutibacterium acnes colonization — bacteria within comedones release free fatty acids from sebum, driving inflammation and cyst wall rupture
- Inflammation — rupture of the cyst wall releases oily and keratinous debris, triggering a foreign-body inflammatory reaction
Lesion Types
| Lesion | Description |
|---|---|
| Closed comedone (whitehead) | 1–2 mm pebbly white papule; follicular orifice blocked; precursor to inflammatory lesions |
| Open comedone (blackhead) | Dilated follicular orifice filled with oxidized, darkened sebum; rarely inflammatory |
| Papule | Small inflammatory lesion |
| Pustule | Inflammatory lesion containing pus |
| Nodule/cyst | Large inflammatory lesions; may drain and cause scarring |
The earliest lesions in adolescence are typically noninflammatory or mildly inflamed comedones on the forehead, followed by inflammatory lesions on the cheeks, nose, and chin. The chest and back are also commonly involved.
Aggravating Factors
- Mechanical friction — headbands, chin straps of helmets
- Comedogenic topical agents — certain cosmetics, hair preparations
- Industrial chemical exposure (chronic topical)
- Medications — glucocorticoids (topical or systemic), progestin-only contraception, lithium, isoniazid, androgenic steroids, halogens (iodides, bromides), phenytoin, phenobarbital
- Systemic conditions — polycystic ovarian syndrome (PCOS), hyperandrogenic states
Severity Classification
- Mild — predominantly comedonal; minimal inflammatory lesions; no scarring
- Moderate — papules and pustules; may involve face, chest, back
- Severe — large inflammatory nodules/cysts; significant potential for scarring
Treatment
Treatment is matched to pathophysiology and severity:
Topical Agents
| Agent | Mechanism | Notes |
|---|---|---|
| Retinoids (tretinoin, adapalene, tazarotene, trifarotene) | Normalize follicular epithelium differentiation; loosen microcomedones; anti-inflammatory | Apply to entire acne-prone area once daily; tretinoin in the evening (UV inactivation); benefit not evident for 6–8 weeks; apparent flare in first month is expected |
| Benzoyl peroxide | Bactericidal against C. acnes; reduces free fatty acids | Reduces risk of antibiotic resistance; used with retinoids and antibiotics |
| Topical antibiotics (clindamycin, erythromycin) | Anti-inflammatory; suppresses C. acnes | Used with benzoyl peroxide to limit resistance |
| Topical dapsone | Anti-inflammatory | Particularly useful in adult female acne |
Systemic Agents
| Agent | Use Case |
|---|---|
| Oral antibiotics (doxycycline, minocycline, sarecycline) | Moderate–severe inflammatory acne; reduce C. acnes and inflammation |
| Oral contraceptives (combined estrogen-progestin) | Hormonal acne in females; reduces androgen-driven sebum production |
| Spironolactone | Anti-androgen; adult female acne |
| Isotretinoin (oral) | Severe nodular/cystic acne; scarring acne unresponsive to other therapies; reduces sebum production profoundly; teratogenic — requires iPLEDGE program in the US |
Procedural Options
- Intralesional triamcinolone for large individual cysts
- Comedone extraction
- Chemical peels, laser, light therapy (adjunctive)
Key Points
- The comedone is the primary lesion — all inflammatory lesions arise from it
- Most acne does not scar; a small subset with nodular/cystic disease requires aggressive early intervention to prevent permanent scarring
- Retinoids address the root cause (follicular keratinization) and are foundational to most regimens
- Antibiotic monotherapy should be avoided; always pair with benzoyl peroxide to limit C. acnes resistance
- Isotretinoin is the most effective therapy for severe disease but requires careful monitoring (liver function, lipids, mandatory contraception due to teratogenicity)
Sources: Harrison's Principles of Internal Medicine 22E; Dermatology 2-Volume Set 5e (Elsevier)
This is a shared conversation. Sign in to Orris to start your own chat.