I now have all the content needed for a comprehensive introduction. Here is the full disease overview:
Glomerulonephritis (GN) — Disease Overview & Introduction
1. Definition
Glomerulonephritis refers to a group of disorders characterized by inflammation of the glomeruli — the microscopic capillary tufts within the kidney responsible for filtering blood. The presentations range widely: from an asymptomatic individual found incidentally to have hematuria or proteinuria on a routine check, to a fulminant illness with acute kidney injury (AKI) and life-threatening extrarenal disease.
The most dramatic symptomatic presentations are actually uncommon. Asymptomatic urine abnormalities are far more frequent, though they may indicate a wide range of glomerular or non-glomerular diseases.
— Comprehensive Clinical Nephrology, 7th Edition, p. 234
2. The Glomerulus — What Is Being Inflamed?
Each kidney contains approximately 1 million nephrons, each with a glomerulus at its head. The glomerulus consists of:
| Component | Structure & Role |
|---|
| Fenestrated endothelium | Lines capillaries; allows fluid filtration |
| Glomerular Basement Membrane (GBM) | Type IV collagen network (α3:α4:α5); structural scaffold |
| Podocytes | Epithelial cells with foot processes; form the slit-pore membrane |
| Mesangial cells | Structural support; phagocytic; contractile |
The slit-pore membrane between adjacent podocyte foot processes — formed by proteins including nephrin, podocin, CD2AP, and TRPC6 — acts as the final protein size filter. Damage to any of these components leads to proteinuria or hematuria.
Podocytes attach to the GBM by special foot processes and are replenished by migrating parietal epithelial cells from Bowman's capsule; impaired replenishment results in heavy proteinuria.
— Harrison's Principles of Internal Medicine 22E, p. 2407
3. How GN Presents Clinically
GN is associated with three core features:
Hypertension + Volume expansion + Abnormal urinalysis
Volume expansion manifestations:
- Adults: Edema (peripheral, periorbital), hypertension, orthopnea, dyspnea on exertion
- Children: Ascites may develop
- Elderly: Restlessness and anxiety may be the first signs of incipient acute pulmonary edema
Urinary findings:
- Oliguria (low urine output) or rarely anuria
- Low urine sodium + concentrated urine → salt and water retention
- Spun urinary sediment examination is ESSENTIAL to diagnose active GN
The nephritic urinalysis shows:
- Hematuria (microscopic or macroscopic)
- Proteinuria
- Dysmorphic red blood cells — RBCs become misshapen as they cross the damaged GBM
- RBC casts — the hallmark of glomerular origin of bleeding
- Mixed inflammatory cells including PMN leukocytes (pyuria)
Macroscopic hematuria: described as "cola" or "tea-colored" urine — hemoglobin enters acid urine and forms hematin. This is classic in post-streptococcal GN and IgA nephropathy (IgA can produce frank red blood-red urine).
Blood clots or overtly blood-red urine accompanied by dysuria → suggests a lower urinary tract source, not glomerular.
— Harrison's Principles of Internal Medicine 22E, p. 2406
4. Primary vs Secondary GN
Primary (Idiopathic) GN — no underlying systemic disease identified:
- IgA Nephropathy (most common worldwide)
- Minimal Change Disease
- Focal Segmental Glomerulosclerosis (FSGS)
- Membranous Nephropathy
- MPGN (Membranoproliferative GN)
Secondary GN — caused by or associated with:
- Autoimmune: SLE (lupus nephritis), vasculitis (ANCA-associated)
- Infections: Post-streptococcal, hepatitis B/C, HIV, endocarditis
- Metabolic: Diabetes mellitus, amyloidosis
- Malignancy: Lung/breast/GI adenocarcinoma → membranous nephropathy; Hodgkin disease → minimal change; Non-Hodgkin lymphoma → MPGN
- Drugs/toxins: NSAIDs, penicillamine, pamidronate, heroin, cyclosporine
- Genetic: Alport syndrome, mutations in podocin/nephrin (FSGS)
- Obesity: Morbid obesity → secondary FSGS
Kidney disease is occasionally the first manifestation of an underlying tumor.
— Comprehensive Clinical Nephrology, 7th Edition, p. 234
5. Classification by Course
| Type | Onset | Timeframe | Example |
|---|
| Acute GN | Sudden | Days to weeks | Post-streptococcal GN |
| Rapidly Progressive GN (RPGN) | Rapid deterioration | Days to weeks | Crescentic GN, Goodpasture |
| Chronic GN | Smoldering, insidious | Months to years | IgA nephropathy, Lupus nephritis |
The pathologic correlate of this spectrum — from acute inflammatory/proliferative/necrotizing lesions to chronic sclerotic/atrophic changes on biopsy — reflects the acuity vs. chronicity of the disease. Early diagnosis is therefore critical, as treatment of acute reversible disease must be instituted as quickly as possible.
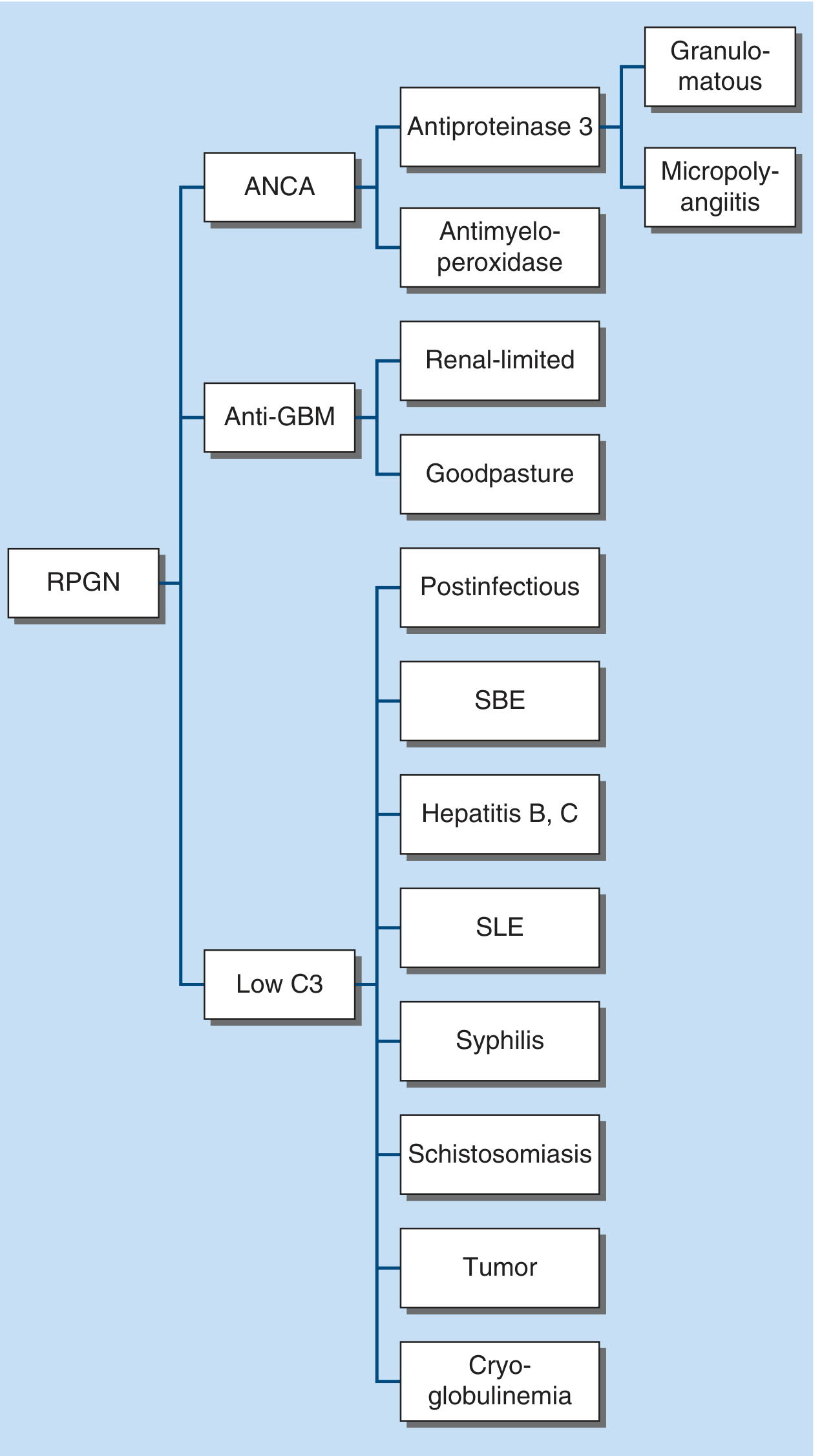
6. RPGN — Classification by Immunopathology
The most urgent category is Rapidly Progressive Glomerulonephritis (RPGN), classified into three types based on immunofluorescence and serology:
| Type | Mechanism | IF Pattern | Examples |
|---|
| Type I | Anti-GBM antibodies | Linear IgG | Goodpasture disease (renal-limited or with lung hemorrhage) |
| Type II | Immune complex | Granular IgG | PSGN, SLE, IgA nephropathy, MPGN, SBE, Hepatitis B/C |
| Type III | Pauci-immune (ANCA+) | Scant/negative | GPA (Granulomatosis with polyangiitis), Microscopic polyangiitis |
C3 is synthesized in the liver, bound to circulating infectious or neoplastic antigens with their antibody complexes, and deposited in the glomerular subendothelium — explaining why immune complex GN is associated with low C3. Cryoglobulinemia (hepatitis C/myeloma) often lowers C4 as well.
— Harrison's Principles of Internal Medicine 22E, Fig. 319-1
7. Clinical Evaluation Framework
History, physical examination, and investigations aim at three goals:
- Exclude non-glomerular disease (e.g., UTI, lower tract bleeding)
- Find evidence of associated multisystem disease (diabetes, SLE, vasculitis, amyloid)
- Establish kidney function (creatinine, eGFR, urinalysis)
Key clinical clues:
- Hearing loss → Alport syndrome
- Recent URTI + hematuria within 1–2 days → IgA nephropathy
- Hematuria 2–3 weeks after throat/skin infection → Post-streptococcal GN
- Hemoptysis + hematuria → Goodpasture disease or ANCA vasculitis
- Butterfly rash + joint pains → SLE/lupus nephritis
- Foamy urine + edema → Heavy proteinuria / nephrotic component
8. The Two Major Clinical Syndromes
| Feature | Nephritic Syndrome | Nephrotic Syndrome |
|---|
| Hematuria | Yes (prominent) | Mild or absent |
| Proteinuria | Mild–moderate | Heavy (>3.5 g/day) |
| Hypertension | Common | Variable |
| Edema | Yes | Yes (severe) |
| Hypoalbuminemia | Mild | Severe |
| Hyperlipidemia / Lipiduria | No | Yes |
| Hallmark | RBC casts, dysmorphic RBCs | Frothy urine, anasarca |
Many forms of GN present with overlapping nephritic-nephrotic features, particularly IgA nephropathy and lupus nephritis.
9. Why Classification Is Challenging
Classification of GN has been difficult because of overlapping features between infection-related and immunologically mediated pathology. There is no single clinical, laboratory, or imaging finding that reliably distinguishes all forms — renal biopsy with light microscopy, immunofluorescence (IF), and electron microscopy (EM) remains the gold standard for definitive diagnosis and classification.
Summary Table
| Feature | Detail |
|---|
| Definition | Glomerular inflammation → impaired filtration |
| Hallmark urine finding | RBC casts + dysmorphic RBCs |
| Core clinical triad | Hematuria + Proteinuria + Hypertension |
| Pathology gold standard | Renal biopsy (LM + IF + EM) |
| Main clinical syndromes | Nephritic vs Nephrotic (can overlap) |
| Acute emergency | RPGN — crescents on biopsy |
| Most common primary GN | IgA nephropathy (worldwide) |
| Classic acute GN | Post-streptococcal GN |
Sources:
- Harrison's Principles of Internal Medicine, 22nd Edition (2025) — Chapter 319: Glomerulonephritis
- Comprehensive Clinical Nephrology, 7th Edition — Chapter 16: Introduction to Glomerular Disease: Clinical Presentations