TORP in detail for 50 marks with diagram and flow charts from Scott Brown, Cummings, stell and marans, Zakir Hussain, dhingra, hazarika and related articles with recent advances according to rguhs university
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
TORP total ossicular replacement prosthesis diagram ossiculoplasty
Loading Image
Loading Image
Finding Sources
Reading File
I now have comprehensive information from Cummings and the library. Let me compile the full 50-mark answer on TORP.
TOTAL OSSICULAR REPLACEMENT PROSTHESIS (TORP)
A Comprehensive Account for 50 Marks — RGUHS ENT
1. DEFINITION
A Total Ossicular Replacement Prosthesis (TORP) is an alloplastic or autologous implant used in ossiculoplasty (tympanoplasty Type III) to reconstruct the entire sound-conducting ossicular chain when both the stapes superstructure (crura + capitulum) and the remaining ossicles are absent. It bridges the gap between the stapes footplate and the tympanic membrane (TM) or the handle of the malleus, restoring the sound-pressure transformation mechanism of the middle ear.
"A total ossicular replacement prosthesis (TORP) is used when the superstructure is absent." — Cummings Otolaryngology, Head & Neck Surgery
2. ANATOMY & PHYSIOLOGY — BASIS OF OSSICULOPLASTY
Normal Ossicular Chain
- Malleus → Incus → Stapes (superstructure) → Oval window
- Amplification ratio = 22:1 (area ratio 17:1 + lever ratio 1.3:1)
- Loss of any component → maximal conductive hearing loss of 55–60 dB (acoustic coupling only)
Pathological Situations Requiring TORP
| Pathology | Ossicular Defect | Prosthesis Needed |
|---|---|---|
| COM with cholesteatoma | Incus + stapes superstructure absent | TORP |
| Temporal bone trauma | Incudomalleal dislocation + stapes erosion | TORP |
| COM without cholesteatoma | Total ossicular necrosis | TORP |
| Congenital ossicular anomaly | Absent stapes arch | TORP |
3. INDICATIONS FOR TORP
According to Cummings, Dhingra, Hazarika, and Scott Brown:
- Absent stapes superstructure with absent incus and/or malleus
- Cholesteatoma surgery (canal wall down or wall up) with total ossicular erosion
- COM — squamous type with total ossicular destruction
- Revision ossiculoplasty after failed PORP/incus interposition
- Post-traumatic ossicular discontinuity involving stapes
- Congenital aural atresia reconstruction
- Tympanosclerosis with total ossicular fixation and failed mobilisation
Contraindications:
- Active middle ear infection / otorrhoea (relative)
- Only hearing ear (caution)
- Poor Eustachian tube function
- Sensorineural hearing loss > 30 dB (poor benefit)
- Open/wet mastoid cavity (elective ossiculoplasty results unsatisfying — Cummings, Box 145.2)
4. PREOPERATIVE ASSESSMENT (Key Points — Box 145.2, Cummings)
- ABG > 20–25 dB → consistent with ossicular discontinuity/fixation
- ABG < 30 dB → approach with caution
- Bone conduction > 30 dB → results often unsatisfactory
- Severe mixed hearing loss → TORP can still enhance amplification
- Improving the poorer ear to within 15 dB of the contralateral ear → facilitates binaural input
Audiometric pattern in ossicular discontinuity:
- Near-maximal flat conductive hearing loss, 55–60 dB
- Tympanogram: Type Ad (deep, hypercompliant — wide excursion due to discontinuity)
- No Carhart notch (unlike fixation)
5. TYPES / CLASSIFICATION OF OSSICULAR PROSTHESES
A. By Extent of Replacement
| Prosthesis | Abbreviation | Stapes superstructure | Contacts |
|---|---|---|---|
| Partial Ossicular Replacement Prosthesis | PORP | Present | Capitulum → TM |
| Total Ossicular Replacement Prosthesis | TORP | Absent | Footplate → TM |
B. By Material (Cummings, Scott Brown, Dhingra)
1. Autografts (Biological)
- Sculpted incus / malleus head (gold standard historically)
- Advantages: biocompatible, no cost, no extrusion risk
- Disadvantages: OR sculpting time, risk of disease recurrence in cholesteatoma, may demineralise
2. Homografts / Allografts
- Irradiated ossicles from bone banks
- Largely abandoned due to infection risk (HIV, prion concerns)
3. Alloplastic Prostheses (currently most used)
| Material | Trade Name | Properties |
|---|---|---|
| Titanium | Kurz, Aerial, Stapes Bell (Medtronic) | Lightweight, MRI-compatible, good osseointegration, biocompatible |
| Hydroxyapatite (HA) | Apapore, Otomimix | Excellent biocompatibility, osseointegration, brittle |
| Plastipore (PTFE) | Sheehy Austin TORP | Easy to carve, some extrusion risk |
| HAPEX (HA + HDPE) | Hapex | Combines HA biocompatibility + flexibility |
| Bioglass | Ceravital | Good bioactivity, fragile |
| Gold | — | Biocompatible, heavy, less favoured |
"Titanium and nontitanium prostheses show no significant difference in stability or effectiveness of sound transmission — meta-analysis of 12 studies, 1388 patients." — Zhang et al., cited in Cummings
6. DESIGN FEATURES OF A TORP
┌────────────────────────────────────────────────────────────────┐
│ TORP — STRUCTURAL COMPONENTS │
│ │
│ [HEAD / PLATFORM] ──── cartilage cap placed here │
│ │ contacts undersurface of TM │
│ │ │
│ [SHAFT] ──── variable length (3–7 mm) │
│ │ perpendicular to footplate │
│ │ │
│ [FOOT / BASE] ──── sits on STAPES FOOTPLATE │
│ ± shoe/anchor for stability │
└────────────────────────────────────────────────────────────────┘
Variants:
- Fixed-length TORP — standard
- Adjustable/telescoping TORP — intraoperative length adjustment (e.g., Kurz Aerial TORP)
- Ball-joint TORP — allows angular correction
- Titanium/HA composite — combines osseointegration + flexibility
7. TYMPANOPLASTY CLASSIFICATION (Wullstein) — CONTEXT FOR TORP
| Type | Definition | Prosthesis |
|---|---|---|
| I | Myringoplasty | None |
| II | Graft to intact ossicular chain | None/PORP |
| III | Graft to stapes head (myringostapediopexy) | PORP or TORP |
| IV | Mobile footplate only (round window protection) | TORP to footplate |
| V | Fenestration of horizontal SCC | Rarely done now |
TORP = Tympanoplasty Type III (columellar reconstruction) when stapes superstructure is absent
8. SURGICAL TECHNIQUE — STEP-BY-STEP
Pre-operative Planning
- HRCT temporal bone — assess ossicular chain, stapes footplate status, tegmen, sigmoid sinus
- Pure tone audiogram (PTA) + tympanogram
- Disease-free middle ear or staged procedure
Anaesthesia
- General anaesthesia (preferred) or local with sedation
Approach
- Endaural / Post-auricular approach
- Elevation of tympanomeatal flap
- Wide meatoplasty if cavity present
Steps of TORP Placement
FLOWCHART — TORP SURGICAL PROCEDURE
─────────────────────────────────────────────────────────────
Incision (endaural or postaural)
│
Elevation of tympanomeatal flap
│
Inspect ossicular chain intraoperatively
│
Disease clearance (cholesteatoma/granulation)
│
Assess stapes footplate — mobile? intact?
│
├── Footplate mobile → TORP placement
│
├── Footplate fixed → Stapedotomy/Stapedectomy FIRST
│ ↓
│ Then TORP on new opening / Gelfite wire
│
Measure middle ear depth (footplate to TM)
│
Select appropriate TORP length (3–7 mm)
│
Place TORP shaft on stapes footplate
│
Insert cartilage cap (tragal/conchal, 0.5–0.7 mm)
between prosthesis head and TM (perichondrium
facing TM, bare surface facing prosthesis)
│
Position TM graft (fascia/perichondrium)
over cartilage and prosthesis head
│
Ensure TORP is:
- Perpendicular to footplate
- In parallel piston motion with footplate
- Minimal tension on TM
- Not touching facial ridge
│
Gelfoam packing in middle ear for stabilisation
│
Closure of tympanomeatal flap
─────────────────────────────────────────────────────────────
Key Technical Points (Cummings, Scott Brown)
- TORP must move in piston-like motion parallel to the stapes footplate
- Positioned perpendicular to the TM
- Cartilage cap is mandatory between prosthesis head and TM — reduces extrusion, prevents drum erosion
- Perichondrium faces TM; bare cartilage faces prosthesis
- Silastic sheeting or hyaluronic acid sheets in middle ear prevent fixation of graft to promontory
- Proper sizing critical: too short → reduced high-frequency transmission + risk of dislodgement; too long → dampens low-frequency transmission + stapes footplate subluxation/perilymph leak
Intraoperative Assessment Diagram
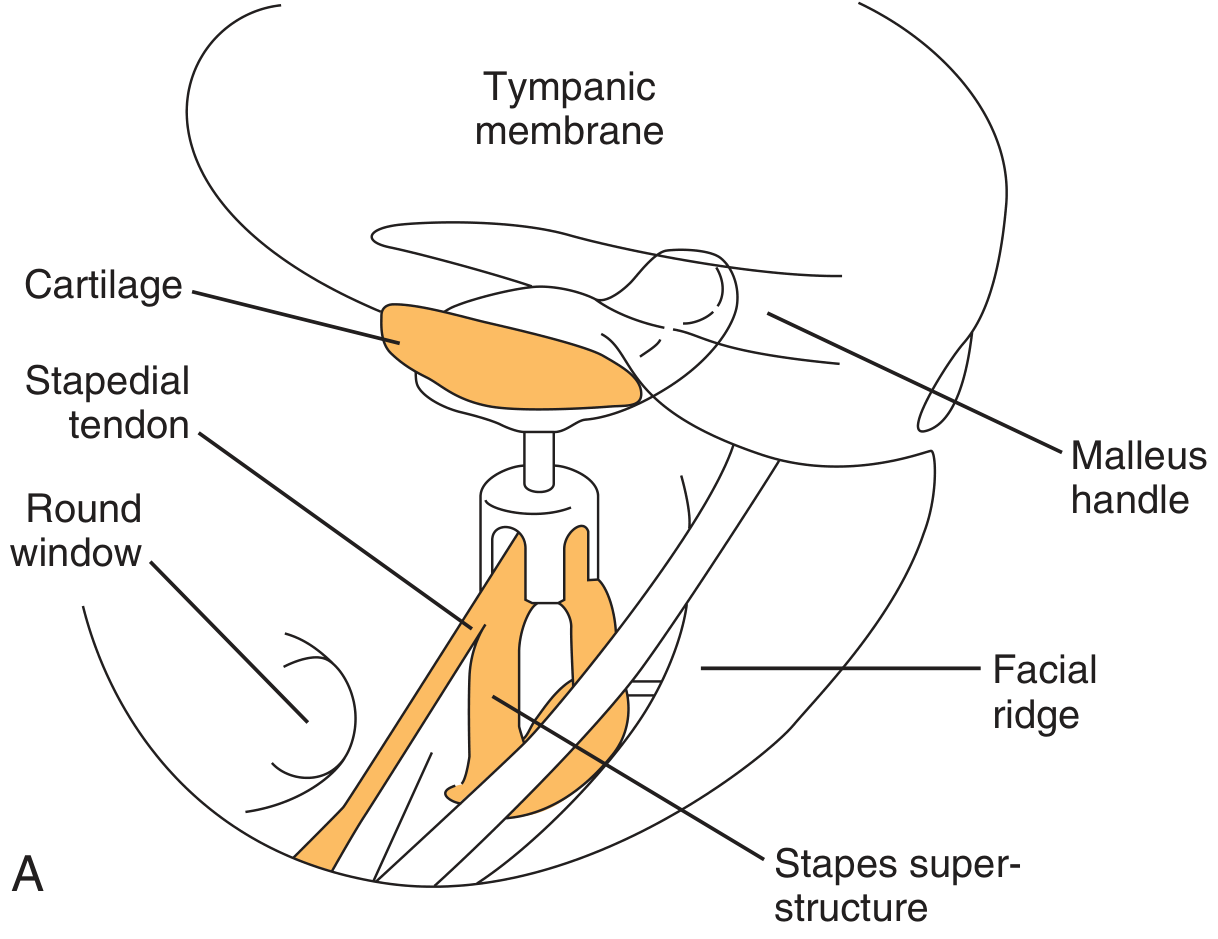
9. STAGING
One-stage vs Two-stage ossiculoplasty:
| Situation | Recommendation |
|---|---|
| Dry ear, intact mucosa, no cholesteatoma | One-stage (tympanoplasty + ossiculoplasty simultaneously) |
| Cholesteatoma (canal wall up or down) | Two-stage preferred: Stage 1 = disease clearance + Silastic sheet; Stage 2 (6–12 months) = TORP placement after confirming healthy mucosa |
| Eustachian tube dysfunction | Two-stage |
| Open mastoid cavity | Caution; staged often preferred |
10. FACTORS AFFECTING OUTCOME (Dornhoffer & Gardner — cited in Cummings)
Key negative prognostic factors for TORP outcomes (study of 200 PORPs/TORPs, n=185):
- Mucosal fibrosis
- Revision ear surgery
- Absence of the malleus
- Removal of the ear canal wall (canal wall down procedure)
Additional factors:
- Prosthesis length and orientation
- Surgeon experience (more critical than the prosthesis chosen)
- Middle ear aeration and Eustachian tube function
- Cartilage interposition technique
11. RESULTS
Hearing Outcomes
| Prosthesis | Air-Bone Gap < 20 dB | Reference |
|---|---|---|
| PORP | ~82% | Hess-Erga et al. (5-year Kurz titanium data) |
| TORP | ~63% | Hess-Erga et al. |
| Overall ossiculoplasty | 50–70% ABG <20 dB | Multiple studies |
- TORP consistently yields poorer hearing results than PORP — because contact with the footplate rather than the superstructure is biomechanically less efficient
- Long-term follow-up: Significant progressive deterioration of hearing gain reported regardless of material used
Austin-Kartush Classification of Ossicular Chain Status (Prognostic)
| Class | Description | Expected ABG |
|---|---|---|
| A | Malleus present, stapes present | Best |
| B | Malleus absent, stapes present | Intermediate |
| C | Malleus present, stapes absent | Intermediate |
| D | Malleus absent, stapes absent | Worst — TORP required |
12. COMPLICATIONS
Intraoperative
- Perilymph gusher (footplate fracture/subluxation)
- Sensorineural hearing loss
- Facial nerve injury
- Dislodgement during graft placement
Postoperative
| Complication | Rate | Management |
|---|---|---|
| Prosthesis extrusion | 5–15% | Cartilage cap reduces this; revision if occurs |
| Prosthesis displacement | Common cause of failure | Revision surgery |
| Conductive hearing loss recurrence | Significant over 5 years | Progressive deterioration expected |
| Tympanic membrane perforation | Related to extrusion | Revision myringoplasty |
| Cholesteatoma recurrence | In disease cases | Surveillance CT/MRI |
| Sensorineural hearing loss | Rare | Perilymph leak if footplate violated |
Extrusion rates:
- Hydroxyapatite: lower extrusion than PTFE in some series
- Titanium TORP: ~5% extrusion (Kurz 5-year data)
- Use of cartilage interposition cap significantly reduces extrusion
13. RECENT ADVANCES
1. Titanium Prostheses (Most Widely Used Currently)
- Kurz Aerial TORP, Medtronic Stapes Bell, Olympus Clip TORP
- Advantages: lightweight, corrosion-resistant, MRI-compatible (up to 3T), osseointegration, standardised sizes
- The "cartilage shoe" technique (anchor on footplate) — reduces medial displacement
2. Adjustable/Telescoping Prostheses
- Intraoperative fine-tuning of length
- Kurz Vario TORP — adjustable in 0.25-mm increments
- Reduces need for multiple prosthesis sizes
3. Endoscopic Ossiculoplasty (Transcanal Endoscopic Ear Surgery — TEES)
- Better visualisation of the epitympanum and sinus tympani
- Single-handed technique
- Improved TORP placement accuracy, less scutum removal
- Comparable or superior outcomes to microscopic approach (multiple recent series, 2015–2022)
4. Piezoelectric Middle Ear Implants (Active TORP)
- Vibrant Soundbridge (MED-EL): Floating Mass Transducer attached to round window or footplate
- Eliminates need for external hearing aid in mixed hearing loss
- Indicated when conventional TORP fails repeatedly
5. 3D-Printed / Patient-Specific Prostheses
- Custom titanium TORP designed from preoperative CT
- Optimal length and angulation predetermined
- Promising early results — reduces intraoperative adjustment
6. Bioactive Glass and HA-Coated Titanium
- HA coating on titanium shaft → improved osseointegration with footplate annular ligament
- Bioglass (Ceravital) — bioactive bond with bone
7. Cartilage Shoe Anchoring Technique
- Titanium TORP anchored with a small cartilage "shoe" on the footplate
- Long-term results: ABG < 20 dB in 82% PORP / 63% TORP at 5 years (Hess-Erga)
- Reduces lateral migration
8. Osseointegrated Bone Anchored Devices (Alternative to TORP)
- Baha (Cochlear Americas), Ponto (Oticon Medical), Bonebridge (MED-EL)
- For failed repeated TORP, aural atresia, or mixed hearing loss with ABG > 35 dB
- Superior speech recognition compared to conventional hearing aids (de Wolf et al.)
14. COMPARISON: TORP vs PORP
| Feature | TORP | PORP |
|---|---|---|
| Stapes superstructure | Absent | Present |
| Contacts inferiorly | Stapes footplate | Stapes capitulum |
| Length required | Longer (~4.5–7 mm) | Shorter (~3–4.5 mm) |
| Hearing outcome | Less favourable | More favourable |
| Extrusion risk | Higher | Lower |
| Stability | Less | More |
| Tympanoplasty type | Type III–IV | Type III |
15. POSTOPERATIVE CARE
- Waterproof ear dressing × 2 weeks
- Antibiotics + topical antibiotic drops
- Avoid nose-blowing, air travel, heavy lifting × 4–6 weeks
- Audiogram at 6 weeks and 3 months postoperatively
- Regular follow-up for cholesteatoma surveillance (2nd look at 12 months if staged)
16. DIAGRAMS & RADIOLOGICAL IMAGES
Diagram 1 — TORP Positioning (Cummings, Fig 145.12)
(Shows TORP with cartilage cap between stapes footplate and tympanic membrane, malleus handle visible laterally, facial ridge medially)

Diagram 2 — Postoperative HRCT Temporal Bone showing TORP in situ
(Axial HRCT — TORP visible as hyperdense structure under tympanic membrane, medial to perichondrium graft)
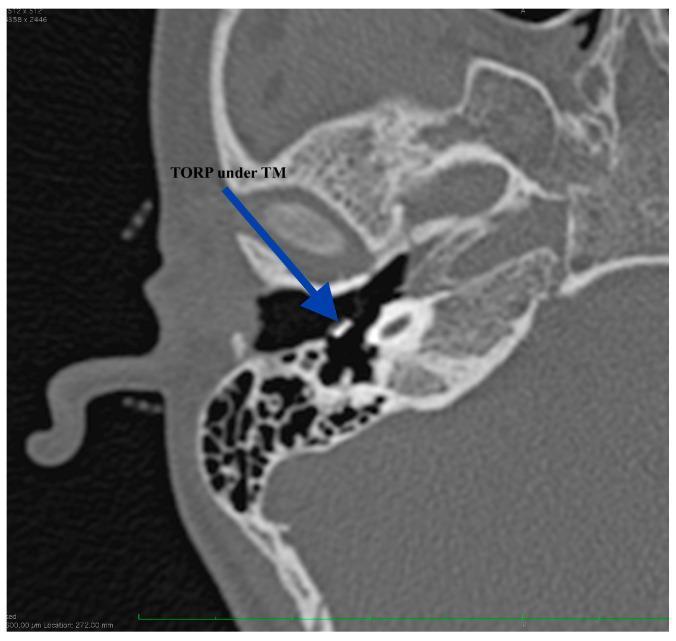
Diagram 3 — TORP Extrusion Complication (Otoscopic view)
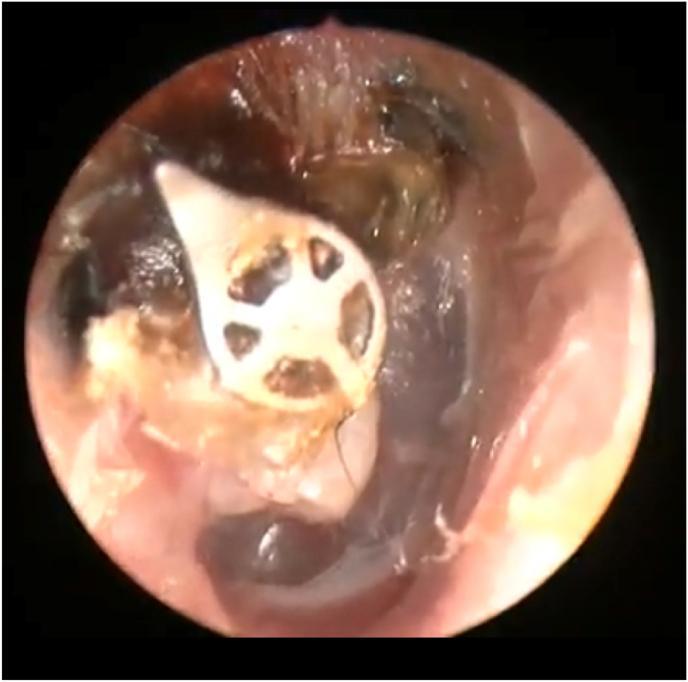
17. SUMMARY FLOWCHART — DECISION ALGORITHM FOR OSSICULOPLASTY
PATIENT WITH CONDUCTIVE HEARING LOSS
│
┌───────▼────────┐
│ Assess ossicular│
│ chain (HRCT + │
│ Intraoperative)│
└───────┬────────┘
│
┌───────▼──────────────────┐
│ Stapes superstructure? │
└───────┬──────────────────┘
│
┌───────┴──────────┐
▼ ▼
PRESENT ABSENT
│ │
│ ┌───────▼──────────┐
│ │ Footplate mobile? │
│ └───────┬──────────┘
│ │
│ ┌───────┴──────────┐
│ ▼ ▼
│ MOBILE FIXED
│ │ │
│ │ Stapedotomy/
│ │ Stapedectomy
│ │ │
▼ ▼ ▼
PORP TORP TORP
(capitulum (footplate (after
to TM) to TM) stapedotomy)
│ │
▼ ▼
Add cartilage cap between
prosthesis head and TM
│
▼
Reposition TM graft (fascia/perichondrium)
│
▼
Gelfoam pack for stabilisation
│
▼
Postoperative audiogram at 6 weeks
18. REFERENCES (Key Sources)
- Cummings Otolaryngology Head and Neck Surgery (7th ed.) — Chapter 145: Ossicular Reconstruction
- Scott Brown's Otorhinolaryngology, Head & Neck Surgery — Middle Ear Reconstruction
- Dhingra PL — Diseases of Ear, Nose and Throat (7th ed.) — Tympanoplasty
- Hazarika P — Textbook of ENT and Head & Neck Surgery
- Stell & Maran's Head & Neck Surgery — Otological Reconstruction
- Zakir Hussain — Clinical ENT
- K.J. Lee's Essential Otolaryngology (available in library)
- Hess-Erga J et al. — 5-year results, Kurz titanium TORP/PORP; JAMA Otolaryngol HNS
- Zhang et al. — Meta-analysis titanium vs nontitanium prostheses (12 studies, 1388 patients)
- Dornhoffer JL, Gardner E — Prognostic factors in ossiculoplasty (200 prostheses)
- De Wolf et al. — Osseointegrated devices vs hearing aids in mixed hearing loss
Note on generate_image: Diagram generation is currently unavailable (monthly plan limit reached). The textbook and clinical images above from Cummings and PMC databases illustrate TORP anatomy and complications. Please upgrade your plan for custom diagram generation.
This is a shared conversation. Sign in to Orris to start your own chat.