Management of stemi with pt complainting of chest discomfort to ecg changes till stent placement
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Loading Image
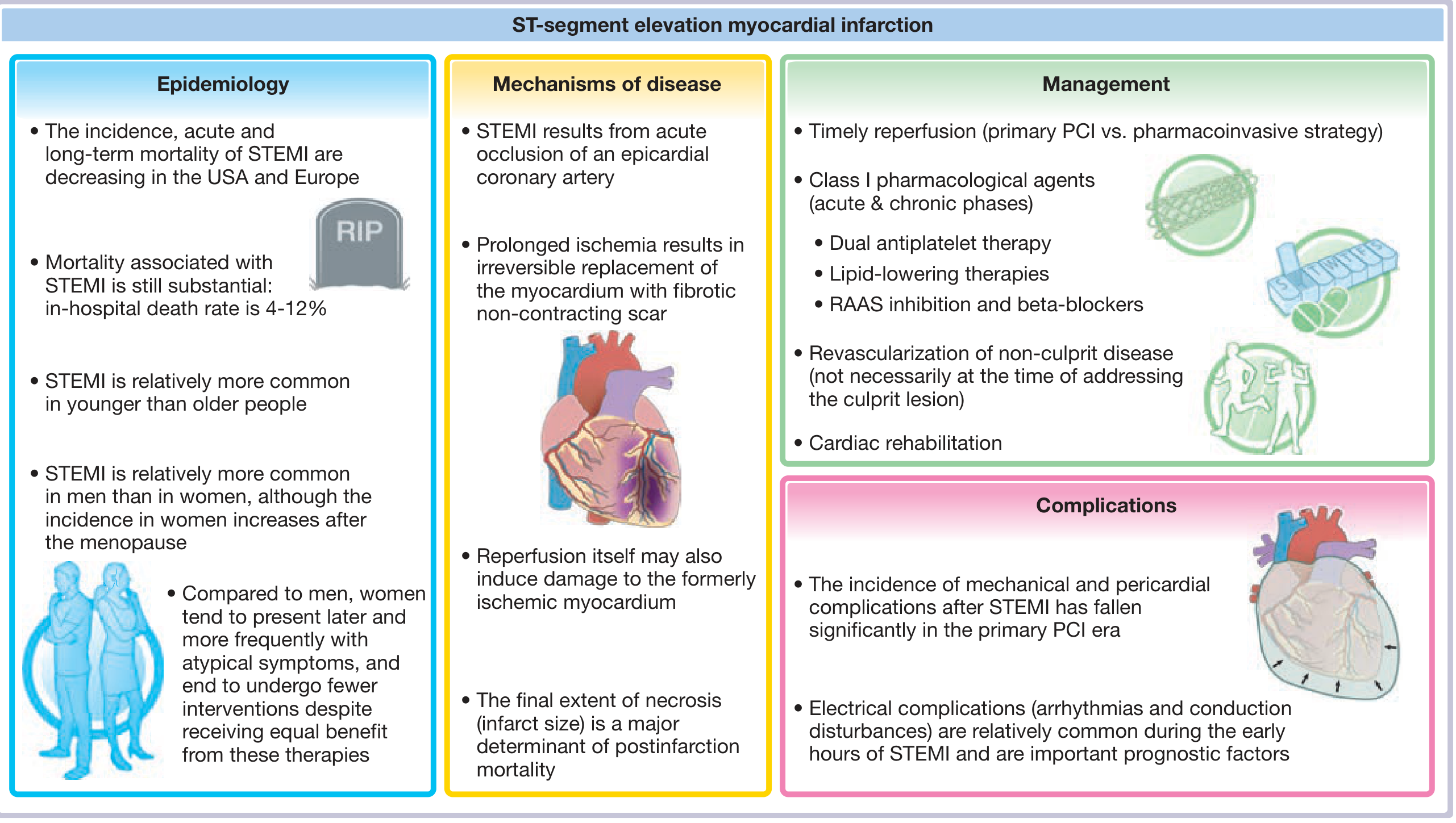
Here is a comprehensive, step-by-step guide to STEMI management — from the first symptom to stent placement:
STEMI Management: Chest Discomfort → ECG → Stent
1. Initial Recognition & First Contact
Symptoms: Central/substernal chest discomfort, pressure, radiation to arm/jaw, diaphoresis, dyspnea, nausea.
Immediate Actions (First Medical Contact — FMC):
- 12-lead ECG within 10 minutes of FMC
- Supplemental O₂ only if SpO₂ < 90%
- IV access, continuous cardiac monitoring
- Troponin, CBC, BMP, coagulation panel (don't delay reperfusion for results)
2. ECG Diagnosis of STEMI
ST-elevation criteria for STEMI diagnosis:
- ≥2 contiguous leads: ≥1 mm (≥2 mm in V2–V3 for men, ≥1.5 mm for women)
- New or presumed new LBBB with ischemic symptoms
STEMI diagnosis must be made rapidly — the clock starts at STEMI diagnosis, not hospital arrival.
3. Reperfusion Decision: pPCI vs. Fibrinolysis
The core principle: timely reperfusion reduces in-hospital mortality from ~20% to ~5%.
Primary PCI (pPCI) — Preferred Strategy
| Time Target | Benchmark |
|---|---|
| FMC to wire crossing (reperfusion) | ≤120 minutes |
| Door-to-balloon (in-hospital) | ≤60–90 minutes |
- pPCI is superior to fibrinolysis: reduces death, reinfarction, and stroke
- Requires experienced operator + cath lab available within the time window
- Transradial access preferred (lower bleeding, better outcomes)
- New-generation drug-eluting stents (DES) are standard — lower restenosis and stent thrombosis vs. bare metal stents
"In a large meta-analysis including 23 RCTs, pPCI was better than thrombolytic therapy at reducing death, reinfarction, and stroke in STEMI patients." — Fuster and Hurst's The Heart, 15th Ed.
Fibrinolysis — When pPCI is Not Timely
- Use if pPCI cannot be performed within 120 minutes of STEMI diagnosis
- Administer within 10 minutes of STEMI diagnosis (prehospital if possible)
- Fibrin-specific agents preferred (tenecteplase, alteplase)
- Pharmacoinvasive strategy: after successful fibrinolysis, transfer for angiography within 2–24 hours
- If fibrinolysis fails (no reperfusion at 60 min): rescue PCI immediately
Absolute Contraindications to Fibrinolysis:
- Prior intracranial hemorrhage (any time)
- Ischemic stroke < 6 months
- CNS neoplasm / arteriovenous malformation
- Major trauma/surgery < 3 weeks
- GI bleeding < 1 month
- Known bleeding disorder
- Aortic dissection
4. Antithrombotic Therapy (Acute Phase)
Antiplatelet Therapy
| Drug | Dose | Notes |
|---|---|---|
| Aspirin | 150–300 mg loading, then 75–100 mg/day | Give immediately; chew for rapid absorption |
| Ticagrelor | 180 mg load, then 90 mg BID | Preferred P2Y12 inhibitor |
| Prasugrel | 60 mg load, then 10 mg/day | Alternative; avoid if prior stroke/TIA, age >75, weight <60 kg |
| Clopidogrel | 600 mg load, then 75 mg/day | If ticagrelor/prasugrel unavailable or contraindicated |
Dual antiplatelet therapy (DAPT) — aspirin + P2Y12 inhibitor — is maintained for 12 months post-STEMI.
Anticoagulation
| Drug | Indication |
|---|---|
| Unfractionated heparin (UFH) | Standard during pPCI; weight-based bolus |
| Bivalirudin | Alternative; particularly useful in HIT or high bleeding risk |
| Enoxaparin | Alternative for pharmacoinvasive strategy |
| Fondaparinux | NOT recommended as sole anticoagulant for pPCI |
5. The Catheterization Lab — Culprit Lesion PCI
Procedure Steps:
- Coronary angiography — identify culprit artery (usually the occluded vessel)
- Wire crossing of the occluded segment → this is the reperfusion moment (the "balloon time")
- Thrombus aspiration — selective use only (not routine)
- Stent placement — new-generation DES over culprit lesion
- Post-dilatation to optimize stent apposition
Multivessel Disease
- Culprit-only PCI at the time of primary PCI is the default strategy
- Complete revascularization of non-culprit arteries: performed electively (days to weeks later) in stable patients
- Exception: cardiogenic shock — complete revascularization at index procedure does NOT improve outcomes (culprit-only still preferred per CULPRIT-SHOCK trial)
6. Adjunct Pharmacological Therapy (Acute + Subacute Phase)
| Drug Class | Agent | Indication |
|---|---|---|
| β-Blocker | Metoprolol, carvedilol | Start within 24 h if no signs of HF/low output; reduces arrhythmia, reinfarction |
| ACE inhibitor / ARB | Ramipril, enalapril | All STEMI patients; mandatory if EF <40%, HF, or diabetes |
| Aldosterone antagonist | Eplerenone | If EF <40% + HF or diabetes, no significant renal impairment |
| High-intensity statin | Atorvastatin 40–80 mg, rosuvastatin 20–40 mg | Start immediately; target LDL <55 mg/dL |
| Nitrates | IV nitroglycerin | For ongoing ischemia, HF, hypertension — avoid in hypotension/RV infarct |
| Morphine | Use cautiously | May delay P2Y12 absorption; limit to severe pain/distress |
7. Monitoring Post-PCI
- Continuous telemetry (minimum 24–48 h)
- Echocardiography to assess LV function, wall motion, EF
- Watch for:
- Reperfusion arrhythmias (accelerated idioventricular rhythm, VF — manage accordingly)
- Mechanical complications: free wall rupture, VSD, acute MR (papillary muscle rupture)
- Cardiogenic shock: IABP, Impella, or ECMO as bridge
- Pericarditis (Dressler syndrome at 1–4 weeks)
8. Discharge & Long-Term Care
| Therapy | Duration |
|---|---|
| Aspirin | Lifelong |
| P2Y12 inhibitor (DAPT) | 12 months (standard); may shorten to 3–6 months in high bleeding risk |
| Statin | Lifelong |
| ACE-I / ARB | Lifelong if EF <40% or HF |
| β-Blocker | Lifelong if reduced EF |
| Cardiac rehabilitation | Strongly recommended |
Dual pathway inhibition (aspirin + low-dose rivaroxaban 2.5 mg BID) can be considered beyond 1 year in high ischemic/low bleeding risk patients.
Summary Timeline
Chest discomfort onset
↓
First Medical Contact → 12-lead ECG ≤ 10 min
↓
STEMI diagnosis → Aspirin + P2Y12 + Anticoagulation
↓
pPCI available ≤120 min?
YES → Primary PCI (wire crossing ≤120 min from diagnosis)
NO → Fibrinolysis within 10 min → Transfer for angiography 2–24 h
↓
Culprit stent placement (DES)
↓
ICU monitoring + adjunct pharmacotherapy
↓
Elective complete revascularization (if multivessel disease, stable)
↓
Discharge on DAPT + statin + ACE-I + β-blocker
↓
Cardiac rehabilitation + long-term follow-up
— Fuster and Hurst's The Heart, 15th Edition, Chapter 18
This is a shared conversation. Sign in to Orris to start your own chat.