Harlequin icthyosia
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Loading Image
I now have comprehensive information to provide a thorough answer on harlequin ichthyosis.
Harlequin Ichthyosis (HI)
OMIM #242500 | Synonyms: Harlequin baby, Harlequin fetus, Ichthyosis congenita gravior
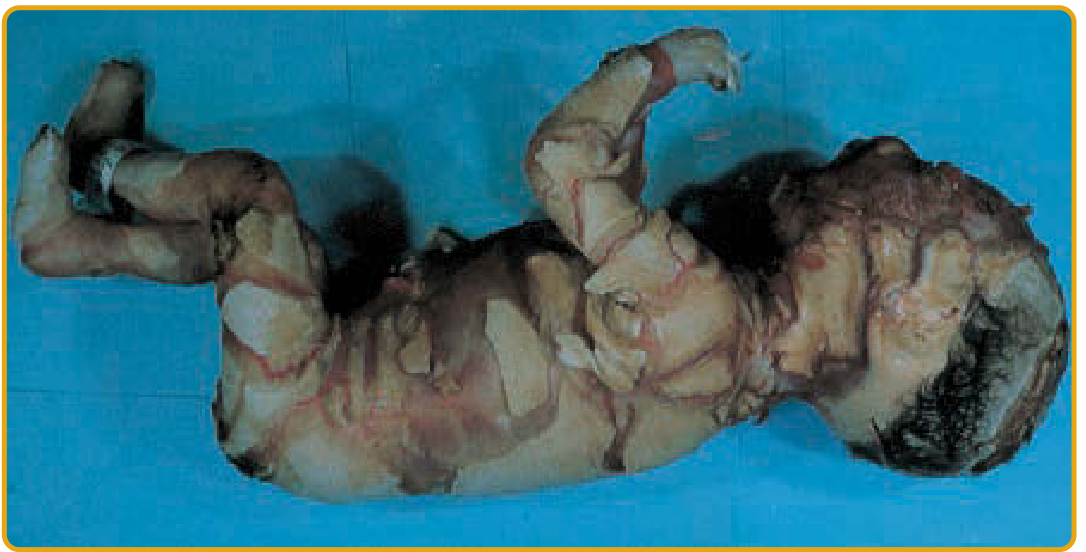
Harlequin ichthyosis in a neonate: thick "plates" of stratum corneum separated by deep red fissures, with distorted facial features.
Definition & Background
Harlequin ichthyosis is the most severe form of autosomal recessive congenital ichthyosis (ARCI). First described in 1750 by Reverend Oliver Hart, the name "harlequin" refers to the resemblance of the diamond-shaped scale pattern and facial features to the costume of the Italian Commedia dell'Arte character. Historically called "harlequin fetus" due to premature delivery and near-uniform fatality, improved survival has led to the current terminology.
Incidence: ~1 in 300,000 births. Autosomal recessive inheritance with wide ethnic distribution.
Genetics & Molecular Pathology
The causative gene is ABCA12, encoding an ATP-binding cassette transporter responsible for secreting lipids into lamellar granules in the skin. Biallelic loss-of-function mutations in ABCA12 result in:
- Absent or abnormal lamellar bodies in the granular layer
- Absent extracellular lipid lamellae
- Accumulation of lipid inclusions/remnant organelles in the stratum corneum
- Failure of normal skin barrier formation
Hypomorphic ABCA12 mutations also cause a milder form of lamellar ichthyosis.
Clinical Features
Neonatal Presentation
Affected neonates are typically born prematurely (mean gestational age ~35 weeks) encased in a hard, armor-like, massively thickened stratum corneum. Shortly after birth, this hyperkeratotic cast cracks and forms:
- Large, yellow, adherent plates separated by broad, deep, intensely red fissures
- Marked ectropion (eversion of eyelids) and eclabium (eversion of lips)
- Rudimentary or absent ear and nasal cartilage
- Edematous, swollen hands and feet, often covered by a mitten-like casing
- Tapered fingertips with hyperconvex nails
- Absent eyelashes and eyebrows; scalp hair may be present
- Occasionally microcephaly
The taut skin severely restricts movement and can impair ventilation. Eclabium and taut facial skin prohibit effective suckling.
Immediate Complications
| Complication | Mechanism |
|---|---|
| Respiratory insufficiency | Mechanical restriction of chest wall |
| Sepsis | Skin fissures as portals of entry |
| Dehydration | Massively elevated transepidermal water loss |
| Hypernatremia | Water loss > sodium loss |
| Temperature instability | Impaired thermoregulation |
| Autoamputation of digits | Constricting skin bands |
Histopathology
The hallmark finding is an extraordinarily thickened, compact orthokeratotic stratum corneum (parakeratosis is occasionally seen). Additional features:
- Prominent hyperkeratotic plugging of hair follicles and sweat ducts
- Concentric accumulation of keratotic material around hair shafts (historically used for prenatal diagnosis on second-trimester skin biopsy)
- EM: absent/abnormal lamellar bodies, absent extracellular lipid lamellae
Survival & Long-Term Course
Uniformly fatal before 1980. Improved neonatal intensive care and systemic retinoid therapy have substantially changed outcomes:
- >50% of affected individuals now survive beyond the neonatal period
- The oldest known HI patient was >25 years of age
All survivors develop a severe, exfoliative ichthyosiform erythroderma. Long-term complications include:
- Painful palmoplantar keratoderma (PPK) — in ~50%
- Dystrophic nails (small, thickened)
- Poor hair growth
- Recurrent skin infections
- Reduced sweating → heat intolerance (a major morbidity)
- Ocular problems (persistent ectropion → corneal exposure, infections)
- Chronic constipation
- Vitamin D deficiency and anemia
- Arthralgias, arthritis, and joint contractures
- Delayed motor development (intelligence is normal)
Diagnosis
- Clinical: characteristic neonatal appearance is usually sufficient
- Molecular: ABCA12 mutation analysis (prenatal diagnosis possible)
- Prenatal: second-trimester skin biopsy (follicular hyperkeratosis) — largely replaced by molecular testing
- Electron microscopy: absent lamellar bodies (not routine)
Management
Neonatal ICU Phase
- Humidified incubator to minimize transepidermal water loss
- Aggressive fluid/electrolyte management
- Emollient application (e.g., petroleum jelly) multiple times daily
- Ophthalmologic care (lubricant eye drops, patching as needed)
- Nutritional support (nasogastric feeding due to eclabium)
- Monitoring and prophylaxis/treatment of infection
- Gentle debridement of scales
Systemic Retinoids
Oral retinoids (acitretin or isotretinoin) are the cornerstone of treatment:
- Promote shedding of the hyperkeratotic shell in neonates
- Reduce scale burden and improve mobility long-term
- Must be used with monitoring for hepatotoxicity, hyperlipidemia, and teratogenicity
Long-term
- Daily emollient use remains essential throughout life
- Regular dermatology, ophthalmology, and multidisciplinary follow-up
- Sunscreen and heat-avoidance strategies (due to anhidrosis/hypohidrosis)
Classification Context
HI falls within the nonsyndromic ARCI category, alongside lamellar ichthyosis (LI) and congenital ichthyosiform erythroderma (CIE). It represents the most extreme phenotype in this spectrum, driven by near-complete loss of ABCA12 function.
Sources: Fitzpatrick's Dermatology, Vol. 1–2, p. 819–820; Dermatology 2-Volume Set, 5e, pp. 1089–1091; Andrews' Diseases of the Skin, p. 2773
This is a shared conversation. Sign in to Orris to start your own chat.