treatment and management of neurocysticercosis in detail
Reading File
Finding Sources
Searching PubMed
"neurocysticercosis"[MeSH Terms] AND treatment
Searching the Web
neurocysticercosis treatment management guidelines 2024 2025
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading Web Page
neurocysticercosis treatment management antiparasitic corticosteroids surgery
Reading File
Reading File
Loading Image
I now have comprehensive, authoritative information from multiple sources. Here is a detailed, well-organized answer:
Neurocysticercosis (NCC): Treatment and Management
NCC is the most common parasitic disease of the human CNS, caused by larval Taenia solium infection, and is the leading cause of symptomatic epilepsy worldwide. Treatment must be individualized — no singular approach applies to all forms.
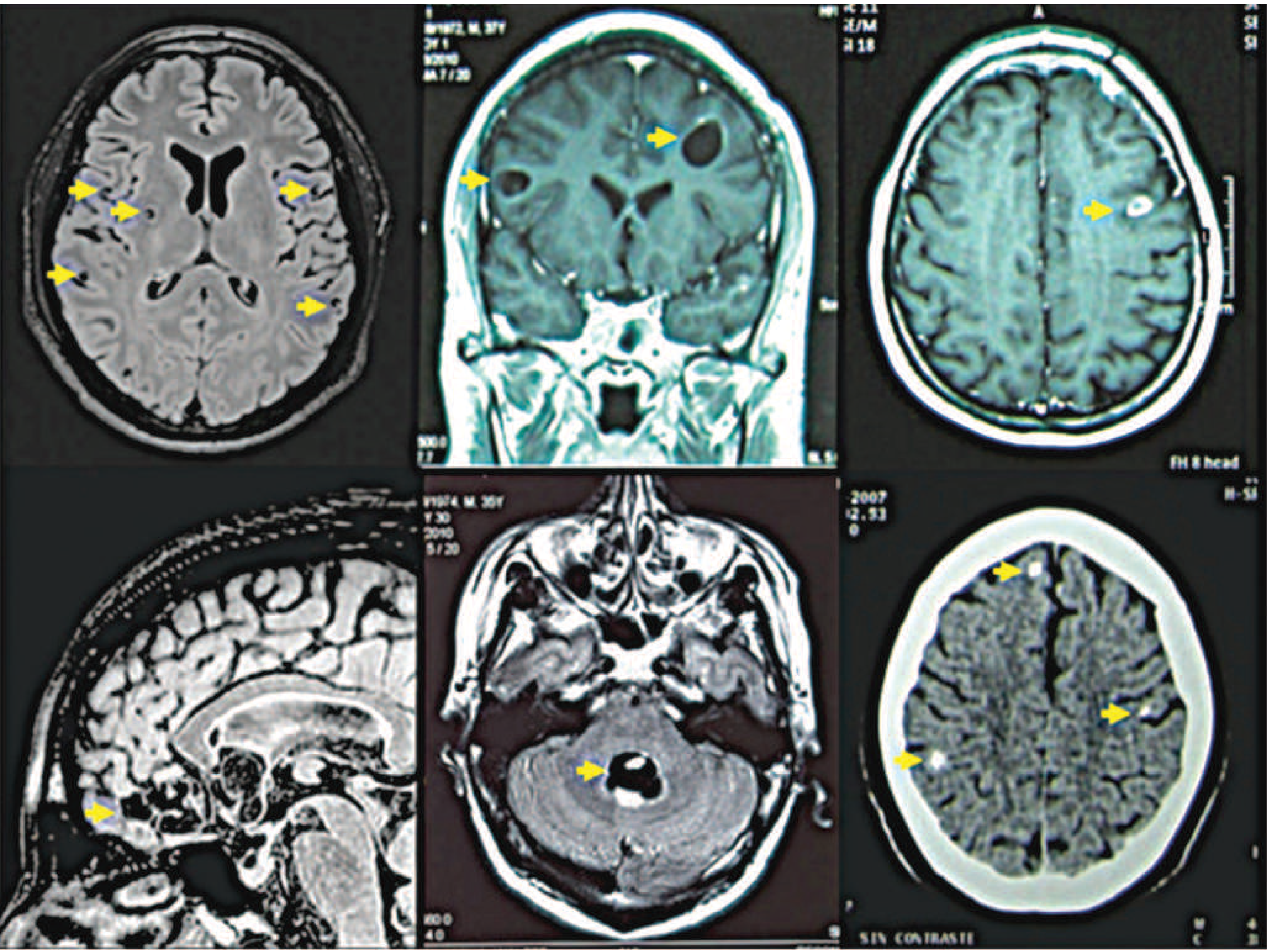
Core Principles
Four overarching management principles guide all decisions:
- Individualize based on number, location, and viability of parasites.
- Prioritize ICP management — antiparasitic drugs must never be started in patients with elevated intracranial pressure.
- Antiparasitic therapy is never an emergency — stabilize with antiseizure medications and anti-inflammatory agents first.
- Treat seizures as secondary (remote symptomatic) seizures from an organic focus.
"Antiparasitic drug treatment is never an emergency in neurocysticercosis and should wait until patients are stabilized." — Harrison's 22E
I. Symptomatic / Supportive Management
Antiseizure Medications (ASMs)
- Seizure control is the first priority — most patients present with seizures.
- Antiepileptic monotherapy controls seizures in the majority of cases.
- Duration of ASM therapy:
- Single enhancing lesion (SEL): Taper after 6 months if imaging normalizes and no breakthrough seizures.
- Multiple parenchymal lesions: Continue for 1–2 years; taper only after lesion resolution and seizure freedom.
- Calcified cysts: Higher risk of recurrent seizures, especially with perilesional edema — may require prolonged or indefinite ASMs.
- In 80–90% of parenchymal NCC, lesions resolve within 3–6 months, leaving patients seizure-free. Up to 20% continue to have seizures requiring ongoing therapy.
Management of Raised ICP
- Mannitol 2 g/kg/day for acute intracranial hypertension.
- High-dose corticosteroids (see below).
- Surgical intervention (shunting) for hydrocephalus — before any antiparasitic drug.
II. Antiparasitic Therapy
Available Agents
| Drug | Dose | Notes |
|---|---|---|
| Albendazole | 15 mg/kg/day (max 1200 mg/day) in 2 divided doses with food | Drug of choice — better CNS penetration, shorter course, lower cost, levels increased by dexamethasone |
| Praziquantel | 50 mg/kg/day in divided doses | Second-line; bioavailability reduced by corticosteroids and anticonvulsants (phenytoin, carbamazepine) |
| Combination (both) | As above | Superior in patients with >2 cysts; praziquantel also raises albendazole sulfoxide plasma levels |
Albendazole is preferred over praziquantel because it:
- Has shorter course and lower cost
- Has improved penetration into the subarachnoid space
- Has increased (not decreased) levels when co-administered with corticosteroids
- Has fewer drug–drug interactions with anticonvulsants
⚠️ Both agents may exacerbate the inflammatory response around the dying parasite, worsening seizures or hydrocephalus — careful monitoring is essential.
III. Treatment by Clinical Form
A. Parenchymal NCC
1–2 Viable (Live) Cysts or Enhancing (Degenerating) Cysts
- Albendazole monotherapy × 10–14 days + corticosteroids
- If cystic lesions persist at 6 months → repeat course
>2 Viable Cysts
- Combination albendazole + praziquantel × 10–14 days + corticosteroids
- Combination therapy improves efficacy; praziquantel raises albendazole sulfoxide plasma levels
Calcified Cysts (Fibro-calcified)
- No antiparasitic treatment — calcified cysts are dead parasites; antiparasitic drugs offer no benefit
- Symptomatic therapy only (ASMs)
- Consider surgical evaluation for refractory epilepsy with a focal calcified seizure source
- Corticosteroids not routinely recommended for isolated calcified NCC with perilesional edema
Cysticercal Encephalitis (Diffuse cerebral edema)
- No antiparasitic treatment — antiparasitic drugs would worsen inflammatory cerebral edema
- Corticosteroids are the primary treatment — up to dexamethasone 32 mg/day may be needed to control brain edema
- Antiparasitic therapy only introduced after ICP normalizes
B. Intraventricular NCC
- Surgical removal is the treatment of choice
- Lateral or third ventricle cysts: Neuroendoscopic removal (procedure of choice for free-floating cysts)
- Fourth ventricle cysts: Neuroendoscopic or microsurgical (posterior approach) based on surgeon's experience
- Antiparasitic drugs make cysts more friable — avoid prior to surgery
- If surgical removal is successful → no antiparasitic therapy required afterward
- If removal is not feasible (e.g., cyst adherent to ventricular pathway with ependymitis):
- Ventricular shunting for hydrocephalus first
- Then antiparasitic drugs + corticosteroids (antiparasitic therapy alone can precipitate hydrocephalus)
- Recent meta-analyses (PMID 40381508, 2025) support neuroendoscopic management with good outcomes.
C. Subarachnoid NCC
- Most severe and difficult-to-treat form
- Prolonged combination antiparasitic therapy (albendazole + praziquantel × several weeks until resolution; multiple courses often required) + prolonged corticosteroids
- Shunting if hydrocephalus is present — shunt first, then antiparasitic drugs
- Corticosteroids are essential to reduce arachnoiditis and accompanying vasculitis
- "Hydrocephalus with no visible cysts on neuroimaging" → shunt only, no antiparasitic treatment
D. Spinal Cysticercosis
| Type | Management |
|---|---|
| Intramedullary | Individualized: surgical removal or antiparasitic + steroids |
| Extramedullary | Preferably surgical removal |
E. Ocular Cysticercosis
- Surgical resection of cysts — antiparasitic drugs contraindicated, as dying cysts in the eye cause severe inflammatory damage
- Pre-treatment ophthalmic examination is mandatory before starting any antiparasitic therapy to rule out intraocular cysticerci
IV. Corticosteroids (Anti-inflammatory Therapy)
Corticosteroids are a cornerstone of NCC management and should be initiated before and continued during antiparasitic treatment:
| Indication | Regimen |
|---|---|
| Standard adjunct during antiparasitic therapy | Dexamethasone 4.5–12 mg/day (0.1–0.4 mg/kg/day) |
| Long-term steroid requirement | Prednisone 1 mg/kg/day (up to 60 mg/day) replacing dexamethasone |
| Cysticercal encephalitis / subarachnoid disease | Dexamethasone up to 32 mg/day until edema controlled |
Key steroid interactions:
- Dexamethasone increases albendazole sulfoxide levels (beneficial)
- Dexamethasone decreases praziquantel bioavailability (clinically important — a reason to prefer albendazole)
Before starting corticosteroids:
- Screen for Strongyloides stercoralis (can cause fatal hyperinfection)
- Screen for latent tuberculosis and vitamin D deficiency
V. Surgical Management
| Indication | Procedure |
|---|---|
| Intraventricular cysts (lateral/3rd ventricle) | Neuroendoscopic removal |
| 4th ventricular cysts | Endoscopic or microsurgical removal |
| Hydrocephalus (cyst not removable) | Ventriculoperitoneal (VP) shunting |
| Ocular NCC | Surgical cyst excision |
| Spinal NCC (selective) | Surgical decompression/excision |
| Refractory epilepsy with calcified focus | Surgical resection of epileptic focus |
Historically, VP shunt failure was a major problem in NCC. Risk of shunt failure may be reduced by postoperative antiparasitic drugs + glucocorticoids.
VI. Monitoring and Follow-up
- MRI is the preferred neuroimaging modality — repeat at least every 6 months until resolution of cystic components
- CT is useful for detecting calcified lesions
- Re-treat if cystic lesions persist at 6 months
- ASMs can be tapered after:
- 6 months for single enhancing lesion with imaging resolution
- 1–2 years for multiple lesions with resolution and seizure freedom
VII. Drug Interactions (Clinically Important)
| Antiparasitic | Interaction | Effect |
|---|---|---|
| Albendazole | + Dexamethasone, praziquantel, cimetidine | ↑ Albendazole sulfoxide levels (beneficial) |
| Albendazole | + Phenytoin, phenobarbital, carbamazepine, ritonavir | ↓ Albendazole levels |
| Praziquantel | + Corticosteroids | ↓ Praziquantel bioavailability |
| Praziquantel | + Phenytoin, carbamazepine | ↓ Praziquantel bioavailability |
VIII. A Newer Agent: Oxfendazole
A newer antiparasitic, oxfendazole, has demonstrated efficacy in porcine cysticercosis. Human safety and tolerability are now established, and it is currently being assessed in clinical trials for solitary cysticercosis in Peru (Singh et al., Current Opinion in Neurology, 2025).
Summary Table (IDSA/ASTMH 2017 + Current Evidence)
| Form | Subgroup | Treatment |
|---|---|---|
| Parenchymal viable | 1–2 cysts | Albendazole + corticosteroids × 10–14 days |
| Parenchymal viable | >2 cysts | Albendazole + praziquantel + corticosteroids × 10–14 days |
| Parenchymal calcified | Any | No antiparasitic; ASMs only |
| Cysticercal encephalitis | — | Corticosteroids only (no antiparasitic until ICP resolves) |
| Intraventricular (removable) | Lateral/3rd ventricle | Neuroendoscopic removal; no post-op antiparasitic |
| Intraventricular (not removable) | — | VP shunt → antiparasitic + steroids |
| Subarachnoid | — | Shunt if hydrocephalic + prolonged combo antiparasitic + prolonged steroids |
| Hydrocephalus, no visible cysts | — | VP shunt only |
| Spinal | — | Individualized: surgery or antiparasitic + steroids |
| Ocular | — | Surgical resection only |
Sources:
- Harrison's Principles of Internal Medicine, 22E (2025), Ch. 242
- Bradley and Daroff's Neurology in Clinical Practice, Table 79.7 (IDSA/ASTMH 2017 guidelines)
- Katzung's Basic and Clinical Pharmacology, 16E
- Red Book 2021 (AAP Committee on Infectious Diseases)
- Tintinalli's Emergency Medicine
- Singh et al., Current Opinion in Neurology 38(4):381–387, 2025 — latest paradigms
- WHO Guidelines on Management of T. solium Neurocysticercosis (2021)
This is a shared conversation. Sign in to Orris to start your own chat.