Infracts with arterial territory
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Based on the textbook content gathered, here is a comprehensive overview of cerebral infarcts by arterial territory:
Cerebral Infarcts by Arterial Territory
Pathological Background
Cerebral arterial occlusion leads to ischemia and then infarction in the distribution of the compromised vessel. The size, location, and shape of the infarct depend on:
- Which artery is occluded
- Availability of collateral circulation
- Duration and completeness of occlusion
With hemodynamic ischemia (hypotension), the arterial border/watershed zones are most vulnerable. With direct occlusion, a wedge-shaped infarct in the center of the arterial territory results.
— Bradley and Daroff's Neurology in Clinical Practice
1. Anterior Circulation
Internal Carotid Artery (ICA)
- Occlusion may cause symptoms in both MCA and ACA territories
- May present with ipsilateral amaurosis fugax (ophthalmic artery branch)
- Contralateral hemiplegia, hemisensory loss, aphasia (dominant hemisphere)
Anterior Cerebral Artery (ACA)
- Contralateral leg > arm weakness and sensory loss (leg area on medial cortex)
- Personality changes, abulia, frontal lobe signs
- Urinary incontinence
Middle Cerebral Artery (MCA)
The most commonly infarcted vessel:
| Division | Dominant (Left) Deficits | Non-dominant Deficits |
|---|---|---|
| Superior trunk | Broca aphasia, contralateral face/arm > leg weakness | Dysarthria, contralateral weakness |
| Inferior trunk | Wernicke aphasia, contralateral hemianopia | Neglect, anosognosia, constructional apraxia |
| Complete MCA | Global aphasia, dense contralateral hemiplegia | Contralateral neglect + hemiplegia |
Anterior Choroidal Artery
- Arises from the ICA
- Classic triad: contralateral hemiplegia + hemisensory loss + homonymous hemianopia
- Infarction in the posterior limb of the internal capsule (Fig. 65.15, shown below)
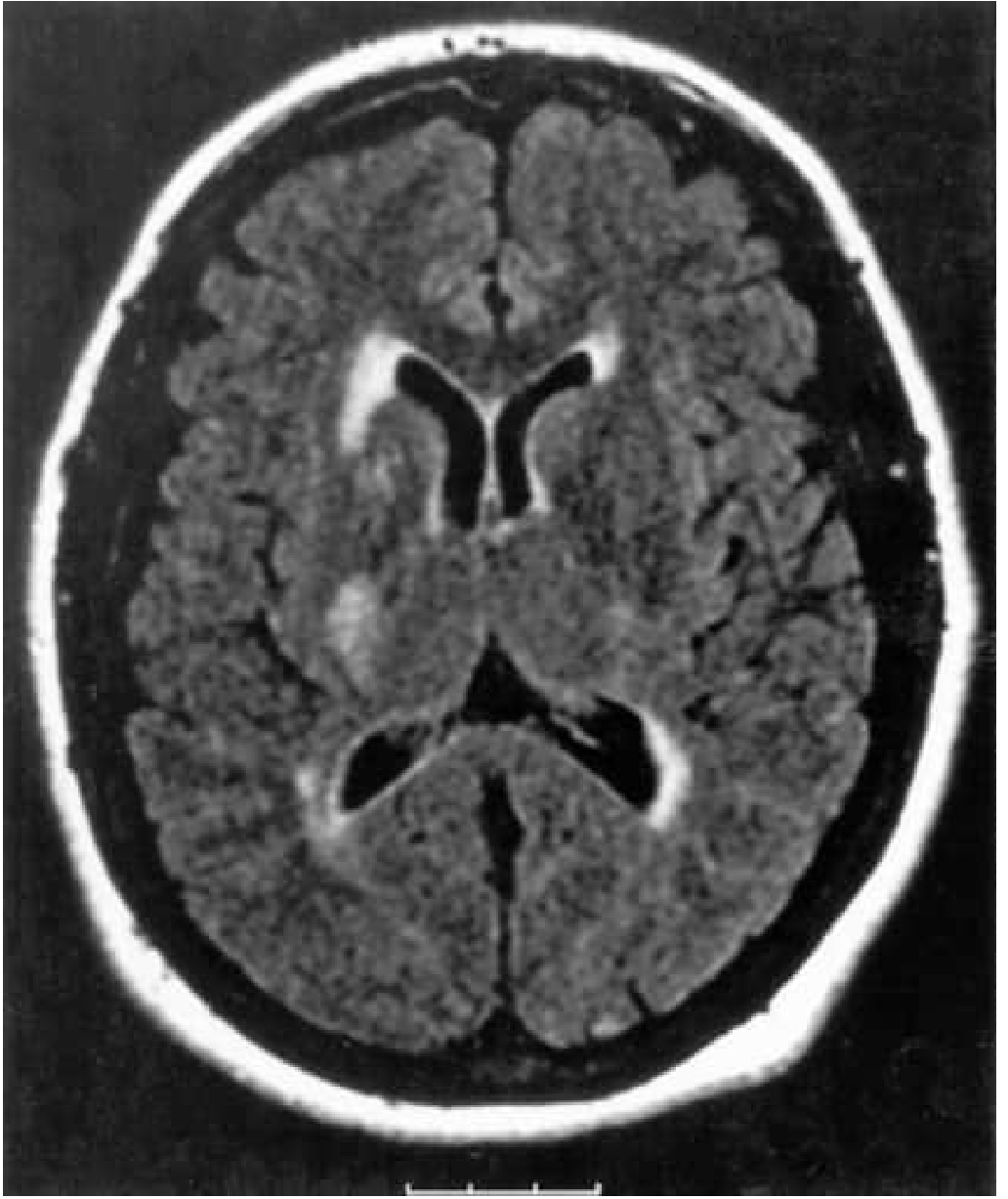
Anterior choroidal artery territory infarct in posterior limb of internal capsule — Bradley and Daroff's Neurology in Clinical Practice
2. Posterior Circulation
Posterior Cerebral Artery (PCA)
- Contralateral homonymous hemianopia (occipital lobe) with macular sparing (if collaterals preserved)
- Dominant: alexia without agraphia, visual agnosia, color anomia
- Non-dominant: topographic disorientation, prosopagnosia
- Deep branches → thalamic infarction (see below)
Vertebrobasilar System
- Bilateral or shifting motor/sensory signs
- Diplopia, dysarthria, dysphagia, vertigo (combination)
- Cranial nerve palsies with contralateral limb weakness (crossed syndromes)
Lateral Medullary (Wallenberg) Syndrome — PICA territory:
- Ipsilateral: facial pain/temperature loss, Horner's, ataxia, dysphagia
- Contralateral: body pain/temperature loss
Basilar Artery Occlusion (catastrophic):
- "Locked-in" syndrome, coma, quadriplegia, CN palsy
3. Thalamic Infarcts by Arterial Territory
The thalamic arteries arise from the posterior communicating artery and perimesencephalic posterior cerebral artery. Four main pedicles:
| Artery | Origin | Thalamic Territory | Key Deficits |
|---|---|---|---|
| Polar arteries | Posterior communicating a. | Reticular, ventral anterior nuclei | Amnesia, behavioral change |
| Paramedian thalamomesencephalic | Basilar communicating (P1 PCA) | Medial nuclei, centromedian, midline | Amnesia, vertical gaze palsy, hypersomnia |
| Thalamogeniculate pedicle | PCA (proximal to geniculate) | Ventral caudal (VP) nuclei | Contralateral hemisensory loss — Déjerine-Roussy syndrome |
| Posteromedial choroidal | PCA (just distal to PComm ostium) | Pulvinar, medial geniculate, centromedian | Visual/auditory disturbances, pain |
The responsible arterial territory for a thalamic infarct can be inferred from the clinical syndrome.
— Localization in Clinical Neurology, 8e
4. Watershed (Border-Zone) Infarcts
Occur at junctions between major arterial territories during hypoperfusion (cardiac arrest, severe hypotension):
| Zone | Location | Deficit |
|---|---|---|
| ACA–MCA border | Parasagittal frontal cortex | "Man-in-a-barrel" — proximal arm > distal weakness |
| MCA–PCA border | Temporoparieto-occipital junction | Visual–spatial deficits, transcortical aphasia |
| Internal watershed | Periventricular white matter | Pure motor/sensory, cognitive impairment |
5. Small Vessel (Lacunar) Infarcts
Occlusion of deep penetrating arteries (lenticulostriate, thalamoperforating) produces small (<1.5 cm) infarcts. Classic syndromes:
| Syndrome | Location |
|---|---|
| Pure motor hemiplegia | Posterior limb internal capsule / pons |
| Pure sensory stroke | Thalamus (VPL nucleus) |
| Ataxic hemiparesis | Internal capsule / pons |
| Dysarthria–clumsy hand | Pons / genu internal capsule |
| Sensorimotor stroke | Thalamo-capsular |
Summary Table: Artery → Infarct Location → Key Deficit
| Artery | Territory | Hallmark Deficit |
|---|---|---|
| MCA (superior) | Frontal + parietal operculum | Motor/Broca aphasia |
| MCA (inferior) | Temporal–parietal | Wernicke aphasia / neglect |
| ACA | Medial frontal | Leg > arm weakness |
| PCA | Occipital + thalamus | Hemianopia ± thalamic pain |
| PICA | Lateral medulla + cerebellum | Wallenberg syndrome |
| AICA | Lateral pons + cerebellum | Ipsilateral facial palsy + deafness |
| SCA | Superior cerebellum | Cerebellar ataxia ± CN IV |
| Ant. choroidal | Posterior internal capsule | Hemi-plegia + sensory + visual |
| Lenticulostriate | Basal ganglia / deep capsule | Lacunar syndromes |
Sources: Bradley and Daroff's Neurology in Clinical Practice; Localization in Clinical Neurology, 8e; Harrison's Principles of Internal Medicine 22E
This is a shared conversation. Sign in to Orris to start your own chat.