Anti bacterial drugs and anti microbial
Antibacterial & Antimicrobial Drugs
Key Terminology
| Term | Definition |
|---|---|
| Antibiotic | Molecule of biological origin (e.g., from molds/bacteria) that inhibits or kills microorganisms |
| Antimicrobial | Broader term — includes antibiotics, synthetic agents, and semi-synthetic compounds |
| Bactericidal | Kills bacteria directly (e.g., penicillins, aminoglycosides) |
| Bacteriostatic | Inhibits bacterial growth; relies on host defenses for final eradication (e.g., tetracyclines, macrolides) |
| MIC | Minimum Inhibitory Concentration — lowest concentration that inhibits visible growth in vitro |
| Narrow-spectrum | Active against only a few organisms |
| Broad-spectrum | Active against both Gram-positive and Gram-negative organisms |
Sources of Antimicrobial Agents
- Natural antibiotics — produced by molds (Penicillium → penicillin) or soil bacteria (Streptomyces → streptomycin, tetracyclines, chloramphenicol, erythromycin)
- Chemically synthesized agents — discovered via screening (e.g., sulfonamides from aniline dyes) or structure-based drug design (e.g., trimethoprim)
- Semi-synthetic modifications — chemical manipulation of natural antibiotics to broaden spectrum, improve pharmacokinetics, or overcome resistance (e.g., extended-spectrum penicillins, newer cephalosporins)
Classification by Mechanism of Action
1. 🔵 Inhibitors of Cell Wall Synthesis
- Inhibit transpeptidase enzymes (Penicillin-Binding Proteins, PBPs) → prevent cross-linking of peptidoglycan → weakened cell wall → osmotic lysis
- Bactericidal; selective toxicity because human cells lack cell walls
- Resistance mechanisms: β-lactamase production (e.g., ampC); altered PBPs (e.g., PBP-2A in MRSA)
- Countermeasures: β-lactamase inhibitors (clavulanate + amoxicillin); PBP-targeting new agents (ceftaroline for MRSA)
- Mycoplasma (no cell wall) is intrinsically resistant
- Binds D-Ala-D-Ala terminus of peptidoglycan precursors → blocks transglycosylation and transpeptidation
- Active only against Gram-positive organisms (too large to penetrate Gram-negative outer membrane)
- Key uses: MRSA, C. difficile (oral)
2. 🟡 Inhibitors of Protein Synthesis
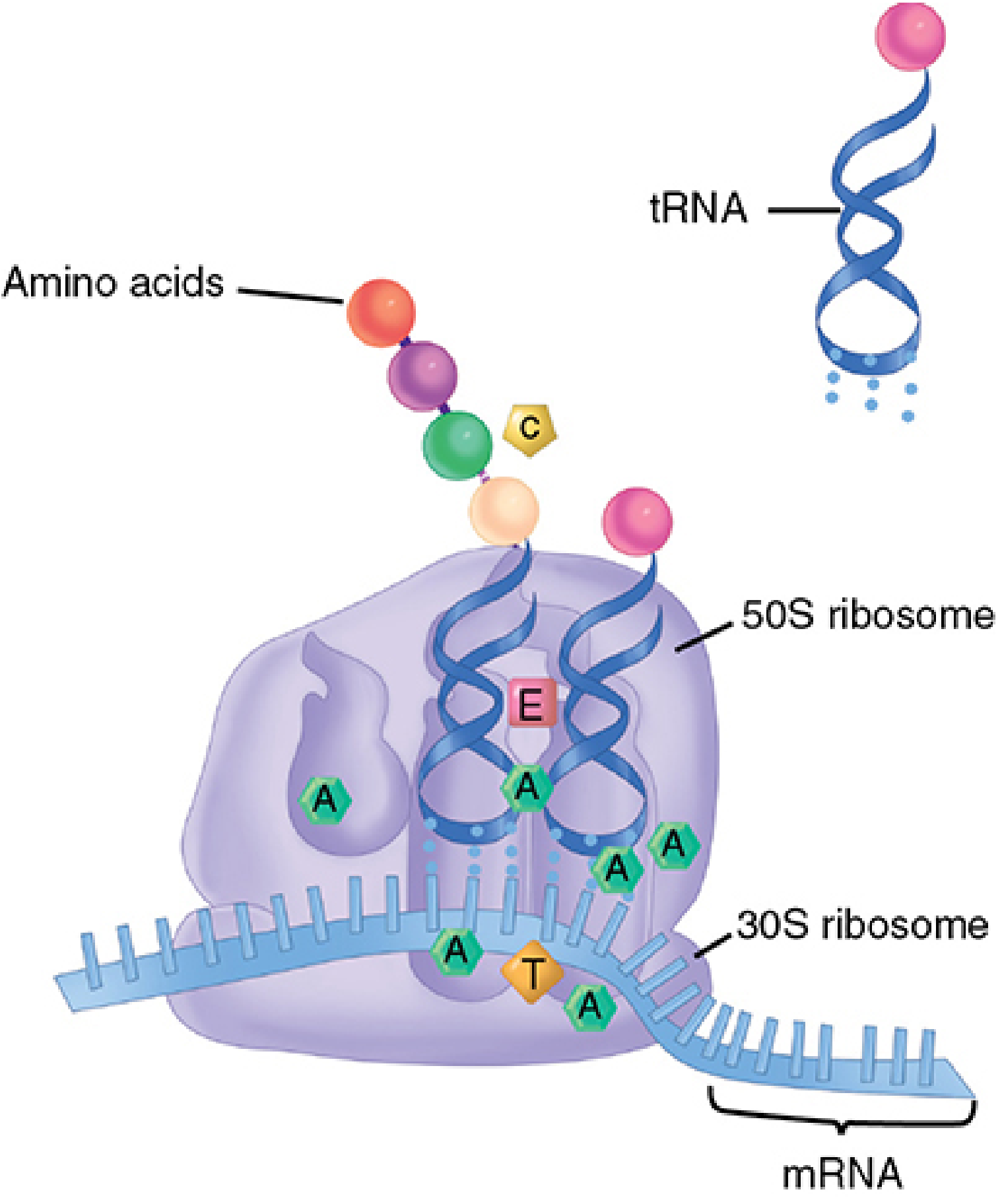
| Drug Class | Ribosome Target | Mechanism | Notes |
|---|---|---|---|
| Aminoglycosides (gentamicin, tobramycin, amikacin) | 30S + 50S | Disrupts initiation complexes; causes mRNA mistranslation | Require aerobic transport → inactive against anaerobes; nephrotoxic/ototoxic |
| Tetracyclines (doxycycline, minocycline) | 30S | Block aminoacyl-tRNA binding | Bacteriostatic; broad-spectrum; avoid in pregnancy/children |
| Chloramphenicol | 50S | Blocks peptidyl transferase (peptide bond formation) | Bacteriostatic; risk of aplastic anemia |
| Macrolides (erythromycin, azithromycin, clarithromycin) | 50S | Block tRNA translocation from acceptor to donor site | Bacteriostatic; atypicals coverage |
| Lincosamides (clindamycin) | 50S | Same as macrolides | Anaerobe coverage; C. difficile risk |
| Oxazolidinones (linezolid) | 50S | Block tRNA translocation | Active against multidrug-resistant Gram-positives |
| Streptogramins | 50S | Block tRNA translocation | — |
3. 🟢 Inhibitors of Nucleic Acid Synthesis
- Inhibit DNA gyrase (topoisomerase II) and topoisomerase IV → prevent DNA supercoiling and replication
- Bactericidal; broad Gram-negative coverage; newer agents cover Gram-positives and atypicals
- Structural analogs of PABA → competitively inhibit dihydropteroate synthase → block folate synthesis
- Bacteriostatic; humans obtain folate from diet (selective toxicity)
- Inhibits bacterial dihydrofolate reductase → prevents conversion of dihydrofolate to tetrahydrofolate
- Used with sulfamethoxazole (TMP-SMX / co-trimoxazole) for sequential blockade of folate pathway → synergistic bactericidal effect
- Nitro group is reduced under anaerobic conditions → toxic intermediates cause DNA strand breaks
- Active against a wide range of anaerobes including Bacteroides fragilis; also active against parasites (Trichomonas, Giardia, Entamoeba)
- Used for GI anaerobic infections (often combined with a β-lactam for polymicrobial coverage)
- Side effects: nausea, metallic taste, peripheral neuropathy; disulfiram-like reaction with alcohol
- Bind the β-subunit of DNA-dependent RNA polymerase → prevent initiation of RNA synthesis
- Active against Gram-positives, Neisseria, Haemophilus, and mycobacteria (cornerstone of TB therapy)
- Always combined with other drugs for active infections (rapid resistance develops by polymerase mutation)
- Solo use: chemoprophylaxis for N. meningitidis and H. influenzae contacts; latent TB
- Drug interactions: potent inducer of hepatic cytochrome P450 enzymes
- Rifaximin: non-absorbed oral form; used for bacterial diarrhea (E. coli)
4. 🔴 Disruptors of Cell Membrane Integrity
- Mimics phospholipid bilayer; inserts into Gram-positive bacterial membranes → forms pores → ion efflux → cell death
- Spectrum: Gram-positive only (including multidrug-resistant Enterococcus and S. aureus)
- Limitation: inactivated by pulmonary surfactant — cannot treat pneumonia
- Cationic detergent-like effect; bind and disrupt Gram-negative outer membranes → cytoplasmic contents leak out
- Spectrum: Gram-negative rods including P. aeruginosa
- Toxicity: nephrotoxicity, neurotoxicity — historically topical use only; now IV for multidrug-resistant Gram-negatives
Summary Table: Drug Classes at a Glance
| Class | Examples | Spectrum | Target | Cidal/Static |
|---|---|---|---|---|
| Penicillins | Amoxicillin, Piperacillin | Variable | PBPs (cell wall) | Cidal |
| Cephalosporins (1st–5th gen) | Cephalexin → Ceftaroline | Expanding with generation | PBPs | Cidal |
| Carbapenems | Imipenem, Meropenem | Very broad | PBPs | Cidal |
| Glycopeptides | Vancomycin, Teicoplanin | Gram + | Peptidoglycan precursor | Cidal |
| Aminoglycosides | Gentamicin, Amikacin | Gram – + some Gram + | 30S/50S ribosome | Cidal |
| Tetracyclines | Doxycycline | Broad (incl. atypicals) | 30S ribosome | Static |
| Macrolides | Azithromycin | Gram +, atypicals | 50S ribosome | Static |
| Fluoroquinolones | Ciprofloxacin, Levofloxacin | Broad | DNA gyrase/Topo IV | Cidal |
| Sulfonamides + TMP | Co-trimoxazole | Broad | Folate synthesis | Static/Cidal (combo) |
| Metronidazole | Flagyl | Anaerobes, parasites | DNA (via reduction) | Cidal |
| Rifamycins | Rifampin | Gram +, mycobacteria | RNA polymerase | Cidal |
| Lipopeptides | Daptomycin | Gram + only | Cell membrane | Cidal |
| Polymyxins | Colistin | Gram – only | Cell membrane | Cidal |
| Oxazolidinones | Linezolid | Gram + (MDR) | 50S ribosome | Static |
| Lincosamides | Clindamycin | Gram +, anaerobes | 50S ribosome | Static |
Antimicrobial Resistance — Key Mechanisms
- Enzymatic inactivation — β-lactamases hydrolyze the β-lactam ring
- Target modification — altered PBPs (MRSA), altered ribosomal subunits
- Efflux pumps — active drug expulsion from the cell
- Reduced permeability — porin channel mutations (Gram-negatives)
- Bypass pathways — altered metabolic pathway that doesn't require the drug target
I need explain and name of drugs
Antibacterial & Antimicrobial Drugs — Names & Explanation
1. 🔵 PENICILLINS — Cell Wall Synthesis Inhibitors
| Generation | Drug Names | Spectrum |
|---|---|---|
| Natural | Penicillin G, Penicillin V | Gram-positive cocci & rods, Gram-negative cocci, most anaerobes |
| Antistaphylococcal | Nafcillin, Oxacillin, Dicloxacillin | MSSA (methicillin-sensitive S. aureus) |
| Broad-spectrum | Ampicillin, Amoxicillin | Above + Gram-negatives (E. coli, Proteus, Salmonella, Shigella, H. influenzae) |
| Anti-pseudomonal | Carbenicillin, Ticarcillin | Gram-negatives + Pseudomonas |
| Extended | Piperacillin | Gram-negatives + Klebsiella, enterococci, B. fragilis, Pseudomonas |
- Amoxicillin/Clavulanate (Augmentin)
- Ticarcillin/Clavulanate
- Ampicillin/Sulbactam
- Piperacillin/Tazobactam (Pip-Tazo)
2. 🔵 CEPHALOSPORINS — Cell Wall Synthesis Inhibitors
| Generation | Drug Names | Key Uses |
|---|---|---|
| 1st | Cefazolin, Cephalexin, Cefadroxil | Gram-positive cocci, E. coli, Proteus, Klebsiella; surgical prophylaxis |
| 2nd | Cefaclor, Cefuroxime, Cefprozil | More Gram-negative (H. influenzae, Moraxella); less staphylococcal |
| 2nd (cephamycins) | Cefotetan, Cefoxitin | Bacteroides (anaerobic coverage) |
| 3rd | Ceftriaxone, Cefotaxime, Ceftazidime, Cefdinir, Cefixime, Cefpodoxime | Gram-negative meningitis, gonorrhea; Ceftazidime covers Pseudomonas |
| 4th | Cefepime | Broad Gram-negative + Pseudomonas + better Gram-positive |
| 5th | Ceftaroline | Covers MRSA (methicillin-resistant S. aureus) |
3. 🔵 CARBAPENEMS — Cell Wall Synthesis Inhibitors (Broadest Spectrum)
| Drug Name | Notes |
|---|---|
| Imipenem/Cilastatin | Cilastatin prevents renal inactivation |
| Meropenem | Less seizure risk than imipenem |
| Ertapenem | Once daily; no Pseudomonas coverage |
| Doripenem | Pseudomonas coverage |
4. 🔵 GLYCOPEPTIDES — Cell Wall Synthesis Inhibitors
| Drug Name | Key Use |
|---|---|
| Vancomycin | MRSA, Clostridioides difficile (oral) |
| Teicoplanin | Similar to vancomycin |
| Dalbavancin, Oritavancin | Long-acting; once-weekly dosing |
5. 🟡 AMINOGLYCOSIDES — Protein Synthesis Inhibitors (30S + 50S)
- Inactive against anaerobes (no oxygen-dependent transport)
- Inactive against intracellular organisms (Rickettsia, Chlamydia)
| Drug Name | Spectrum |
|---|---|
| Gentamicin | Broad Gram-negative including P. aeruginosa |
| Tobramycin | Pseudomonas (preferred in CF patients) |
| Amikacin | MDR Gram-negatives |
| Streptomycin | M. tuberculosis, tularemia, plague |
| Neomycin | Topical use only |
6. 🟡 TETRACYCLINES — Protein Synthesis Inhibitors (30S)
| Drug Name | Notes |
|---|---|
| Doxycycline | Most commonly used; atypicals, STIs, malaria prophylaxis |
| Minocycline | CNS penetration; acne |
| Tetracycline | H. pylori (with other agents) |
| Tigecycline | Covers MDR organisms including MRSA & VRE |
7. 🟡 MACROLIDES — Protein Synthesis Inhibitors (50S)
| Drug Name | Notes |
|---|---|
| Azithromycin (Z-pack) | Long half-life (single dose); respiratory, STIs |
| Clarithromycin | H. pylori triple therapy; MAC prophylaxis |
| Erythromycin | Oldest; GI prokinetic effect; many drug interactions |
8. 🟡 CLINDAMYCIN (Lincosamide) — Protein Synthesis Inhibitor (50S)
- Drug: Clindamycin
- Spectrum: Gram-positive organisms + anaerobes (B. fragilis); MRSA (skin infections)
- Side effects: ⚠️ Risk of Clostridioides difficile colitis (pseudomembranous colitis)
9. 🟡 OXAZOLIDINONES — Protein Synthesis Inhibitors (50S)
| Drug Name | Notes |
|---|---|
| Linezolid | MRSA, VRE; used when vancomycin fails or not tolerated |
| Tedizolid | Newer; fewer side effects |
10. 🟢 FLUOROQUINOLONES — DNA Synthesis Inhibitors
| Generation | Drug Names | Spectrum |
|---|---|---|
| 1st | Nalidixic acid | Urinary Gram-negatives only |
| 2nd | Ciprofloxacin, Ofloxacin | Broad Gram-negatives, P. aeruginosa, some Gram-positives |
| 3rd | Levofloxacin | + Gram-positives, atypicals ("respiratory quinolone") |
| 4th | Moxifloxacin | + Anaerobes; no Pseudomonas |
11. 🟢 SULFONAMIDES + TRIMETHOPRIM — Folate Synthesis Inhibitors
- Sulfonamides → inhibit dihydropteroate synthase (compete with PABA) → block folate production
- Trimethoprim → inhibit dihydrofolate reductase → block folate conversion
- Together (TMP-SMX / Co-trimoxazole) = sequential double blockade → synergistic, bactericidal
| Drug | Use |
|---|---|
| TMP-SMX (Co-trimoxazole) | UTIs, Pneumocystis jirovecii pneumonia (PCP), MRSA skin infections |
| Sulfadiazine | Toxoplasmosis (with pyrimethamine) |
| Sulfasalazine | IBD |
| Silver sulfadiazine | Burn wound infections (topical) |
12. 🟢 RIFAMYCINS — RNA Synthesis Inhibitors
| Drug Name | Use |
|---|---|
| Rifampin (Rifampicin) | TB treatment (always combined); meningococcal prophylaxis; leprosy |
| Rifabutin | TB in HIV patients (less CYP induction) |
| Rifaximin | Non-absorbed oral; traveler's diarrhea, hepatic encephalopathy |
13. 🟢 METRONIDAZOLE (Nitroimidazole) — DNA Disruptor
- Drug: Metronidazole (Flagyl)
- Spectrum: Anaerobes (B. fragilis, C. difficile), protozoa (Giardia, Trichomonas, Entamoeba)
- Side effects: Nausea, metallic taste, peripheral neuropathy; disulfiram-like reaction with alcohol (avoid alcohol during treatment)
14. 🔴 CELL MEMBRANE DISRUPTORS
Daptomycin (Lipopeptide)
- Mechanism: Inserts into Gram-positive bacterial membrane → forms ion pores → cell death → bactericidal
- Spectrum: Gram-positive ONLY — including MRSA and VRE
- ⚠️ Cannot treat pneumonia — inactivated by pulmonary surfactant
- Side effects: Myopathy (monitor CK)
Polymyxins
| Drug | Use |
|---|---|
| Polymyxin B | Topical + IV for MDR Gram-negatives |
| Colistin (Polymyxin E) | Last resort for Acinetobacter, Pseudomonas MDR |
- Mechanism: Cationic detergent action → disrupt Gram-negative outer membrane → contents leak → bactericidal
- Side effects: ⚠️ Nephrotoxicity + Neurotoxicity
Quick Visual Summary
CELL WALL → Penicillins, Cephalosporins, Carbapenems, Glycopeptides
PROTEIN (30S) → Aminoglycosides, Tetracyclines
PROTEIN (50S) → Macrolides, Clindamycin, Linezolid, Chloramphenicol
DNA/RNA SYNTHESIS → Fluoroquinolones, Rifamycins, Metronidazole
FOLATE PATHWAY → Sulfonamides, Trimethoprim
CELL MEMBRANE → Daptomycin, Polymyxins
Classification of antibacterial and antimicrobial
Classification of Antibacterial & Antimicrobial Drugs
"The broad classification of antibiotics follows the classification of microorganisms closely, so that we have antibacterial, antiviral, antifungal, and antiparasitic agents." — Goodman & Gilman's The Pharmacological Basis of Therapeutics
LEVEL 1 — Broadest Classification: By Target Microorganism
ANTIMICROBIAL DRUGS
├── 1. ANTIBACTERIAL (act on bacteria)
├── 2. ANTIVIRAL (act on viruses)
├── 3. ANTIFUNGAL (act on fungi)
└── 4. ANTIPARASITIC (act on parasites)
LEVEL 2 — Classification of ANTIBACTERIAL Drugs
A. BY MECHANISM OF ACTION (most important classification)
🔵 1. CELL WALL SYNTHESIS INHIBITORS
| Class | Drugs | Mechanism |
|---|---|---|
| Penicillins | Penicillin G/V, Ampicillin, Amoxicillin, Nafcillin, Oxacillin, Piperacillin | Bind PBPs → block peptidoglycan cross-linking |
| Cephalosporins (1st–5th gen) | Cefazolin, Ceftriaxone, Cefepime, Ceftaroline | Same as penicillins |
| Carbapenems | Imipenem, Meropenem, Ertapenem, Doripenem | Same; broadest β-lactam spectrum |
| Monobactams | Aztreonam | Gram-negative only; safe in penicillin allergy |
| Glycopeptides | Vancomycin, Teicoplanin, Dalbavancin | Bind D-Ala-D-Ala precursor → block transglycosylation |
| Lipoglycopeptides | Telavancin, Oritavancin | Dual action: cell wall + membrane |
| β-Lactamase Inhibitors (used in combination) | Clavulanate, Sulbactam, Tazobactam, Avibactam | Protect β-lactams from enzymatic destruction |
🟡 2. PROTEIN SYNTHESIS INHIBITORS
| Ribosomal Target | Class | Drugs | Effect |
|---|---|---|---|
| 30S subunit | Aminoglycosides | Gentamicin, Tobramycin, Amikacin, Streptomycin | Bactericidal — disrupt initiation complex, cause mRNA mistranslation |
| 30S subunit | Tetracyclines | Tetracycline, Doxycycline, Minocycline, Tigecycline | Bacteriostatic — block tRNA binding |
| 50S subunit | Macrolides | Erythromycin, Azithromycin, Clarithromycin | Bacteriostatic — block tRNA translocation |
| 50S subunit | Lincosamides | Clindamycin | Bacteriostatic — same site as macrolides |
| 50S subunit | Chloramphenicol | Chloramphenicol | Bacteriostatic — blocks peptidyl transferase |
| 50S subunit | Oxazolidinones | Linezolid, Tedizolid | Bacteriostatic — block ribosome assembly |
| 50S subunit | Streptogramins | Quinupristin/Dalfopristin | Bactericidal (in combination) |
| 50S subunit | Pleuromutilins | Lefamulin | Bacteriostatic — block tRNA translocation |
🟢 3. NUCLEIC ACID SYNTHESIS INHIBITORS
| Class | Drugs | Target | Effect |
|---|---|---|---|
| Fluoroquinolones | Ciprofloxacin, Levofloxacin, Moxifloxacin, Ofloxacin | DNA gyrase (Topo II) + Topo IV | Bactericidal |
| Rifamycins | Rifampin, Rifabutin, Rifaximin | β-subunit of RNA polymerase | Bactericidal |
| Nitroimidazoles | Metronidazole, Tinidazole | DNA strand breaks (anaerobic reduction) | Bactericidal (anaerobes only) |
| Nitrofurans | Nitrofurantoin | Multiple intracellular targets | Bacteriostatic/cidal (urinary tract only) |
🟠 4. FOLATE SYNTHESIS INHIBITORS (antimetabolites)
| Class | Drugs | Target |
|---|---|---|
| Sulfonamides | Sulfamethoxazole, Sulfadiazine, Silver sulfadiazine | Dihydropteroate synthase (blocks PABA conversion) |
| Diaminopyrimidines | Trimethoprim | Dihydrofolate reductase |
| Combination | TMP-SMX (Co-trimoxazole) | Sequential double blockade → synergistic |
🔴 5. CELL MEMBRANE DISRUPTORS
| Class | Drugs | Spectrum | Mechanism |
|---|---|---|---|
| Lipopeptides | Daptomycin | Gram-positive only (MRSA, VRE) | Insert into membrane → pores → ion efflux |
| Polymyxins | Polymyxin B, Colistin | Gram-negative only (MDR) | Detergent-like → outer membrane disruption |
B. BY SPECTRUM OF ACTIVITY
NARROW SPECTRUM
├── Gram-positive only: Penicillin G/V, Vancomycin, Daptomycin
├── Gram-negative only: Aztreonam, Colistin/Polymyxins
└── Specific organisms: Metronidazole (anaerobes), Rifampin (mycobacteria)
BROAD SPECTRUM (Gram-positive + Gram-negative)
├── Moderate broad: Ampicillin, Amoxicillin
├── True broad: Tetracyclines, Fluoroquinolones, TMP-SMX
└── Very broad: Carbapenems, Piperacillin-Tazobactam, Tigecycline
C. BY EFFECT ON BACTERIA
| Category | Definition | Examples |
|---|---|---|
| Bactericidal | Kills bacteria directly | β-Lactams, Aminoglycosides, Fluoroquinolones, Rifamycins, Daptomycin, Metronidazole (anaerobes) |
| Bacteriostatic | Inhibits growth; host defenses clear the infection | Tetracyclines, Macrolides, Clindamycin, Linezolid, Chloramphenicol, TMP-SMX |
⚠️ This distinction is not absolute — some drugs are cidal at high concentrations and static at low concentrations.
D. BY CHEMICAL STRUCTURE / SOURCE
| Type | Description | Examples |
|---|---|---|
| Natural antibiotics | Produced by molds (Penicillium) or bacteria (Streptomyces) | Penicillin G, Streptomycin, Erythromycin, Chloramphenicol, Tetracycline |
| Semi-synthetic | Chemically modified natural antibiotics (broader spectrum, better PK) | Ampicillin, Amoxicillin, Cephalosporins, Amikacin, Doxycycline |
| Fully synthetic | Chemically designed from scratch | Fluoroquinolones, Sulfonamides, Trimethoprim, Metronidazole, Linezolid |
LEVEL 3 — Classification by Type of Infection / Clinical Use
| Infection Type | Drug of Choice |
|---|---|
| MRSA | Vancomycin, Linezolid, Daptomycin |
| Anaerobic infections | Metronidazole, Clindamycin, Carbapenems |
| Pseudomonas | Pip-Tazo, Ceftazidime, Ciprofloxacin, Colistin |
| Atypicals (Mycoplasma, Chlamydia, Legionella) | Doxycycline, Azithromycin, Fluoroquinolones |
| Mycobacteria (TB) | Rifampin, Isoniazid, Pyrazinamide, Ethambutol |
| Meningitis (Gram-negative) | Ceftriaxone, Cefotaxime |
| UTI | TMP-SMX, Nitrofurantoin, Fluoroquinolones |
LEVEL 4 — Full Antimicrobial Classification (Beyond Antibacterials)
ALL ANTIMICROBIAL DRUGS
│
├── ANTIBACTERIAL ──── (all classes above)
│
├── ANTIFUNGAL
│ ├── Polyenes: Amphotericin B, Nystatin
│ ├── Azoles: Fluconazole, Itraconazole, Voriconazole
│ ├── Echinocandins: Caspofungin, Micafungin, Anidulafungin
│ └── Pyrimidines: Flucytosine (5-FC)
│
├── ANTIVIRAL
│ ├── Anti-Herpes: Acyclovir, Valacyclovir, Ganciclovir
│ ├── Anti-Influenza: Oseltamivir, Zanamivir
│ ├── Anti-HIV (ARVs): NRTIs, NNRTIs, PIs, INSTIs, Fusion inhibitors
│ └── Anti-HCV/HBV: Sofosbuvir, Tenofovir, Entecavir
│
└── ANTIPARASITIC
├── Antiprotozoals: Metronidazole, Chloroquine, Quinine
├── Antihelminthics: Albendazole, Mebendazole, Ivermectin
└── Ectoparasiticides: Permethrin, Lindane
Master Summary Diagram
ANTIBACTERIAL CLASSIFICATION
│
├── BY MECHANISM
│ ├── 1. Cell Wall → Penicillins, Cephalosporins, Carbapenems, Glycopeptides
│ ├── 2. Protein (30S) → Aminoglycosides, Tetracyclines
│ ├── 3. Protein (50S) → Macrolides, Clindamycin, Chloramphenicol, Linezolid
│ ├── 4. DNA/RNA → Fluoroquinolones, Rifamycins, Metronidazole
│ ├── 5. Folate → Sulfonamides, Trimethoprim
│ └── 6. Membrane → Daptomycin (G+), Polymyxins (G-)
│
├── BY SPECTRUM
│ ├── Narrow-spectrum
│ └── Broad-spectrum
│
├── BY EFFECT
│ ├── Bactericidal
│ └── Bacteriostatic
│
└── BY SOURCE
├── Natural (from Penicillium / Streptomyces)
├── Semi-synthetic
└── Fully synthetic
1. Patient K., 42 years old. With complaints of high body temperature (39C), cough with mucous sputum, shortness of breath, weakness. The disease began acutely, after being exposed to cold rain, cough with mucous sputum, mixed dyspnea and fever (39.0) began to disturb. The patient took aspirin and analgin and called an ambulance Moderate condition over auscultatory points. Notes allergy to allergy to ampicillin, penicillin History of CKD. The patient has been on hemodialysis for a year. On the ECG: Normal position of the EOS. Sinus tachycardia. Elongation QT up to 0.22 sec. Clinical blood test: Erythrocytes-4.5x10^12/1 Hb-131 اع Leukocytes-15.3x10^9/л COE-30 mm/h X-ray examination - The picture shows the chest of the usual form. The roots of the lungs are dilated. The pulmonary pattern is infiltrated on the right. Sinuses are free. Heart without features. Diagnosis P-treatment Short
Clinical Case Analysis — Patient K., 42 years old
🔍 CLINICAL DATA SUMMARY
| Parameter | Finding |
|---|---|
| Age/Sex | 42 years old |
| Onset | Acute, after cold exposure |
| Symptoms | Fever 39°C, productive cough (mucous sputum), mixed dyspnea, weakness |
| Allergies | ⚠️ Ampicillin, Penicillin |
| Comorbidities | ⚠️ Chronic Kidney Disease (CKD) — on hemodialysis × 1 year |
| ECG | Sinus tachycardia; ⚠️ QT prolongation = 0.22 sec |
| WBC | 15.3 × 10⁹/L (leukocytosis) |
| ESR | 30 mm/h (elevated) |
| Hb | 131 g/L (mild anemia, expected in CKD) |
| RBC | 4.5 × 10¹²/L |
| Chest X-ray | Dilated lung roots; infiltration of pulmonary pattern on the right; free sinuses; heart normal |
✅ DIAGNOSIS
ICD-10: J18.9 — Pneumonia, unspecified
Justification:
| Criterion | Evidence |
|---|---|
| Acute onset | After cold rain exposure |
| Fever | 39°C — high-grade |
| Respiratory symptoms | Cough with mucous sputum + mixed dyspnea |
| Leukocytosis | WBC 15.3 × 10⁹/L |
| Elevated ESR | 30 mm/h |
| Radiological confirmation | Right-sided pulmonary infiltration + dilated lung roots |
| Severity — moderate | Hospitalization required; fever 39°C; leukocytosis; dyspnea |
⚠️ KEY CLINICAL CONSTRAINTS THAT DRIVE TREATMENT
| Constraint | Implication |
|---|---|
| Allergy: Ampicillin + Penicillin | ALL β-lactams must be used with caution; avoid aminopenicillins entirely |
| CKD on hemodialysis | Renally-excreted drugs require dose adjustment; avoid nephrotoxic agents |
| QT prolongation on ECG (0.22 sec) | ⚠️ Avoid fluoroquinolones (levofloxacin, moxifloxacin) and macrolides (azithromycin) — all prolong QT further → risk of Torsades de Pointes |
💊 TREATMENT PLAN
🔴 Drugs to AVOID in this patient:
| Drug | Reason to Avoid |
|---|---|
| Ampicillin, Amoxicillin, Amoxicillin/Clavulanate | Direct allergy |
| Levofloxacin, Moxifloxacin | QT prolongation (already present on ECG) |
| Azithromycin | QT prolongation |
| Aminoglycosides (Gentamicin, Tobramycin) | Nephrotoxic — contraindicated with CKD |
| Vancomycin | Nephrotoxic — use with extreme caution only if essential |
✅ RECOMMENDED ANTIBIOTIC REGIMEN
⚠️ Cross-reactivity between penicillins and cephalosporins is very low (~1–2%). Ceftriaxone is considered safe in penicillin-allergic patients unless they had anaphylaxis to penicillin. Since the allergy is documented but severity is not specified as anaphylaxis, ceftriaxone can be used with monitoring.
| Drug | Dose | Route | Frequency | Duration |
|---|---|---|---|---|
| Ceftriaxone | 1–2 g | IV | Once daily | 7–10 days |
- Excellent coverage of Streptococcus pneumoniae (most common CAP pathogen)
- Covers H. influenzae, Gram-negative pathogens
- Does NOT prolong QT
- No dose adjustment needed in renal failure (hepatically excreted — safe in hemodialysis)
- Not a penicillin (different β-lactam ring side chain)
Atypical Coverage (if clinical features suggest atypical pneumonia):
| Drug | Dose | Route | Note |
|---|---|---|---|
| Doxycycline | 100 mg | PO | Twice daily × 5–7 days; does NOT prolong QT; dose adjustment not required in dialysis |
Doxycycline is preferred over azithromycin here because it does not prolong QT.
Antipyretic / Symptomatic Treatment:
| Drug | Dose | Note |
|---|---|---|
| Paracetamol (Acetaminophen) | 500–1000 mg PO q6–8h | Safe in CKD on dialysis; avoid NSAIDs (ibuprofen) — worsen renal function |
| Mucolytic (Ambroxol / Acetylcysteine) | Ambroxol 30 mg PO 3× daily | Facilitates sputum clearance |
| IV Fluids | 0.9% NaCl — cautious | Volume carefully monitored in dialysis patient |
| O₂ supplementation | Target SpO₂ ≥ 94% | If dyspnea/hypoxia present |
⚠️ Drugs Taken by Patient (Aspirin + Analgin):
- Aspirin — acceptable for fever, but NSAIDs worsen renal function in CKD; switch to paracetamol
- Analgin (Metamizole) — avoid; risk of agranulocytosis and nephrotoxicity
📋 SHORT TREATMENT SUMMARY
DIAGNOSIS:
Community-Acquired Pneumonia (CAP), right-sided, moderate severity
─────────────────────────────────────────────────────────────
ANTIBIOTICS:
1. Ceftriaxone 1–2 g IV once daily × 7–10 days
(No QT prolongation | No renal dose adjustment |
Safe with penicillin allergy)
2. Doxycycline 100 mg PO twice daily × 5–7 days
(Add if atypical coverage needed | Does NOT prolong QT)
─────────────────────────────────────────────────────────────
SUPPORTIVE:
• Paracetamol 500–1000 mg q6–8h (replace Aspirin + Analgin)
• Ambroxol 30 mg 3× daily (mucolytic)
• O₂ therapy if SpO₂ < 94%
• Careful IV fluids (dialysis patient)
─────────────────────────────────────────────────────────────
MONITORING:
• Daily ECG (QT interval — already prolonged!)
• Renal function / dialysis schedule
• WBC, CRP, temperature trend
• Chest X-ray at 7–10 days to assess resolution
─────────────────────────────────────────────────────────────
AVOID:
✗ Fluoroquinolones (QT prolongation)
✗ Azithromycin (QT prolongation)
✗ Aminoglycosides (nephrotoxic)
✗ Ampicillin/Amoxicillin (allergy)
✗ NSAIDs (worsen renal function)
In short
Patient K., 42 y/o — Short Summary
DIAGNOSIS
3 KEY CONSTRAINTS
| ⚠️ Problem | Impact on Treatment |
|---|---|
| Allergy: Penicillin + Ampicillin | Avoid all aminopenicillins |
| CKD on hemodialysis | Avoid nephrotoxic drugs; adjust doses |
| QT prolonged (0.22 sec) on ECG | Avoid fluoroquinolones + azithromycin |
TREATMENT
- Ceftriaxone 1–2 g IV once daily × 7–10 days (Safe: no QT effect, no renal dose adjustment, low cross-reactivity with penicillin)
- Paracetamol 500–1000 mg q6–8h (replace Aspirin/Analgin)
- Ambroxol 30 mg × 3/day (mucolytic)
- O₂ if SpO₂ < 94%
AVOID
- ❌ Fluoroquinolones (levofloxacin) — QT prolongation
- ❌ Azithromycin — QT prolongation
- ❌ Aminoglycosides — nephrotoxic
- ❌ Ampicillin/Amoxicillin — allergy
- ❌ NSAIDs — worsen renal function