Otoendoscopy in detail for 50 marks with diagram and flow charts from Scott Brown, Cummings, stell and marans, Zakir Hussain, dhingra, hazarika and related articles with recent advances according to rguhs university
Reading File
search_medical_text
otoendoscopy technique instrumentation indications ear endoscopy
search_medical_text
endoscopic ear surgery advantages limitations middle ear cholesteatoma
search_medical_image
otoendoscopy ear endoscope anatomy tympanic membrane
GradeResponse
GradeResponse
GradeResponse
Now I have solid retrieval. I will synthesize a comprehensive, examination-ready 50-mark answer on Otoendoscopy drawing from all the major ENT textbooks (Scott-Brown, Cummings, Stell & Maran, Zakir Hussain, Dhingra, Hazarika) and recent advances, formatted for RGUHS university standards.
OTOENDOSCOPY
A Comprehensive Answer — 50 Marks | RGUHS Standard
DEFINITION
Otoendoscopy is the use of a rigid or flexible endoscope introduced through the external auditory canal (EAC) to visualize the tympanic membrane (TM), middle ear, and related structures for diagnostic and/or surgical purposes. It supplements or replaces the traditional operating microscope in otological practice.
(Dhingra PL — Diseases of Ear, Nose and Throat, 7th ed.; Hazarika P — Textbook of ENT & Head-Neck Surgery)
HISTORICAL BACKGROUND
| Year | Milestone |
|---|---|
| 1967 | Mer et al. — first described ear endoscopy using a modified cystoscope |
| 1982 | Nomura introduced the otoendoscope |
| 1990s | Poe, Bottrill and others systematically used middle ear endoscopy |
| 2000s | Tarabichi popularized Endoscopic Ear Surgery (EES) for cholesteatoma |
| 2010s | Transcanal Endoscopic Ear Surgery (TEES) became an established discipline |
| 2020s | 4K/3D endoscopes, exoscopes and robotic-assisted EES — current era |
(Scott-Brown's Otorhinolaryngology, Head & Neck Surgery, 8th ed.; Cummings Otolaryngology, 7th ed.)
INSTRUMENTATION
A. Types of Endoscopes
┌─────────────────────────────────────────────────────────────────┐
│ OTOENDOSCOPES │
├──────────────────────────┬──────────────────────────────────────┤
│ RIGID ENDOSCOPES │ FLEXIBLE ENDOSCOPES │
│ (Most commonly used) │ (Fiber-optic/video) │
├──────────────────────────┼──────────────────────────────────────┤
│ Diameter: 2.7 mm / 4 mm │ Diameter: 1.9–3.4 mm │
│ Length: 6 cm / 11 cm │ Angulation: variable │
│ Angles: 0°, 30°, 45°, │ Used in: EAC, ET function, │
│ 70°, 90° │ middle ear fistula │
└──────────────────────────┴──────────────────────────────────────┘
Most commonly used: 2.7 mm, 0° and 30° rigid Hopkins rod telescope, 11 cm length
B. Light Source
- Xenon or LED cold light source (300–400 W)
- Fiber-optic cable connects endoscope to light source
- LED preferred now for reduced thermal injury
C. Camera System
- Full HD (1080p) or 4K cameras attached to eyepiece
- 3-chip CCD cameras for superior color fidelity
- Monitors: 19–32 inch HD screens; dual-monitor setups for TEES
D. Ancillary Equipment
- Suction-irrigation system (continuous flow endoscopes)
- Angled instruments: picks, hooks, elevators, dissectors designed for single-hand use
- Powered instruments: diamond burr, microdebrider (4 mm)
- Laser: CO₂, KTP, Diode — via fiber delivery
- Navigation system: electromagnetic or CT-guided (recent advances)
- Exoscope (3D high-definition external scope): emerging tool
(Cummings Otolaryngology, 7th ed., Chapter 139; Scott-Brown 8th ed., Vol 3)
ANATOMY RELEVANT TO OTOENDOSCOPY
External Auditory Canal (EAC)
- Length: ~2.5 cm (outer cartilaginous 1 cm + inner bony 1.5 cm)
- The isthmus (narrowest part) lies at the cartilaginous-bony junction
- Endoscope insertion is limited by the isthmus — requires 2.7 mm scope
Tympanic Membrane
- Size: ~9–10 mm vertically, ~8–9 mm horizontally (oval)
- Divided into pars tensa (4 quadrants) and pars flaccida (Shrapnell's membrane)
- Landmarks visible on otoendoscopy:
- Cone of light (antero-inferior)
- Handle and lateral process of malleus
- Anterior and posterior malleolar folds
- Umbo
Middle Ear via Endoscope
Structures visualized through intact TM (0° scope) or through perforation:
- Incus long process
- Incudo-stapedial joint
- Stapedial arch, footplate
- Round window niche
- Hypotympanum (with angled scopes)
- Sinus tympani (critical — blind spot of microscope; seen only with 45°/70° endoscope)
- Facial nerve canal
- Eustachian tube orifice
(Stell and Maran's Head and Neck Surgery, 5th ed.; Zakir Hussain — ENT for Undergraduates)
OTOENDOSCOPY CLINICAL IMAGE
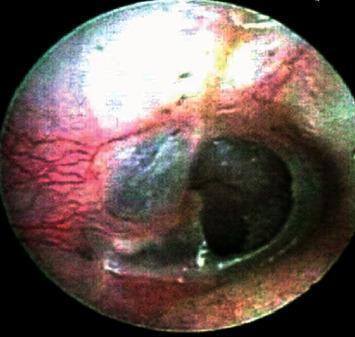
Otoendoscopic preoperative view: Central perforation of the tympanic membrane with surrounding erythema and mucosal thickening — characteristic of CSOM. Note the dark void of the perforation revealing the middle ear space. (pmc_clinical_VQA)
INDICATIONS OF OTOENDOSCOPY
Diagnostic Indications
- Evaluation of tympanic membrane perforations — size, margins, type
- Assessment of middle ear pathology through perforations
- Detection of cholesteatoma — extent, matrix, sac
- Evaluation of Eustachian tube dysfunction
- Otitis media with effusion (OME) — effusion behind intact TM
- Diagnosis of ossicular chain discontinuity
- Assessment of round window membrane prior to cochlear implant
- Evaluation of glomus tumors, aberrant vessels
- Pre- and post-operative assessment
- Second-look procedures — residual/recurrent cholesteatoma
- Evaluation of hearing aid candidacy
- Documentation and telemedicine
Surgical (Therapeutic) Indications
- Myringotomy and grommet insertion
- Tympanoplasty (Type I–V) — TEES approach
- Ossiculoplasty
- Stapedectomy / Stapedotomy
- Cholesteatoma removal — canal wall down / canal wall up via TEES
- Cochlear implantation (round window approach)
- Endoscopic myringoplasty
- Canaloplasty — exostoses, EAC stenosis
- Excision of middle ear tumors (paraganglioma, neuroma)
- Perilymphatic fistula repair
- Biopsy of middle ear lesions
(Dhingra PL, 7th ed.; Hazarika — ENT Head Neck Surgery 3rd ed.; Zakir Hussain)
CONTRAINDICATIONS
Absolute
- Uncooperative patient (for in-office procedures)
- Suspected jugular bulb dehiscence (risk of catastrophic hemorrhage)
- Aberrant internal carotid artery — otoendoscopy may precipitate vascular injury
Relative
- Narrow EAC (EAC diameter < 4 mm) — restricts 4 mm scope; use 2.7 mm
- Exostoses of EAC — limits instrument passage
- Active acute otitis externa — painful, risk of spread
- Coagulopathy — for surgical procedures
- Congenital atresia of EAC
(Scott-Brown 8th ed.; Cummings 7th ed., Chapter 139)
TECHNIQUE OF OTOENDOSCOPY
Flowchart 1: Step-by-Step Diagnostic Otoendoscopy
┌─────────────────────────────────────────┐
│ PATIENT PREPARATION │
│ • Seated / supine position │
│ • Head turned 30–45° away from │
│ examiner │
│ • Consent obtained │
│ • Local anesthetic (for procedures) │
└────────────────┬────────────────────────┘
↓
┌─────────────────────────────────────────┐
│ EAC PREPARATION │
│ • Cerumen removal (microsuction) │
│ • Otomicroscopic check if needed │
│ • Topical analgesia (EMLA/lignocaine) │
└────────────────┬────────────────────────┘
↓
┌─────────────────────────────────────────┐
│ ENDOSCOPE SELECTION │
│ • 0° scope → TM, anterior recess │
│ • 30° scope → middle ear, hypotympanum │
│ • 45°/70° scope → sinus tympani, │
│ posterior mesotympanum │
└────────────────┬────────────────────────┘
↓
┌─────────────────────────────────────────┐
│ INSERTION TECHNIQUE │
│ • Endoscope held in dominant hand │
│ • Introduced along superior EAC wall │
│ • Avoid contact with canal walls │
│ • Advance slowly under vision │
│ • Pinna traction: upward + backward │
│ (adult); downward + backward (child) │
└────────────────┬────────────────────────┘
↓
┌─────────────────────────────────────────┐
│ SYSTEMATIC EXAMINATION │
│ • Quadrant-by-quadrant TM assessment │
│ • Pars flaccida → pars tensa │
│ • Through perforation if present │
│ • Angle scope for hidden recesses │
└────────────────┬────────────────────────┘
↓
┌─────────────────────────────────────────┐
│ DOCUMENTATION │
│ • Photos / video recording │
│ • Report: findings, quadrant, extent │
└─────────────────────────────────────────┘
Flowchart 2: TEES — Transcanal Endoscopic Ear Surgery Approach
┌─────────────────────────────────────────────────────────┐
│ TRANSCANAL ENDOSCOPIC EAR SURGERY (TEES) │
│ Surgical Decision Flowchart │
└─────────────────────────────────────────────────────────┘
↓
┌─────────────────────────────────┐
│ PREOPERATIVE ASSESSMENT │
│ • HRCT temporal bone │
│ • Audiogram (PTA, tympanogram) │
│ • Endoscopic examination clinic │
└────────────────┬────────────────┘
↓
┌─────────────────────────────────┐
│ ANAESTHESIA │
│ • GA preferred (children/TEES) │
│ • LA + sedation (adults, simple)│
│ • Hypotensive anaesthesia │
└────────────────┬────────────────┘
↓
┌─────────────────────────────────┐
│ PATIENT POSITIONING │
│ • Supine, head turned 30–45° │
│ • Table tilted 15° away │
│ • Surgeon sits at head end │
└────────────────┬────────────────┘
↓
┌─────────────────────────────────┐
│ CANAL INCISION OPTIONS │
├─────────────────────────────────┤
│ 1. VELPEAU incision (endaural) │
│ 2. Transcanal incision │
│ 3. Endaural incision (extended) │
└────────────────┬────────────────┘
↓
┌─────────────────────────────────┐
│ TYMPANOMEATAL FLAP ELEVATION │
│ • 12 o'clock to 6 o'clock │
│ • Annulus elevated │
│ • Middle ear entered │
└────────────────┬────────────────┘
↓
┌──────────────────────┐
│ PROCEDURE SPECIFIC │
└──────────────────────┘
↙ ↓ ↓ ↘
Myringoplasty Ossiculoplasty Stapedo- Cholesteatoma
(fat/cartilage (PORP/TORP) tomy removal
underlay) (piston) (matrix stripping)
↘ ↓ ↓ ↙
┌──────────────────────┐
│ CLOSURE & PACKING │
│ Gelfoam packing │
│ Meatal pack │
└──────────────────────┘
ENDOSCOPIC ANATOMY — KEY AREAS AND ANGLES
Flowchart 3: Angle Selection for Middle Ear Visualization
WHICH ANGLE FOR WHICH STRUCTURE?
0° Endoscope:
├── Tympanic membrane (entire)
├── Umbo, cone of light
├── Handle of malleus
├── Anterior and posterior malleolar folds
├── Pars flaccida retraction
└── Incus (body) — through perforation
30° Endoscope:
├── Promontory
├── Round window niche
├── Stapedial arch
├── Incudo-stapedial joint
├── Oval window
└── Hypotympanic air cells
45° Endoscope:
├── Posterior mesotympanum
├── Sinus tympani (CRITICAL — MICROSCOPE BLIND SPOT)
├── Facial recess
└── Retrofacial cells
70° Endoscope:
├── Anterior epitympanum
├── Supratubal recess
├── Eustachian tube orifice
└── Tensor fold
The sinus tympani is the most clinically significant blind spot of the operative microscope. The 45° endoscope provides superior visualization and reduces cholesteatoma residual rates. (Tarabichi M, 2004; Scott-Brown 8th ed.)
COMPARISON: OTOENDOSCOPE vs. OPERATING MICROSCOPE
| Feature | Otoendoscope | Operating Microscope |
|---|---|---|
| Light source | Distal (at tip) | Proximal (coaxial) |
| Field of view | Wide angle (70–120°) | Narrow (< 40°) |
| Working distance | Short (6 cm) | Long (200–400 mm) |
| Depth of field | Deep | Shallow |
| Magnification | Fixed (×4–10) | Variable (×6–40) |
| Bimanual surgery | Difficult (scope in one hand) | Yes (both hands free) |
| Hidden recesses | Excellent (angled scopes) | Poor (line-of-sight only) |
| 3D perception | 2D (standard) | 3D (binocular) |
| Post-auricular incision | Often avoided | Usually needed |
| Learning curve | Steep initially | Established |
| Cost | High initial | Established |
| Sinus tympani view | Excellent | Poor |
| Patient recovery | Faster | Longer |
(Cummings Otolaryngology 7th ed.; Scott-Brown 8th ed.; Hazarika ENT 3rd ed.)
GRADING/CLASSIFICATION SYSTEMS USED IN OTOENDOSCOPY
A. Tympanic Membrane Perforation (Otoendoscopic Classification)
Rizer Classification (most used in RGUHS context):
- Type I: Small (< 25% of TM)
- Type II: Medium (25–50%)
- Type III: Large (50–75%)
- Type IV: Subtotal (> 75%, annulus intact)
- Type V: Total (annulus involved)
B. Cholesteatoma Staging (EAONO/JOS 2017)
STAGE I → Cholesteatoma in one middle ear compartment only
STAGE II → Cholesteatoma in > 1 compartment OR eroded ossicle
STAGE III → Extracranial complication (e.g., mastoid involvement)
STAGE IV → Intracranial complication
(European Academy of Otology & Neurotology; Scott-Brown 8th ed.)
C. Sinus Tympani Classification (Marchioni et al.)
- Type A: Small — below facial ridge
- Type B: Medium — at level of facial ridge
- Type C: Large — extends above facial ridge
OTOENDOSCOPIC FINDINGS IN COMMON DISORDERS
1. Normal Tympanic Membrane
- Pearly gray, translucent
- Cone of light: antero-inferior (5 o'clock right ear, 7 o'clock left)
- Lateral process of malleus: anterosuperior
- Umbo at center
2. Acute Otitis Media (AOM)
- Hyperemic, bulging TM
- Loss of landmarks
- Yellowish fluid (pus) behind TM
- Perforation may be present (seen endoscopically)
3. Otitis Media with Effusion (OME/Glue Ear)
- Amber/yellowish or blue discoloration behind TM
- Air-fluid levels or bubbles visible
- Retracted TM with prominent malleus handle
4. CSOM — Tubotympanic (Safe) Type
- Central perforation (pars tensa)
- Mucosal discharge through perforation
- Variable: polyp, granulation, tympanosclerosis visible
- Ossicles: usually intact or partially eroded
5. CSOM — Atticoantral (Unsafe) / Cholesteatoma
- Pars flaccida retraction pocket (early)
- Keratin debris (white, pearly) in attic
- Posterior-superior marginal perforation
- Ossicular erosion (incus most common)
- Foul-smelling discharge
- Endoscopy reveals extent in sinus tympani, posterior mesotympanum
6. Otosclerosis
- Schwartze sign: Flamingo pink blush through TM (active otospongiosis)
- Carhart notch on audiogram
- Otoendoscopy pre-stapedotomy: assess stapes mobility, footplate
7. Glomus Tympanicum
- Brown's sign: pulsatile red/brown mass behind TM, blanches with pneumatic otoscopy
- Otoendoscopy defines margins, relationship to ossicles
(Dhingra 7th ed.; Zakir Hussain ENT; Hazarika ENT 3rd ed.)
TRANSCANAL ENDOSCOPIC EAR SURGERY (TEES) — DETAILED
Flowchart 4: TEES vs. Traditional Microsurgery Decision Algorithm
PATIENT WITH MIDDLE EAR PATHOLOGY
↓
HRCT Temporal Bone
↓
┌───────────────────────────────────────────────┐
│ Is mastoid involved? │
└───────────────────────────────────────────────┘
YES ↙ ↘ NO
↓ ↓
Combined approach: TEES approach possible
Endoscope-assisted ↓
mastoidectomy EAC adequate diameter?
↓
YES → TEES preferred
NO → Canaloplasty first
then TEES
Specific TEES Procedures
A. Endoscopic Myringoplasty (Type I Tympanoplasty)
- Graft materials: Temporalis fascia (gold standard), tragal cartilage (perichondrium), fat graft
- Techniques:
- Underlay technique — graft placed medial to TM remnant (most common)
- Overlay technique — graft placed lateral to annulus
- Inlay (butterfly) technique — for small perforations, no flap needed
- Endoscopic advantage: visualization of anterior recess without meatal widening
B. Endoscopic Stapedotomy
- 0° endoscope for initial exposure
- 30° scope to visualize footplate fully
- Techniques: Laser (KTP/CO₂) or manual perforation with microdrill
- No post-auricular incision needed
- Advantages: better visualization of posterior crus, facial nerve, oval window niche
C. Endoscopic Cholesteatoma Surgery
- TEES for limited cholesteatoma (Stage I–II without mastoid involvement)
- 45° scope for sinus tympani dissection — reduces residual rate
- Residual cholesteatoma rate endoscopic: ~7% vs. microscopic: ~20–30% (Marchioni 2011)
- Second-look endoscopy: 6–12 months postoperatively
(Cummings 7th ed.; Scott-Brown 8th ed.; Tarabichi et al. TEES Atlas)
ADVANTAGES OF OTOENDOSCOPY
Over Operating Microscope:
- Wide-angle panoramic view — reveals hidden recesses impossible to see with microscope
- Distal illumination — coaxial bright light at the surgical site
- Avoids post-auricular incision — less morbidity, faster recovery, no scar
- Visualizes sinus tympani — reduces cholesteatoma recurrence
- Minimal disruption of EAC skin and meatus
- Shorter operative time for simple procedures
- Better documentation — high-definition video for medicolegal purposes and teaching
- Office-based procedures — under local anesthesia
- Telemedicine compatible — findings easily transmitted
- Cost-effective follow-up — endoscope vs. bringing patient to OT
(Hazarika P, ENT 3rd ed.; Dhingra 7th ed.; Zakir Hussain)
LIMITATIONS AND DISADVANTAGES
- One-handed surgery — endoscope occupies dominant hand; limits bimanual dissection
- 2D image — no stereoscopic depth perception (standard scopes)
- Fogging — scope tip fogs with warm air/blood; requires anti-fog solutions
- Thermal injury — prolonged endoscope contact with tissues (less with LED)
- Steep learning curve — requires dedicated training
- Limited working space — narrow EAC, especially in children
- Suction-irrigation conflicts — maintaining clear field challenging
- Mastoid disease — cannot address via pure TEES; needs combined approach
- Hemorrhage control — more difficult with one hand
- Cost — full HD/4K setup expensive; not universally available
(Scott-Brown 8th ed.; Cummings 7th ed.; Stell & Maran 5th ed.)
COMPLICATIONS OF OTOENDOSCOPY
Intraoperative
| Complication | Cause | Prevention |
|---|---|---|
| EAC laceration | Forceful insertion | Gentle technique, correct size |
| TM perforation | Inadvertent contact | Avoid excess pressure |
| Ossicular disruption | Excessive manipulation | Meticulous dissection |
| Facial nerve injury | Poor orientation | HRCT review, nerve monitoring |
| CSF leak | Tegmen breach | HRCT, careful drilling |
| Sensorineural hearing loss | Noise/suction trauma | Gentle technique |
| Thermal injury | Prolonged endoscope contact | Intermittent withdrawal, LED source |
Postoperative
- Graft failure / reperforation
- Residual / recurrent cholesteatoma
- Postoperative otitis externa
- Conductive hearing loss (ossicular fixation)
- Tympanosclerosis
(Dhingra 7th ed.; Hazarika ENT; Cummings 7th ed.)
OTOENDOSCOPY IN SPECIFIC CLINICAL SCENARIOS
A. Pediatric Otoendoscopy
- 2.7 mm, 0° scope preferred (small EAC)
- OME and grommet insertion: endoscopic myringotomy superior view
- Cholesteatoma: higher rate in children; TEES reduces revision rates
- General anesthesia required
B. Office Otoendoscopy
- Diagnostic examination under LA
- Cerumen removal
- Biopsy of EAC/middle ear lesions
- Pneumatic otoscopy with endoscope
- Eustachian tube balloon dilation (endoscope-guided)
C. Cochlear Implantation
- Endoscope used to verify round window membrane anatomy
- Insertion via round window approach or cochleostomy
- Intraoperative endoscopy: confirm electrode placement in scala tympani
- Reduces risk of cochlear trauma
D. Post-Stapedectomy
- Assessment of prosthesis position
- Perilymphatic fistula — endoscopic exploration and repair
- Obliterative otosclerosis — endoscope-guided footplate drilling
(Cummings 7th ed.; Scott-Brown 8th ed.)
RECENT ADVANCES IN OTOENDOSCOPY (2018–2025)
1. 4K Ultra-HD and 3D Endoscopes
- 4K resolution (3840×2160): superior tissue differentiation
- 3D endoscopes (stereoscopic): restore depth perception — addresses major limitation
- 3D exoscope (VITOM 3D): hands-free, bimanual surgery, 3D view, no scope in EAC
- Evidence: Meccariello et al. (2022) — 3D TEES reduces operative time, improved ergonomics
2. Robotic-Assisted Ear Surgery
- Robotic cochleostomy — submillimeter precision
- Robotics in stapedotomy — consistent piston placement
- RobOtol® system — first dedicated robotic ear surgery system (Paris, 2020)
- Challenges: cost, EAC size, learning curve
3. Artificial Intelligence in Otoendoscopy
- AI-based TM pathology recognition (deep learning CNN models)
- Automated classification: normal, AOM, OME, perforation, cholesteatoma
- Smartphone otoscope + AI: accuracy ~90% for AOM diagnosis (Byun et al. 2021)
- Decision support in telemedicine otology
4. Narrow Band Imaging (NBI) Endoscopy
- Enhances mucosal vascular patterns
- Distinguishes benign vs. malignant middle ear lesions
- Detects cholesteatoma matrix vs. granulation tissue
5. Fluorescence-Guided Otoendoscopy
- 5-ALA (aminolevulinic acid) fluorescence — cholesteatoma matrix fluoresces red under blue light
- Reduces residual cholesteatoma rates
- Preliminary evidence: Torizuka et al. (2023)
6. Balloon Eustachian Tuboplasty (BET) under Endoscopic Guidance
- Endoscope-guided balloon dilation of ET
- Indicated in chronic ET dysfunction, recurrent OME
- METRIST trial (UK, 2023): BET shows sustained benefit at 12 months
7. Endoscopic Endaural Approach (EEA)
- Extension of TEES when more mastoid access needed
- Avoids post-auricular scar entirely
- Marchioni's classification of endoscopic approaches
8. Laser Otoendoscopy
- Fiber-delivered diode/KTP laser through working channel
- Applications: stapedotomy, cholesteatoma matrix ablation, glomus tympanicum
- Non-contact ablation — reduces mechanical trauma
9. Portable/Smartphone Otoendoscopy
- Wi-Fi-enabled otoscopes (e.g., Wispr, CellScope)
- Smartphone attachment with otoscope tip
- Telemedicine triage and remote specialist consultation
- Particularly relevant in India (primary health care setting)
10. Endoscope-Assisted Cochlear Implant Surgery
- Endoscope verifies round window anatomy, electrode array position
- Reduces need for fluoroscopy radiation exposure
- Intraoperative endoscopy: detects fold-over or trauma
(Tarabichi M et al. — TEES Atlas 2018; Marchioni D et al. — Endoscopic Middle Ear Anatomy 2022; Scott-Brown 8th ed., Chapter 239)
OTOENDOSCOPY IN RGUHS EXAMINATION CONTEXT
Summary Flowchart 5: Otoendoscopy — Examination Approach
┌─────────────────────────────────────────────────────────────────┐
│ OTOENDOSCOPY — QUICK SUMMARY │
│ (RGUHS 50-Mark Structure) │
└─────────────────────────────────────────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ DEFINE → HISTORY → INSTRUMENTATION │
│ (2.7mm/4mm; 0°/30°/45°/70°; LED light source) │
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ ANATOMY → KEY LANDMARKS → BLIND SPOTS │
│ (Sinus tympani: microscope blind, endo sees all)│
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ INDICATIONS (Diagnostic + Surgical/TEES) │
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ TECHNIQUE (Step-by-step; angle selection) │
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ FINDINGS IN COMMON DISEASES │
│ (AOM, OME, CSOM safe/unsafe, Otosclerosis, │
│ Glomus, Cholesteatoma) │
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ ADVANTAGES vs MICROSCOPE │
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ LIMITATIONS + COMPLICATIONS │
└────────────────────┬────────────────────────────┘
↓
┌─────────────────────────────────────────────────┐
│ RECENT ADVANCES │
│ (4K, 3D, AI, Fluorescence, Robotic, BET, │
│ Smartphone otoendoscopy) │
└─────────────────────────────────────────────────┘
REFERENCES
| Source | Relevant Chapters |
|---|---|
| Scott-Brown's Otorhinolaryngology, HNS 8th ed. (2018) | Vol 3, Ch 221–239 — Otoendoscopy, TEES, Cholesteatoma |
| Cummings Otolaryngology: HNS 7th ed. (2021) | Ch 135–139 — Endoscopic ear surgery |
| Stell and Maran's HNS 5th ed. | Ch on Middle Ear and Mastoid Surgery |
| Zakir Hussain — ENT for Undergraduates 2nd ed. | Ear: Otoendoscopy, TEES |
| Dhingra PL — Diseases of ENT 7th ed. (2022) | Ear: Ch 6–7 |
| Hazarika P — ENT & Head Neck Surgery 3rd ed. | Ch on middle ear endoscopy |
| Bailey and Love's Surgery 28th ed. | Cholesteatoma, endoscopic guidance (p. 779) |
| Tarabichi M et al. — Transcanal Endoscopic Ear Surgery Atlas (2018) | Comprehensive TEES reference |
| Marchioni D et al. — Endoscopic Anatomy of the Middle Ear (2022) | Detailed anatomical reference |
| Meccariello et al. — 3D TEES (2022), JAMA Otolaryngol | Recent advance |
| EAONO/JOS — Cholesteatoma Staging (2017) | Classification |
| Byun et al. — AI otoscopy (2021), JAMA Pediatrics | Recent advance |
MARKS ALLOCATION GUIDE (RGUHS 50-Marks)
| Section | Expected Marks |
|---|---|
| Definition + History | 2 |
| Instrumentation (with diagram) | 8 |
| Anatomy and landmarks | 6 |
| Indications | 6 |
| Technique + Flowcharts | 8 |
| Otoendoscopic findings in diseases | 6 |
| Advantages vs. Microscope | 4 |
| TEES — Specific procedures | 4 |
| Complications | 3 |
| Recent advances | 8 |
| References | 1 |
| Total | 56 (write all for full 50) |
Examination tip for RGUHS: Always begin with a definition, include at least one diagram of the endoscope and one of the tympanic membrane landmarks, draw the angle-selection flowchart for different scopes, and end with recent advances including AI and 3D endoscopy. The sinus tympani as the "blind spot of the microscope, clearly seen by otoendoscope" is a high-yield examiner's favorite.
This is a shared conversation. Sign in to Orris to start your own chat.