i am having an exam on bone cartilage histology explain it to me
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
I now have all the content I need. Let me compile a comprehensive exam-ready guide.
Bone & Cartilage Histology — Exam Guide
Source: Histology: A Text and Atlas with Correlated Cell and Molecular Biology (Pawlina & Ross)
PART 1 — CARTILAGE
Overview
Cartilage is an avascular connective tissue composed of:
- Chondrocytes — the only cell type
- Extracellular matrix (ECM) — makes up >95% of cartilage volume
The ECM contains type II collagen fibrils (tension-resisting) + heavily hydrated proteoglycan aggregates (compression-bearing). This combination gives cartilage its characteristic resilience and pliability. Because it is avascular, nutrients diffuse from surrounding perichondrium through the matrix to reach the chondrocytes.
The 3 Types of Cartilage
| Feature | Hyaline | Elastic | Fibrocartilage |
|---|---|---|---|
| Dominant ECM | Type II collagen + proteoglycans | Type II collagen + elastic fibers/lamellae | Type I collagen (abundant) + minimal matrix |
| Perichondrium | Yes (except articular + growth plate) | Yes | No |
| Calcifies? | Yes (aging, endochondral ossification) | No | No |
| Locations | Articular surfaces, costal cartilages, tracheal rings, larynx, fetal skeleton, epiphyseal plate | Auricle of ear, epiglottis, Eustachian tube, vocal folds | IVD (annulus fibrosus), pubic symphysis, menisci, TMJ disc, sternal-clavicular joint |
| Function | Cushioning, smooth joint surface, structural support | Flexibility/elasticity | Resists compression and shearing |
| Stain for elastic | — | Orcein (elastic fibers stain brown) | — |
Hyaline Cartilage — Close-Up
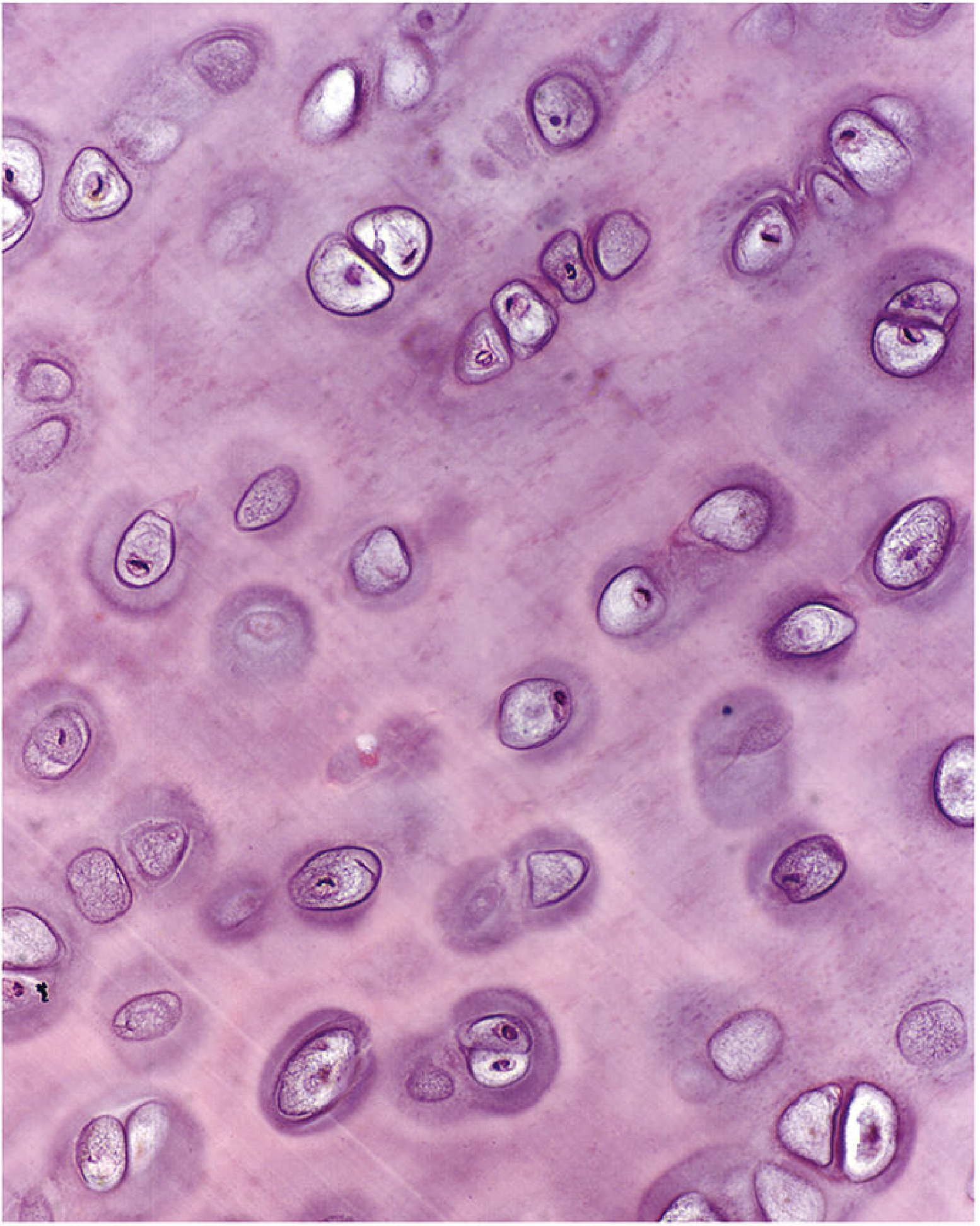
H&E ×450: Chondrocytes in lacunae dispersed within the extensive, lightly basophilic matrix. Pairs of chondrocytes = isogenous groups (daughter cells from mitotic division still sharing a lacuna).
Key cellular terms:
- Chondroblasts — active cells on the surface/perichondrium; secrete matrix
- Chondrocytes — mature cells within lacunae; maintain matrix
- Isogenous groups — clusters of 2–8 chondrocytes derived from one progenitor; a marker of interstitial growth
Matrix zones (from cell outward):
- Capsular (pericellular) matrix — immediately surrounds each chondrocyte; highest concentration of sulfated proteoglycans + type VI collagen; intensely basophilic/metachromatic
- Territorial matrix — surrounds the isogenous group; less intensely stained
- Interterritorial matrix — between groups; least stained; bulk of the matrix
Staining properties:
- Matrix stains basophilic with H&E (sulfated proteoglycans attract hematoxylin)
- Matrix stains metachromatic with toluidine blue (sulfated GAGs)
Elastic Cartilage
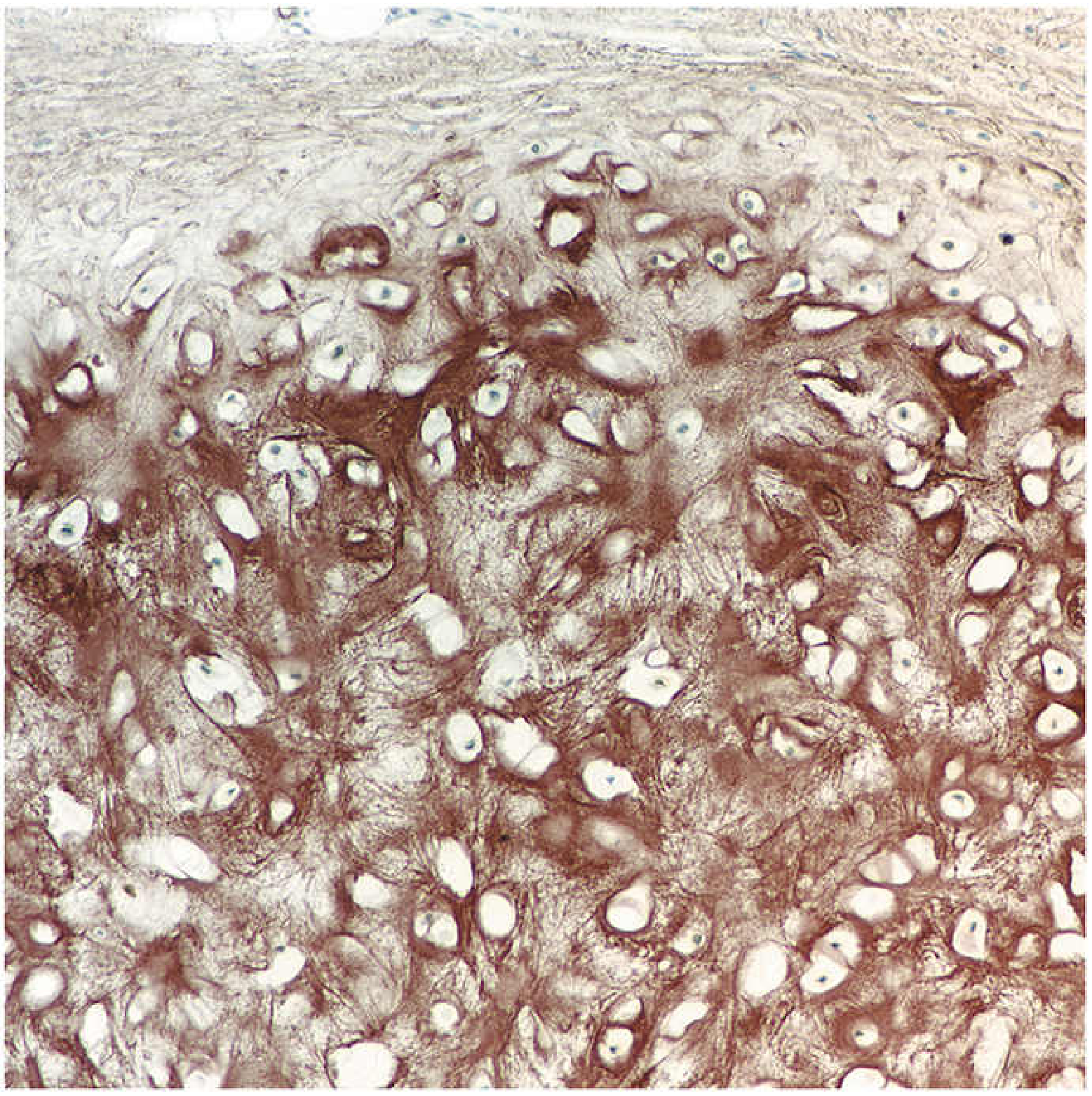
Orcein stain ×180: Dense network of brown elastic fibers among chondrocytes. Perichondrium visible at top.
Looks like hyaline cartilage on H&E but has abundant elastic fibers visible only with orcein or Weigert stains. Does not calcify with aging — clinically important distinction.
Fibrocartilage
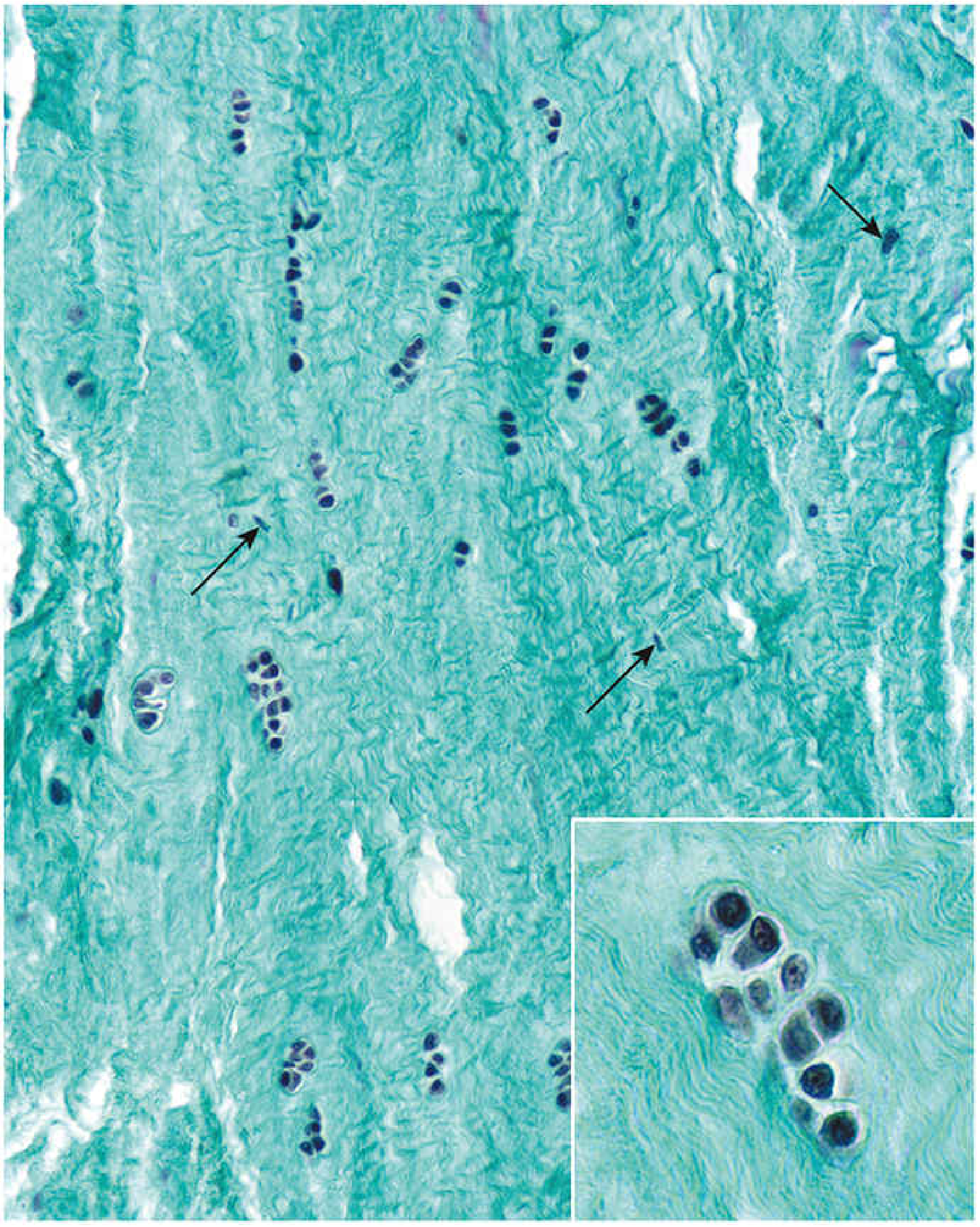
Gomori trichrome ×60: Dense green type I collagen bundles. Chondrocytes (round nuclei) arranged in rows and isogenous groups among fibroblasts (elongated, flattened nuclei). Inset shows an isogenous group at high magnification.
Key exam point: Fibrocartilage has no perichondrium, contains fibroblasts alongside chondrocytes, and its ECM is dominated by type I collagen (unlike other cartilage types).
Cartilage Growth
- Appositional growth — new chondrocytes arise from the inner chondrogenic layer of the perichondrium and add to the surface → increases width
- Interstitial growth — chondrocytes within the matrix divide mitotically → expands cartilage from within → seen as isogenous groups; occurs mainly during fetal/early life
Cartilage Repair
Hyaline cartilage has very limited repair capacity — avascular, chondrocytes cannot easily migrate. Damage typically heals as fibrocartilage scar.
PART 2 — BONE
General Classification
| Type | Description |
|---|---|
| Compact (cortical) | Dense outer shell; consists primarily of osteons (Haversian systems) |
| Spongy (cancellous) | Internal lattice of trabeculae; spaces filled with marrow |
| Woven (immature) | Developing bone; collagen fibers randomly oriented; temporary |
| Lamellar (mature) | Organized concentric lamellae; collagen fibers in alternating parallel arrays |
Bone Cells (Must Know All 4)
| Cell | Origin | Function | Key Feature |
|---|---|---|---|
| Osteoprogenitor | Mesenchymal stem cells (bone marrow) | Precursor; divides to replenish osteoblasts | Activated by CBFA1/RUNX2 transcription factor |
| Osteoblast | Osteoprogenitor cells | Secretes osteoid (unmineralized matrix); mineralization triggered by matrix vesicles | Cuboidal cells lining bone surface; abundant rER + Golgi |
| Osteocyte | Trapped osteoblasts | Maintain bone matrix; mechanosensing | Enclosed in lacunae; communicate via canaliculi (cell processes); network = canalicular system |
| Osteoclast | Hematopoietic progenitors (monocyte lineage) | Resorb bone | Large multinucleated cells; sit in Howship's lacunae (resorption pits); ruffled border faces bone |
RANK–RANKL pathway: Osteoblasts express RANKL → binds RANK on osteoclast precursors → osteoclast differentiation. PTH acts on osteoblasts (not osteoclasts directly) to upregulate RANKL. OPG (osteoprotegerin) from osteoblasts blocks RANKL → inhibits osteoclastogenesis.
Bone ECM (Osteoid)
- Organic (35%): ~90% type I collagen; non-collagenous proteins (osteocalcin, osteopontin, bone sialoprotein)
- Inorganic (65%): Hydroxyapatite — Ca₁₀(PO₄)₆(OH)₂ — deposited along collagen fibrils
The Osteon (Haversian System)
The structural unit of compact bone:
Central Haversian canal (blood vessels + nerves)
↑ surrounded by
Concentric lamellae (mineralized bone matrix in rings)
↑ between lamellae
Lacunae (osteocytes) → connected by → Canaliculi
↑ outer boundary
Cement line (marks boundary of one osteon)
- Volkmann (perforating) canals — run perpendicular to the long axis; connect Haversian canals to each other and to the periosteum/endosteum
- Interstitial lamellae — remnants of old, remodeled osteons between current osteons
- Circumferential lamellae — outer and inner rings of lamellar bone just beneath periosteum/endosteum
Ground section ×80: Circular osteons with central Haversian canals (dark = air or India ink). Interstitial lamellae fill spaces between osteons. Circumferential lamellae visible at periphery.
Bone Formation — Two Methods
1. Intramembranous Ossification
- No cartilage precursor — bone forms directly in mesenchyme
- Bones formed: Flat bones of skull, mandible, clavicle
- Sequence: mesenchymal condensation → osteoprogenitors → osteoblasts secrete osteoid → mineralization → woven bone → remodeled to lamellar bone
2. Endochondral Ossification
- Uses a hyaline cartilage model as scaffold
- Most bones in the body form this way

Fetal digit H&E ×210: Epiphyses (E) = cartilage. Hypertrophic chondrocytes (HC) in center. Calcified cartilage matrix (CCM) darker staining. Periosteal bony collar (BC) forming around shaft.
Stages:
- Cartilage model forms (hyaline)
- Chondrocytes at center hypertrophy → matrix calcifies
- Periosteal bony collar forms around diaphysis (via intramembranous ossification of periosteum)
- Blood vessels invade → primary ossification center in diaphysis
- Secondary ossification centers form in epiphyses later (most postnatal)
- Epiphyseal growth plate (physis) persists between primary and secondary centers until skeletal maturity
Epiphyseal Growth Plate — Zones (Proximal → Distal)
| Zone | What's Happening | Key H&E Feature |
|---|---|---|
| Reserve (resting) zone | Small chondrocytes, storing lipid/glycogen | Cells scattered, matrix pale |
| Proliferative zone | Rapid mitosis → columns (stacks) of flat chondrocytes | Columns ("coins stacked") = interstitial growth |
| Hypertrophic zone | Cells enlarge; matrix calcification begins | Large clear cytoplasm |
| Calcified cartilage zone | Chondrocytes die; matrix mineralized | Dark-staining matrix |
| Resorption (ossification) zone | Osteoclasts resorb cartilage; osteoblasts lay down bone | Bone trabeculae on calcified cartilage spicules |
Mnemonic: "Really Pretty Healthy Children" → Reserve, Proliferative, Hypertrophic, Calcified
Periosteum & Endosteum
| Periosteum | Endosteum | |
|---|---|---|
| Location | Outer surface of bone | Inner surface (marrow cavity, trabeculae, canals) |
| Layers | Outer fibrous + inner osteogenic (cambium) layer | Single layer of osteoprogenitors + osteoblasts |
| Function | Appositional growth, fracture repair | Remodeling, fracture repair |
Bone Remodeling & Calcium Regulation
- BMU (bone remodeling unit): Coupled osteoclasts + osteoblasts working together
- PTH: ↑ osteoclast activity (via RANKL on osteoblasts) → bone resorption → ↑ blood Ca²⁺
- Calcitonin: Inhibits osteoclasts → ↓ bone resorption → ↓ blood Ca²⁺
- Vitamin D (1,25-OH₂D₃ / calcitriol): ↑ Ca²⁺ absorption from gut + ↑ renal reabsorption
Fracture Repair (Secondary / Indirect)
- Hematoma formation
- Periosteal cells activated → form soft callus (fibrocartilage)
- Soft callus replaced by hard (bony) callus via endochondral ossification
- Callus remodeled to lamellar bone
Quick High-Yield Summary Table
| Feature | Cartilage | Bone |
|---|---|---|
| Vascularity | Avascular | Vascular (Haversian + Volkmann canals) |
| Main collagen | Type II (hyaline/elastic), Type I (fibrocartilage) | Type I |
| Cell in matrix | Chondrocyte (in lacuna) | Osteocyte (in lacuna + canaliculi) |
| Nutrition | Diffusion through matrix | Canalicular system + blood vessels |
| Mineralization | Hyaline only (aging/ossification) | Always — hydroxyapatite |
| Repair capacity | Very limited → fibrocartilage scar | Good — callus formation |
| Growth | Interstitial + appositional | Appositional only (adult) |
Source: Histology: A Text and Atlas with Correlated Cell and Molecular Biology, 9th ed. (Pawlina & Ross)
This is a shared conversation. Sign in to Orris to start your own chat.