angina pectoralis
Reading File
search_medical_text
angina pectoris pathophysiology classification stable unstable diagnosis management
search_medical_image
angina pectoris ECG coronary artery disease ischemia
GradeResponse
GradeResponse
Angina Pectoris
Angina pectoris is chest pain or discomfort resulting from myocardial ischemia — an imbalance between myocardial oxygen supply and demand — most commonly due to obstructive coronary artery disease (CAD).
Pathophysiology
The fundamental mechanism is myocardial ischemia: coronary blood flow is insufficient to meet the metabolic demands of the myocardium. This occurs via:
- Fixed coronary stenosis (atherosclerotic plaque): limits maximal perfusion, causing exertional symptoms
- Dynamic obstruction: vasospasm superimposed on plaque (variant/Prinzmetal angina) or at sites of endothelial dysfunction
- Plaque rupture/erosion: triggers thrombus formation, precipitating unstable angina or ACS
- Microvascular dysfunction: impaired coronary microcirculation (angina with no obstructive CAD — ANOCA)
When ischemia occurs, anaerobic metabolism generates lactate and adenosine, stimulating cardiac nociceptors → pain referred to chest, jaw, arm, or epigastrium.
Classification
| Type | Key Features |
|---|---|
| Stable angina | Predictable, exertion- or stress-induced; relieved by rest or nitroglycerin within minutes; fixed-threshold |
| Unstable angina (UA) | New-onset, accelerating, or rest angina; part of ACS spectrum; no troponin rise (unlike NSTEMI) |
| Variant (Prinzmetal) angina | Coronary vasospasm; often at rest, nocturnal; ST elevation during episodes |
| Microvascular angina | Chest pain with ischemic features but no obstructive epicardial CAD; more common in women |
| Silent ischemia | ECG/imaging evidence of ischemia without symptoms; common in diabetics |
Canadian Cardiovascular Society (CCS) Classification for Stable Angina:
| Class | Description |
|---|---|
| I | Angina only with strenuous exertion; ordinary activity does not cause angina |
| II | Slight limitation of ordinary activity (e.g., walking >2 blocks, climbing >1 flight of stairs) |
| III | Marked limitation of ordinary activity |
| IV | Inability to perform any activity without discomfort; angina at rest |
Clinical Presentation
Classic features (Harrison's, p. 530):
- Onset: gradual, reaching maximal intensity over minutes
- Character: pressure, heaviness, squeezing, tightness (rarely described as "sharp")
- Location: retrosternal; may radiate to left arm, jaw, neck, shoulder, epigastrium
- Duration: typically 2–10 minutes for stable angina; ≥30 minutes suggests MI
- Relief: rest and/or sublingual nitroglycerin within minutes (stable angina); poor response in UA/MI
Atypical presentations (more common in women, elderly, diabetics): dyspnea, fatigue, nausea, diaphoresis — sometimes without chest pain ("anginal equivalent").
ECG and Imaging Correlation
The image below illustrates the classic correlation between ischemic ECG changes and coronary anatomy:
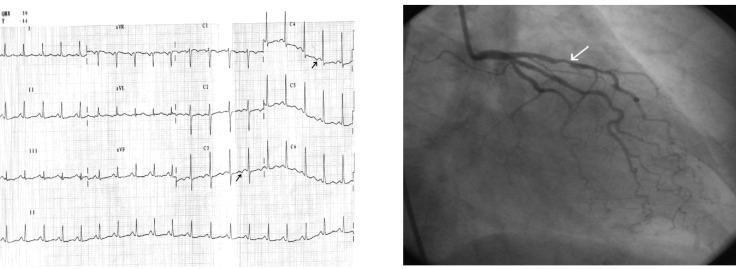
Diagnosis
History & Physical
- Characterize chest pain (onset, character, radiation, duration, relieving/aggravating factors)
- Assess cardiovascular risk factors: HTN, DM, dyslipidemia, smoking, family history, obesity
Investigations
| Test | Role |
|---|---|
| Resting ECG | May show ST depression, T-wave changes, Q waves; often normal between episodes |
| Exercise stress test (EST) | First-line functional test for stable angina; ST depression ≥1 mm at peak exertion is significant |
| Stress echocardiography | Detects wall motion abnormalities during stress; higher sensitivity/specificity than EST |
| Nuclear imaging (MPS) | Perfusion defects identify ischemic territories; good for risk stratification |
| CT coronary angiography (CTCA) | Non-invasive anatomical assessment; high NPV; preferred in intermediate pre-test probability |
| Invasive coronary angiography | Gold standard for coronary anatomy; required before revascularization |
| Troponin (hs-cTn) | Elevated in UA → NSTEMI transition; normal in stable angina |
| CBC, lipids, fasting glucose, HbA1c, TFTs | Identify contributory conditions and risk factors |
Management
Acute Relief
- Sublingual nitroglycerin (0.4 mg SL q5 min × 3 doses): first-line for acute episodes
- If no relief after 3 doses → call emergency services (possible ACS)
Antianginal Therapy (Chronic Stable Angina)
| Drug Class | Examples | Mechanism |
|---|---|---|
| Beta-blockers (first-line) | Metoprolol, atenolol, bisoprolol | ↓ HR, ↓ contractility → ↓ O₂ demand |
| Calcium channel blockers | Amlodipine, diltiazem, verapamil | Vasodilation + ↓ HR (non-DHP) |
| Long-acting nitrates | Isosorbide mononitrate | Venodilation → ↓ preload; tolerance requires nitrate-free interval |
| Ranolazine | Ranolazine | Inhibits late INa; ↓ ischemia without hemodynamic effects |
| Ivabradine | Ivabradine | Sinus node If channel inhibitor; ↓ HR in sinus rhythm |
Secondary Prevention (All Patients with CAD)
| Intervention | Drug/Target |
|---|---|
| Antiplatelet | Aspirin 75–100 mg/day (lifelong); add P2Y12 inhibitor post-ACS/PCI |
| Statin (high-intensity) | Atorvastatin 40–80 mg; target LDL <1.4 mmol/L (<55 mg/dL) per ESC 2021 |
| ACE inhibitor/ARB | Especially if HFrEF, HTN, or DM |
| BP control | Target <130/80 mmHg |
| Lifestyle | Smoking cessation, Mediterranean diet, exercise, weight management |
Revascularization
- PCI (percutaneous coronary intervention): preferred for single/two-vessel disease; symptom relief; drug-eluting stents
- CABG (coronary artery bypass grafting): preferred for left main disease, three-vessel disease (especially with reduced EF or diabetes), complex anatomy
- Decision guided by: SYNTAX score, anatomy, LV function, comorbidities, patient preference
Differentiation: Stable vs. Unstable Angina vs. NSTEMI
| Feature | Stable Angina | Unstable Angina | NSTEMI |
|---|---|---|---|
| Trigger | Exertion/stress | Rest or minimal exertion | Rest |
| Duration | <10 min | Variable | ≥30 min |
| Troponin | Normal | Normal | Elevated |
| ECG | Normal or T-wave changes | ST depression, T-wave changes | ST depression, T-wave changes |
| Treatment | Medical ± elective PCI | Hospitalize, anticoagulate, urgent angiography | Hospitalize, anticoagulate, urgent angiography |
Prognosis
Annual mortality in stable angina with medical therapy is approximately 1–3%. Risk stratification using stress imaging and coronary anatomy determines whether revascularization improves outcomes beyond symptom control. Key adverse predictors: reduced LVEF, three-vessel/left main disease, large ischemic burden, and recurrent ACS.
This is a shared conversation. Sign in to Orris to start your own chat.