Dengue
Reading File
search_medical_text
dengue fever etiology pathophysiology epidemiology
search_medical_text
dengue clinical features diagnosis classification warning signs
search_medical_image
dengue rash clinical presentation
GradeResponse
GradeResponse
GradeResponse
search_medical_text
dengue management treatment fluid therapy severe dengue
Dengue Fever
Etiology & Epidemiology
Dengue is caused by Orthoflavivirus dengue (serotypes 1–4), a member of the family Flaviviridae. It is transmitted primarily by the Aedes aegypti mosquito (and to a lesser extent Ae. albopictus). Dengue is endemic in tropical and subtropical regions, with an estimated 100–400 million infections annually worldwide. Second infection with a heterologous serotype carries a significantly higher risk of severe disease due to antibody-dependent enhancement (ADE).
Phases of Illness
| Phase | Timing | Key Features |
|---|---|---|
| Febrile | Days 1–3 | Abrupt high fever (39–40°C), severe myalgia/arthralgia ("breakbone fever"), retro-orbital headache, facial flushing, early rash |
| Critical | Days 4–6 (around defervescence) | Increased capillary permeability, plasma leakage, warning signs, risk of severe dengue |
| Recovery | Days 7–10 | Reabsorption of leaked fluids, improvement, secondary "convalescent" rash |
Clinical Classification (WHO 2009)
1. Dengue without warning signs
- Fever + 2 of: nausea/vomiting, rash, aches and pains, positive tourniquet test, leukopenia
2. Dengue with warning signs (requires close monitoring/hospitalization)
- Abdominal pain — progressive, continuous, or sustained and intense (especially at end of febrile stage)
- Mucosal bleeding — gums, epistaxis, vaginal bleeding, hematuria
- Hepatomegaly > 2 cm below costal margin
- Sensory changes — irritability, drowsiness, lethargy
- Rapid clinical deterioration
- Persistent vomiting
- Clinical fluid accumulation (ascites, pleural effusion)
- Rising hematocrit concurrent with rapid platelet drop
3. Severe dengue
- Severe plasma leakage → shock (dengue shock syndrome) or fluid accumulation with respiratory distress
- Severe bleeding
- Severe organ involvement (liver, CNS, heart, kidneys)
(Clinical Management of Arboviral Diseases: Dengue, Chikungunya, Zika and Yellow Fever, p. 27)
Rash
The characteristic dengue rash typically appears 3–6 days after fever onset:
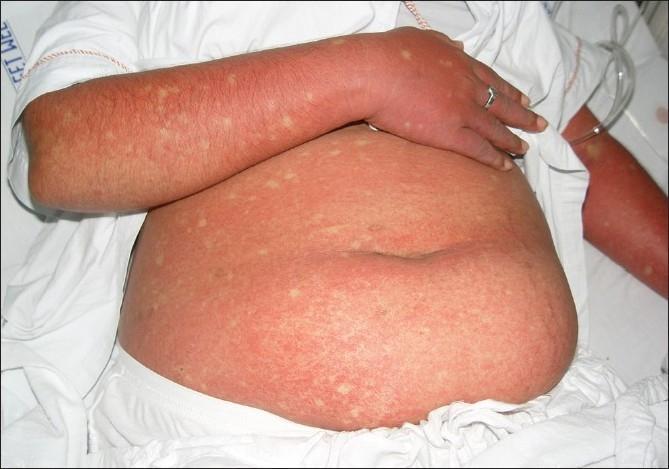
"White islands in a sea of red" — coalesced maculopapular erythema with scattered patches of normal skin. This pattern helps differentiate dengue from other viral exanthems.
Diagnosis
| Test | Details |
|---|---|
| NS1 antigen | Positive days 1–5 (febrile phase); high sensitivity early |
| IgM/IgG serology | IgM rises from day 5; IgG indicates prior infection |
| RT-PCR | Gold standard in first 5 days; identifies serotype |
| CBC | Leukopenia, thrombocytopenia, rising hematocrit (marker of plasma leakage) |
| Tourniquet test | ≥10 petechiae/inch² = positive; useful in resource-limited settings |
Management
Dengue without warning signs (Outpatient)
- Oral hydration — encourage fluids (water, ORS, juices)
- Antipyretics — paracetamol only (NSAIDs and aspirin are contraindicated — risk of bleeding and Reye syndrome)
- Daily monitoring of CBC
- Education on warning signs — return immediately if they develop
Dengue with warning signs (Inpatient)
- IV fluid resuscitation with isotonic crystalloids (0.9% NaCl or Ringer's lactate)
- Careful fluid titration — avoid over-hydration (risk of pulmonary edema during recovery phase)
- Serial hematocrit monitoring every 4–6 hours
- Platelet transfusion only for active significant bleeding with severe thrombocytopenia (not prophylactically)
Severe Dengue (ICU-level care)
- Aggressive but judicious fluid resuscitation
- Colloids (e.g., dextran 70) for refractory shock
- Blood transfusion for significant hemorrhage
- Organ-specific supportive care (ventilation, renal support)
Complications
- Dengue shock syndrome (DSS) — plasma leakage → circulatory failure
- Dengue hemorrhagic fever (DHF) — thrombocytopenia + hemorrhagic manifestations
- Hepatitis, myocarditis, encephalitis (rare but recognized)
- Fluid overload from excessive IV fluids (iatrogenic)
Prevention
- Vaccine: Dengvaxia (CYD-TDV) — approved in seropositive individuals ≥9 years; risk of severe dengue in seronegative recipients means pre-vaccination serology testing is essential
- Vector control: Eliminate standing water, use insect repellents (DEET), wear protective clothing
- No specific antiviral therapy exists
(Clinical Management of Arboviral Diseases: Dengue, Chikungunya, Zika and Yellow Fever, pp. 20, 27)
This is a shared conversation. Sign in to Orris to start your own chat.