8 year boy sustained a fall on outstreached hand and sustained injury near right elbow presenting with pain, swelling and S shaped deformity near elbow a. What is best probable clinical diagnosis b. What are differential diagnosis c. Investigations d. Treatment options for the child
Reading File
search_medical_text
supracondylar fracture humerus child S-shaped deformity diagnosis classification
search_medical_text
supracondylar fracture humerus child treatment options CRPP surgical management
search_medical_image
supracondylar fracture humerus child X-ray
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive clinical answer:
Pediatric Elbow Injury: 8-Year-Old Male, Fall on Outstretched Hand (FOOSH)
a. Best Probable Clinical Diagnosis
Supracondylar Fracture of the Humerus (Extension Type)
This is the most common elbow fracture in children (50–70% of all pediatric elbow fractures), with a peak incidence between 5–8 years of age. The mechanism — fall on outstretched hand (FOOSH) with the elbow hyperextended — is the classic presentation of the extension type (accounts for ~97% of supracondylar fractures).
The "S-shaped" or "reverse S-shaped" deformity at the elbow is pathognomonic, resulting from:
- Posterior displacement of the distal fragment
- The proximal fragment tent-ing through the brachialis muscle anteriorly
- This gives the appearance similar to a "S" when viewed from the side
(Bailey and Love's Short Practice of Surgery, 28th Ed., p. 461)
b. Differential Diagnoses
| Condition | Distinguishing Features |
|---|---|
| Lateral condyle fracture | Lateral swelling, intra-articular, Milch classification; more common in 5–10 yr |
| Medial epicondyle avulsion | Medial tenderness, associated with elbow dislocation, valgus stress |
| Elbow dislocation (posterior) | Complete loss of normal bony landmarks; olecranon displaced posteriorly |
| Radial neck fracture | Lateral elbow pain, restricted pronation/supination, tenderness over radial head |
| Fracture-separation of distal humeral physis | Seen in neonates/infants; may mimic dislocation on X-ray; widened physis |
| Lateral condyle physis fracture (Salter-Harris IV) | Intra-articular, risk of non-union/AVN; requires anatomic reduction |
| Nursemaid's elbow (Radial head subluxation) | Younger children (<5 yr), pulled elbow, no bony injury on X-ray |
| Simple soft tissue injury / haematoma | No fracture line; however, always X-ray given mechanism |
c. Investigations
Imaging
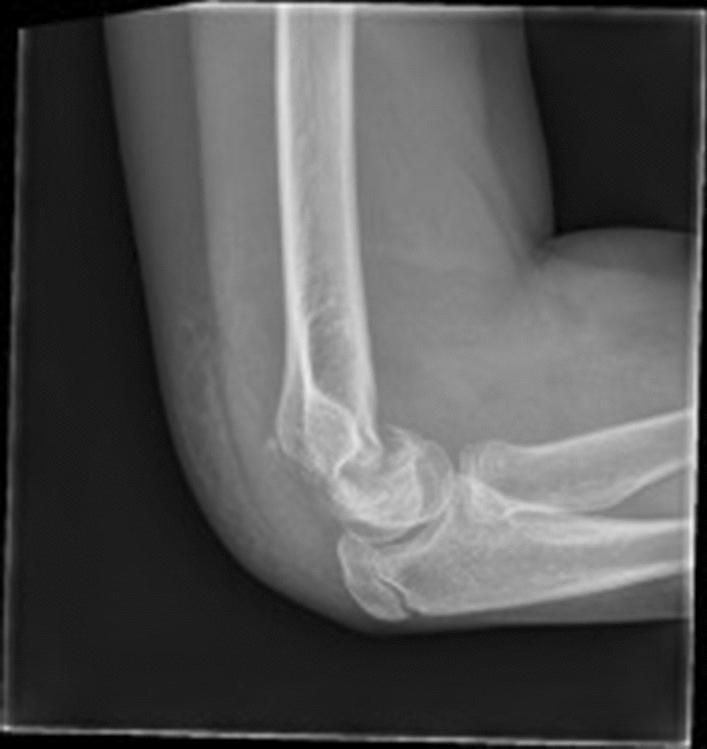
1. X-Ray Elbow — AP and True Lateral (first-line)
- Look for fracture line in the supracondylar region
- Assess displacement (posterior/anterior/lateral)
Key radiological signs:
- Anterior Humeral Line (AHL): A line drawn along the anterior cortex of the humerus on lateral view should pass through the middle third of the capitellum. In extension-type supracondylar fractures, it passes anterior to or the anterior third of the capitellum.
- Posterior fat pad sign ("sail sign"): Effusion lifting the posterior fat pad — indicative of intra-articular fracture even when fracture line is subtle.
- Anterior fat pad elevation (visible normally, but large = abnormal)
- Baumann's angle on AP view (normal 70–75°) — used to assess varus/valgus alignment
2. Contralateral elbow X-ray — for comparison of growth plates if diagnosis uncertain
3. CT scan — not routine; reserved for complex intra-articular fractures or to assess rotation in cases where operative planning is complex
4. MRI — rarely needed; useful if growth plate injury or soft tissue injury suspected and X-rays inconclusive
Neurovascular Assessment (Critical — not just imaging)
- Anterior interosseous nerve (AIN) — most commonly injured nerve; test by "OK sign" (flexion of thumb IP and index finger DIP)
- Radial nerve (posterolateral displacement)
- Median nerve / ulnar nerve
- Brachial artery — check radial pulse, capillary refill; pink pulseless hand is a vascular emergency
d. Treatment Options
Treatment is guided by the Gartland Classification:
| Gartland Grade | Description | Treatment |
|---|---|---|
| Type I | Undisplaced | Conservative |
| Type II | Displaced, posterior cortex intact (hinge intact) | Conservative or percutaneous pinning |
| Type IIb | Type II + rotational malalignment | Percutaneous pinning |
| Type III | Completely displaced, no cortical contact | CRPP or ORIF |
| Type IV (Wilkins) | Multidirectional instability | CRPP/ORIF |
1. Conservative (Type I, selected Type II)
- Collar and cuff / above-elbow backslab with elbow in 90° flexion and forearm in neutral/pronation
- Duration: 3 weeks, followed by progressive mobilisation
- Avoid circumferential cast in acute phase (swelling risk)
- (Bailey and Love's, p. 461)
2. Closed Reduction + Percutaneous K-wire Pinning (CRPP) — Gold Standard for Type II-III
- Performed under general anaesthesia
- Reduction manoeuvre: traction → correction of medial/lateral displacement → flexion
- Two or three lateral K-wires (avoids ulnar nerve injury compared to medial pin)
- Cross-pin configuration provides rotational stability
- Post-op: above-elbow backslab for 3–4 weeks, then wire removal
- Most preferred operative technique globally for displaced supracondylar fractures in children
3. Open Reduction + Internal Fixation (ORIF)
- Indicated when:
- Closed reduction fails (soft tissue interposition)
- Vascular injury requiring brachial artery exploration
- Open fractures
- Irreducible fractures
- Approaches: anterior (Henry), lateral, or medial depending on neurovascular status
4. Traction (Historical / Rarely Used)
- Dunlop's skin traction or overhead skeletal traction
- Reserved for settings where operative resources are unavailable
- Prolonged hospital stay; largely replaced by CRPP
5. Vascular Emergency Protocol
If pulseless pink hand → urgent CRPP; if pulse doesn't return post-reduction → brachial artery exploration
If pulseless white (ischaemic) hand → immediate surgical exploration
Key Complications to Monitor
| Complication | Notes |
|---|---|
| Volkmann's ischaemic contracture | Most feared; due to compartment syndrome from brachial artery injury |
| Cubitus varus ("gunstock deformity") | Most common late complication; cosmetic, due to malunion |
| Nerve injury | AIN most common (usually neurapraxia, resolves in 3 months) |
| Myositis ossificans | Risk increased with aggressive physiotherapy too early |
| Avascular necrosis of trochlea | Rare |
Summary: This presentation is a Gartland Type III supracondylar fracture of the humerus until proven otherwise. Immediate neurovascular assessment is mandatory. Most cases require CRPP under GA as definitive treatment. Early recognition and prompt management prevent devastating complications like Volkmann's contracture.
This is a shared conversation. Sign in to Orris to start your own chat.