IS THERE ANY SPECIFIC DIAGNOSTIC TESTS FOR Pulmonary embolism
Reading File
search_medical_text
pulmonary embolism diagnostic tests Wells score D-dimer CT pulmonary angiography
search_medical_image
pulmonary embolism CT scan CTPA imaging findings diagnosis
GradeResponse
GradeResponse
Here is a comprehensive overview of the specific diagnostic tests for Pulmonary Embolism (PE):
Diagnostic Tests for Pulmonary Embolism
Diagnosis of PE follows a structured, stepwise approach starting with clinical probability assessment, followed by laboratory and imaging studies.
Step 1: Pre-Test Probability Assessment
Wells Score for PE
The Wells Criteria stratifies patients into Low, Intermediate, or High probability before ordering any tests:
| Clinical Feature | Points |
|---|---|
| Clinical signs/symptoms of DVT | +3 |
| PE is #1 diagnosis OR equally likely | +3 |
| Heart rate > 100 bpm | +1.5 |
| Immobilization ≥ 3 days OR surgery in past 4 weeks | +1.5 |
| Previous DVT or PE | +1.5 |
| Hemoptysis | +1 |
| Malignancy (on treatment or in past 6 months) | +1 |
Interpretation:
- ≤ 4 points → Low/Intermediate probability
-
4 points → High probability
PERC Rule (Pulmonary Embolism Rule-Out Criteria)
Used in low-probability patients. If ALL 8 criteria are negative, PE can be excluded without further testing:
- Age < 50, HR < 100, SpO₂ ≥ 95%, no unilateral leg swelling, no hemoptysis, no recent surgery/trauma, no prior DVT/PE, no exogenous estrogen use.
Step 2: Laboratory Tests
1. D-Dimer
- Most important initial lab test for low/intermediate pre-test probability patients.
- A negative high-sensitivity D-dimer effectively rules out PE (NPV ~97–99%).
- Not useful in high-probability patients — proceed directly to imaging.
- Age-adjusted D-dimer threshold: age × 10 µg/L (in patients > 50 years) improves specificity.
According to the "Evaluation of Patients With Suspected Acute Pulmonary Embolism" guidelines (p. 8): "Clinicians should obtain a high-sensitivity D-dimer measurement as the initial diagnostic test in patients who have an intermediate pretest probability of PE or in patients with low pretest probability who do not meet all PERC criteria. Clinicians should NOT use imaging studies as the initial test in patients with low or intermediate pretest probability."
2. Arterial Blood Gas (ABG)
- May show hypoxemia, hypocapnia, and respiratory alkalosis.
- Non-specific; not diagnostic on its own.
3. Troponin (I or T) & BNP/NT-proBNP
- Markers of right ventricular (RV) strain and myocardial injury.
- Elevated in massive/submassive PE — used for risk stratification, not diagnosis.
Step 3: Imaging Studies
1. CT Pulmonary Angiography (CTPA) — Gold Standard
- Test of choice for PE diagnosis when imaging is indicated.
- Directly visualizes thrombus as a hypodense filling defect within pulmonary arteries.
- Highly sensitive (~83%) and specific (~96%).
- Can diagnose alternative conditions (pneumonia, aortic dissection, etc.).
Below is a classic CTPA demonstrating a saddle embolus at the bifurcation of the main pulmonary artery:
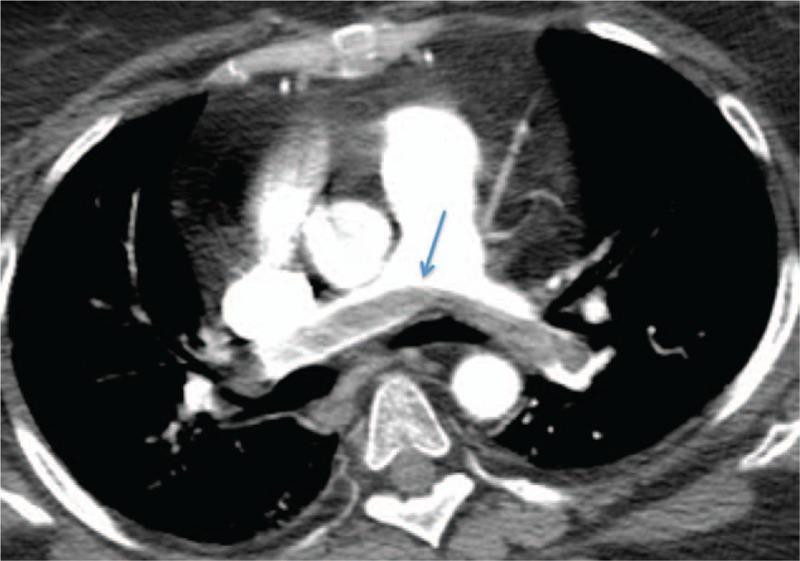
2. Ventilation-Perfusion (V/Q) Scan
- Used when CTPA is contraindicated (renal failure, contrast allergy, pregnancy).
- Results reported as: normal (rules out PE), low/intermediate probability, or high probability.
- A high-probability V/Q scan with high clinical suspicion is diagnostic.
3. Pulmonary Angiography (Conventional / Catheter-Based)
- Historically the gold standard, now rarely used — replaced by CTPA.
- Reserved for cases where CTPA is non-diagnostic and high suspicion persists.
- Also used when catheter-directed thrombolysis is being performed.
4. Echocardiography (Echo)
- Bedside TTE or TEE — especially valuable in hemodynamically unstable patients.
- Findings: RV dilation, RV hypokinesis, paradoxical septal motion, tricuspid regurgitation, McConnell's sign.
- Can directly visualize clot in right heart or proximal pulmonary arteries.
- Used for risk stratification (massive PE) and guiding reperfusion decisions.
5. Compression Ultrasonography (CUS) of Lower Limbs
- Detects DVT (proximal or distal) as the source of PE.
- If DVT is confirmed in a patient with suspected PE, anticoagulation can be initiated without further imaging.
- Used as an adjunct, especially when CTPA is unavailable.
6. Chest X-Ray (CXR)
- Usually normal or non-specific in PE.
- Classic (rare) findings:
- Westermark sign — oligemia distal to embolus
- Hampton's hump — wedge-shaped pleural-based opacity (pulmonary infarction)
- Palla's sign — enlarged right descending pulmonary artery
- Mainly used to exclude other diagnoses (pneumothorax, pneumonia, CHF).
7. ECG (Electrocardiogram)
- Commonly shows sinus tachycardia (most frequent).
- Classic but rare findings of RV strain:
- S1Q3T3 pattern
- Right bundle branch block (RBBB)
- Right axis deviation
- T-wave inversions in V1–V4
- Not diagnostic; used to assess RV strain and exclude MI.
8. MRI Pulmonary Angiography (MRPA)
- Limited use due to availability, cost, and motion artifact.
- Alternative to CTPA in pregnant patients or those with contrast/radiation concerns.
Diagnostic Algorithm Summary
Clinical Suspicion for PE
↓
Assess Pre-Test Probability (Wells Score)
↓
Low/Intermediate Probability → D-Dimer
→ Negative D-Dimer: PE EXCLUDED
→ Positive D-Dimer: → CTPA
↓
High Probability → CTPA directly (skip D-dimer)
↓
Hemodynamically Unstable → Bedside Echo first
Quick Reference Table
| Test | Role | Key Point |
|---|---|---|
| Wells Score | Pre-test probability | First step always |
| PERC Rule | Rule-out in low-risk | All 8 criteria must be negative |
| D-Dimer | Screen low/intermediate risk | Negative rules out PE |
| CTPA | Confirm diagnosis | Gold standard imaging |
| V/Q Scan | Alternative to CTPA | For contrast/renal contraindications |
| Echo | Unstable patients; RV strain | Guides resuscitation |
| CUS (leg DVT) | Adjunct | DVT = anticoagulate |
| ECG | Adjunct | Sinus tach; S1Q3T3 |
| CXR | Exclude differentials | Westermark/Hampton's hump (rare) |
| Troponin/BNP | Risk stratification | Not diagnostic |
The CTPA remains the definitive test for confirming PE, while D-dimer is the critical gatekeeper to avoid unnecessary imaging in low-to-intermediate risk patients.
This is a shared conversation. Sign in to Orris to start your own chat.