I have all the context I need. Let me now compose the full, comprehensive anatomy answer from my knowledge, supplemented by the retrieved material.
Comprehensive Human Anatomy Guide
1. Heart: Structure and Topography. Pericardium
Topography (Location)
The heart lies in the mediastinum (middle compartment of the thoracic cavity), between the two lungs. It sits on the diaphragm, behind the sternum, and is slightly tilted to the left. About 2/3 of the heart is to the left of the midline.
Borders:
- Superior: 2nd rib level (great vessels emerge here)
- Inferior: 5th intercostal space (apex beat felt here)
- Right border: Right atrium
- Left border: Left ventricle + left auricle
External Structure
The heart has 4 chambers:
| Chamber | Function |
|---|
| Right Atrium (RA) | Receives deoxygenated blood from body (via SVC + IVC) |
| Right Ventricle (RV) | Pumps deoxygenated blood to lungs |
| Left Atrium (LA) | Receives oxygenated blood from lungs (4 pulmonary veins) |
| Left Ventricle (LV) | Pumps oxygenated blood to the whole body |
External surfaces:
- Anterior (sternocostal): Mainly RV
- Posterior (base): Mainly LA
- Inferior (diaphragmatic): RV + LV
- Apex: LV, points down-left to 5th intercostal space, mid-clavicular line
Sulci (grooves):
- Coronary sulcus (atrioventricular groove): Separates atria from ventricles; contains coronary arteries and coronary sinus
- Anterior interventricular sulcus: Front, separates two ventricles
- Posterior interventricular sulcus: Back, separates two ventricles
Internal Structure
Right Atrium:
- Receives SVC (superiorly) and IVC (inferiorly)
- Fossa ovalis — oval depression; remnant of foramen ovale (fetal)
- Crista terminalis — smooth muscle ridge
- Pectinate muscles — rough muscular ridges
Right Ventricle:
- Inlet: tricuspid valve (3 leaflets)
- Trabeculae carneae (irregular muscle ridges)
- Papillary muscles → connect to tricuspid cusps via chordae tendineae (prevent valve eversion)
- Outlet: pulmonary valve (3 semilunar cusps) → pulmonary trunk
Left Atrium:
- Receives 4 pulmonary veins
- Smooth walls posteriorly; auricle is rough
- Outlet: mitral valve (bicuspid — 2 leaflets)
Left Ventricle:
- Thickest wall (~3x thicker than RV — pumps systemic circulation)
- Inlet: mitral valve
- Outlet: aortic valve (3 semilunar cusps) → ascending aorta
- Interventricular septum — mostly muscular, upper part membranous
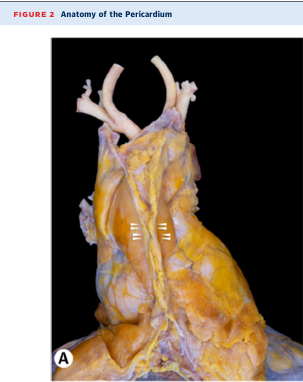
Pericardium
The pericardium is a double-layered fibro-serous sac enclosing the heart.
Layers:
Fibrous pericardium (outer)
↓
Parietal layer of serous pericardium
↓
Pericardial cavity (contains ~15–50 mL of fluid — acts as lubricant)
↓
Visceral layer of serous pericardium = EPICARDIUM (directly on heart surface)
Fibrous pericardium:
- Tough, inextensible connective tissue
- Attached inferiorly to central tendon of diaphragm
- Anteriorly attached to sternum by sternopericardial ligaments
- Fused with roots of great vessels (aorta, pulmonary trunk, SVC, IVC)
- Prevents overdistension of the heart
Serous pericardium:
- Parietal layer lines the inside of fibrous pericardium
- Visceral layer (epicardium) covers the heart surface
- Between them: pericardial cavity with serous fluid
Pericardial Sinuses (important surgically):
- Transverse pericardial sinus: Behind aorta + pulmonary trunk, in front of SVC; surgeons use it to clamp great vessels
- Oblique pericardial sinus: Behind the heart, between pulmonary veins and IVC; blind-ended recess
Clinical relevance: Excess fluid = pericardial effusion → can compress the heart → cardiac tamponade (life-threatening)
Cadaveric dissection showing pericardium and great vessels at the base of the heart.
2. Arch of the Aorta and Its Branches. Common, External & Internal Carotid Arteries. Subclavian Artery. Arterial Circle of the Brain
Aorta Overview
The aorta is the largest artery in the body. It has 4 parts:
- Ascending aorta (gives off coronary arteries)
- Arch of aorta
- Descending thoracic aorta
- Abdominal aorta
Arch of the Aorta
The arch begins at the level of the sternal angle (angle of Louis, T4), curves over the left pulmonary root, and becomes the descending thoracic aorta at T4.
3 Branches (right to left):
| Branch | What it supplies |
|---|
| Brachiocephalic trunk (innominate artery) | Divides into right common carotid + right subclavian |
| Left common carotid artery | Head and neck (left side) |
| Left subclavian artery | Left upper limb |
Memory tip: "Bring Lunch, Come Supper Leaving" or simply: BraCh, LCC, LSC
Common Carotid Artery (CCA)
- Right CCA: Branch of brachiocephalic trunk
- Left CCA: Direct branch of aortic arch
- Both ascend in the carotid sheath (with internal jugular vein and vagus nerve)
- Bifurcate at the level of C4 (upper border of thyroid cartilage) into:
- Internal carotid artery (ICA)
- External carotid artery (ECA)
At the bifurcation:
- Carotid sinus — baroreceptor (pressure sensor), on ICA origin
- Carotid body — chemoreceptor (O₂/CO₂ sensor)
External Carotid Artery (ECA)
Supplies: face, scalp, neck, oral cavity, pharynx, dura
8 Branches (mnemonic: "Some Anatomists Like Finding Odd Parts Somewhere Meaningful"):
| Branch | Area Supplied |
|---|
| Superior thyroid | Thyroid gland |
| Ascending pharyngeal | Pharynx, meninges |
| Lingual | Tongue |
| Facial | Face |
| Occipital | Back of scalp |
| Posterior auricular | Behind ear |
| Superficial temporal | Scalp (terminal) |
| Maxillary | Deep face, teeth, meninges (terminal) |
Internal Carotid Artery (ICA)
- No branches in the neck
- Enters skull via carotid canal in petrous temporal bone
- Passes through cavernous sinus
- Enters cranial cavity and supplies the brain
Main branches inside skull:
- Ophthalmic artery → orbit and eye
- Anterior cerebral artery (ACA) → medial frontal/parietal lobe
- Middle cerebral artery (MCA) → lateral hemisphere (largest branch; most common stroke vessel)
- Posterior communicating artery (PComA) → connects to posterior circulation
Subclavian Artery
- Right: from brachiocephalic trunk
- Left: direct from aortic arch
Passes between anterior and middle scalene muscles (with brachial plexus — scalene gap).
Major branches:
| Branch | Supply |
|---|
| Vertebral artery | Brain (posterior circulation), spinal cord |
| Internal thoracic (mammary) artery | Anterior chest wall, breast |
| Thyrocervical trunk | Thyroid, neck muscles |
| Costocervical trunk | Deep neck, 1st–2nd intercostals |
| Dorsal scapular artery | Rhomboid muscles |
Beyond the lateral border of 1st rib → becomes the axillary artery.
Arterial Circle of the Brain (Circle of Willis)
A ring of anastomosing arteries at the base of the brain, surrounding the optic chiasm and pituitary stalk. It equalizes blood pressure and provides collateral flow if one vessel is blocked.
Components (going around):
Anterior communicating artery (AComA)
|
Left ACA ←—→ Right ACA
|
Left ICA Right ICA
| |
Left PComA Right PComA
| |
Left PCA ←—→ Right PCA
|
Basilar artery (from two vertebral arteries)
Anterior circulation (ICA territory): ACA + MCA
Posterior circulation (vertebrobasilar): PCA + basilar + vertebral arteries
Clinical: Most berry (saccular) aneurysms occur at junctions in the Circle of Willis — especially at the AComA (most common), followed by PComA.
3. Thoracic Aorta. Axillary Artery. Arteries of the Upper Limb
Thoracic (Descending) Aorta
Runs from T4 to T12 (where it passes through the aortic hiatus of the diaphragm → becomes abdominal aorta).
Branches:
| Type | Branch | Supply |
|---|
| Visceral | Pericardial branches | Pericardium |
| Bronchial arteries (2 left, 1 right) | Lung parenchyma |
| Esophageal branches | Esophagus |
| Mediastinal branches | Mediastinal nodes/connective tissue |
| Parietal | Posterior intercostal arteries (3–11) | Intercostal spaces |
| Subcostal arteries | Below 12th rib |
| Superior phrenic arteries | Diaphragm (superiorly) |
Axillary Artery
Continuation of subclavian artery from lateral border of 1st rib to lower border of teres major (then becomes brachial artery).
Divided into 3 parts by the pectoralis minor muscle:
| Part | Location | Branches |
|---|
| 1st (medial to pec minor) | — | Superior thoracic |
| 2nd (behind pec minor) | — | Thoracoacromial, lateral thoracic |
| 3rd (lateral to pec minor) | — | Subscapular, anterior/posterior circumflex humeral |
Arteries of the Upper Limb
Subclavian → Axillary → Brachial
|
Radial ←———→ Ulnar
| |
Deep palmar arch ← Superficial palmar arch
|
Digital arteries
Brachial artery:
- Main artery of the arm (upper limb above elbow)
- Runs with median nerve in the medial bicipital groove
- Divides at the neck of radius (cubital fossa) into radial and ulnar arteries
- Profunda brachii = deep branch supplying posterior compartment (with radial nerve in spiral groove)
Radial artery:
- Lateral forearm → wrist → "anatomical snuffbox" → palm
- Forms deep palmar arch (with deep branch of ulnar)
- Used for arterial blood gas sampling and coronary catheterization
Ulnar artery:
- Medial forearm → enters hand via Guyon's canal
- Forms superficial palmar arch (main arch, with superficial branch of radial)
Palmar arches → common palmar digital arteries → proper digital arteries (supply fingers)
4. Abdominal Aorta. Common, External & Internal Iliac Arteries. Lower Limb Arteries
Abdominal Aorta
From T12 (aortic hiatus) to L4 (where it bifurcates into two common iliac arteries). Runs just to the left of the midline on the anterior surface of lumbar vertebrae.
Branches:
| Type | Branch | Level | Supply |
|---|
| Unpaired visceral | Celiac trunk | T12/L1 | Foregut (stomach, liver, spleen, upper duodenum) |
| Superior mesenteric artery (SMA) | L1 | Midgut (small intestine, right colon) |
| Inferior mesenteric artery (IMA) | L3 | Hindgut (left colon, sigmoid, rectum) |
| Paired visceral | Suprarenal arteries | L1 | Adrenal glands |
| Renal arteries | L1–L2 | Kidneys |
| Gonadal arteries | L2 | Testes/ovaries |
| Parietal | Lumbar arteries (4 pairs) | L1–L4 | Posterior wall |
| Inferior phrenic | T12 | Diaphragm |
| Median sacral | L4 | Sacrum |
Common Iliac Arteries
At L4, the aorta bifurcates into two common iliac arteries. Each runs inferolaterally and divides at the sacroiliac joint into:
- External iliac artery → lower limb
- Internal iliac artery → pelvis
Internal Iliac Artery (Hypogastric)
Supplies the pelvic organs, buttocks, and perineum.
Anterior division:
- Superior/inferior vesical → bladder
- Uterine artery (females)
- Obturator → medial thigh
- Internal pudendal → perineum, external genitalia
- Inferior gluteal → gluteal region
Posterior division:
- Superior gluteal → gluteal region (largest branch)
- Iliolumbar, lateral sacral
External Iliac Artery
Gives off:
- Inferior epigastric artery → anterior abdominal wall
- Deep circumflex iliac artery → iliac region
Then passes under the inguinal ligament → becomes femoral artery.
Lower Limb Arteries
Aorta (L4) → Common Iliac → External Iliac
↓
Femoral artery (in femoral triangle)
↓
Deep femoral (profunda femoris) ← thigh muscles
↓
Popliteal artery (behind the knee)
/ \
Anterior tibial Posterior tibial
↓ ↓
Dorsalis pedis Peroneal (fibular)
(dorsum of foot) + Plantar arteries → plantar arch
Femoral artery:
- Main artery of the thigh
- Lies in the femoral triangle (bounded by inguinal ligament, sartorius, adductor longus)
- Deep femoral (profunda femoris): biggest branch — supplies thigh muscles and hip
- Passes through the adductor canal (Hunter's canal) → becomes popliteal artery
Popliteal artery:
- Behind the knee in the popliteal fossa
- Terminates by dividing into anterior and posterior tibial arteries
Anterior tibial: → passes through interosseous membrane → continues as dorsalis pedis artery on dorsum of foot
Posterior tibial: → runs in posterior compartment → passes behind medial malleolus → divides into medial and lateral plantar arteries → plantar arch
5. Superior and Inferior Vena Cava
Superior Vena Cava (SVC)
- Formed by union of right and left brachiocephalic (innominate) veins at the level of the right 1st costal cartilage
- Brachiocephalic veins are formed by union of the internal jugular vein + subclavian vein (at the angle of confluence = venous angle of Pirogov)
- SVC descends ~7 cm, enters the right atrium at the level of the 3rd costal cartilage
- Lower half of SVC is within the pericardium
- No valves
- Drains: head, neck, upper limbs, thoracic wall
Tributaries of SVC:
- Left and right brachiocephalic veins
- Azygos vein (enters just before reaching RA)
- Small mediastinal and pericardial veins
Inferior Vena Cava (IVC)
- Formed at L5 by union of the two common iliac veins
- Ascends on the right of the aorta
- Passes through caval opening in diaphragm at T8
- Enters right atrium from below
- Contains a valve (valve of IVC / Eustachian valve) — rudimentary in adults
Tributaries (from below upward):
| Tributary | What it drains |
|---|
| Common iliac veins (L + R) | Pelvis and lower limbs |
| Lumbar veins | Posterior abdominal wall |
| Right gonadal vein | Right testis/ovary (left drains to left renal vein) |
| Renal veins | Kidneys |
| Right suprarenal vein | Right adrenal |
| Hepatic veins (3) | Liver |
| Inferior phrenic veins | Diaphragm |
Note: The left gonadal vein and left suprarenal vein drain into the left renal vein, not directly into the IVC.
6. Portal Vein. Venous Anastomoses. Fetal Circulation
Portal Vein
The hepatic portal vein carries nutrient-rich blood from the GI tract and spleen to the liver (for processing) before it enters the systemic circulation.
Formation: Formed behind the neck of the pancreas at L2 by union of:
- Superior mesenteric vein (SMV) — from small intestine + right colon
- Splenic vein — from spleen + inferior mesenteric vein (left colon, sigmoid, rectum)
Course: Ascends in the free edge of lesser omentum (hepatoduodenal ligament) with hepatic artery (left) and bile duct (right) → enters liver at the porta hepatis → divides into right and left portal branches → sinusoids → hepatic veins → IVC
Normal portal pressure: 5–10 mmHg
Portal hypertension: >12 mmHg → causes varices, ascites, splenomegaly
Porto-Systemic (Venous) Anastomoses
These are critical connections between the portal and systemic venous systems. They open up (become dilated = varices) when portal pressure is high:
| Site | Portal vessel | Systemic vessel | Clinical result |
|---|
| Lower esophagus | Left gastric vein | Azygos/hemiazygos | Esophageal varices (most dangerous — can rupture and cause fatal hemorrhage) |
| Rectum/anal canal | Superior rectal vein | Middle/inferior rectal vein | Rectal varices / hemorrhoids |
| Umbilicus | Paraumbilical veins | Superficial epigastric veins | Caput medusae (dilated veins radiating from umbilicus) |
| Retroperitoneum | Colic/splenic veins | Renal/lumbar veins | Retroperitoneal varices (Retzius veins) |
| Bare area of liver | Portal tributaries | Phrenic/intercostal veins | — |
Fetal Circulation
Fetal circulation differs because the lungs are non-functional and the placenta is the site of gas exchange.
Key structures unique to fetal circulation:
| Structure | Description | Fate after birth |
|---|
| Umbilical vein | Carries oxygenated blood from placenta to fetus | Becomes ligamentum teres (round ligament of liver) |
| Ductus venosus | Shunts oxygenated blood past liver sinusoids → IVC | Becomes ligamentum venosum |
| Foramen ovale | Opening in atrial septum → blood flows RA → LA (bypasses lungs) | Closes → becomes fossa ovalis |
| Ductus arteriosus | Connects pulmonary trunk → aorta (bypasses lungs) | Closes → becomes ligamentum arteriosum |
| Umbilical arteries (x2) | Carry deoxygenated blood from fetus → placenta | Become medial umbilical ligaments |
Fetal blood flow path:
Placenta (O₂ rich)
→ Umbilical vein
→ Ductus venosus (bypasses liver)
→ IVC
→ Right atrium
→ Foramen ovale → LEFT atrium (most of the oxygenated blood)
→ Left ventricle → Aorta → Body
Some blood: RA → RV → Pulmonary trunk
→ Ductus arteriosus → Aorta (bypasses lungs)
After birth: Lungs expand, pulmonary resistance drops → foramen ovale closes (pressure change), ductus arteriosus closes (O₂ increase → prostaglandin drop).
7. Lymphatic System: Trunks, Tributaries, Regional Lymph Nodes, Thoracic Duct
Overview
The lymphatic system:
- Returns interstitial fluid to blood
- Transports dietary fats (chylomicrons) from gut
- Provides immune surveillance
Levels: Lymph capillaries → lymphatic vessels → lymph nodes → lymphatic trunks → lymphatic ducts → venous angles (subclavian + jugular veins)
Lymphatic Trunks (9 paired/unpaired trunks):
| Trunk | Drains |
|---|
| Jugular trunks (L + R) | Head and neck |
| Subclavian trunks (L + R) | Upper limbs |
| Bronchomediastinal trunks (L + R) | Thoracic organs |
| Lumbar trunks (L + R) | Lower limbs, pelvis, kidneys |
| Intestinal trunk (single) | GI tract, liver, spleen |
Thoracic Duct
The largest lymphatic vessel in the body (~38–45 cm long).
Formation: Begins in the abdomen as the cisterna chyli (at L1–L2), a dilated lymphatic sac formed by:
- Left + right lumbar trunks
- Intestinal trunk
Course:
- Ascends through the aortic hiatus of the diaphragm (with aorta)
- Runs in the posterior mediastinum between the aorta (left) and azygos vein (right)
- At T5, crosses to the left side
- Ascends behind the left carotid sheath
- Terminates at the left venous angle (junction of left internal jugular + left subclavian veins)
Tributaries (in addition to cisterna chyli):
- Left jugular trunk
- Left subclavian trunk
- Left bronchomediastinal trunk
The thoracic duct drains ~75% of the body (everything EXCEPT the right upper quadrant).
Regional Lymph Nodes (key groups):
| Region | Nodes | Drainage |
|---|
| Head/neck | Cervical (deep + superficial), occipital, parotid, submandibular, submental | Head, neck, face |
| Axilla | Anterior, posterior, lateral, central, apical | Upper limb, breast, chest wall |
| Thorax | Paratracheal, tracheobronchial, mediastinal | Lung, heart, esophagus |
| Abdomen | Celiac, mesenteric, para-aortic (lumbar) | Abdominal viscera |
| Pelvis | Internal/external iliac, sacral, obturator | Pelvic organs |
| Inguinal | Superficial + deep inguinal | Lower limb, perineum |
8. Right Lymphatic Duct
A short vessel (~1.5 cm) formed by union of:
- Right jugular trunk (head/neck right side)
- Right subclavian trunk (right upper limb)
- Right bronchomediastinal trunk (right thorax)
Terminates at the right venous angle (right internal jugular + right subclavian vein junction).
Drains the right upper quadrant of the body:
- Right side of head and neck
- Right upper limb
- Right thorax
- Right side of heart
- Right lung
- Right upper lobe of liver
The rest of the body (everything else = ~75%) drains via the thoracic duct into the left venous angle.
9. Sense Organs. Organ of Vision. Eyeball Structure. Auxiliary Apparatus. Vestibulcocochlear Organ. Outer, Middle & Inner Ear
Classification of Sense Organs
| Type | Description | Examples |
|---|
| Type I | Sensory neurons directly exposed | Olfactory epithelium |
| Type II | Specialized epithelial receptor cells → synapse onto sensory neurons | Taste buds, hair cells of ear |
| Type III | Receptor = dendritic endings of sensory neurons | Skin receptors (touch, pain) |
Organ of Vision — The Eye
Eyeball Structure
The eyeball has 3 concentric layers (tunics):
1. Fibrous tunic (outer):
- Sclera (posterior 5/6): White, tough, maintains shape; extraocular muscles attach here
- Cornea (anterior 1/6): Transparent, avascular, most refractive surface of the eye
2. Vascular tunic (middle = uvea):
- Choroid: Posterior, highly vascular; nourishes outer retina; dark (absorbs scattered light)
- Ciliary body: Contains ciliary muscle (controls lens shape for accommodation) and produces aqueous humor
- Iris: Pigmented ring with central pupil; contains sphincter pupillae (constricts — parasympathetic CN III) and dilator pupillae (dilates — sympathetic)
3. Nervous tunic (inner) = Retina:
- 10 layers, including:
- Photoreceptors: rods (dim light, peripheral vision) and cones (color, detail, central)
- Bipolar cells → Ganglion cells → axons form optic nerve
- Fovea centralis: Point of sharpest vision (highest cone density); located in the macula lutea
- Optic disc (blind spot): Where optic nerve exits; no photoreceptors
Internal compartments:
- Anterior chamber: Between cornea and iris; contains aqueous humor (produced by ciliary body; drains via canal of Schlemm at the iridocorneal angle)
- Posterior chamber: Between iris and lens
- Vitreous chamber: Behind lens; filled with vitreous humor (gel-like, maintains shape)
Lens:
- Biconvex, transparent, avascular, elastic
- Suspended by zonular fibers (suspensory ligaments of Zinn) from ciliary body
- Accommodation: ciliary muscle contracts → zonules relax → lens becomes more convex → focuses near objects
Auxiliary (Accessory) Apparatus of the Eye
| Structure | Function |
|---|
| Eyelids (palpebrae) | Protect eye; distribute tears |
| Conjunctiva | Mucous membrane lining lids + anterior sclera |
| Lacrimal apparatus | Lacrimal gland (superolateral) → lacrimal fluid → puncta → lacrimal sac → nasolacrimal duct → inferior nasal meatus |
| Extraocular muscles (6) | Move the eyeball |
| Eyebrows | Shield from sweat and light |
6 Extraocular Muscles:
| Muscle | Action | Nerve |
|---|
| Superior rectus | Elevation, adduction, intorsion | CN III (oculomotor) |
| Inferior rectus | Depression, adduction, extorsion | CN III |
| Medial rectus | Adduction | CN III |
| Lateral rectus | Abduction | CN VI (abducens) |
| Superior oblique | Depression, abduction, intorsion | CN IV (trochlear) |
| Inferior oblique | Elevation, abduction, extorsion | CN III |
Mnemonic: "LR₆SO₄" = Lateral Rectus → CN6, Superior Oblique → CN4, rest → CN3
Vestibulocochlear Organ (CN VIII) — Ear
The ear has 3 parts:
Outer Ear
- Auricle (pinna): Elastic cartilage covered by skin; collects and funnels sound waves
- External acoustic meatus: Canal (~2.5 cm) from pinna to tympanic membrane; lined with skin, contains ceruminous glands (produce ear wax)
- Tympanic membrane (eardrum): Semitransparent, obliquely set membrane; vibrates with sound waves; consists of 3 layers (outer epithelium, middle fibrous layer, inner mucosa)
Middle Ear (Tympanic Cavity)
- Air-filled cavity in the petrous temporal bone
- Ossicles (3 smallest bones in body):
- Malleus (hammer): Handle attached to tympanic membrane; head articulates with incus
- Incus (anvil): Middle bone
- Stapes (stirrup): Footplate sits in oval window → transmits vibrations to inner ear
- Muscles: Tensor tympani (CN V₃ → dampens vibration), Stapedius (CN VII → dampens loud noise)
- Auditory (Eustachian) tube: Connects middle ear to nasopharynx; equalizes air pressure
- Mastoid air cells: Communicate with middle ear
Inner Ear (Labyrinth)
Located in the petrous part of temporal bone.
Has two parts:
- Bony labyrinth — outer shell of bone; filled with perilymph (similar to CSF/ECF)
- Membranous labyrinth — inner sac system; filled with endolymph (high K⁺, like ICF)
Bony labyrinth consists of:
| Structure | Function |
|---|
| Cochlea | Hearing (snail-shaped, 2.5 turns) |
| Vestibule | Houses utricle + saccule; equilibrium (linear acceleration + gravity) |
| Semicircular canals (3) | Rotational/angular acceleration sensing |
Cochlea:
- 3 scalae: Scala vestibuli, Scala tympani, Scala media (cochlear duct, membranous)
- Organ of Corti — on basilar membrane inside cochlear duct; contains inner and outer hair cells → detect sound vibrations → CN VIII (cochlear branch)
- Tonotopic organization: High frequency detected at base; low frequency at apex
Vestibular apparatus:
- Utricle and Saccule → maculae with otoliths (otoconia) → detect gravity and linear acceleration
- 3 Semicircular canals (anterior, posterior, lateral) → ampullae with cristae (hair cells in cupula) → detect rotational head movements
- → CN VIII (vestibular branch) → vestibular nuclei → cerebellum + brainstem + spinal cord + eye muscles
10. Organs of Smell and Taste. Skin and Its Derivatives. Breast
Organ of Smell (Olfaction)
- Located in the olfactory epithelium in the upper nasal cavity (superior nasal concha region)
- Contains olfactory receptor neurons (Type I sense organ) — bipolar neurons with cilia projecting into mucus
- Odorant molecules dissolve in mucus → bind receptors → action potential
- Axons pass through cribriform plate of ethmoid → olfactory bulb → olfactory tract → primary olfactory cortex (piriform cortex, amygdala) — no thalamic relay (unique among senses)
Organ of Taste (Gustation)
- Taste buds located on papillae of the tongue:
- Fungiform papillae (anterior 2/3) — mushroom-shaped
- Circumvallate (vallate) papillae (posterior, at sulcus terminalis) — largest, surrounded by moat
- Foliate papillae (lateral tongue edges)
- Filiform papillae — no taste buds (tactile)
- 5 basic tastes: Sweet, Sour, Salty, Bitter, Umami
- Taste receptor cells (Type II) → synapse onto sensory neurons
Nerve supply:
- Anterior 2/3 tongue: CN VII (chorda tympani branch — taste) + CN V₃ (lingual nerve — general sensation)
- Posterior 1/3: CN IX (glossopharyngeal — taste + sensation)
- Epiglottis/pharynx: CN X (vagus)
- All taste signals → solitary nucleus (medulla) → thalamus → gustatory cortex (insula)
Skin (Integument)
The largest organ of the body (~1.5–2 m², ~16% body weight).
Layers:
| Layer | Description |
|---|
| Epidermis | Outer, avascular epithelium; 5 layers (stratum basale, spinosum, granulosum, lucidum, corneum) |
| Dermis | Dense connective tissue; contains blood vessels, nerves, hair follicles, glands |
| Hypodermis (subcutaneous) | Loose CT + fat; not true skin layer |
Epidermis layers (BSGC = Bottom to top):
- Stratum basale: Stem cells + melanocytes (produce melanin)
- Stratum spinosum: Keratinocytes connected by desmosomes
- Stratum granulosum: Keratohyalin granules form
- Stratum lucidum: Only in thick skin (palms/soles)
- Stratum corneum: Dead keratinocytes; protective outer barrier
Skin Derivatives (Appendages):
| Derivative | Description |
|---|
| Hair follicles | Produce hair; arrector pili muscle attached (goosebumps) |
| Sebaceous glands | Produce sebum (oil); usually drain into hair follicle |
| Eccrine sweat glands | All over body; temperature regulation |
| Apocrine sweat glands | Axilla, groin; activated at puberty; odor |
| Nails | Hard keratin plates; protect fingertips |
| Mammary glands | Modified apocrine glands |
Functions of skin: Protection, thermoregulation, sensation, vitamin D synthesis, immunological surveillance, excretion.
Breast (Mamma)
- Located in the anterior chest wall between the 2nd and 6th ribs, from lateral sternal border to mid-axillary line
- The breast lies on the pectoralis major muscle and fascia (also partly on serratus anterior)
- Axillary tail (of Spence): Extension of breast tissue into the axilla
Structure:
- 15–20 lobes of glandular tissue (modified sweat glands) arranged radially
- Each lobe has a lactiferous duct → converges at the nipple
- Lactiferous sinuses: Small dilations just beneath the areola — milk storage
- Separated by fibrous septa (Cooper's ligaments) — support breast; when invaded by cancer → skin dimpling
- Surrounded by fat (gives shape)
Nipple and areola:
- Nipple: Projection; contains 15–20 lactiferous duct openings
- Areola: Pigmented ring; contains Montgomery's glands (modified sebaceous glands)
Blood supply:
- Internal thoracic (mammary) artery → medial breast
- Lateral thoracic artery → lateral breast
- Intercostal arteries
Lymphatic drainage (very important clinically):
- ~75% drains to axillary lymph nodes (especially anterior/pectoral group)
- ~25% to internal mammary (parasternal) nodes
- Also to: posterior intercostal, clavicular, supraclavicular nodes
- Sentinel lymph node = first axillary node to receive drainage; biopsied in breast cancer staging
11. General Overview of the Nervous System. Spinal Cord
Overview of the Nervous System
Divisions:
Nervous System
├── Central Nervous System (CNS)
│ ├── Brain
│ └── Spinal Cord
└── Peripheral Nervous System (PNS)
├── Somatic (voluntary — skeletal muscles, skin)
└── Autonomic (involuntary — viscera, smooth muscle, glands)
├── Sympathetic ("fight or flight")
└── Parasympathetic ("rest and digest")
Cells:
- Neurons — functional units; consist of cell body, dendrites (input), axon (output)
- Neuroglia (glia) — supportive cells: astrocytes, oligodendrocytes (CNS myelin), Schwann cells (PNS myelin), microglia (immune), ependymal cells (CSF production)
Spinal Cord
Macrostructure and Topography
- Extends from the medulla oblongata (foramen magnum) to L1–L2 (conus medullaris) in adults
- Below L2: Cauda equina (bundle of lumbar/sacral nerve roots floating in CSF)
- The filum terminale (glial/connective tissue strand) anchors the cord to the coccyx
- Length: ~45 cm in adults; diameter: ~1 cm
Enlargements:
- Cervical enlargement (C4–T1): For upper limb innervation (brachial plexus)
- Lumbosacral enlargement (L1–S3): For lower limb innervation (lumbar/sacral plexus)
31 pairs of spinal nerves:
- 8 Cervical (C1–C8)
- 12 Thoracic (T1–T12)
- 5 Lumbar (L1–L5)
- 5 Sacral (S1–S5)
- 1 Coccygeal
Each spinal nerve has:
- Dorsal (posterior) root — carries sensory fibers; has dorsal root ganglion (DRG) with sensory cell bodies
- Ventral (anterior) root — carries motor fibers
Gray Matter (H-shaped in cross-section)
| Horn | Content | Function |
|---|
| Anterior (ventral) horn | Lower motor neurons (α, γ motor neurons) | Skeletal muscle control |
| Posterior (dorsal) horn | Sensory interneurons (substantia gelatinosa, nucleus proprius) | Process incoming sensory signals |
| Lateral horn (T1–L2, S2–S4) | Preganglionic autonomic neurons | Sympathetic (T1–L2), Parasympathetic (S2–S4) |
| Central gray (around central canal) | — | — |
Rexed laminae: Gray matter organized into 10 laminae (I–X) based on cytoarchitecture.
White Matter
Organized into 3 paired funiculi (columns):
| Funiculus | Location | Main tracts |
|---|
| Posterior (dorsal) | Between two posterior horns | Fasciculus gracilis + fasciculus cuneatus = dorsal column-medial lemniscal pathway (fine touch, vibration, proprioception — IPSILATERAL) |
| Lateral | Between anterior and posterior horns | Lateral corticospinal tract (voluntary motor, contralateral); Spinothalamic tract (pain/temperature, crosses within 2 segments); Rubrospinal, spinocerebellar tracts |
| Anterior (ventral) | Anterior to anterior horns | Anterior corticospinal tract (crosses in medulla); vestibulospinal, reticulospinal tracts |
Meninges (Coverings of Spinal Cord)
From outside in:
| Layer | Description |
|---|
| Dura mater | Tough outer layer; forms epidural space (containing fat + epidural veins) outside it |
| Arachnoid mater | Middle delicate layer; subdural space between dura and arachnoid (potential space) |
| Pia mater | Innermost; directly on cord surface; subarachnoid space between arachnoid and pia — contains CSF; denticulate ligaments of pia anchor cord to dura |
Lumbar puncture is performed at L3–L4 or L4–L5 (safely below the conus medullaris at L1–L2) to sample CSF from the subarachnoid space.
12. Base and Midline Section of the Brain. Cranial Nerves. Medulla Oblongata
Brain Divisions
| Division | Components |
|---|
| Telencephalon | Cerebral hemispheres (cortex, basal ganglia, limbic structures) |
| Diencephalon | Thalamus, hypothalamus, epithalamus (pineal), subthalamus |
| Mesencephalon | Midbrain (cerebral peduncles, tectum, tegmentum) |
| Metencephalon | Pons + Cerebellum |
| Myelencephalon | Medulla oblongata |
The brainstem = Midbrain + Pons + Medulla.
12 Pairs of Cranial Nerves
Origin from brain and exit through skull:
| CN | Name | Type | Exit from Brain | Exit from Skull |
|---|
| I | Olfactory | Sensory | Olfactory bulb | Cribriform plate (ethmoid) |
| II | Optic | Sensory | Diencephalon (LGN) | Optic canal |
| III | Oculomotor | Motor | Midbrain (interpeduncular fossa) | Superior orbital fissure |
| IV | Trochlear | Motor | Midbrain (dorsal, only CN to exit posteriorly) | Superior orbital fissure |
| V | Trigeminal | Mixed | Pons (lateral) | V₁: SOF; V₂: Foramen rotundum; V₃: Foramen ovale |
| VI | Abducens | Motor | Pontomedullary junction (medially) | Superior orbital fissure |
| VII | Facial | Mixed | Pontomedullary junction (laterally) | Internal acoustic meatus → stylomastoid foramen |
| VIII | Vestibulocochlear | Sensory | Pontomedullary junction | Internal acoustic meatus |
| IX | Glossopharyngeal | Mixed | Medulla (post-olivary groove) | Jugular foramen |
| X | Vagus | Mixed | Medulla (post-olivary groove) | Jugular foramen |
| XI | Accessory | Motor | Medulla + cervical spinal cord | Jugular foramen |
| XII | Hypoglossal | Motor | Medulla (pre-olivary groove) | Hypoglossal canal |
Mnemonic for names: "On Old Olympus' Towering Tops A Finn And German Viewed Some Hops"
Mnemonic for type (S/M/B): "Some Say Marry Money But My Brother Says Big Brains Matter More"
Medulla Oblongata
The most inferior part of the brainstem, continuous with the spinal cord at the foramen magnum.
External features:
- Anterior median fissure — continuous with spinal cord
- Pyramids (bilateral): Contain corticospinal fibers; pyramidal decussation (motor cross) occurs at lower medulla — explains contralateral control
- Olives (inferior olivary nuclei) — oval bulges lateral to pyramids; involved in cerebellar coordination
- Post-olivary groove: CN IX, X, XI emerge here
- Pre-olivary groove: CN XII emerges here
Internal — Gray Matter Nuclei:
| Nucleus | CN | Function |
|---|
| Hypoglossal nucleus | XII | Tongue muscles |
| Dorsal motor nucleus of vagus | X | Parasympathetic to thoracic/abdominal viscera |
| Nucleus ambiguus | IX, X, XI | Motor to pharynx, larynx, palate (swallowing/voice) |
| Solitary nucleus | VII, IX, X | Taste; visceral sensory (heart, lungs, gut) |
| Spinal trigeminal nucleus | V | Pain and temperature from face (extends into medulla) |
| Inferior olivary nucleus | — | Cerebellar learning/coordination relay |
| Cochlear nuclei | VIII | Hearing relay |
| Vestibular nuclei | VIII | Balance, eye movements, posture |
| Vital centers | — | Respiratory center, cardiovascular center, vomiting center |
Internal — White Matter Tracts:
| Tract | Location | Function |
|---|
| Pyramidal (corticospinal) tracts | Pyramids anteriorly | Voluntary movement, cross at decussation |
| Medial lemniscus | Medially | Fine touch/vibration/proprioception (from nucleus gracilis + cuneatus) |
| Spinothalamic tract | Lateral | Pain and temperature (from spinal cord) |
| Medial longitudinal fasciculus (MLF) | Near midline | Coordinates eye movements (CN III, IV, VI) |
| Inferior cerebellar peduncle | Posterolateral | Connects medulla to cerebellum |
Clinical significance of medulla:
- Lateral medullary syndrome (Wallenberg): Blockage of PICA (posterior inferior cerebellar artery) → ipsilateral face loss of pain/temp + contralateral body loss + vertigo + dysphagia + Horner's syndrome
- Damage to medullary vital centers → life-threatening (respiratory arrest, cardiac arrest)
This completes the full anatomy review across all listed topics. Each section covers the key structural and functional points you need for anatomy examinations. Let me know if you want any topic expanded further with more detail, diagrams, or clinical correlations.