Is this butterfly rash? Is Butterfly rash seen in dust allergy other than sle?
Reading File
search_medical_text
butterfly malar rash SLE lupus diagnosis features
search_medical_text
malar rash differential diagnosis causes other than SLE
search_medical_image
butterfly malar rash SLE lupus face
GradeResponse
GradeResponse
GradeResponse
Image Analysis
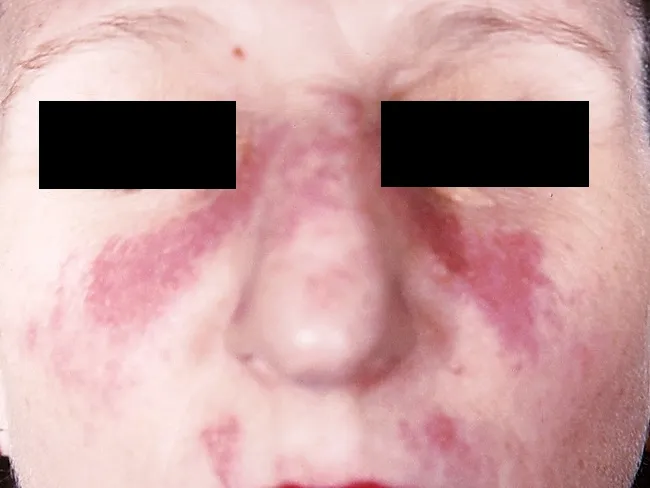
Looking at the photograph, there is bilateral facial discoloration/hyperpigmentation across both cheeks and the nose bridge. However, this does not appear to be a classic butterfly (malar) rash. Here's why:
What a true butterfly/malar rash looks like (for comparison):
The classic malar rash of SLE shows:
- Flat or slightly raised erythema (redness) over both cheeks and nasal bridge
- Spares the nasolabial folds (the creases from nose to mouth corners)
- Photosensitive — worsens with sun exposure
- Warm, flushed appearance
What is visible in this image:
- The changes appear to be brownish hyperpigmentation/post-inflammatory discoloration, not the acute erythema (redness/flush) of a butterfly rash
- There is no distinct malar flush or erythematous plaque
- The pigmentation looks patchy and involves areas beyond the typical malar distribution
This is more consistent with melasma, post-inflammatory hyperpigmentation, or sun-induced pigmentation rather than a butterfly rash.
Butterfly Rash: Is It Seen in Dust Allergy?
No — butterfly/malar rash is not a feature of dust allergy. Dust allergy (allergic rhinitis, atopic reactions to house dust mites) causes:
- Sneezing, nasal congestion, watery eyes
- Urticaria (hives) or eczema in sensitized individuals
- Not a fixed malar distribution rash
Conditions That Can Cause a Malar/Butterfly Rash (besides SLE):
| Condition | Key Distinguishing Features |
|---|---|
| SLE | Most classic; associated with ANA, anti-dsDNA, systemic features |
| Rosacea | Does NOT spare nasolabial folds; flushing, telangiectasia, pustules |
| Seborrheic dermatitis | Greasy scaling; involves nasolabial folds, eyebrows |
| Mixed Connective Tissue Disease (MCTD) | Overlap of SLE + myositis + scleroderma features; anti-U1-RNP positive (Harrison's, p. 10145) |
| Dermatomyositis | Heliotrope rash on eyelids; Gottron's papules on knuckles |
| Polymorphous light eruption | Photosensitive; resolves away from sun |
| Contact dermatitis | History of topical exposure; may mimic distribution |
| Fifth disease (Parvovirus B19) | "Slapped cheek" appearance; viral prodrome |
Important Recommendation
The facial changes in this image warrant an in-person evaluation by a dermatologist or rheumatologist. If there are associated symptoms like:
- Joint pain/swelling
- Fatigue
- Hair loss
- Oral ulcers
- Photosensitivity
...then SLE workup (ANA, anti-dsDNA, CBC, urinalysis) should be considered. If the picture is purely cosmetic pigmentation without systemic symptoms, a dermatologist can evaluate for melasma or other pigmentary disorders.
This is not a substitute for clinical examination. Please consult a physician for proper diagnosis.
No ulcers no fatigue no joint swelling only rashes no hair loss and buring when exposes to sun?
search_medical_text
photosensitive malar rash burning sun exposure no systemic symptoms differential diagnosis
search_medical_text
polymorphous light eruption rosacea photodermatitis facial rash burning sun
GradeResponse
GradeResponse
The clinical picture is becoming clearer. With no systemic symptoms (no joint pain, no fatigue, no oral ulcers, no hair loss) but photosensitivity with burning, the likely diagnoses shift away from SLE toward primary skin conditions.
Most Likely Diagnoses Given This Clinical Picture
1. Subacute Cutaneous Lupus Erythematosus (SCLE) — Must Rule Out
Even without systemic SLE features, SCLE can present as isolated photosensitive facial rash. Only ~50% of SCLE patients meet full SLE criteria. A simple ANA + anti-Ro/SSA antibody test can screen for this. This is important not to miss.
2. Rosacea (High probability)
- Chronic redness/flushing over cheeks and nose
- Burning and stinging on sun exposure is a hallmark feature
- No nasolabial fold sparing required
- Worsened by: sun, heat, spicy food, alcohol
- The brownish pigmentation seen in the photo can be post-inflammatory from chronic rosacea
3. Polymorphous Light Eruption (PMLE) (Harrison's, p. 1702)
- Most common photosensitivity disorder
- Burning/itching rash on sun-exposed areas
- Appears in spring/summer, may improve with continued exposure ("hardening")
- Face can be involved
- No systemic features
4. Photocontact Dermatitis / Chronic Photodamage
- Pigmentation + burning triggered by sun
- Can look very similar to what is seen in the photo
- Related to sun-sensitizing products (creams, fragrances, certain medications)
5. Melasma with Photosensitivity
- Brown patches on cheeks, nose, forehead
- Worsens dramatically with sun exposure
- Very common in South Asian women (middle-aged)
- Burning can occur if skin barrier is compromised
Summary Table
| Feature | Rosacea | PMLE | SCLE | Melasma |
|---|---|---|---|---|
| Facial rash | ✅ | ✅ | ✅ | ✅ |
| Burning with sun | ✅ | ✅ | ✅ | Mild |
| Systemic symptoms | ❌ | ❌ | Mild/none | ❌ |
| Pigmentation | Post-inflammatory | Rare | Sometimes | ✅ prominent |
| ANA positive | ❌ | ❌ | Often ✅ | ❌ |
What to Do
- Blood tests: ANA, anti-Ro/SSA — to exclude SCLE even without systemic symptoms
- See a dermatologist — clinical examination + possibly a skin biopsy can distinguish these conditions definitively
- Sun protection immediately: broad-spectrum SPF 50+ sunscreen every morning, regardless of the diagnosis — this will reduce burning and prevent worsening of pigmentation
Dust allergy does not cause this pattern — the rash and burning with sun exposure are unrelated to dust/allergen exposure.
This is clinical guidance only and not a substitute for in-person examination.
This is a shared conversation. Sign in to Orris to start your own chat.