Swelling over elbow joint case sheet orthopaedics and importantpoints
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Searching Images
olecranon bursitis elbow swelling
Searching the Web
orthopaedic case sheet swelling elbow joint history examination diagnosis important points
Loading Image
Loading Image
Reading Web Page
elbow swelling examination case sheet orthopaedic important points
Now I have comprehensive information to construct a thorough orthopaedic case sheet for swelling over the elbow joint. Let me compile everything:
📋 Orthopaedic Case Sheet — Swelling Over the Elbow Joint
Clinical Images
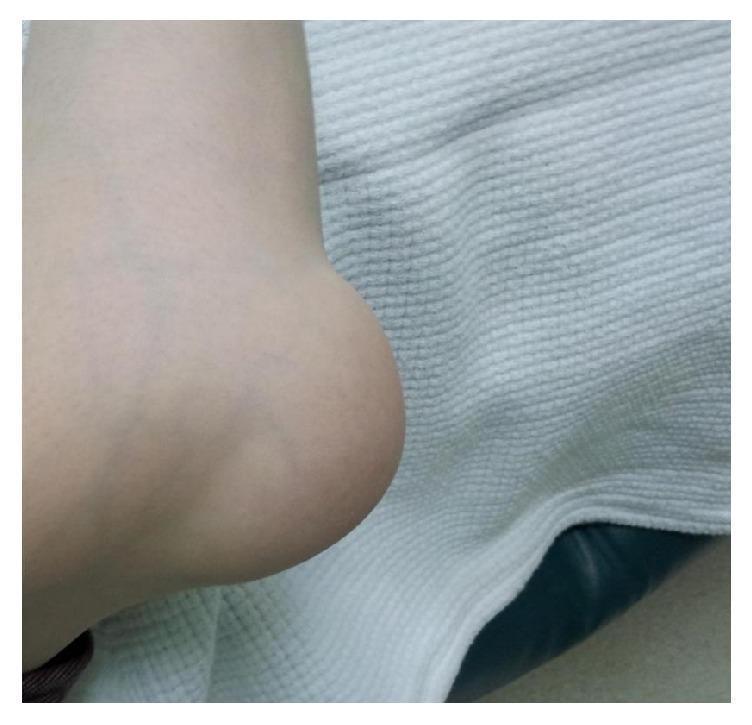
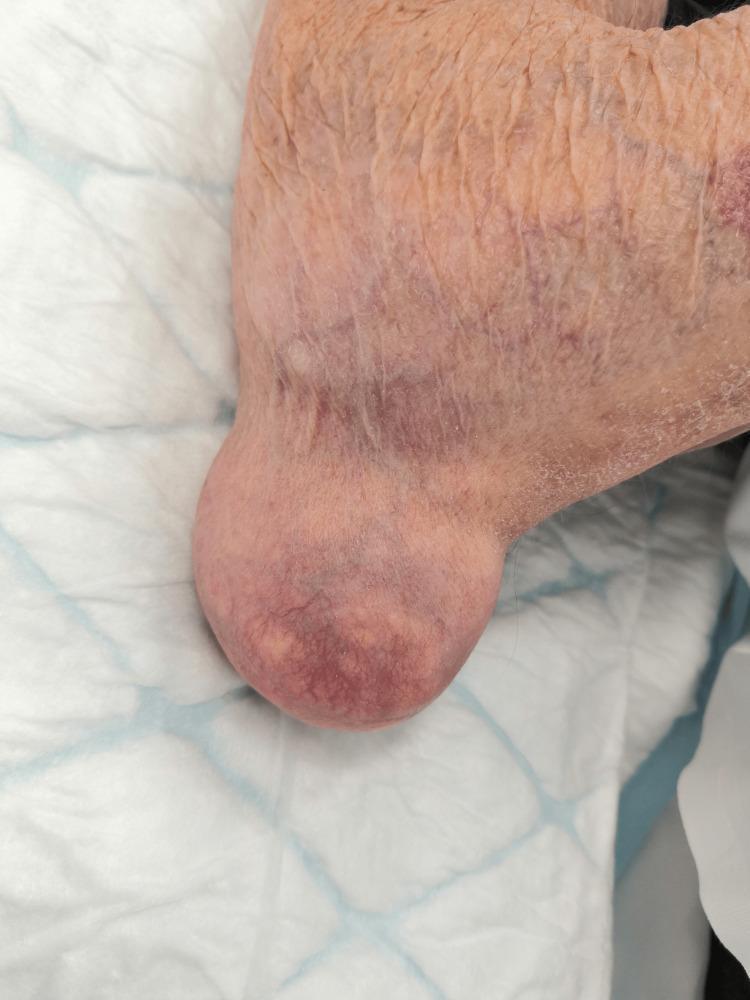
SECTION 1: HISTORY (Chief Complaints & HPI)
Biodata
| Field | Details |
|---|---|
| Name / Age / Sex | _____ |
| Occupation | ⚠️ Critical — laborers, miners, gardeners, plumbers (repetitive elbow trauma) |
| Dominant hand | Right / Left |
| Address | _____ |
Chief Complaint
"Swelling over the elbow of ___ duration"
History of Presenting Illness — Ask in SOCRATES Format
Site
- Posterior (olecranon region) → Bursitis, gout tophi, rheumatoid nodule
- Lateral → Lateral epicondyle swelling, loose body
- Medial → Medial epicondyle, cubital tunnel ganglion
- Diffuse / whole joint → Septic arthritis, rheumatoid, haemarthrosis, fracture
Onset
- Sudden after trauma → Fracture, haemarthrosis, traumatic bursitis
- Rapid (hours) with fever → Septic bursitis / septic arthritis ⚠️
- Gradual, progressive → Rheumatoid arthritis, chronic bursitis, gout, OA, tumour
- Recurrent episodes → Gout (most common cause of recurrent acute joint swelling)
Duration — days / weeks / months / years
Character of Swelling
- Soft, fluctuant → Bursitis (fluid), effusion, ganglion
- Firm/hard → Tophus, rheumatoid nodule, osteochondroma
- Progressive enlargement + hard → Soft tissue tumour / bone tumour ⚠️ Red flag
Associated Symptoms
- Pain: Constant vs activity-related; severity (VAS 1–10); radiation
- Redness / warmth → Septic, crystal arthropathy
- Morning stiffness >1 hour → Rheumatoid arthritis
- Stiffness worsening with activity → Osteoarthritis
- Fever, chills → Septic process ⚠️
- Restricted movement → Fracture, septic arthritis, severe effusion
- Numbness/tingling in ring & little fingers → Ulnar nerve involvement (cubital tunnel syndrome)
- Locking / clicking → Loose body (osteochondritis dissecans)
- Skin wounds, abrasions over the swelling → Portal of entry for septic bursitis
Relieving / Aggravating Factors
- Worse with extension pressure (leaning on elbow) → Bursitis
- Worse with wrist extension against resistance → Lateral epicondylitis (tennis elbow)
- Worse with wrist flexion → Medial epicondylitis (golfer's elbow)
Past History
- Previous similar episodes (recurrent gout, RA flares)
- Prior trauma to the same elbow
- Previous surgery or aspiration of the swelling
- Tuberculosis (TB) — ask specifically for septic/monoarthritis differential
Medical History
- Gout / hyperuricaemia
- Rheumatoid arthritis, SLE, psoriasis
- Diabetes mellitus ⚠️ (risk factor for septic bursitis)
- Chronic renal failure, dialysis patients (gout + RA associations)
- Alcohol abuse (gout, septic risk)
- Haemophilia (haemarthrosis)
- Malignancy (metastatic swelling, immunocompromise)
- Immunosuppression (steroid use, chemotherapy)
Drug History
- Corticosteroids → predispose to infection, tendon rupture
- Fluoroquinolones → tendinopathy
- Diuretics → precipitate gout
- Allopurinol / urate-lowering therapy — already on treatment?
- NSAIDs — on regular use?
Family History
- Gout (strong hereditary component)
- Rheumatoid arthritis
- Haemophilia
Occupational & Social History
- ⚠️ Key question: Repetitive elbow trauma at work (gardening, plumbing, mining, manual labour) → olecranon bursitis
- Sports (tennis, golf, throwing sports)
- Alcohol intake (gout risk)
SECTION 2: PHYSICAL EXAMINATION
General Examination
- Build, nutrition, pallor, icterus, cyanosis, clubbing, lymphadenopathy, oedema
- Temperature (fever → septic process)
- Other joint involvement (polyarthritis → RA, gout, psoriatic)
- Skin: tophi elsewhere (ear pinnae, finger joints), rheumatoid nodules, psoriatic plaques, cellulitis
LOCAL EXAMINATION — Elbow
LOOK (Inspection)
| Parameter | What to Note |
|---|---|
| Position of arm | Carried at side vs flexed (flexion relieves pain in effusion) |
| Skin colour | Erythema → septic/crystal; normal skin → chronic bursitis/RA |
| Swelling site | Posterior (olecranon) vs diffuse (whole joint effusion) |
| Skin changes | Abrasions, sinuses, scars, skin thinning, pustules (portal of entry) |
| Muscle wasting | Disuse atrophy → chronic disease |
| Carrying angle (valgus) | Normal: 5–10° male, 10–15° female |
| Cubitus varus/valgus | Post-traumatic deformity |
| Visible tophi | Chalky white deposits (tophaceous gout) |
FEEL (Palpation)
| Parameter | Technique & Significance |
|---|---|
| Temperature | Back of hand — warmth = active inflammation |
| Tenderness | Point tenderness over olecranon, lateral epicondyle, medial epicondyle |
| Swelling consistency | Soft/fluctuant → fluid; firm → nodule/tophus; hard → bony/calcified |
| Fluctuation | Using two fingers — confirm fluid-filled bursa |
| Transillumination | Ganglion transilluminates; solid tumour does not |
| Boundaries | Well-defined → bursitis, ganglion; ill-defined → malignancy ⚠️ |
| Skin pinchability | Can skin be lifted over swelling? No → adherent to underlying structure (malignancy) |
| Posterolateral / posteromedial triangles | Palpate fat pads — fullness = joint effusion |
| Lateral epicondyle | Tenderness → tennis elbow |
| Medial epicondyle | Tenderness → golfer's elbow; check ulnar nerve in cubital groove |
| Ulnar nerve | Thickening at cubital tunnel? |
| Regional lymph nodes | Epitrochlear, axillary — enlargement suggests infection/malignancy |
MOVE (Range of Motion)
| Movement | Normal Range | Notes |
|---|---|---|
| Flexion | 0–145° | Limited in effusion, RA, OA |
| Extension | 0° (full extension) | Loss of extension = early effusion sign |
| Pronation | 0–85° | Involves proximal radioulnar joint |
| Supination | 0–90° |
⚠️ Key point: In olecranon bursitis, passive ROM at the elbow is relatively preserved and painless, except at full flexion (which compresses the inflamed bursa). This distinguishes bursitis from septic arthritis where all movements are painful.
Special Tests
| Test | Condition |
|---|---|
| Mill's test (resisted wrist extension) | Lateral epicondylitis (tennis elbow) |
| Cozen's test | Lateral epicondylitis |
| Golfer's elbow test (resisted wrist flexion) | Medial epicondylitis |
| Tinel's sign at cubital tunnel | Cubital tunnel syndrome |
| Elbow flexion test | Cubital tunnel compression (tingling in ulnar distribution after 1 min) |
| Valgus stress test | Medial collateral ligament integrity |
| Varus stress test | Lateral collateral ligament integrity |
Neurovascular Examination
- Radial pulse (distal)
- Median nerve: Thenar wasting, grip strength, palmar sensation
- Ulnar nerve: Interossei, hypothenar, ring/little finger sensation
- Radial nerve: Wrist/finger extension, dorsal hand sensation
SECTION 3: DIFFERENTIAL DIAGNOSIS OF ELBOW SWELLING
| Diagnosis | Key Features |
|---|---|
| Olecranon bursitis (most common) | Posterior swelling, fluctuant, ROM mostly preserved, no joint pain |
| Septic bursitis | Rapid onset, fever, erythema, warmth, skin portal of entry, WBC >10,000/mm³ in fluid |
| Septic arthritis | ⚠️ Hot swollen joint = septic until proven otherwise; all movements painful |
| Gouty bursitis/arthritis | Recurrent attacks, hyperuricaemia, tophi, crystals in fluid |
| Rheumatoid arthritis | Polyarthritis, morning stiffness >1hr, RA nodules, RF/anti-CCP positive |
| Osteoarthritis | Older age, stiffness worsens with use, reduced ROM, osteophytes on X-ray |
| Haemarthrosis | After trauma, rapid diffuse swelling, coagulopathy/trauma history |
| Fracture/dislocation | Significant trauma, bony deformity, crepitus |
| Osteochondritis dissecans | Young patients, locking, clicking, loose body |
| Ganglion cyst | Transilluminates, not fixed to deep structure |
| Lipoma | Soft, lobulated, non-tender, no joint communication |
| Soft tissue sarcoma | ⚠️ Progressive firm painless swelling, fixed, >5 cm, night pain |
SECTION 4: INVESTIGATIONS
Bedside / Bursal Fluid Aspiration (Most Important!)
Aspirate if septic bursitis is suspected — diagnostic AND therapeutic
| Fluid Parameter | Septic | Non-Septic/Traumatic | Crystal-Induced |
|---|---|---|---|
| Appearance | Purulent/serosanguineous | Straw-coloured/bloody | Straw-coloured to bloody |
| WBC/mm³ | >3,000 (mean ~54,000) | <1,000–2,000 | 1,000–6,000 |
| PMN | >50% | Predominantly mononuclear | Variable |
| Glucose (bursal:serum) | <50% (90% of cases) | >50% | Unknown |
| Gram stain | Positive in 70% | Negative | Negative |
| Culture | Positive | Negative | Negative |
| Crystals | Absent* | Absent | Present (urate = needle-shaped negative birefringent; CPPD = rhomboid positive birefringent) |
*Crystals do not rule out concurrent infection
Blood Investigations
- CBC with differential (leucocytosis in septic)
- ESR, CRP (acute phase reactants)
- Serum uric acid (gout — but may be normal during acute attack!)
- Blood culture (if fever/systemic sepsis)
- RF, anti-CCP (rheumatoid arthritis)
- HLA-B27 (spondyloarthropathy)
- Serum calcium, ALP (metabolic bone)
- Blood glucose (if diabetic)
Imaging
- X-ray elbow (AP + lateral): Bony erosions (RA, gout), calcifications, fractures, osteophytes (OA), joint space narrowing, soft tissue shadow
- Ultrasound: Best for bursal fluid, extent, guided aspiration; detect lipoma, ganglion
- MRI: Soft tissue tumour characterisation, ligament/tendon integrity, marrow involvement
- CT scan: Bony detail, suspected tumour extent
SECTION 5: TREATMENT PRINCIPLES
Non-Infective Olecranon Bursitis
- Rest, compression bandage, ice packs
- NSAIDs (ibuprofen, diclofenac)
- Avoid inciting activity (no leaning on elbow)
- Aspiration (therapeutic) if large and symptomatic
- Intra-bursal corticosteroid injection (only after infection excluded)
Septic Bursitis
- Aspiration — drain all fluid; send for culture
- Antibiotics: Cover Staphylococcus + Streptococcus + MRSA
- Outpatient: TMP-SMX DS BD or Doxycycline 100 mg BD × 10–14 days
- Inpatient: IV Vancomycin 15–20 mg/kg ± piperacillin/tazobactam
- Follow up at 24–48 hours to check culture results and response
- Bursectomy if refractory to aspiration + antibiotics
- ⚠️ Indications for admission: Systemic sepsis, extensive cellulitis, immunocompromise, failure of outpatient treatment, suspected joint involvement
Gout
- Acute: NSAIDs, colchicine, corticosteroids
- Chronic: Allopurinol (urate-lowering), lifestyle modification, hydration
Rheumatoid Arthritis
- DMARDs (methotrexate first-line), biologics; orthopaedic referral for synovectomy/reconstruction
⭐ IMPORTANT POINTS TO REMEMBER (Exam Keys)
-
Olecranon bursitis is the most common cause of posterior elbow swelling — the olecranon bursa is the only bursa of the elbow joint and is most vulnerable to isolated pathology.
-
⚠️ Hot swollen joint = septic arthritis until proven otherwise — this is a surgical emergency requiring urgent aspiration.
-
Bursitis vs Septic Arthritis distinction:
- Bursitis: ROM relatively preserved, pain only at full flexion (bursa compression)
- Septic arthritis: ALL movements painful, generalised joint swelling, fever
-
Occupational history is critical — repetitive elbow trauma (gardening, plumbing, mining) is the most common cause of olecranon bursitis.
-
Bursal fluid WBC cutoffs: <1,000 → traumatic/non-septic; >3,000 (mean ~54,000) → septic; 1,000–6,000 → crystal-induced.
-
Serum uric acid can be NORMAL during an acute gout attack — do not rule out gout based on a normal uric acid level.
-
Skin integrity over the bursa must be checked — abrasions/lacerations are the portal of entry for septic bursitis.
-
Crystal types: Gout = needle-shaped, negatively birefringent monosodium urate; CPPD = rhomboid, positively birefringent calcium pyrophosphate.
-
Red flags for malignancy: Progressive painless firm swelling >5 cm, fixed to deep structures, night pain, skin not pinchable → urgent MRI + biopsy.
-
Always examine joint above (shoulder) and below (wrist) to complete the elbow examination — cubital tunnel/ulnar nerve must be assessed with every elbow case.
-
Staphylococcus aureus accounts for the majority of septic bursitis infections (including increasing MRSA prevalence — adjust antibiotics per local sensitivities).
-
Rheumatoid nodules are firm, non-tender, found at pressure points (olecranon, sacrum) — can mimic bursitis clinically.
Sources: Tintinalli's Emergency Medicine, ROSEN's Emergency Medicine, Geeky Medics OSCE Framework, TeachMeSurgery Elbow Examination
This is a shared conversation. Sign in to Orris to start your own chat.