Atrophic rhinitis
Reading File
Finding Sources
Searching PubMed
"atrophic rhinitis"[MeSH Terms]
Reading File
Reading File
Finding Sources
Searching Images
atrophic rhinitis nasal mucosa crusting ozena
Reading File
Loading Image
I now have comprehensive content from three textbooks plus a clinical endoscopy image. Here is the full synthesis:
Atrophic Rhinitis
Synonyms: Rhinitis sicca, Ozena (advanced primary form)
Definition & Overview
Atrophic rhinitis is a chronic condition characterized by progressive atrophy of the nasal mucosa, submucosa, glands, turbinate bones, and neurovascular supply, leading to paradoxical nasal obstruction (the nasal cavity is actually spacious, but sensory function is lost). It occurs in primary and secondary forms.
Classification
Primary Atrophic Rhinitis
- Most prevalent in developing countries in subtropical and temperate climate zones
- Etiology is incompletely understood but bacterial colonization is strongly implicated:
- Klebsiella ozaenae (most characteristic)
- Staphylococcus aureus
- Proteus mirabilis
- Escherichia coli
- More common in young women; often begins at puberty
- More severe and progressive course
Secondary Atrophic Rhinitis
- More prevalent in developed countries; less severe and less progressive
- Causes include:
- Iatrogenic — excessive turbinate resection (sinonasal surgery), "empty nose syndrome"
- Granulomatous disease — GPA (Wegener's), sarcoidosis, leprosy
- Radiation therapy to the head and neck
- Cocaine abuse
- Autoimmune/systemic inflammatory disorders — SLE
- Rhinitis medicamentosa (a form of secondary atrophic rhinitis)
Note: Atrophic rhinitis is considered a distinct entity from "empty nose syndrome," which specifically refers to nasal obstruction following excessive turbinate tissue removal. — K.J. Lee's Essential Otolaryngology
Pathology & Histology
The nasal mucosa undergoes characteristic degenerative changes:
| Feature | Detail |
|---|---|
| Squamous metaplasia | Replacement of ciliated columnar epithelium |
| Glandular atrophy | Loss of seromucous glands → dryness |
| Endarteritis obliterans | Diffuse small-vessel obliteration → ischemia |
| Loss of mucociliary function | Stagnant secretions → crusting and infection |
| Turbinate and bone atrophy | Markedly spacious nasal cavities |
— K.J. Lee's Essential Otolaryngology
Clinical Features
Classic symptom triad of primary atrophic rhinitis (ozena):
- Foul smell (cacosmia/ozena) — perceived by others but often not by the patient due to anosmia
- Anosmia — progressive loss of smell
- Yellow-green nasal crusting — thick, adherent crusts throughout the nasal cavities
Additional symptoms:
- Paradoxical nasal obstruction/congestion (large empty cavity but abnormal airflow sensation)
- Nasal dryness
- Epistaxis (from friable mucosa)
- Headache
- Elderly patients are particularly prone to crusting and foul odor — Textbook of Family Medicine 9e
Endoscopic Appearance
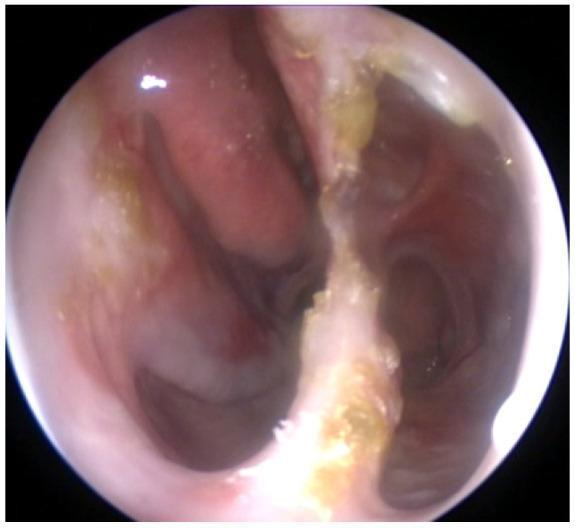
Nasal endoscopy: widely spacious nasal cavity with markedly atrophic, thin mucosa; nearly absent turbinates; and extensive yellow-gold and gray crusting adherent to septal remnants and posterior nasal walls — consistent with severe atrophic rhinitis.
Diagnosis
- Primarily clinical — history and anterior rhinoscopy/nasal endoscopy are usually sufficient
- Nasal endoscopy: wide nasal cavities, atrophic turbinates, crusting
- Bacterial culture: identify causative organisms for targeted antibiotic therapy
- If etiology unclear → biopsy to exclude granulomatous disease, malignancy
- CT sinuses: assess degree of turbinate and bony atrophy — Textbook of Family Medicine 9e
- Serology (c-ANCA, ANA, ACE) if systemic disease suspected
Management
The Cochrane Collaboration has found insufficient evidence for any single consistently effective treatment, so management is largely supportive. — Textbook of Family Medicine 9e
Medical (Conservative)
| Treatment | Rationale |
|---|---|
| Nasal saline irrigation | Removes crusts, moisturizes mucosa; first-line |
| Saline + aloe vera / oil combinations | Additional moisturization |
| Culture-directed topical antibiotics | Target specific colonizing organisms |
| Systemic antibiotics | Rifampicin, ampicillin, or ciprofloxacin for K. ozaenae |
| Glucose-glycerine nasal spray | Inhibits bacterial growth |
| Estrogen nasal drops | May stimulate mucosal regeneration (limited evidence) |
| Vitamins (A, D) | Support mucosal integrity |
Surgical
- Surgery to reduce nasal cavity size — paradoxical; reducing the spacious cavity improves mucociliary function and airflow sensation
- Submucosal implants (cartilage, bone, Teflon)
- Young's operation — surgical closure of one or both nostrils (temporary or permanent)
- Autologous lipoaspirate transfer and platelet-rich plasma — newer regenerative approaches (Cummings Otolaryngology)
- For secondary causes: address underlying pathology (treat GPA, stop cocaine, manage systemic disease)
Summary Table
| Feature | Primary | Secondary |
|---|---|---|
| Geography | Developing countries | Developed countries |
| Severity | More severe, progressive | Less severe |
| Causes | K. ozaenae, idiopathic | Surgery, radiation, drugs, granulomatous disease |
| Bacteria | K. ozaenae, S. aureus, Proteus, E. coli | Secondary colonizers |
| Key histology | Squamous metaplasia, endarteritis obliterans | Same but less marked |
Sources:
- Cummings Otolaryngology Head and Neck Surgery
- K.J. Lee's Essential Otolaryngology
- Textbook of Family Medicine, 9th Edition
This is a shared conversation. Sign in to Orris to start your own chat.