I have to make a detailed notes on ABVS , slgive me a detailed note , which i can write in exam, add as much as detail you know like definition, history background, indications , instrumentation, technical parameters , patient positioning techniques, modes of display , analysis, application etc.
Checking Date & Time
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching PubMed
automated breast volume scanner ABVS
Reading Article
Reading Article
Reading Article
Searching the Web
ABVS automated breast volume scanner detailed review indications technique parameters coronal plane
Searching PubMed
ABVS breast ultrasound coronal reconstruction three-dimensional
Finding Sources
Reading File
Reading Article
Searching PubMed
ABVS breast ultrasound sensitivity specificity dense breast screening
Searching Images
automated breast volume scanner ABVS coronal plane ultrasound
Loading Image
Loading Image
I now have all the information needed. Here are the comprehensive exam notes:
AUTOMATED BREAST VOLUME SCANNER (ABVS)
Comprehensive Exam Notes
1. DEFINITION
Automated Breast Volume Scanner (ABVS) is a high-end, three-dimensional (3D) ultrasound imaging system that uses a wide-footprint, motorized transducer to automatically sweep across the entire breast in a single standardized acquisition, generating volumetric datasets that can be reconstructed in coronal, transverse, and sagittal planes — including the coronal (en face) plane, which is unique to this technology and not obtainable by conventional hand-held ultrasound (HHUS).
Also known as: Automated Breast Ultrasound System (ABUS) or Whole Breast Automated Ultrasound (WBUS)
The landmark commercial system is the Siemens ACUSON S2000 ABVS, FDA-cleared in 2012 for supplemental screening in women with dense breasts.
2. HISTORICAL BACKGROUND
| Year | Milestone |
|---|---|
| 1950s–1970s | Early automated breast ultrasound (ABUS) attempts — low-frequency transducers, water bath coupling; poor sensitivity for small solid lesions |
| 1970s–1980s | Prototype systems used patients in prone position with breast immersed in water; uncomfortable and impractical for clinical use |
| 2000s | Technological advances: high-frequency transducers (5–14 MHz), digital image processing, 3D workstations |
| 2008–2009 | Siemens develops the modern ABVS system with flexible robotic arm, high-resolution transducer, prone-position scanning |
| 2010 | First major clinical publications; Wöhrle et al. describe technical parameters and clinical utility (Der Radiologe, 2010) |
| 2012 | FDA clearance for ABVS as supplemental screening modality in women with dense breasts |
| 2015 | Meta-analysis (Meng et al., Eur Radiol) — pooled sensitivity 92%, specificity 84.9% |
| 2019–2025 | Growing evidence for use in screening dense breasts, AI integration, photoacoustic hybrid systems |
Key driver: Dense breast tissue (ACR BI-RADS category C/D) reduces mammographic sensitivity from ~85% to ~30–50%. ABVS was developed as a non-operator-dependent, reproducible supplemental screening tool.
3. INDICATIONS
Primary Indications
- Supplemental screening in women with dense breast tissue (ACR BI-RADS density C or D) — most important indication
- Characterization of breast lesions detected on mammography or HHUS
- Preoperative assessment — accurate lesion extent measurement for surgical planning
- Monitoring response to neoadjuvant chemotherapy
- Post-treatment follow-up after breast-conserving surgery (BCS)
- High-risk screening — BRCA mutation carriers, family history, prior chest radiation
- Difficult-to-examine breasts — large breasts where HHUS coverage is incomplete
Additional/Extended Indications
- Evaluation of multi-focal/multi-centric disease
- Screening in younger women (<40 years) where radiation exposure from mammography is a concern
- Novel application: soft tissue tumor evaluation beyond the breast (Chen et al., 2015)
Contraindications / Limitations
- Open wounds or skin lesions over the breast
- Patients unable to maintain prone position
- Very small breasts (may not achieve adequate coupling)
- Not suitable as a standalone diagnostic tool — requires correlation with mammography/HHUS
4. INSTRUMENTATION
System Components (Siemens ACUSON S2000 ABVS)
A. Transducer
- Type: Wide-aperture (15.4 cm footprint), linear array transducer
- Frequency range: 5–14 MHz (high-frequency, broad bandwidth)
- Footprint: ~15 cm × 17 cm — much wider than HHUS transducers
- Contains hundreds of piezoelectric elements arranged in a linear array
B. Motorized Scanning Unit
- A flexible robotic arm holds the transducer
- Automated, motorized sweep mechanism moves the transducer across the breast at a constant, controlled speed
- Eliminates operator-dependent variability in angulation and pressure
C. Coupling Pad / Membrane
- A soft silicon membrane (coupling pad) is pre-filled with aqueous gel
- Conforms to breast contour, providing uniform acoustic coupling
- Ensures consistent stand-off distance across the entire breast surface
D. Touchscreen Interface
- Controls scan parameters, breast size selection, scan position
- Allows marking of breast position (LCC, LML, LMLO equivalent orientations)
E. 3D Workstation
- High-performance workstation with dedicated post-processing software
- Reconstructs 3D volume from raw data
- Generates multiplanar reconstructions (MPR) in all three planes
- Allows scrolling through volumetric dataset slice by slice
- Integrated with PACS for image storage and reporting
5. TECHNICAL PARAMETERS
| Parameter | Specification |
|---|---|
| Transducer frequency | 5–14 MHz |
| Transducer footprint | ~15 cm width |
| Scan depth | Up to 6 cm (adjustable per breast size) |
| Acquisition time per position | ~60–90 seconds |
| Slice thickness (coronal) | 0.5–2 mm |
| Volume dataset | 3D volumetric dataset (hundreds of image slices) |
| Frame rate | Continuous during automated sweep |
| Spatial resolution | ~0.3–0.5 mm in-plane |
Presettings Based on Breast Size
The system provides size-based presettings (small / medium / large / extra-large) that automatically adjust:
- Scan depth
- Focus zones
- Gain curves
- Number of scan positions required
Coupling Medium
- Aqueous gel inside a flexible silicon membrane pad
- Alternative: direct gel application + membrane
6. PATIENT POSITIONING TECHNIQUES
Standard Prone Position Protocol
- Patient lies prone on a dedicated examination table with a breast aperture (hole in the table through which the breast hangs freely)
- The affected breast hangs dependently through the aperture
- The ABVS transducer (with coupling pad) is applied to the inferior surface of the breast from below
- The motorized arm performs the automated sweep
This prone position ensures the breast is pendulous, maximally uncompressed, and well-separated from the chest wall — unlike the supine position used in HHUS.
Standard Scan Positions (3 scans per breast for complete coverage)
Most protocols use 3 acquisitions per breast:
| Scan Position | Coverage Area |
|---|---|
| Anterior (central) | Nipple-areolar complex, central breast |
| Lateral | Outer/lateral quadrants (upper outer + lower outer) |
| Medial | Inner/medial quadrants (upper inner + lower inner) |
- For large breasts, 4–5 acquisitions may be needed
- The axilla/tail of Spence may require an additional dedicated scan
- Each scan takes ~90 seconds; total examination = ~10–15 minutes per breast
Positioning Variants
- Some protocols allow supine/semi-supine positioning with modified transducer application (used in certain commercial ABUS systems)
- Nipple must be marked to serve as an anatomical reference for MPR alignment
Patient Preparation
- No special preparation required
- Inform patient about prone positioning and mild transducer pressure
- Gel application to membrane or breast surface
7. MODES OF DISPLAY (Multiplanar Reconstruction — MPR)
ABVS generates a 3D volumetric dataset that is displayed in three orthogonal planes simultaneously on the workstation:
A. Transverse (Axial) Plane
- Standard 2D cross-sectional view (equivalent to HHUS B-mode)
- Shows lesion shape, echogenicity, margins in the horizontal plane
- Familiar to sonographers accustomed to HHUS
B. Sagittal Plane
- Vertical cross-section from superior to inferior
- Complements the transverse plane for lesion characterization
C. Coronal Plane ⭐ (UNIQUE to ABVS — Most Important)
- En face view of the breast from front to back
- Cannot be obtained by HHUS
- Shows the entire breast parenchymal architecture in one plane
- Allows visualization of lesion relationship to entire breast and chest wall
- Shows Cooper's ligaments converging toward the nipple ("convergence sign")
Key Coronal Plane Signs:
| Sign | Description | Significance |
|---|---|---|
| Retraction phenomenon / Sunburst sign | Spiculations radiating outward from a central hypoehoic mass, pulling Cooper's ligaments inward | Highly specific for malignancy |
| Convergence sign | Normal radiating pattern of Cooper's ligaments converging toward the nipple | Normal finding |
| White-wall sign | Hyperechoic rim in the coronal plane corresponding to posterior acoustic enhancement | Seen in cysts / high-grade carcinoma |
| Nipple shadowing artifact | Dark shadow behind nipple in coronal plane — can mimic architectural distortion | False positive — correlate with HHUS |
D. Volume Rendering / 3D Rendering Mode
- Produces a rendered 3D image of the breast volume
- Useful for surgical planning and lesion localization
- Less used in routine diagnosis
8. ANALYSIS — LESION CHARACTERIZATION
BI-RADS Descriptors Used with ABVS
ABVS findings are classified using the ACR BI-RADS (Breast Imaging Reporting and Data System) lexicon, as with HHUS.
Key Sonographic Features Assessed
Shape
- Oval / Round → Benign
- Irregular → Suspicious
Margins
- Circumscribed → Benign
- Spiculated / Angular / Microlobulated → Malignant
- Spiculated + stellate margin in coronal plane → High specificity for malignancy (Wang et al., 2012)
Orientation
- Parallel (wider-than-tall) → Benign
- Non-parallel (taller-than-wide) → Suspicious
Echogenicity
- Hyperechoic → Benign (lipoma, fat necrosis)
- Hypoechoic → Requires evaluation
- Anechoic → Cyst (if with posterior enhancement)
- Complex / Heterogeneous → Worrisome
Posterior Acoustic Features
- Enhancement → Cysts, high-grade tumors
- Shadowing → Fibrosis, malignancy
- No change → Indeterminate
Coronal Plane Specific Analysis
- Presence/absence of retraction phenomenon — single most important ABVS-specific feature
- Assessment of architectural distortion in the en face view
- Relationship of lesion to nipple, skin, chest wall
Measurement
- ABVS allows 3D volumetric measurement of lesion in all three planes simultaneously
- More accurate than 2D HHUS for preoperative extent assessment (Tozaki & Fukuma, 2010)
9. COMPARISON: ABVS vs. HAND-HELD ULTRASOUND (HHUS)
| Feature | ABVS | HHUS |
|---|---|---|
| Operator dependency | Low (automated) | High (operator-dependent) |
| Reproducibility | High | Variable |
| Coronal plane imaging | Yes (unique) | No |
| 3D volumetric data | Yes | No (unless special probes) |
| Scan time | ~15 min/breast | ~10 min/breast |
| Real-time imaging | No | Yes |
| Spatial resolution (small lesions) | Slightly lower than HHUS | Slightly higher |
| Lesion characterization | Good | Slightly better (real-time) |
| Reproducibility for follow-up | Excellent | Poor |
| Sensitivity (vs mammography) | Higher (similar to HHUS) | Similar to ABVS |
| Patient comfort | Good (prone) | Good (supine) |
| Cost | Higher | Lower |
Wang et al. (2012): Detection rate and diagnostic accuracy were similar between ABVS and HHUS, but both were significantly superior to mammography in dense breasts.
10. PERFORMANCE METRICS (Evidence-Based)
From Meng et al. meta-analysis (Eur Radiol, 2015) — 13 studies:
| Metric | Value (95% CI) |
|---|---|
| Sensitivity | 92% (89.9–93.8%) |
| Specificity | 84.9% (82.4–87.0%) |
| Positive Likelihood Ratio | 6.17 (4.36–8.73) |
| Negative Likelihood Ratio | 0.101 (0.075–0.136) |
| Diagnostic Odds Ratio | 72.2 (39.6–131.6) |
Combined modality (ABVS + HHUS + Mammography): Sensitivity 97.1%, Specificity 95.2%, Accuracy 96.4%
11. ADVANTAGES OF ABVS
- Operator independence — results are not dependent on sonographer skill/experience
- Standardized, reproducible images — ideal for serial monitoring
- Coronal plane — unique en face visualization unavailable with HHUS
- 3D volumetric assessment — accurate lesion size/extent measurement
- Complete breast coverage — standardized full-volume acquisition
- No ionizing radiation — safer than mammography/CT for repeated use
- Shorter per-patient time than HHUS for screening large populations
- Better documentation — complete archived volume for retrospective review
- Surgical planning — coronal view aids localization relative to Cooper's ligaments, chest wall
- Telemedicine compatibility — stored volumes can be read remotely
12. LIMITATIONS / DISADVANTAGES
- No real-time imaging — cannot perform dynamic maneuvers (compression, color Doppler during scan)
- No Doppler during acquisition — vascular information not captured in automated sweep
- Nipple shadowing artifact in coronal plane — can mimic architectural distortion (false positive)
- Acoustic shadowing from ribs/chest wall — limits posterior visualization
- Learning curve for coronal plane interpretation — radiologists unfamiliar with en face view
- High initial cost of equipment and workstation
- Longer reading time — large volumetric datasets take more time to review
- Not real-time — cannot guide biopsies directly (biopsy still requires HHUS)
- Positioning challenges for patients unable to lie prone
- Limited axillary coverage — tail of Spence may need additional scan position
- Inter-rater reliability — published studies show heterogeneous quality; more standardization needed
13. ARTIFACTS IN ABVS
| Artifact | Cause | Appearance | Significance |
|---|---|---|---|
| Nipple shadow | Acoustic shadowing from nipple | Dark vertical band on coronal view | Common false positive |
| Rib shadow | Acoustic block from ribs | Dark bands posteriorly | Limits deep tissue evaluation |
| Coupling artifact | Air trapped under membrane | Echo-poor area at skin surface | Technique error — rescan |
| Motion artifact | Patient movement during acquisition | Blurring of image planes | Repeat acquisition needed |
| Reverberation | Skin/membrane interfaces | Parallel bright lines near surface | Near-field artifact |
14. CLINICAL APPLICATIONS
A. Breast Cancer Screening
- Primary role: Supplemental screening in dense breasts (BI-RADS C/D)
- Detects mammographically occult cancers — especially in dense glandular tissue
- Particularly valuable for invasive lobular carcinoma (ILC) — which is notoriously difficult to detect on mammography
B. Lesion Characterization
- Distinguishes benign vs malignant based on BI-RADS descriptors
- Retraction phenomenon in coronal plane → highly specific for malignancy
- Cysts: white-wall sign in coronal plane
C. Preoperative Staging
- Accurate 3D measurement of tumor extent
- Assessment of multifocality/multicentricity
- Tumor-to-nipple distance measurement for surgical planning
D. Neoadjuvant Chemotherapy Monitoring
- Serial volumetric measurements for treatment response assessment
- Standardized, reproducible follow-up scans
E. Post-Treatment Surveillance
- Follow-up after BCS and radiation
- Detecting local recurrence
F. High-Risk Screening
- Complementary to MRI in BRCA mutation carriers
- Alternative when MRI is contraindicated (pacemaker, claustrophobia)
G. Novel Applications
- Soft tissue tumors outside the breast (Chen et al., 2015)
- Photoacoustic hybrid ABVS (PAUS-ABVS) — experimental, combining optical and acoustic imaging for functional information
15. REPORTING SYSTEM — BI-RADS INTEGRATION
ABVS findings are reported using the ACR BI-RADS lexicon:
| BI-RADS Category | Assessment | Management |
|---|---|---|
| 0 | Incomplete | Additional imaging |
| 1 | Negative | Routine screening |
| 2 | Benign | Routine screening |
| 3 | Probably benign | Short-interval follow-up (6 months) |
| 4 | Suspicious | Tissue sampling (biopsy) |
| 5 | Highly suggestive of malignancy | Biopsy |
| 6 | Known malignancy | Treatment planning |
16. IMAGES
Fig 1: ABVS Coronal Plane — Normal Convergence Sign
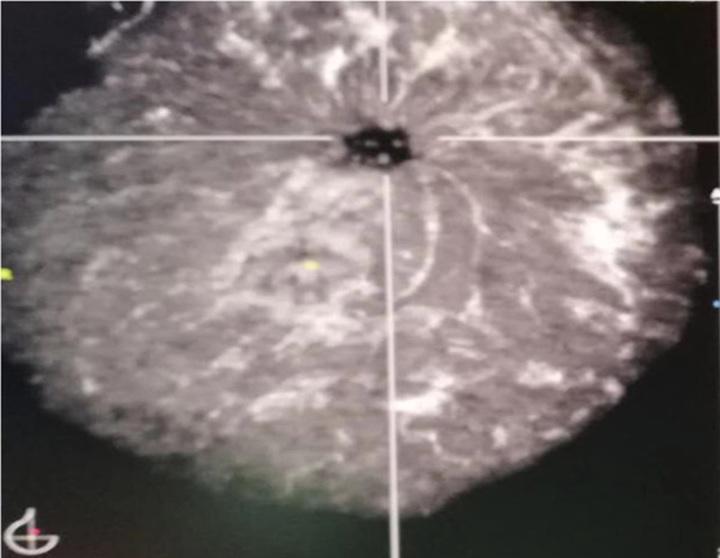 Normal coronal en face view: bright Cooper's ligaments radiate toward the central nipple — this normal "convergence sign" should not be mistaken for pathological retraction.
Normal coronal en face view: bright Cooper's ligaments radiate toward the central nipple — this normal "convergence sign" should not be mistaken for pathological retraction.

Fig 2: ABVS vs HHUS — Invasive Lobular Carcinoma
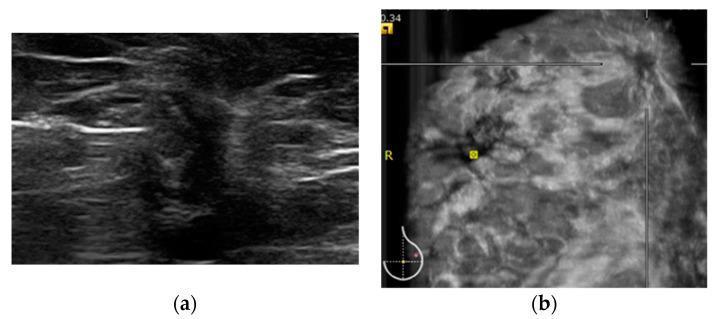 (a) HHUS transverse view: architectural distortion, hypoechoic area. (b) ABVS coronal view: classic "retraction phenomenon/sunburst sign" — Cooper's ligaments pulled inward toward the malignant focus, highly specific for invasive malignancy.
(a) HHUS transverse view: architectural distortion, hypoechoic area. (b) ABVS coronal view: classic "retraction phenomenon/sunburst sign" — Cooper's ligaments pulled inward toward the malignant focus, highly specific for invasive malignancy.

17. KEY EXAM POINTS TO REMEMBER
Mnemonic — ABVS = "A Beautiful View of the breast in 3D Space"
- ABVS uses a 15 cm wide-footprint transducer at 5–14 MHz
- Patient positioned prone (hanging breast through aperture)
- 3 scan positions per breast = complete coverage
- Coronal plane = unique feature, not available with HHUS
- Retraction phenomenon / Sunburst sign on coronal = specific for malignancy
- Nipple shadow = most common false positive artifact in coronal plane
- Meta-analysis sensitivity = 92%, specificity = 84.9%
- No real-time imaging — cannot guide biopsy directly
- FDA cleared 2012 for supplemental screening in dense breasts
- Combined with mammography + HHUS: accuracy reaches 96.4%
- BI-RADS classification applies as with conventional ultrasound
- Major advantage: operator independence and reproducibility
Sources: Meng Z et al., Eur Radiol 2015 [PMID 25916389] | Wang ZL et al., Radiol Med 2012 [PMID 22744341] | Wöhrle NK et al., Radiologe 2010 [PMID 20949253] | Xiao Y et al., Eur J Gynaecol Oncol 2017 [PMID 29953776] | Berek & Novak's Gynecology (whole-breast ultrasound screening context)
This is a shared conversation. Sign in to Orris to start your own chat.