Describe Fertilization and gametogenesis obg
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
I now have comprehensive content from both "The Developing Human" and "Langman's Medical Embryology" to provide a thorough, well-illustrated answer.
Gametogenesis and Fertilization
Sources: The Developing Human: Clinically Oriented Embryology; Langman's Medical Embryology
1. GAMETOGENESIS
Gametogenesis is the process of formation and development of specialized sex cells (gametes — spermatozoa and oocytes) from bipotential primordial germ cells (PGCs). Its primary purposes are:
- Reducing the chromosome number from diploid (46) to haploid (23) via meiosis
- Cytodifferentiation to prepare gametes for fertilization
Primordial Germ Cells (PGCs)
- Formed in the epiblast during the 2nd week; migrate through the primitive streak during gastrulation
- Move to the wall of the yolk sac, then migrate to the developing gonads (arriving by end of week 5)
- Mitotic divisions increase their number during migration and after gonadal arrival
- PGCs that stray from their migratory path may give rise to teratomas
Meiosis — The Core of Gametogenesis
Meiosis consists of two sequential divisions without an intervening DNA replication between them:
| Division | What Happens | Result |
|---|---|---|
| Meiosis I (Reduction division) | Homologous chromosomes pair in prophase, then segregate → crossing over occurs | Diploid → Haploid (46 → 23 double-chromatid chromosomes) |
| Meiosis II (Equatorial division) | Each double-chromatid chromosome splits → chromatids pulled to opposite poles | Similar to mitosis but in haploid cells |
Key functions of meiosis:
- Maintains constant chromosome number across generations
- Allows random assortment of maternal and paternal chromosomes
- Produces genetic recombination via crossing over ("shuffles the genes")
A. Spermatogenesis
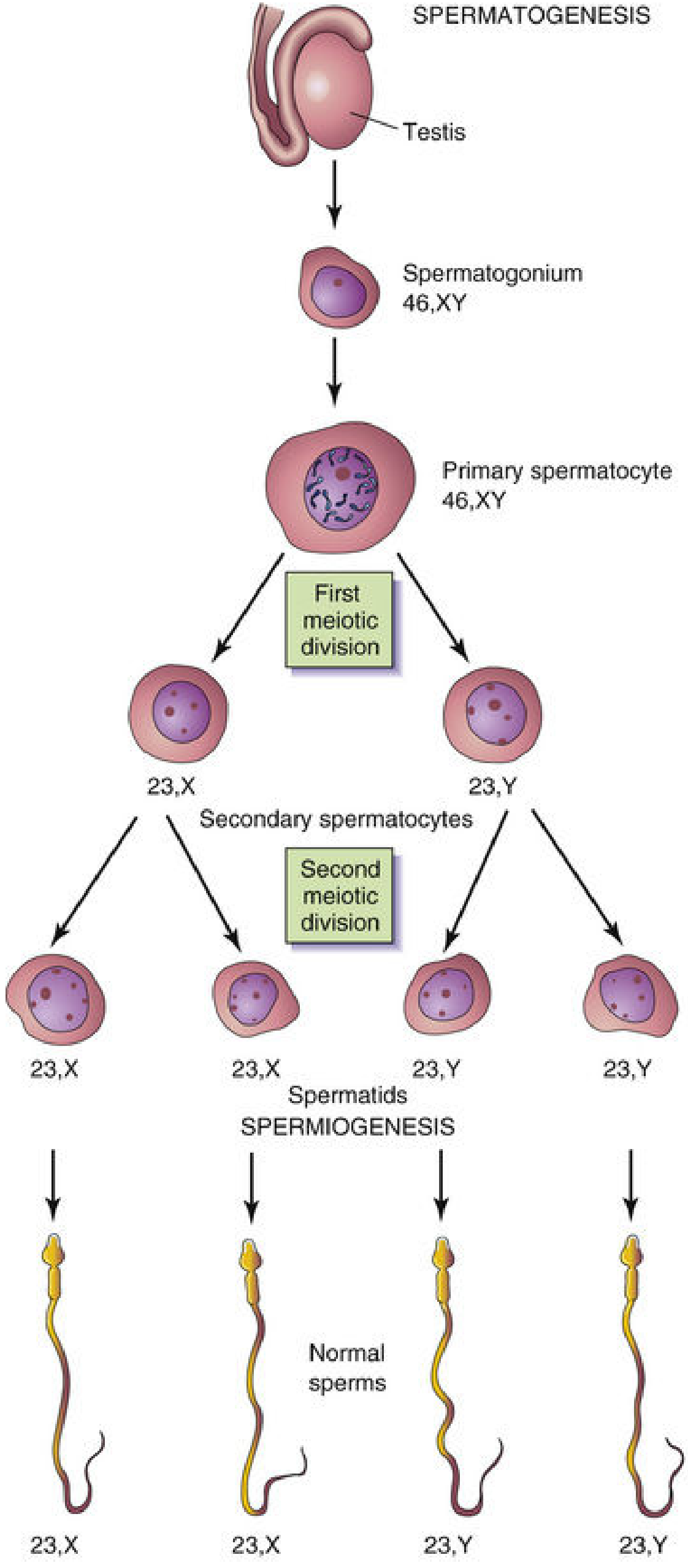
Spermatogenesis begins at puberty in the seminiferous tubules of the testes and continues throughout reproductive life.
| Stage | Chromosome Count | Notes |
|---|---|---|
| Spermatogonium | 46, XY | Diploid stem cell |
| Primary spermatocyte | 46, XY | Undergoes Meiosis I |
| Secondary spermatocyte | 23, X or 23, Y | Haploid; undergoes Meiosis II |
| Spermatid | 23, X or 23, Y | Haploid; undergoes spermiogenesis |
| Spermatozoon | 23, X or 23, Y | Mature sperm |
Key points:
- 1 primary spermatocyte → 4 spermatozoa (efficient cytoplasm division)
- Spermiogenesis = transformation of spermatids into spermatozoa (head, acrosome cap, flagellum development)
- Spermatogenesis is a continuous process from puberty onward
- ~10% of ejaculated sperm are morphologically abnormal but typically cannot pass through cervical mucus
B. Oogenesis
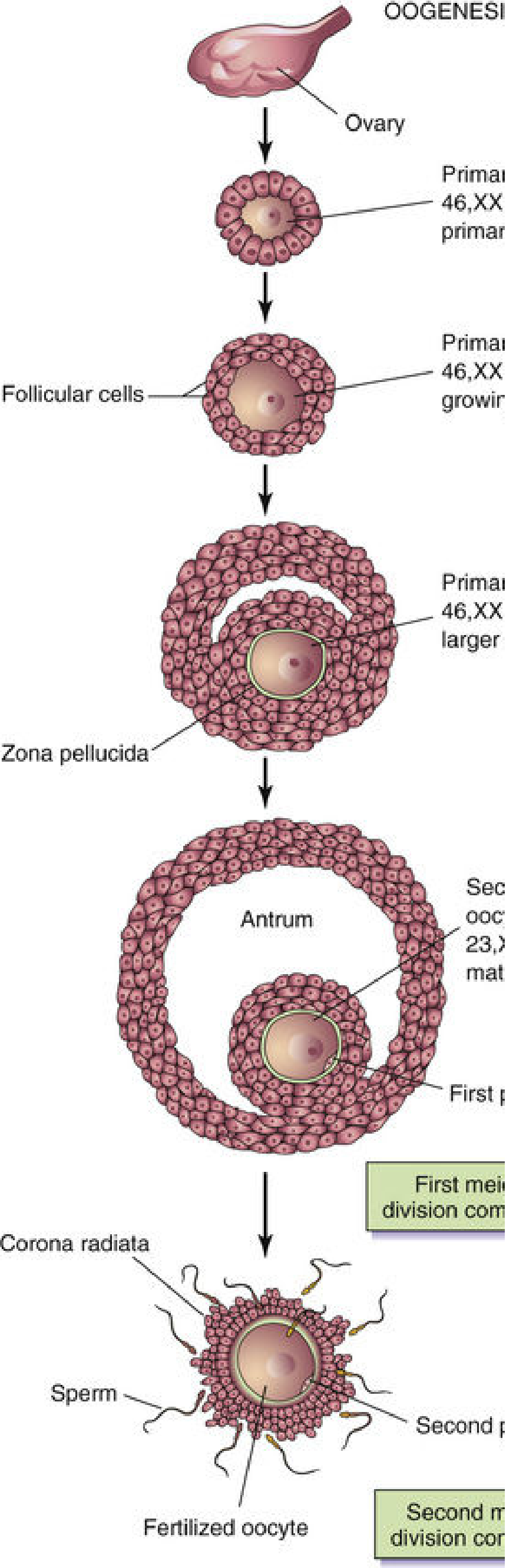
Oogenesis begins before birth and is unique in its arrest at two points during meiosis.
| Stage | When | Notes |
|---|---|---|
| Oogonia (mitosis) | Fetal life | Differentiate before birth into primary oocytes |
| Primary oocyte (46, XX) | Fetal life → birth → puberty | Arrested in prophase of Meiosis I (diplotene stage) — may remain for decades |
| Secondary oocyte (23, X) + 1st polar body | Just before ovulation (LH surge) | Meiosis I completes; oocyte arrested in Metaphase of Meiosis II |
| Mature oocyte (23, X) + 2nd polar body | Only if fertilization occurs | Meiosis II completes after sperm penetration |
Key distinctions from spermatogenesis:
| Feature | Spermatogenesis | Oogenesis |
|---|---|---|
| Yield per primary cell | 4 spermatids | 1 oocyte + 3 polar bodies |
| Cytoplasm conservation | Divided equally | Conserved in large oocyte; polar bodies are small/non-functional |
| Timing of meiosis | Continuous from puberty | Arrested twice; completes only with fertilization |
| Begin | Puberty | Fetal life |
C. Abnormal Gametogenesis
Nondisjunction — failure of homologous chromosomes (or chromatids) to separate during meiosis:
- Results in gametes with 24 chromosomes (trisomy if fertilized) or 22 chromosomes (monosomy if fertilized)
- Example: Trisomy 21 (Down syndrome) from an oocyte with 24 chromosomes
- Risk increases with maternal age (ideal reproductive age: 20–35 years)
- Advanced paternal age also increases the risk of de novo gene mutations
2. FERTILIZATION
Site
Fertilization normally occurs in the ampulla of the uterine tube (the widest portion, near the ovary). If the oocyte is not fertilized there, it passes to the uterus and degenerates (~12–24 hrs viability). Spermatozoa can remain viable in the female tract for several days.
Of 200–300 million sperm deposited in the vagina:
- Only ~1% enter the cervix
- Only 300–500 reach the site of fertilization
- Only 1 sperm fertilizes the egg
Prerequisites for Fertilization
Capacitation
A period of conditioning lasting ~7 hours in the female reproductive tract (primarily in the uterine tube epithelium):
- A glycoprotein coat and seminal plasma proteins are removed from the acrosomal region of the sperm plasma membrane
- Only capacitated sperm can penetrate corona cells and undergo the acrosome reaction
- "Racing to the ampulla" is not an advantage — the sperm must wait for capacitation to complete
Acrosome Reaction
Triggered by binding to the zona pellucida (ZP3 protein):
- Perforations form in the acrosome membrane
- Hydrolytic enzymes are released: acrosin (most important — proteolytic), esterase, neuraminidase, hyaluronidase
Phases of Fertilization
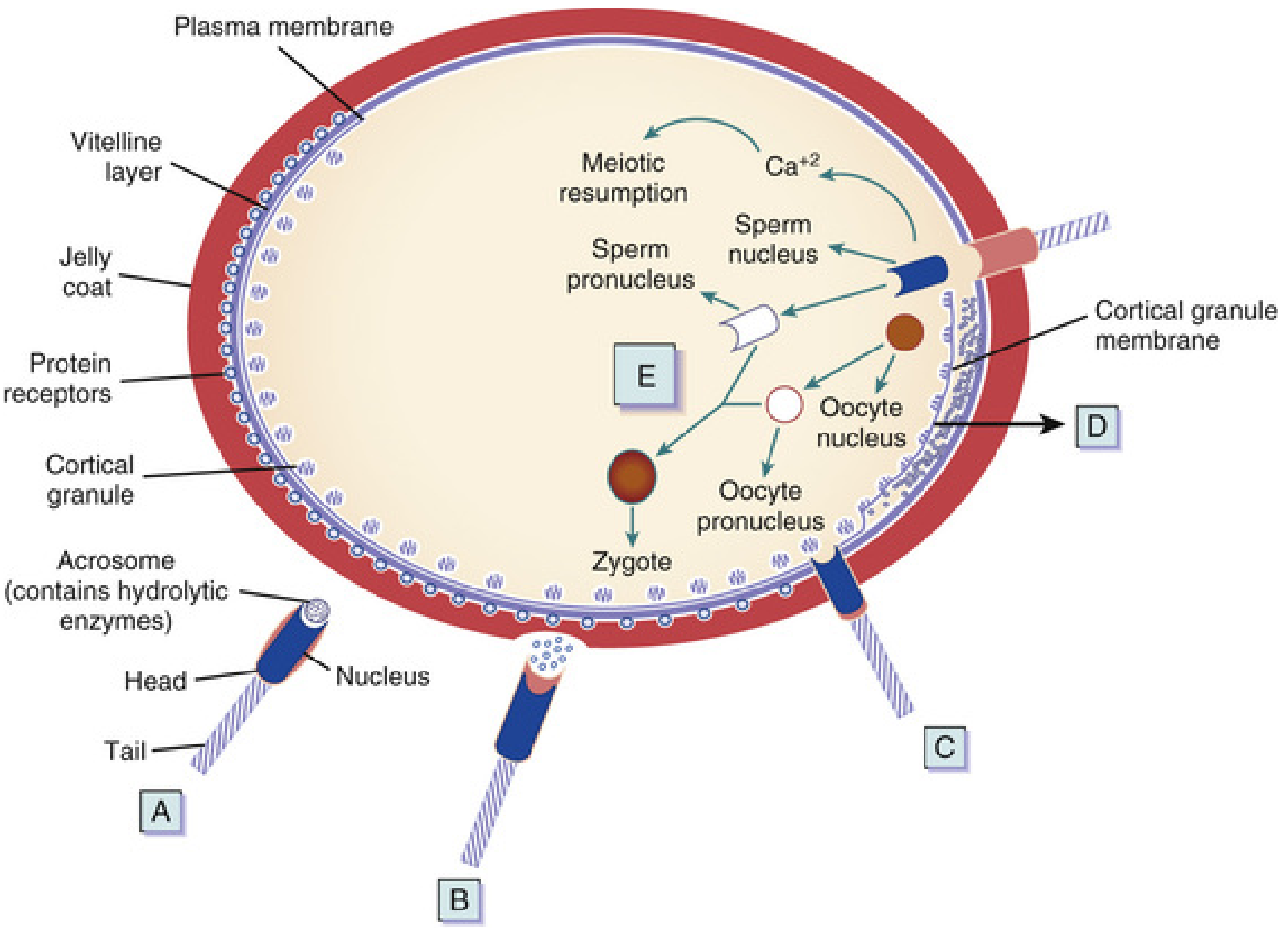
Phase 1 — Penetration of the Corona Radiata
- Capacitated sperm penetrate the surrounding follicular (corona) cells
- Aided by hyaluronidase from the acrosome and movements of the sperm tail
Phase 2 — Penetration of the Zona Pellucida
- The zona pellucida is a glycoprotein shell; sperm binds via SED1 protein → ZP3
- Acrosomal enzymes (chiefly acrosin) lyse a path through
- Once one sperm penetrates, the zona reaction occurs:
- Lysosomal enzymes from cortical granules are released into the perivitelline space
- ZP2 and ZP3 are digested → zona becomes impermeable to further sperm (block to polyspermy)
Phase 3 — Fusion of Oocyte and Sperm Cell Membranes
- Sperm proteins (IZUMO, ADAMs, CRISP1) bind oocyte receptors (Juno, integrins, CD9, CD81)
- The head and tail of the sperm enter the oocyte cytoplasm; the sperm's plasma membrane remains behind
- Phospholipase C-zeta from the sperm triggers a Ca²⁺ wave → reactivates cell cycling in the oocyte
Phase 4 — Completion of Meiosis II & Pronucleus Formation
- Sperm entry activates the oocyte to complete Meiosis II → mature oocyte + 2nd polar body
- The oocyte nucleus decondenses → female pronucleus (23, X)
- The sperm nucleus enlarges → male pronucleus (23, X or Y); sperm tail degenerates
- Both pronuclei replicate their DNA (1n, 2c)
- The oocyte at this stage is called an ootid
Phase 5 — Syngamy (Formation of the Zygote)
- The two pronuclei fuse into a single diploid (46 chromosomes) aggregation
- The ootid becomes a zygote — a unicellular embryo
- Chromosomes arrange on a cleavage spindle in preparation for the first mitotic division
Results of Fertilization
| Outcome | Significance |
|---|---|
| Restores diploid number (46 chromosomes) | Genetic continuity |
| Determines sex of embryo | Y-bearing sperm → male; X-bearing sperm → female |
| Initiates cleavage | Zygote undergoes rapid mitotic divisions |
| Creates unique genetic individual | New combination of maternal + paternal chromosomes |
| Completes oocyte meiosis | Second polar body expelled |
Post-Fertilization: Cleavage → Morula → Blastocyst
| Event | Timing | Details |
|---|---|---|
| 2-cell stage | ~30 hrs | First cleavage; blastomeres form |
| 4-cell stage | ~40 hrs | |
| Morula (16 cells) | ~3 days | Compaction → inner cell mass + outer cell mass; surrounded by zona pellucida |
| Blastocyst | ~4–5 days | Blastocele fluid accumulates; zona dissolves |
| Implantation | Day 6 | Trophoblast penetrates uterine epithelium via L-selectin |
- Inner cell mass (embryoblast) → tissues of the embryo proper
- Outer cell mass (trophoblast) → placenta
Clinical Correlates
| Condition | Mechanism |
|---|---|
| Ectopic pregnancy | Fertilization outside ampulla (or fertilized oocyte fails to reach uterus) |
| Down syndrome (Trisomy 21) | Nondisjunction during oogenesis → gamete with 24 chromosomes |
| Turner syndrome (45,X) | Nondisjunction → gamete with no sex chromosome |
| Teratoma | Strayed PGCs or epiblast pluripotent cells differentiate aberrantly |
| Male infertility (oligozoospermia/azoospermia) | Treated with ICSI (intracytoplasmic sperm injection) — associated with higher Y-chromosome deletion and birth defect risk |
| Polyspermy | Failure of cortical/zona reactions; results in non-viable embryo |
— The Developing Human: Clinically Oriented Embryology, pp. 75–125; Langman's Medical Embryology, pp. 34–62
This is a shared conversation. Sign in to Orris to start your own chat.