Esophageal candidiasis
Reading File
search_medical_text
esophageal candidiasis etiology diagnosis management treatment
search_medical_text
esophageal candidiasis endoscopy findings clinical features risk factors
search_medical_image
esophageal candidiasis endoscopy whitish plaques
GradeResponse
GradeResponse
GradeResponse
Esophageal Candidiasis
Esophageal candidiasis is an opportunistic fungal infection of the esophageal mucosa, most commonly caused by Candida albicans, though non-albicans species (C. glabrata, C. tropicalis, C. krusei, C. parapsilosis) are increasingly implicated, particularly in immunocompromised hosts.
Epidemiology & Risk Factors
| Category | Examples |
|---|---|
| HIV/AIDS | Most common cause; occurs when CD4 < 100–200 cells/µL |
| Hematologic malignancy | Leukemia, lymphoma, stem cell transplantation |
| Solid organ transplant | Immunosuppressive therapy |
| Prolonged corticosteroids | Systemic or inhaled (ICS) |
| Broad-spectrum antibiotics | Disruption of normal flora |
| Diabetes mellitus | Impaired host immunity |
| Esophageal dysmotility | Stasis promoting fungal overgrowth |
| Malnutrition / elderly | Reduced cellular immunity |
Clinical Presentation
- Odynophagia (painful swallowing) — hallmark symptom
- Dysphagia (difficulty swallowing, especially solids)
- Retrosternal chest pain or discomfort
- Nausea, reduced oral intake
- Oral thrush is present in ~50–70% of cases but its absence does not exclude esophageal involvement
- Rarely, patients may be asymptomatic (incidental endoscopic finding)
Diagnosis
Endoscopy (Gold Standard)
Endoscopic findings range from mild to severe:
- Early: Few small, raised white plaques on erythematous mucosa
- Advanced: Elevated confluent plaques (cottage-cheese-like) with underlying hyperemia and ulceration
The classic endoscopic appearance below is diagnostic in the appropriate clinical context:
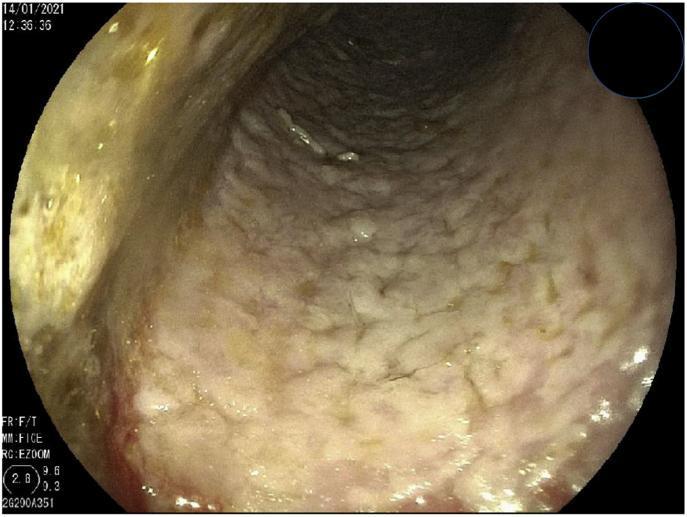
Barium Swallow
- Classic "cobblestone" or "shaggy" esophagus appearance (Prevention and Treatment of OIs in Children with HIV, p. 58)
Histopathology / Brushings
- KOH preparation, Gram stain, PAS stain: budding yeast with pseudohyphae
- Biopsy not always required if clinical/endoscopic picture is classic
- Endoscopy also rules out co-infections: HSV, CMV, Mycobacterium avium complex (Prevention and Treatment of OIs in Children with HIV, p. 58)
Grading (Kodsi Classification)
| Grade | Endoscopic Findings |
|---|---|
| I | Few raised white plaques ≤2 mm, no ulceration |
| II | Multiple raised white plaques >2 mm, no ulceration |
| III | Confluent linear/nodular plaques, hyperemia, ulceration |
| IV | Grade III + mucosal friability, narrowing of lumen |
Treatment
Per IDSA Management of Candidiasis Guidelines (p. 38):
First-Line
- Oral fluconazole 200–400 mg (3–6 mg/kg) daily × 14–21 days (strong recommendation; high-quality evidence)
- Systemic antifungal therapy is always required — topical therapy alone is insufficient
- A diagnostic trial of antifungal therapy is appropriate before endoscopy in the right clinical setting
If Unable to Tolerate Oral Therapy
- IV fluconazole 400 mg (6 mg/kg) daily, OR
- Echinocandin:
- Micafungin 150 mg/day
- Caspofungin 70 mg load → 50 mg/day
- Anidulafungin 200 mg/day
- De-escalate to oral fluconazole once oral intake is tolerated
Less Preferred Alternative
- Amphotericin B deoxycholate 0.3–0.7 mg/kg daily (moderate-quality evidence)
Fluconazole-Refractory Disease
| Agent | Dose |
|---|---|
| Itraconazole solution | 200 mg/day × 14–21 days |
| Voriconazole | 200 mg (3 mg/kg) PO/IV BID × 14–21 days |
| Echinocandin | (doses as above) × 14–21 days |
| AmB deoxycholate | 0.3–0.7 mg/kg/day × 21 days |
| Posaconazole (suspension) | 400 mg BID (weak recommendation) |
| Posaconazole ER tablets | 300 mg/day (weak recommendation) |
Recurrent/Chronic Esophagitis
- Suppressive therapy: Fluconazole 100–200 mg 3× weekly (strong recommendation; high-quality evidence)
Complications
- Esophageal stricture or narrowing (severe Grade IV disease)
- Fistula formation (rare)
- Fungemia / disseminated candidiasis (rare, primarily in severely immunocompromised or critically ill patients)
- Weight loss, malnutrition from impaired oral intake
Special Considerations
- HIV patients: ART initiation alongside antifungal therapy; consider chronic suppression if CD4 remains low. Recurrence is common until immune reconstitution occurs.
- Inhaled corticosteroid users: Encourage spacer use and mouth rinsing post-inhalation; consider switching to alternative ICS formulations.
- Drug interactions: Fluconazole is a potent CYP2C9/CYP3A4 inhibitor — check interactions with anticoagulants, immunosuppressants, and antiretrovirals.
- Azole resistance: Non-albicans species (especially C. glabrata) may be intrinsically resistant or develop acquired resistance; susceptibility testing recommended in refractory cases.
This is a shared conversation. Sign in to Orris to start your own chat.