Dengue like illness
Reading File
Finding Sources
Finding Sources
Searching PubMed
"dengue" AND "differential diagnosis"
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Loading Image
Finding Sources
I now have comprehensive information to synthesize a thorough answer. Let me compile everything.
Dengue-Like Illness
What Is "Dengue-Like Illness"?
The term encompasses acute febrile syndromes that present with the hallmark triad of dengue fever — high fever, severe myalgia/arthralgia, and rash — but may or may not be caused by dengue virus itself. In practice it spans true dengue and its key mimics. It is a notifiable condition in the US surveillance system as a distinct category alongside confirmed dengue.
Dengue Fever: The Prototype
Etiology & Epidemiology
- Four flavivirus serotypes (DENV-1 to -4) transmitted by Aedes aegypti (primarily) and Aedes albopictus
- Estimated 400 million infections/year worldwide, 100 million symptomatic, ~40,000 deaths from severe dengue
- Endemic across tropical/subtropical belt — South/Southeast Asia, Pacific, Americas, Africa
- Leading cause of febrile illness in travelers returning from the Caribbean, Latin America, and South Asia
- Incubation: 3–14 days after the infectious mosquito bite
Clinical Phases (WHO 2009 Classification)
| Phase | Timing | Features |
|---|---|---|
| Febrile phase | Days 1–3 | Abrupt high fever, severe headache, retro-orbital pain, myalgia/arthralgia ("breakbone fever"), facial flushing, injected oropharynx, macular/morbilliform rash, leukopenia |
| Critical phase | Days 3–7 (around defervescence) | Plasma leakage, hemoconcentration (↑ Hct), thrombocytopenia nadir — risk of severe dengue |
| Recovery phase | Days 7–10 | Reabsorption of leaked fluids, bradycardia, generalized pruritus |
WHO Severity Classification
- Dengue without warning signs — fever + ≥2 of: nausea/vomiting, rash, aches/pains, leukopenia, positive tourniquet test
- Dengue with warning signs — above + any of: abdominal pain/tenderness, persistent vomiting, clinical fluid accumulation (ascites, pleural effusion), mucosal bleeding, lethargy/restlessness, liver enlargement >2 cm
- Severe dengue — severe plasma leakage → shock or respiratory distress; severe bleeding; or severe organ involvement (AST/ALT ≥1000 IU/L, impaired consciousness, organ failure)
The Rash
About 50% of patients develop a rash. In 90% it appears on days 3–5, often at defervescence:
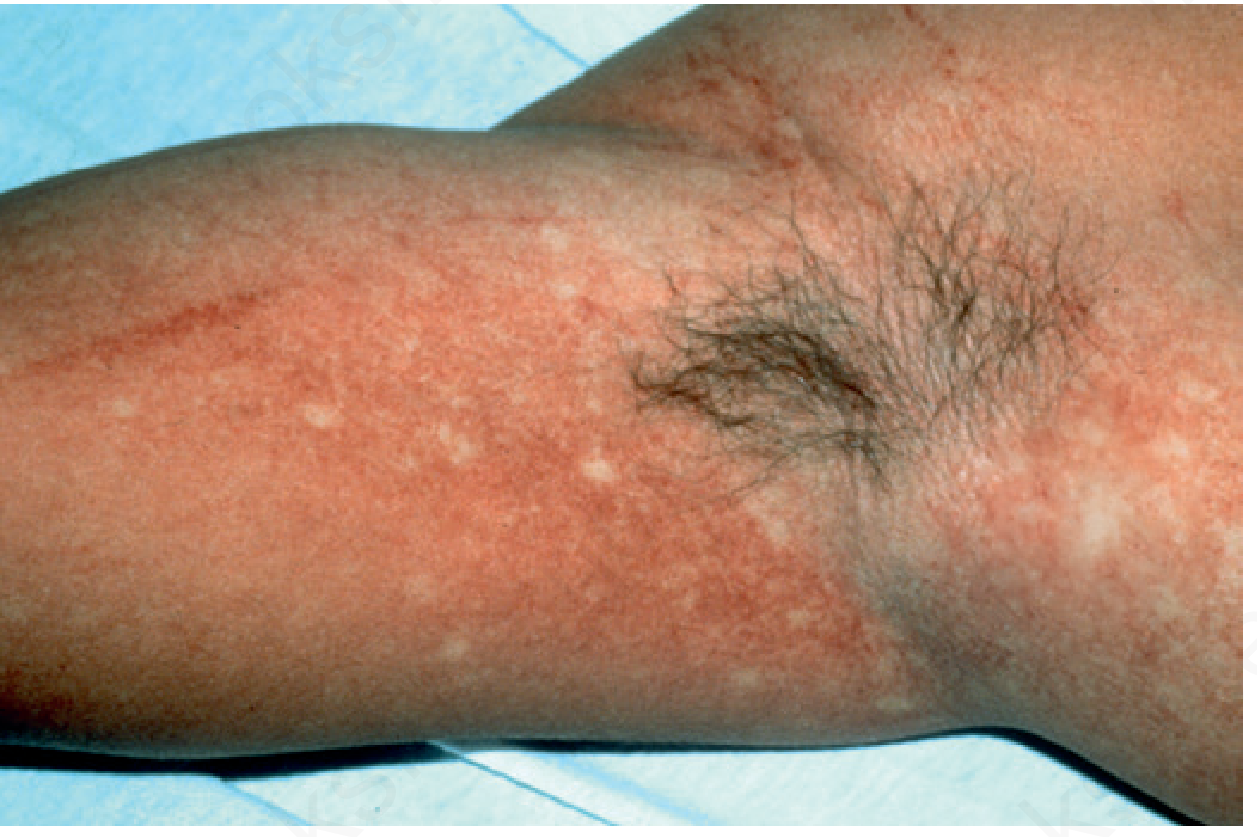
- Macular or morbilliform, usually confluent; "islands of white in a sea of red"
- Involves trunk (20%), extremities (30%), or generalized (50%)
- Mildly pruritic or asymptomatic
- Tourniquet test (Rumpel-Leede): inflate BP cuff for 5 min, wait 2 min → ≥10 petechiae/sq inch = positive
Pathophysiology of Severe Dengue
- Antibody-dependent enhancement (ADE): cross-reactive non-neutralizing antibodies from a prior serotype enhance Fc-receptor-mediated viral uptake into macrophages → amplified viral replication and cytokine storm → massive capillary leak
- Severe dengue predominantly occurs with second heterologous serotype infection (especially DENV-2 as the second serotype)
- Also occurs in infants with maternal anti-dengue antibodies (same ADE mechanism)
Differential Diagnosis — Dengue-Like Illness
The key mimics to consider, especially in a febrile traveler or endemic-area patient:
| Condition | Key distinguishing features |
|---|---|
| Chikungunya | Fever + rash + severe, debilitating polyarthritis/arthralgia (more prominent than dengue); less thrombocytopenia; joint symptoms may persist for months |
| Zika virus | Usually mild; non-purulent conjunctivitis prominent; rash often preceded by itch; teratogenic (microcephaly); associated with Guillain-Barré |
| Malaria | Cyclic fever pattern; splenomegaly; no rash typically; thick/thin blood films or RDT; can be rapidly fatal (P. falciparum) |
| Chikungunya + Dengue co-infection | Both co-circulate in same areas with same vector |
| Leptospirosis | Exposure to contaminated water; conjunctival suffusion; jaundice; can cause Weil's disease; positive serology |
| Rickettsial infections (e.g. RMSF, scrub typhus) | Eschar in scrub typhus; centripetal rash spreading to palms/soles in RMSF; responds to doxycycline |
| Yellow fever | Jaundice; bradycardia (Faget's sign); travel to endemic region; unvaccinated |
| Viral hemorrhagic fevers (Ebola, Marburg, Lassa) | Contact with infected individuals/animals; exposure history; severe bleeding |
| Measles | Koplik spots; cough, coryza, conjunctivitis; many dengue-endemic countries also have measles |
| Typhoid fever | Relative bradycardia, rose spots, diarrhea or constipation; gradual fever onset |
| Colorado tick fever | Tick exposure in Rocky Mountains; saddleback fever (biphasic); described as "dengue-like disease with rash" |
| COVID-19 | Dengue-like petechiae and erythema multiforme-like eruptions reported in early pandemic; PCR confirms |
| Influenza | Respiratory predominance; no rash; no thrombocytopenia |
Sources: Rosen's Emergency Medicine; Goldman-Cecil Medicine; Red Book 2021; Fitzpatrick's Dermatology
Laboratory Findings
| Finding | Significance |
|---|---|
| Leukopenia | Characteristic of dengue (helps distinguish from bacterial infection) |
| Thrombocytopenia (<100,000 in 50% of patients) | Marker of severity; nadir at defervescence |
| ↑ Hematocrit (hemoconcentration) | Signals plasma leakage → severe dengue risk |
| Elevated AST/ALT (~3× normal on average) | Dengue hepatitis; ≥1000 IU/L = severe dengue criterion |
| Positive tourniquet test | Suggests capillary fragility |
Diagnostic Testing
| Test | Window | Notes |
|---|---|---|
| RT-PCR (RNA detection) | Days 1–7 | Most specific for early infection |
| NS1 antigen EIA | Days 1–7–10 | Highly sensitive early; detects nonstructural protein 1 |
| IgM antibody EIA | From day 3–5 onwards; 99% positive by day 10 | Cross-reacts with Zika and other flaviviruses |
| IgG antibody | Persists for life | Fourfold rise (acute vs. convalescent) confirms infection |
| NS1 + IgM combo | Days 1–10 | Identifies ≥90% of primary and secondary cases |
Management
No specific antiviral exists — treatment is supportive
All patients:
- Rest, oral hydration, paracetamol (acetaminophen) for fever/pain
- Avoid NSAIDs and aspirin (risk of bleeding, Reye's syndrome)
- Monitor CBC, Hct, platelets daily around defervescence
Warning signs / critical phase monitoring:
- Watch for: persistent vomiting, severe abdominal pain, mucosal bleeding, early shock signs, rapid ↓ platelets + ↑ Hct
- IV crystalloid fluids for dehydration or plasma leakage
Severe dengue (DHF/DSS):
- ICU admission; fluid resuscitation (IV crystalloids first, then colloids/blood products if refractory shock)
- Blood product transfusion for hemorrhagic sequelae
- Early recognition reduces mortality from ~5–10% to <1%
- Avoid fluid overload during recovery phase (reabsorption phase risk)
Disposition:
- Outpatient: uncomplicated dengue without warning signs
- Admission: warning signs, dehydration requiring IV fluids
- ICU: dengue shock syndrome (DSS)
Vaccines
- Dengvaxia (CYD-TDV): licensed in several countries; only recommended for seropositive individuals (prior dengue infection confirmed) — naive recipients have increased risk of severe dengue on first natural infection post-vaccination (ADE concern)
- TAK-003 (Qdenga): approved in EU, Indonesia, Brazil; for ages 4–60; does not require prior serostatus testing
- Ongoing concern that vaccines might potentiate severe disease through ADE mechanisms remains a key challenge
Special Populations
| Population | Key concern |
|---|---|
| Infants | Maternal dengue antibodies → ADE risk → severe dengue |
| Pregnant women | Vertical transmission ~20% (higher near delivery); preterm birth, low birth weight risk |
| Travelers | Most common febrile illness returning from SE Asia within 1 month; also dominant in Caribbean/Latin America returnees |
| Patients with DM, asthma, sickle cell | Higher risk of severe disease |
| Elderly (>65) | Higher severe disease risk |
Key Clues to Diagnose Dengue Over Other Tropical Febrile Illnesses
From a predictive study in Honduras, the following features favor dengue:
- Petechiae
- Skin rash
- Myalgia
- Retro-ocular pain
- Positive tourniquet test
- Gingival bleeding
Sources: Andrews' Diseases of the Skin; Robbins Pathologic Basis of Disease; Red Book 2021; Harrison's Principles of Internal Medicine 22E (2025); Rosen's Emergency Medicine; Goldman-Cecil Medicine; Brenner & Rector's The Kidney; Fitzpatrick's Dermatology
This is a shared conversation. Sign in to Orris to start your own chat.