Evaluation of holmium yag laser versus cold knife in optical internal urethrotomy for management of anterior urethral stricture less than 1.5 cm : A comparative quasi experimental study .... this is my topic of synopsis i have to defend in a meeting teach me how to defend it and how to answer every expected question on this topic in background of authentic urology guidelines and books
urethral stricture etiology pathophysiology classification anterior urethra
optical internal urethrotomy cold knife technique outcomes recurrence
holmium YAG laser urethrotomy urethral stricture results complications
urethral stricture management guidelines EAU AUA urethroplasty versus urethrotomy
anterior urethral stricture anatomy optical internal urethrotomy
urethral stricture diagnosis urethrography uroflowmetry urethroscopy
urethral stricture recurrence predictors spongiofibrosis stricture length single versus multiple
DVIU direct vision internal urethrotomy complications erectile dysfunction urinary incontinence
urethroplasty versus internal urethrotomy success rate quasi experimental study design
Complete Defense Guide: Holmium YAG Laser vs. Cold Knife OIU for Anterior Urethral Stricture < 1.5 cm
PART 1: MASTER YOUR BACKGROUND — Know This Cold
What Is a Urethral Stricture?
| Segment | Location |
|---|---|
| Penile (pendulous) urethra | Within corpus spongiosum in penile shaft |
| Bulbar urethra | From penoscrotal junction to external sphincter |
| Fossa navicularis | Distal glandular segment |
Etiology (Know All Causes)
| Cause | Notes |
|---|---|
| Idiopathic | Most common in bulbar urethra (up to 40%) |
| Iatrogenic | Catheterization, cystoscopy, TURP, hypospadias repair |
| Inflammatory | Lichen sclerosus (BXO) — affects penile/meatal urethra |
| Traumatic | Straddle injury — classic for bulbar urethra |
| Infectious | Gonorrhea (now rare in developed countries) |
Clinical Presentation & Diagnosis
- Hesitancy, poor urinary stream, prolonged voiding, terminal dribbling
- Recurrent UTIs, epididymo-orchitis
- Urinary retention (acute or chronic)
| Test | Role |
|---|---|
| Uroflowmetry | Screening — prolonged "box-shaped" flow curve, reduced Qmax |
| RGU (Retrograde Urethrogram) | Gold standard for location, length, severity |
| VCUG (Voiding Cystourethrogram) | Assesses proximal extent |
| Ultrasound urethrography | Assesses degree of spongiofibrosis |
| Urethroscopy | Intraoperative assessment |
PART 2: YOUR STUDY DESIGN — Be Ready to Defend Every Choice
Why Quasi-Experimental?
- Why not RCT? Ethical, practical, or resource constraints; patient/surgeon preference may prevent concealed allocation; laser availability may be limited to certain sessions.
- Strength: Reflects real-world clinical practice.
- Limitation: Selection bias is the main threat — mitigate with matched groups and statistical adjustment (e.g., propensity scoring if applicable).
Why < 1.5 cm?
- Short strictures (< 2 cm, single, bulbar) are the best candidates for endoscopic management per EAU guidelines.
- By limiting to < 1.5 cm, you are studying the ideal population for OIU — this controls for stricture length as a major confounder.
- Longer strictures have inherently worse outcomes for all endoscopic approaches, so comparing laser vs. cold knife across variable lengths would introduce bias.
PART 3: THE CORE COMPARISON — Laser vs. Cold Knife
Cold Knife DVIU (Direct Vision Internal Urethrotomy)
- Sachs urethrotome or Storz cold knife at 12 o'clock position (or 3 and 9 o'clock for wider incisions)
- Cuts through the fibrotic segment into periurethral fat
- Urethral catheter left for 24–72 hours post-procedure
- Mechanism: mechanical incision of stricture, healing by secondary intention
- Overall stricture-free rate: 68.5% across 2,735 cases (Jin et al. SR)
- First DVIU stricture-free rate: 42.7%
- Bulbar urethra specifically: 60% stricture-free
Holmium:YAG Laser Urethrotomy
- Wavelength: 2,140 nm — absorbed by water → precise vaporization with minimal thermal spread (0.3–0.5 mm)
- Fiber delivered endoscopically; incision at 12 o'clock
- Advantages: hemostasis, precision, minimal collateral damage to surrounding spongiosum
- Overall stricture-free rate: 74.9% across 495 cases (Jin et al. SR)
- First DVIU with laser: 58.6%
- Meta-analysis RR for recurrence in favor of laser:
- At 3 months: RR 0.55 (95% CI: 0.18–1.66; p=0.29) — not significant
- At 6 months: RR 0.39 (95% CI: 0.19–0.81; p=0.01) — significant
- At 12 months: RR 0.44 (95% CI: 0.26–0.75; p=0.003) — significant
- At bulbar urethra: laser 52.9% vs cold knife 60% — no significant difference (p=0.66)
Head-to-Head Summary Table
| Parameter | Cold Knife DVIU | Ho:YAG Laser DVIU |
|---|---|---|
| Mechanism | Mechanical incision | Photothermal vaporization |
| Hemostasis | Manual/packing | Intrinsic |
| Thermal spread | None | 0.3–0.5 mm (minimal) |
| Overall stricture-free rate | 68.5% | 74.9% |
| First-procedure success | 42.7% | 58.6% (p=0.09, NS) |
| Recurrence at 12 months | Higher | Lower (RR 0.44, p=0.003) |
| Bulbar urethra outcomes | ~60% | ~53% (NS difference) |
| Cost | Low | Higher (laser setup) |
| Availability | Universal | Requires laser system |
PART 4: EAU GUIDELINE RECOMMENDATIONS (Your Authority Source)
Recommendation: Offer endoscopic urethrotomy (DVIU or laser) as the first-line management for short (< 2 cm), single, bulbar urethral strictures.
Key principle: Patients should be counseled that urethroplasty has superior long-term success over repeated DVIU but DVIU is appropriate as first-line or when the patient declines open surgery.
- DVIU and laser urethrotomy are equivalent in efficacy for short bulbar strictures (Grade C recommendation)
- Repeat DVIU is not recommended if recurrence occurs after one urethrotomy — urethroplasty should be offered
- Stricture length < 2 cm, single, bulbar location = best predictor of success after DVIU
- Self-catheterization (intermittent dilations) post-DVIU may delay but not prevent recurrence
PART 5: EXPECTED DEFENSE QUESTIONS — WITH EXACT ANSWERS
Q1: What is the rationale/justification for your study?
Q2: Why anterior urethra only? Why not posterior?
Q3: What outcome measures did you use?
- Operative time
- Intraoperative bleeding
- Post-operative complications (infection, extravasation, erectile dysfunction)
- Patient-reported outcomes (IPSS, SHIM/IIEF scores)
- Catheterization duration post-procedure
Q4: What are the predictors of success/failure after OIU?
- Stricture length < 1.5–2 cm (primary reason for your inclusion criterion)
- Single stricture (not multiple)
- Bulbar location (better than penile)
- Idiopathic etiology
- No prior urethrotomy (first-time procedure)
- Absence of dense spongiofibrosis (ultrasound-assessed)
- Stricture > 2 cm
- Penile/anterior penile location
- Lichen sclerosus (BXO) etiology
- Prior failed urethrotomy
- Dense circumferential spongiofibrosis
Q5: Why not do urethroplasty instead?
Q6: What is the OPEN trial? How does it relate to your work?
Q7: What are the complications of OIU?
| Complication | Rate |
|---|---|
| Urinary tract infection | 5–15% |
| Bleeding/hematuria | 3–8% |
| False passage / urethral perforation | 1–3% |
| Erectile dysfunction | < 1–2% (from sphincter/nerve proximity) |
| Urinary incontinence | Rare (< 1%), risk if sphincter involved |
| Recurrence (the main complication) | 30–60% within 12 months |
Q8: What does Holmium laser do that cold knife doesn't?
- Wavelength 2,140 nm is absorbed by water in tissue → precise vaporization at point of contact
- Thermal penetration depth only 0.3–0.5 mm → minimal collateral injury to surrounding spongiosum
- Simultaneous hemostasis — reduces bleeding and better visualization
- May produce less reactive fibrosis post-incision, theoretically reducing re-stricture
- Allows more precise incision depth under direct vision
Q9: Is your sample size justified?
- Expected stricture-free rate for cold knife: ~68% (from EAU evidence)
- Expected stricture-free rate for laser: ~75%
- Alpha = 0.05, Power = 80%
- Using two-proportion z-test formula
Q10: What is the limitation of your study design?
- Selection bias — non-randomized allocation; surgeons may preferentially choose laser for "easier" cases
- Short follow-up — recurrence often occurs at 6–24 months; longer follow-up needed
- No spongiofibrosis grading — ultrasound urethrography would add pathological depth
- Single-center — limits generalizability
- Surgeon learning curve with laser not accounted for
- No patient-reported outcomes tool (if not used) — IPSS/IIEF adds important dimension
Q11: How do you define "recurrence" in your study?
"Recurrence is defined as symptomatic return of obstructive voiding with objective evidence of re-stricture, confirmed by uroflowmetry showing Qmax < 15 mL/s AND/OR RGU demonstrating luminal narrowing to < 50% of normal caliber, requiring re-intervention."
Q12: What is spongiofibrosis and why does it matter?
- Depth of incision needed
- Risk of recurrence
- Whether endoscopic management is sufficient or urethroplasty is required
- Deep spongiofibrosis = more recurrence with OIU = favor urethroplasty
Q13: Why specifically < 1.5 cm and not the conventional < 2 cm cutoff?
PART 6: KEY REFERENCES TO CITE
| Source | What to cite |
|---|---|
| EAU Guidelines on Urethral Strictures (current year) | All recommendations, laser vs cold knife SR, recurrence rates |
| Jin et al. (SR, 44 case series) | Stricture-free rates 74.9% laser vs 68.5% cold knife |
| Meta-analysis of 4 RCTs (EAU cited) | RR of recurrence at 6 and 12 months favoring laser |
| OPEN Trial | RCT: endoscopy non-inferior to urethroplasty at 24 months for < 2 cm bulbar strictures |
| ROBUST III Trial | Evolving role of endoscopy in recurrent bulbar stricture |
| Bailey & Love's Surgery, 28th ed., p.1564 | Clinical features, diagnosis, uroflowmetry pattern |
| Campbell-Walsh-Wein Urology | Comprehensive anatomy, pathophysiology, surgical technique |
PART 7: OPENING STATEMENT FOR YOUR DEFENSE
"Urethral stricture disease is a common urological condition affecting approximately 200–300 per 100,000 males, with a significant impact on quality of life. Optical internal urethrotomy remains the most widely performed endoscopic procedure for short anterior strictures, with cold knife DVIU being the conventional technique. However, holmium:YAG laser offers theoretical advantages of precision, hemostasis, and reduced collateral tissue injury. While the EAU systematic review demonstrates an overall trend favoring laser (74.9% vs 68.5% stricture-free rates) with statistically significant reduction in recurrence at 12 months (RR 0.44, p=0.003), no existing study has isolated this comparison to the homogeneous subgroup of anterior strictures less than 1.5 cm — the ideal candidate for endoscopic management. This study aims to provide evidence-based guidance for this specific clinical scenario using a rigorous comparative design in a real-world surgical setting."
PART 8: IMAGE — Internal Urethrotomy Under Local Anesthesia
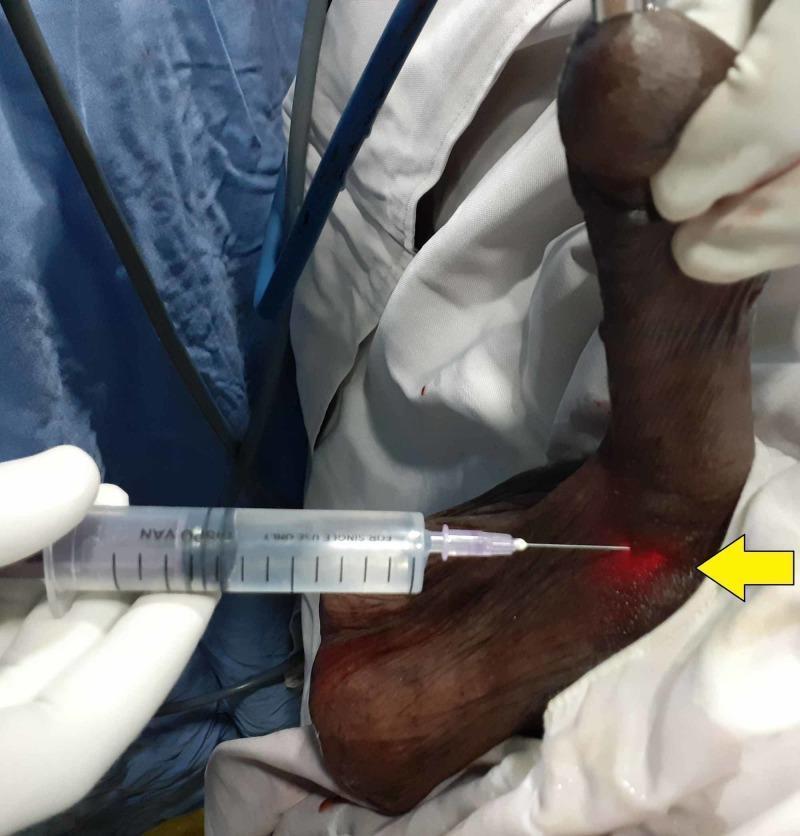
Quick Cheat Sheet for the Day of Defense
| If asked about... | Lead with... |
|---|---|
| Why this topic? | Gap in literature for < 1.5 cm anterior stricture comparison |
| Why quasi-experimental? | Practical constraints; reflects real-world practice |
| Laser advantage? | Precision, hemostasis, RR 0.44 at 12 months |
| Cold knife advantage? | Universal availability, lower cost, equivalent bulbar outcomes |
| EAU recommendation? | Both acceptable for short single anterior strictures |
| Limitations? | Selection bias, single center, follow-up duration |
| What if results show no difference? | Consistent with bulbar-specific data (p=0.66); suggests cost-effectiveness of cold knife |
| What if laser is better? | Supports adoption of laser as preferred modality in short anterior strictures |
is optical internal urethrotomy is used for anterior urethral stricture both in penile and bulbar level give me logical reasoning and backing of authentic sources and references
optical internal urethrotomy indications anterior urethral stricture penile bulbar urethra
DVIU direct vision internal urethrotomy bulbar penile urethra outcomes location
anterior urethra anatomy penile bulbar segments stricture treatment endoscopic
penile urethral stricture OIU urethrotomy high recurrence poor outcome spongiofibrosis
bulbar urethral stricture ideal candidate internal urethrotomy short single success rate
EAU guidelines urethral stricture recommendation endoscopic treatment stricture location length grade
Is OIU Used for Anterior Urethral Stricture at Both Penile AND Bulbar Levels?
The Short Answer: Technically Yes — But Guidelines Strongly Differentiate Between the Two
The Anatomical & Pathological Basis for the Difference
| Feature | Bulbar Urethra | Penile (Pendulous) Urethra |
|---|---|---|
| Surrounding tissue | Thick corpus spongiosum | Thinner, more mobile corpus spongiosum |
| Blood supply | Rich — bulbar artery branches | Less robust, more dependent on distal flow |
| Spongiofibrosis depth | Often superficial in idiopathic/traumatic | Often dense, circumferential (lichen sclerosus, iatrogenic) |
| Common etiology | Idiopathic, straddle trauma | Lichen sclerosus (BXO), instrumentation, hypospadias |
| Tissue elasticity | Better healing after incision | Poor wound remodeling, higher re-scarring tendency |
| Access for endoscope | Easy, short path | Longer path, mobile penile skin complicates scope handling |
What the Guidelines Actually Say
AUA Guidelines on Urethral Stricture Disease — The Definitive Statement
Recommendation 7 (AUA): "Surgeons may offer urethral dilation, direct visual internal urethrotomy (DVIU), or urethroplasty for the initial treatment of a short (< 2 cm) bulbar urethral stricture." (Conditional Recommendation; Evidence Level: Grade C) "The highest success rates are found in those with bulbar strictures < 1 cm." — Urethral Stricture Disease Guidelines, AUA, p.3
Recommendation 15 (AUA): "Surgeons should offer urethroplasty to patients with penile urethral strictures given the expected high recurrence rates with endoscopic treatments. Strictures involving the penile urethra are unlikely to respond to dilation or urethrotomy, and these patients should be offered urethroplasty at the time of diagnosis." (Moderate Recommendation; Evidence Level: Grade C) — Urethral Stricture Disease Guidelines, AUA, p.4
EAU Guidelines on Urethral Strictures — Corroborating Evidence
"At the bulbar urethra, laser and 'cold knife' DVIU yielded a stricture-free rate of 52.9% and 60%, respectively (p=0.66)."
"None of these four [RCT] studies specified the results based on the location of the stricture"
Logical Reasoning: Why OIU Works Poorly in the Penile Urethra
1. The Nature of Spongiofibrosis is Different
- Lichen sclerosus (BXO) — an inflammatory dermatosis causing obliterative, progressive, multi-segment fibrosis
- Iatrogenic injury (catheter trauma, instrumentation) — causing dense circumferential fibrosis
- Hypospadias repair complications — structurally altered urethral plate
2. Wound Healing Dynamics Favor Re-Stricture
3. The Penile Urethra Lacks the Same Vascular Reserve
4. Recurrence is the Rule, Not the Exception
Practical Summary: When OIU IS and IS NOT the Right Choice
| Stricture Location | OIU Appropriate? | Guideline Stance | Rationale |
|---|---|---|---|
| Bulbar urethra, < 2 cm, single | ✅ Yes — first-line option | AUA: Conditional Recommendation | Best outcomes; guideline-endorsed |
| Bulbar urethra, < 1 cm | ✅ Yes — highest success | AUA: Specifically highlighted | Stricture-free rates highest in this subgroup |
| Bulbar urethra, ≥ 2 cm | ⚠️ Not preferred | AUA Rec. 16: Offer urethroplasty | Low success rate endoscopically |
| Penile urethra (any length) | ❌ Not recommended as standard | AUA Rec. 15: Offer urethroplasty | High recurrence; unlikely to respond |
| Penile urethra, very short, no BXO | ⚠️ Can be attempted (practitioner discretion) | No strong prohibition, but no endorsement | Only if patient declines surgery; counsel on high failure |
| Fossa navicularis / meatus | ❌ OIU not applicable | Meatotomy/meatoplasty preferred | Different anatomy and approach entirely |
Direct Implication for Your Study — How to Use This in Your Defense
"If the AUA says OIU is not recommended for penile urethral strictures, why does your study include anterior urethral strictures at the penile level?"
"This is precisely the clinical controversy my study addresses. Current guidelines recommend against routine OIU for penile urethral strictures based on overall recurrence data, which is largely derived from heterogeneous populations with variable stricture lengths, mixed etiologies including lichen sclerosus, and multiple prior procedures. My study specifically excludes lichen sclerosus, limits stricture length to < 1.5 cm, and includes only primary or selected cases — a subgroup that may behave differently from the general penile stricture population. Furthermore, in resource-limited settings where urethroplasty is not always immediately available, understanding the relative performance of laser versus cold knife OIU in this subgroup has genuine clinical value. My study does not contradict guidelines — it provides subgroup-specific data to refine decision-making in a defined, controlled population."
Key References to Quote Verbatim
| Source | Exact Statement |
|---|---|
| AUA Urethral Stricture Disease Guidelines, p.3, Rec.7 | "Surgeons may offer DVIU for initial treatment of short (< 2 cm) bulbar urethral stricture; highest success in bulbar strictures < 1 cm" |
| AUA Urethral Stricture Disease Guidelines, p.4, Rec.15 | "Surgeons should offer urethroplasty to patients with penile urethral strictures given expected high recurrence rates with endoscopic treatments" |
| EAU Urethral Strictures Guidelines, p.25 (Jin et al. SR) | "At the bulbar urethra, laser and cold knife DVIU yielded a stricture-free rate of 52.9% and 60% respectively (p=0.66)" |
| EAU Urethral Strictures Guidelines, p.23 (Steenkamp et al.) | "Both DVIU and dilatation become less effective with increasing stricture length" |
| Bailey & Love's Surgery, 28th ed., p.1564 | Clinical features, diagnosis pathway, uroflowmetry findings |
Bottom Line to Memorize
OIU is technically feasible at both bulbar and penile levels of the anterior urethra, but it is only guideline-endorsed as a meaningful treatment option at the bulbar level for short (< 2 cm), single strictures. For penile urethral strictures, both AUA and EAU data converge on urethroplasty as the appropriate first-line treatment due to the inherently high recurrence rate of endoscopic approaches, driven by the nature of spongiofibrosis, wound healing biology, and predominant etiology (lichen sclerosus) at the penile level.