Acute MI
Reading File
search_medical_text
acute myocardial infarction pathophysiology classification STEMI NSTEMI diagnosis ECG biomarkers
search_medical_text
acute MI management treatment reperfusion thrombolytics PCI antiplatelet anticoagulation
search_medical_image
acute myocardial infarction ECG changes ST elevation STEMI
GradeResponse
GradeResponse
GradeResponse
Acute Myocardial Infarction (AMI)
Definition & Classification
Acute MI is part of the Acute Coronary Syndrome (ACS) spectrum, caused by disruption (rupture or erosion) of an unstable coronary artery atherosclerotic plaque, leading to partial or complete coronary thrombosis and myocardial ischemia/necrosis.
ACS continuum (Management of Patients With Acute Coronary Syndromes, p. 10):
| Condition | Vessel Occlusion | Ischemia Pattern | Troponin | ECG |
|---|---|---|---|---|
| Unstable Angina | Partial | Subendocardial | Negative | No ST elevation |
| NSTEMI | Partial | Subendocardial | Elevated | No ST elevation |
| STEMI | Complete | Transmural | Elevated | ST elevation |
The pathophysiology is dynamic — patients can rapidly progress from UA → NSTEMI → STEMI during initial evaluation and treatment.
Less common causes include coronary artery spasm, embolism, and dissection.
Clinical Presentation
- Chest pain/pressure — classic, often radiating to left arm, jaw, or back
- Diaphoresis, nausea, vomiting
- Dyspnea, especially with reduced LV function
- Silent MI — particularly in diabetics and elderly (no chest pain)
- Killip classification guides severity assessment (I–IV)
Diagnosis
1. ECG
Initial ECG within 10 minutes of presentation is mandatory.
STEMI criteria:
- New ST elevation ≥1 mm in ≥2 contiguous limb leads
- ST elevation ≥2 mm in ≥2 contiguous precordial leads (≥2.5 mm in men <40 y)
- New LBBB (treat as STEMI equivalent)
NSTEMI/UA:
- ST depression, T-wave inversions, or non-specific changes
- Normal ECG does not exclude MI
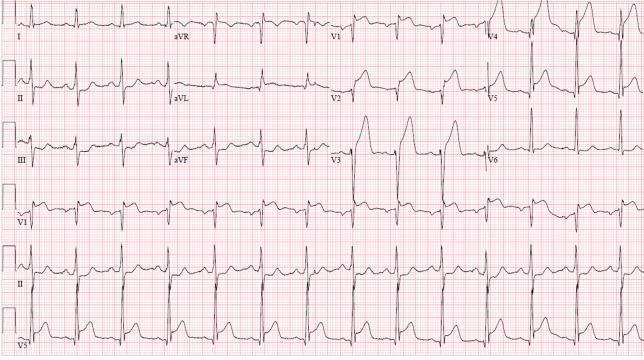
2. Cardiac Biomarkers
- High-sensitivity troponin (hs-cTn) — gold standard; rises within 1–3 hrs, peaks at 12–24 hrs
- 0h/1h or 0h/2h rapid rule-out/rule-in protocols (ESC recommended)
- CK-MB useful for re-infarction detection (shorter half-life)
3. Imaging
- Echo — regional wall motion abnormalities, EF, mechanical complications
- Coronary angiography — definitive; performed at PCI
Management
STEMI — Time-Critical Reperfusion
Primary PCI (PPCI) is the preferred strategy:
- Target: door-to-balloon ≤90 min (≤120 min if transfer required)
- If PPCI unavailable within 120 min: fibrinolysis within 10 min of diagnosis
- Post-fibrinolysis: transfer for angiography within 3–24 hrs ("pharmaco-invasive")
NSTEMI — Risk-Stratified Invasive Strategy
- Very high risk (refractory ischemia, hemodynamic instability, VT/VF): immediate angiography (<2 hrs)
- High risk (elevated troponin, dynamic ECG changes, GRACE score >140): early invasive (<24 hrs)
- Low-to-intermediate risk: selective invasive strategy
Antithrombotic Therapy (Management of Acute Coronary Syndromes, p. 36)
Antiplatelet
- Aspirin 150–300 mg loading dose → 75–100 mg/day indefinitely
- P2Y12 inhibitor (DAPT for 12 months):
- Ticagrelor 180 mg → 90 mg BID (preferred in NSTEMI/STEMI)
- Prasugrel 60 mg → 10 mg/day (STEMI undergoing PCI; avoid if prior stroke/TIA, age >75, weight <60 kg)
- Clopidogrel 300–600 mg → 75 mg/day (if above unavailable/contraindicated; preferred in elderly >70–80 yrs)
Routine pre-treatment with a P2Y12 inhibitor in NSTE-ACS patients planned for early invasive strategy (<24 h) when coronary anatomy is unknown is not recommended.
Anticoagulation
| Setting | Preferred Agent |
|---|---|
| STEMI (PCI) | UFH or bivalirudin |
| NSTE-ACS (PCI) | Enoxaparin or UFH |
| NSTE-ACS (medical/delayed PCI >24h) | Fondaparinux (preferred) |
Other Acute Medications
- Beta-blockers — start within 24 hrs if no contraindications (HF, cardiogenic shock, bradycardia)
- High-intensity statin — atorvastatin 40–80 mg immediately
- ACE inhibitor/ARB — start within 24 hrs, especially if EF <40%, anterior MI, or diabetes
- Nitrates — symptom relief; avoid if RV infarct or hypotension
- Morphine — use cautiously (may delay antiplatelet absorption)
Complications
| Early (<48 hrs) | Late (Days–Weeks) |
|---|---|
| Cardiogenic shock | HF / reduced EF |
| Ventricular fibrillation/VT | Ventricular aneurysm |
| AV block (especially inferior MI) | Dressler's syndrome (pericarditis) |
| Mechanical: free wall rupture, VSD, papillary muscle rupture (acute MR) | Thrombus / embolic stroke |
Mechanical complications present with sudden hemodynamic deterioration + new murmur — require urgent echo and surgical/interventional management.
Risk Stratification & Secondary Prevention
- GRACE score (in-hospital and 6-month mortality) — guides invasive timing in NSTEMI
- TIMI score — widely used bedside risk tool
- Echo pre-discharge — EF guides need for ICD (EF <35% after ≥40 days post-MI)
- Cardiac rehab — reduces mortality and rehospitalization
- Long-term DAPT duration individualized by bleeding vs. ischemic risk (HBR patients may shorten to 3–6 months; high ischemic risk may extend beyond 12 months)
Special Populations
| Population | Key Consideration |
|---|---|
| Elderly (>75 yrs) | Higher bleeding risk; prefer clopidogrel over prasugrel; lower fibrinolytic threshold |
| Diabetes | Higher rate of silent MI; worse outcomes; early invasive preferred |
| CKD | Contrast nephropathy risk; adjust anticoagulant dosing |
| Women | More atypical presentation; higher in-hospital mortality; MINOCA more common |
| Cardiogenic shock | PPCI + hemodynamic support (IABP, Impella); CABG if multivessel disease |
This is a shared conversation. Sign in to Orris to start your own chat.