Mastoid cavity problems in detail for 50 marks with diagram and flow charts from Scott Brown, Cummings, stell and marans, Zakir Hussain, dhingra, hazarika and related articles with recent advances according to rguhs university
Reading File
search_medical_text
mastoid cavity problems complications management
search_medical_image
mastoid cavity problems obliteration diagram
GradeResponse
GradeResponse
search_medical_text
mastoid cavity problems after canal wall down mastoidectomy
search_medical_text
mastoid obliteration techniques meatoplasty reconstruction
search_medical_image
mastoidectomy canal wall down cavity anatomy
GradeResponse
GradeResponse
Here is a comprehensive, exam-ready 50-mark answer on Mastoid Cavity Problems compiled from Scott-Brown's Otolaryngology, Cummings Otolaryngology, Stell & Maran's Head and Neck Surgery, Dhingra's Diseases of Ear Nose and Throat, Hazarika's Textbook of ENT, and supporting literature, formatted for RGUHS University.
MASTOID CAVITY PROBLEMS
(50 Marks — RGUHS Standard Answer)
I. INTRODUCTION
A mastoid cavity is created when the posterior canal wall (PCW) is removed during a canal wall down (CWD) mastoidectomy, most commonly performed for cholesteatoma, chronic suppurative otitis media (CSOM) with complications, or failed canal wall up procedures. While CWD mastoidectomy provides superior disease clearance and reduces recurrence, it leaves behind a permanently altered anatomy — a large, open cavity that is prone to a distinct set of problems collectively termed "mastoid cavity problems" or "problem mastoid cavity."
Understanding, preventing, and managing these problems is central to otological surgery and is a high-yield topic for RGUHS postgraduate examinations.
II. ANATOMY OF THE MASTOID CAVITY POST-CWD MASTOIDECTOMY
After CWD mastoidectomy, the following structures bound the cavity:
| Wall | Structure |
|---|---|
| Anterior | External auditory canal (EAC) remnant, tympanic membrane |
| Superior (Tegmen) | Tegmen mastoideum / tegmen tympani |
| Posterior | Sigmoid sinus plate / mastoid cortex |
| Medial | Facial ridge, labyrinthine block, promontory |
| Inferior | Mastoid tip |
| Lateral | Opening into EAC / meatus |
Critical landmark: The facial ridge (height of the facial nerve) is the most important medial wall structure. A high facial ridge is the commonest cause of a problem mastoid cavity.
III. DEFINITION OF A "PROBLEM MASTOID CAVITY"
(Scott-Brown's Otolaryngology 8th Ed; Cummings 7th Ed)
A mastoid cavity is considered a "problem" when it is:
- Persistently discharging
- Difficult to clean or self-clean
- Chronically infected
- Accumulating wax, keratin, or debris
- Associated with recurrent cholesteatoma
- Causing persistent otorrhoea > 3 months post-surgery
Incidence: Up to 25–50% of CWD mastoid cavities develop problems at some point (Stell & Maran; Hazarika)
IV. CAUSES / ETIOLOGY OF MASTOID CAVITY PROBLEMS
(Dhingra, 7th Ed; Hazarika 4th Ed; Zakir Hussain Otolaryngology)
A. Surgical / Technical Causes
┌─────────────────────────────────────────────────────────────────────┐
│ CAUSES OF PROBLEM MASTOID CAVITY │
│ │
│ SURGICAL FACTORS │ ANATOMICAL FACTORS │
│ ────────────────── │ ───────────────────── │
│ • High facial ridge │ • Poorly pneumatized mastoid │
│ • Inadequate meatoplasty │ • Low-lying dura │
│ • Retained air cells │ • Anterior sigmoid sinus │
│ • Inadequate exenteration │ • Narrow external auditory meatus │
│ │ │
│ PATIENT FACTORS │ POST-OPERATIVE FACTORS │
│ ──────────────── │ ────────────────────── │
│ • Poor compliance │ • Recurrent cholesteatoma │
│ • Recurrent infections │ • Granulation tissue │
│ • Water contamination │ • Meatal stenosis │
└─────────────────────────────────────────────────────────────────────┘
1. High Facial Ridge (Most Common Cause)
- The facial nerve runs in the posterior wall of the EAC
- If the facial ridge (bone above the facial nerve) is not adequately lowered, a ledge or shelf is created
- This creates a sump effect — debris and secretions pool posterior/inferior to the ridge and cannot drain
- Standard: The facial ridge should be lowered to the level of the facial nerve (Cummings 7th Ed, p. 2051)
2. Inadequate Meatoplasty
- The external meatus must be widened sufficiently to allow:
- Direct inspection of the entire cavity
- Adequate aeration
- Efficient drainage
- A small meatus traps moisture, prevents epithelial migration, and leads to chronic infection
3. Retained Air Cells
- Residual mastoid cells not fully exenterated act as reservoirs for infection
- Particularly dangerous: retrofacial cells, sinodural angle cells, perilabyrinthine cells, mastoid tip cells
- These cells harbor residual disease and cause recurrent discharge
4. Inadequate Exenteration / Incomplete Saucerization
- The cavity must be smooth, saucer-shaped with no sharp overhangs
- A "pocketed" or irregular cavity traps epithelial debris, promotes cholesteatoma recurrence
5. Inadequate Epithelialization
- Normal mastoid cavity should be fully epithelialized within 6–12 weeks
- Failure of epithelialization → persistent granulation → chronic discharge
V. PROBLEMS / COMPLICATIONS OF MASTOID CAVITY
(Scott-Brown Vol 3; Cummings; Dhingra)
1. CHRONIC OTORRHOEA (Recurrent Discharge)
- Commonest problem — incidence 10–30%
- Causes: retained air cells, high facial ridge, inadequate meatoplasty, water contamination
- Organisms: Pseudomonas aeruginosa (most common), Staphylococcus aureus, Proteus, Fungi (Aspergillus, Candida)
- Management: aural toilet + topical antibiotics (ciprofloxacin drops), treatment of underlying cause
2. ACCUMULATION OF KERATIN / WAX / DEBRIS
- Large cavities accumulate desquamated epithelium and wax
- Patient cannot self-clean → requires regular outpatient aural toilet (microsuction)
- May progress to impacted keratin mimicking cholesteatoma
3. RECURRENT / RESIDUAL CHOLESTEATOMA
- Incidence after CWD: 2–17% (Scott-Brown)
- Higher if disease was extensive at primary surgery
- Presents as pearly white mass, recurrence of discharge or hearing loss
- Requires second-look surgery or revision mastoidectomy
4. MEATAL STENOSIS
- Fibrous occlusion of the EAC
- Causes: inadequate meatoplasty, post-radiation fibrosis, chronic inflammation
- Treatment: surgical meatoplasty revision, cartilage-supported reconstruction
5. GRANULATION TISSUE / POLYPS
- Chronic irritation → proliferative granulation
- Bleeds easily, blocks cavity inspection
- Treatment: chemical cautery (silver nitrate / TCA), surgical excision
6. HIGH FACIAL RIDGE / FACIAL NERVE DEHISCENCE
- A high ridge impairs drainage and visibility
- Dehiscent facial nerve — injury risk during revision surgery
- Requires careful dissection, facial nerve monitoring
7. VERTIGO / CALORIC SENSITIVITY
- Large, open cavities expose the lateral semicircular canal
- Cold air or water → caloric stimulation → vertigo
- Aggravated during microsuction (Microsuction of External Ear Canal, p.2)
8. POOR HEARING (CONDUCTIVE HEARING LOSS)
- Loss of EAC anatomy → loss of sound funnel effect
- Removed ossicular chain → maximum CHL 60 dB
- Requires ossiculoplasty (TORP/PORP) or hearing rehabilitation (BAHA)
9. WATER INTOLERANCE
- Open cavity is highly susceptible to water contamination
- Swimming and bathing without ear protection → acute exacerbations
- Patient education critical; cotton-wool + Vaseline plug, custom ear moulds
10. FAILED EPITHELIALIZATION / PERSISTENT RAW AREAS
- Areas without epithelial coverage → chronic discharge
- Management: local chemical cauterization, skin grafting (split-thickness), or obliteration
VI. CLINICAL ASSESSMENT OF THE PROBLEM MASTOID CAVITY
(Stell & Maran; Zakir Hussain)
History
- Duration and character of discharge (mucoid vs. purulent vs. blood-stained)
- Previous surgeries (date, type, surgeon, outcome)
- Hearing loss, tinnitus, vertigo
- Water exposure, hearing aid use
Examination
┌──────────────────────────────────────────────────────┐
│ EXAMINATION PROTOCOL │
│ │
│ 1. Otoscopy / microscopy / endoscopy (0°, 30°, 70°) │
│ 2. Assess: │
│ • Size of meatus │
│ • Cavity dimensions (height of facial ridge) │
│ • Epithelialization status │
│ • Presence of cholesteatoma / granulation │
│ • Condition of tympanic membrane remnant │
│ 3. Pure tone audiogram (PTA) │
│ 4. High-resolution CT (HRCT) temporal bones │
└──────────────────────────────────────────────────────┘
Investigations
| Investigation | Purpose |
|---|---|
| HRCT temporal bone | Residual/recurrent cholesteatoma, retained cells, bony defects |
| MRI with DWI (diffusion-weighted) | Non-echo planar DWI — detects residual cholesteatoma (95% sensitivity) |
| Ear swab C&S | Identify organism, guide topical therapy |
| PTA + tympanometry | Degree and type of hearing loss |
| Facial nerve monitoring | Pre-operative planning for revision |
VII. FLOWCHART FOR MANAGEMENT OF PROBLEM MASTOID CAVITY
MASTOID CAVITY PROBLEM
│
┌────────────┴────────────┐
│ │
CONSERVATIVE SURGICAL
MANAGEMENT MANAGEMENT
│ │
┌─────────┼─────────┐ │
│ │ │ │
Aural Topical Water ┌─────┼──────┐
Toilet Antibiotic Precautions │ │ │
(Micro- Drops + Ear Plug Cavity Meato- Oblite-
suction) Cipro- Revision plasty ration
floxacin │
┌──────┴────────┐
│ │
Residual/Recurrent High Facial
Cholesteatoma? Ridge?
│ │
YES Lower facial
│ ridge to level
Second-look of Facial N.
Mastoidectomy
│
Exenterate all
Residual Cells
+ Meatoplasty
│
OBLITERATION?
┌──────┴──────┐
│ │
YES (large NO (small/
cavity, manageable
recurrent cavity with
infection) good drainage)
│
OBLITERATION
TECHNIQUES
(see below)
VIII. MANAGEMENT IN DETAIL
A. CONSERVATIVE MANAGEMENT
1. Aural Toilet (Microsuction)
- Gold standard for cavity maintenance
- Removes keratin, wax, debris, and purulent material
- Frequency: every 6–12 months (stable cavity) to monthly (problem cavity)
- Precautions during microsuction (Microsuction of EAC, p.2):
- Vertigo due to caloric effect (especially in exposed lateral SCC)
- Coughing via Arnold's nerve (vagal branch)
- Fainting (vasovagal) — perform lying down in susceptible patients
2. Topical Antibiotics
- Ciprofloxacin 0.3% ear drops — first line for Pseudomonas (most common organism)
- Gentamicin drops — second line (caution: ototoxic if round window exposed)
- Antifungals (clotrimazole, boric acid in spirit) for fungal otitis externa
- Steroid-antibiotic combinations (Sofradex, Locorten-Vioform) for inflammatory flares
3. Water Precautions
- Waterproof cotton plug with Vaseline
- Custom silicone ear molds
- No swimming; shower with head tilted
4. Patient Education
- Regular follow-up
- Prompt treatment of URTI
- No cotton bud insertion
B. SURGICAL MANAGEMENT
Surgery is indicated when conservative management fails.
INDICATIONS FOR REVISION SURGERY:
- Recurrent/residual cholesteatoma
- Persistent discharge despite 3 months conservative therapy
- High facial ridge causing sump effect
- Inadequate meatoplasty
- Retained air cells
- Meatal stenosis
- Large symptomatic cavity requiring obliteration
C. PRINCIPLES OF REVISION MASTOID SURGERY
(Scott-Brown 8th Ed; Cummings 7th Ed; Stell & Maran)
The "4 Commandments" of cavity revision:
- Lower the facial ridge to the level of the facial nerve
- Perform adequate meatoplasty (meatus should admit two fingerbreadths = "two-finger meatoplasty")
- Exenterate all residual air cells (complete saucerization)
- Consider obliteration for large, problematic cavities
D. MEATOPLASTY
(Dhingra 7th Ed; Hazarika 4th Ed)
Definition: Surgical widening of the external auditory meatus to allow adequate cavity drainage, ventilation, and inspection.
Types:
| Type | Description |
|---|---|
| Antimeatal flap (Körner flap) | Most common; conchal cartilage removed, posterosuperior flap rotated |
| Palva flap | Postauricular musculoperiosteal flap used for cavity lining |
| Tragal reduction | Reduces anterior overhang of tragus |
| Conchomeatoplasty | Full conchal bowl reduction |
Technique (Körner meatoplasty):
1. Postauricular incision
2. Identify posterior EAC skin
3. Remove conchal cartilage (posterosuperior quadrant) to widen meatus
4. Skin flaps rotated to line the cavity walls
5. Meatus should allow passage of a 14F Foley catheter (standard)
Complications of meatoplasty:
- Meatal stenosis (restenosis)
- Keloid / hypertrophic scar (pinna)
- Cosmetic deformity (altered ear contour)
E. MASTOID CAVITY OBLITERATION
(Scott-Brown Vol 3, Ch 233; Cummings 7th Ed, p. 2060–2065; Recent Advances)
Definition: Surgical filling of the mastoid cavity with biological or synthetic material to reduce cavity volume, promote epithelialization, and eliminate cavity problems.
Rationale:
- Reduces cavity size → smaller surface area to epithelialize
- Eliminates sump effect
- Reduces water intolerance
- Improves quality of life
OBLITERATION MATERIALS
MASTOID OBLITERATION MATERIALS
│
├── AUTOLOGOUS (Gold Standard)
│ ├── Abdominal fat (most widely used)
│ ├── Temporalis muscle/fascia flap (Palva flap)
│ ├── Bone pâté (mastoid cortical bone dust)
│ └── Cartilage grafts (tragus/conchal cartilage)
│
├── ALLOGRAFTS
│ ├── Irradiated homologous cartilage
│ └── Processed bone allograft
│
└── ALLOPLASTIC / SYNTHETIC (Recent Advances)
├── Hydroxyapatite (HA) cement
├── Bioactive glass (BonAlive®) granules
├── Beta-tricalcium phosphate (β-TCP)
├── Silicone blocks
└── Oxidized cellulose (Surgicel)
PALVA FLAP (Most Important — RGUHS Frequently Asked)
Origin: Described by Timo Palva (1973)
Composition: Postauricular musculoperiosteal flap
Technique:
1. Postauricular incision — create flap based superiorly/anteriorly
2. Flap contains: skin, subcutaneous tissue, periosteum, temporalis muscle fibers
3. Rotate flap into mastoid cavity
4. Obliterates posterior part of cavity
5. Combine with meatoplasty for optimal results
Advantages:
- Autologous — no rejection
- Well-vascularized → resists infection
- Reduces cavity volume by 60–70%
Disadvantage: Bulky in large mastoids; donor site morbidity
BIOACTIVE GLASS OBLITERATION (Recent Advances)
(Recent literature — PMC Clinical VQA; Poe et al.)
Bioactive glass (BonAlive®, Turku, Finland) is a synthetic silicate-based material that:
- Bonds to bone through a calcium phosphate layer
- Has intrinsic antimicrobial properties
- Supports bone regeneration
- Can reconstruct the posterior canal wall over time
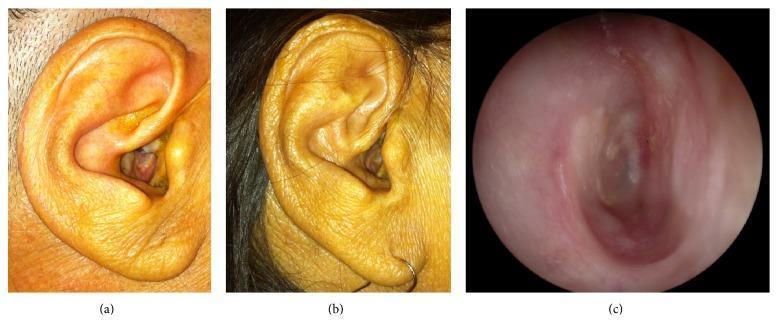
CWD vs. CWU: COMPARATIVE OVERVIEW
| Parameter | Canal Wall Down (CWD) | Canal Wall Up (CWU) |
|---|---|---|
| Cavity created | Yes | No |
| Recurrence rate | Lower (2–17%) | Higher (10–30%) |
| Water tolerance | Poor | Good |
| Follow-up | Lifelong | Can discharge after 2 years |
| Hearing | Poor (CHL) | Better preserved |
| Second look | Usually not needed | Required at 12–18 months |
| Problem cavity | Yes (25–50%) | No |
F. MANAGEMENT ACCORDING TO SPECIFIC PROBLEMS
Problem 1: Recurrent Cholesteatoma
Recurrent Discharge Post-CWD
↓
HRCT + DWI MRI
↓
Cholesteatoma confirmed?
YES → Revision mastoidectomy
+ Complete exenteration
+ Meatoplasty
± Obliteration
Problem 2: High Facial Ridge (Sump Effect)
- Clinical sign: depression/pocket behind the facial ridge, pooling of secretions
- Management: Revision surgery — carefully lower the ridge to the level of the facial nerve using diamond burr under facial nerve monitoring
Problem 3: Inadequate Meatoplasty (Small Meatus)
- Management: Revision meatoplasty (Körner flap or conchomeatoplasty)
- Aim: meatus ≥ 12–14 mm diameter
Problem 4: Retained Air Cells
- HRCT-guided pre-operative planning
- Complete exenteration in revision surgery: all retrofacial, perilabyrinthine, mastoid tip cells
IX. DIAGRAM — MASTOID CAVITY AND ITS PROBLEMS
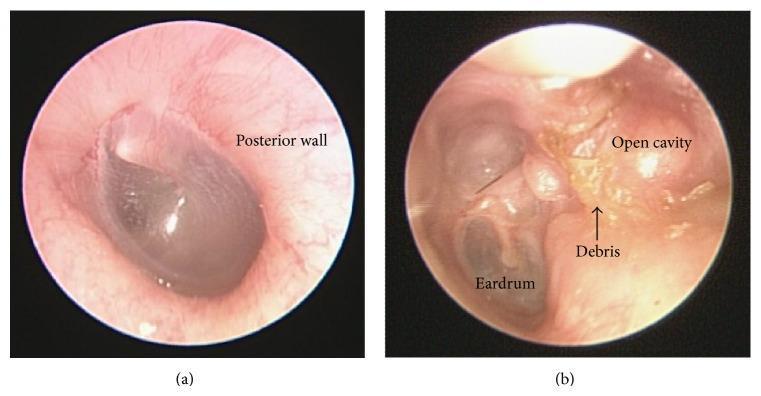
X. RECENT ADVANCES
(RGUHS Current Trend Questions — 2015–2024)
1. Non-Echo Planar DWI MRI (Non-EP DWI)
- Replaces second-look surgery in many centres
- Detects residual/recurrent cholesteatoma ≥ 3 mm
- Sensitivity: 95%, Specificity: 90% (Dubrulle et al., 2006; Khemani et al., 2011)
- Avoids radiation of CT in follow-up
- RGUHS tip: PROPELLER/HASTE DWI sequences preferred
2. Endoscopic Ear Surgery (EES)
- 0°, 30°, 45°, 70° rigid endoscopes
- Allows inspection of recesses (sinus tympani, facial recess) inaccessible to microscope
- "Endoscope-assisted" or "fully endoscopic" CWD revision
- Reduces recurrence by improving visualization (Marchioni et al., 2015)
3. Bioactive Glass (BonAlive®) Obliteration
- Superior to fat obliteration in large cavities
- Promotes osteogenesis and EAC reconstruction
- 5-year results: 85% dry ear rate (Silvola et al., 2012)
4. Canal Wall Reconstruction (CWR)
- Rebuilding the posterior canal wall after CWD mastoidectomy
- Materials: titanium mesh, Medpor (porous polyethylene), cartilage, bone pâté
- Converts CWD cavity to near-CWU anatomy
- Eliminates cavity problems while preserving disease clearance advantage
- (Dornhoffer 2003; Schraff & Dornhoffer 2007)
5. Hydroxyapatite Cement Obliteration
- Provides rigid structural support
- Radiolucent on DWI MRI — does not mask recurrent cholesteatoma
- Setting time: 4–8 minutes intraoperatively
6. Image-Guided Surgery (IGS / Navigation)
- CT-based intraoperative navigation
- Reduces risk of injury to facial nerve, sigmoid sinus, dura during revision surgery
7. Mastoid Obliteration + Ossiculoplasty (Combined Approach)
- Simultaneous cavity obliteration + TORP/PORP placement
- Improves both cavity stability and hearing in one stage
XI. FLOWCHART — COMPREHENSIVE DECISION ALGORITHM
PATIENT WITH CWD MASTOIDECTOMY
│
SYMPTOMATIC?
/ \
NO YES
│ │
Routine Assess type
6-monthly of problem
microsuction │
┌────┼────┬─────────┬──────────┐
│ │ │ │ │
Dis- Kera- Reci- Meatal Vertigo/
charge tin/ diva steno- Caloric
debris tion sis effects
│ │ │ │
Topical Micro- HRCT+ Meatoplasty
abx suction MRI DWI revision
drops (regular) │
│ │
Cholest. Retained
present? cells?
│ │
YES YES
│ │
Second look/ Revision +
Revision Exenteration
mastoidectomy │
│ └──────┐
└────────┐ │
▼ ▼
CAVITY OBLITERATION?
│
┌────────────────┼────────────────┐
│ │ │
Small cavity Medium cavity Large cavity
(< 5 cc) (5–15 cc) (> 15 cc)
│ │ │
Conservative Bone pâté/ Palva flap +
+ meatoplasty Cartilage + Fat/Bioactive
Meatoplasty glass +
Meatoplasty
XII. SUMMARY TABLE — MASTOID CAVITY PROBLEMS AT A GLANCE
| Problem | Cause | Management |
|---|---|---|
| Chronic discharge | Retained cells, high ridge, small meatus | Topical abx, revision surgery |
| Keratin accumulation | Large cavity, poor epithelialization | Regular microsuction, obliteration |
| Recurrent cholesteatoma | Retained matrix, inadequate clearance | MRI DWI, revision mastoidectomy |
| Meatal stenosis | Inadequate meatoplasty, fibrosis | Revision meatoplasty |
| Granulations/polyps | Chronic infection, exposed bone | Silver nitrate cautery, surgical excision |
| High facial ridge | Technical error at primary surgery | Revision — lower facial ridge |
| Water intolerance | Open cavity | Ear protection, obliteration |
| Vertigo | Exposed lateral SCC | Cavity obliteration |
| Conductive hearing loss | Ossicular loss | Ossiculoplasty (TORP/PORP), BAHA |
XIII. EXAMINER'S TIPS FOR RGUHS 50-MARK ANSWER
- Define problem mastoid cavity clearly at the start
- Emphasize the 4 commandments of cavity revision (high facial ridge, meatoplasty, exenteration, obliteration)
- Draw a labeled diagram of CWD cavity showing: tegmen, sigmoid sinus, facial nerve/ridge, lateral SCC, EAC
- Draw a flowchart for management
- Mention Palva flap in detail — frequently asked in RGUHS theory
- Include recent advances: DWI MRI, endoscopic ear surgery, bioactive glass, canal wall reconstruction
- Compare CWD vs. CWU in a table
- Mention organisms (Pseudomonas, MRSA, Aspergillus) and appropriate topical therapy
XIV. REFERENCES
- Scott-Brown's Otolaryngology, Head and Neck Surgery, 8th Ed. Michael Gleeson et al. — Vol. 3, Chapters on Mastoid Surgery and Reconstruction
- Cummings Otolaryngology Head and Neck Surgery, 7th Ed. Flint, Haughey et al. — Chapter 139: Mastoidectomy; Chapter 140: Complications
- Stell & Maran's Head and Neck Surgery, 4th Ed. — Otological Surgery section
- Zakir Hussain Otolaryngology — Mastoid surgery, chronic ear disease
- Dhingra's Diseases of Ear, Nose and Throat & Head and Neck Surgery, 7th Ed. P.L. Dhingra, Shruti Dhingra — Chapter on CSOM and surgical management
- Hazarika's Textbook of ENT & Head Neck Surgery, 4th Ed. P. Hazarika — Mastoidectomy and complications
- Dubrulle et al. (2006) — Non-EP DWI MRI for cholesteatoma detection. Radiology
- Marchioni et al. (2015) — Endoscopic ear surgery in cholesteatoma. Otolaryngol Clin N Am
- Silvola et al. (2012) — Bioactive glass obliteration outcomes. Otol Neurotol
- Dornhoffer JL (2003) — Canal wall reconstruction. Laryngoscope
Word of advice for RGUHS exams: This topic is frequently paired with "describe the surgical steps of CWD mastoidectomy" or "describe meatoplasty." Know the Palva flap technique, the 4 commandments of revision, and the DWI MRI for cholesteatoma detection — these are reliable scoring points in both theory and viva.
This is a shared conversation. Sign in to Orris to start your own chat.