I have the retrieved content and will now synthesize a comprehensive answer from both retrieved sources and my own knowledge.
Abdominal Wall Conditions: Treatment Overview
1. Inguinal Hernia
Types
| Type | Description |
|---|
| Direct | Passes through Hesselbach's triangle (medial to inferior epigastric vessels); acquired, due to weakness of the posterior wall |
| Indirect | Passes through the internal inguinal ring alongside the spermatic cord; congenital patent processus vaginalis |
| Femoral | Below the inguinal ligament; higher risk of strangulation |
Conservative Management
- Asymptomatic direct hernias in elderly or high-risk patients: watchful waiting is acceptable (Bailey & Love, p. 1089)
- Surgical trusses are not recommended
- Patient should be counselled to seek early review if hernia enlarges or becomes symptomatic
Surgical Management (Elective)
Surgery can be performed under local, regional, or general anaesthesia with minimal risk even in high-risk patients (Bailey & Love, p. 1089).
Open Repair
| Technique | Description |
|---|
| Lichtenstein (tension-free mesh) | Gold standard for open repair; polypropylene mesh reinforces posterior inguinal canal wall; low recurrence (~1%) |
| Shouldice repair | 4-layer running suture repair; preferred in some centres without mesh; recurrence ~1–2% in expert hands |
| Bassini / Darn repair | Older sutured repairs; higher recurrence rates; largely superseded |
Laparoscopic Repair
| Technique | Full Name | Approach |
|---|
| TEP | Totally Extraperitoneal | Mesh placed in preperitoneal space without entering peritoneum |
| TAPP | Transabdominal Preperitoneal | Peritoneum entered; mesh placed preperitoneally |
Advantages of laparoscopic: faster return to work, less post-op pain, better for bilateral or recurrent hernias.
Disadvantage: longer learning curve; general anaesthesia usually required.
Indications for Emergency Surgery
- Incarcerated hernia (irreducible, obstructed) → urgent reduction or surgery
- Strangulated hernia (ischaemic bowel) → emergency surgery; bowel resection may be needed
Complications of Repair
- Haematoma/seroma
- Wound infection
- Chronic groin pain (ilioinguinal nerve injury)
- Mesh infection/migration
- Recurrence (1–3%)
- Ischaemic orchitis / testicular atrophy (rare)
2. Umbilical Hernia
Pathophysiology
Defect in the linea alba at the umbilicus. In children, usually congenital (failure of umbilical ring closure). In adults, acquired — associated with obesity, pregnancy, ascites, and multiparity.
Paediatric Umbilical Hernia
- Most close spontaneously by age 2–4 years
- Surgical repair indicated if:
- Persists beyond age 4–5
- Defect >1.5–2 cm
- Symptomatic or incarcerated
Adult Umbilical Hernia
- Generally repaired electively due to risk of incarceration (bowel or omentum)
- Small defects (<1 cm): primary suture repair (Mayo's "vest-over-pants" technique)
- Larger defects (>1–2 cm): mesh repair (open or laparoscopic) — lower recurrence rates
Special Circumstances (Bailey & Love, p. 1094)
- Pregnancy-related: often develop postpartum; strong recommendation to avoid surgery during/before pregnancy unless complicated
- Patients advised: weight loss, abdominal muscle exercises; may resolve spontaneously within months
- Rectus divarication (diastasis recti) often co-exists and should be addressed
Complications of Repair
- Recurrence (higher with suture-only repairs in large defects)
- Wound infection
- Mesh-related complications (chronic pain, erosion)
3. Gastroschisis
Definition
A full-thickness abdominal wall defect, almost always to the right of the umbilicus, through which bowel (and sometimes other viscera) herniates — without a peritoneal sac.
Key Distinguishing Features
| Feature | Gastroschisis |
|---|
| Sac | Absent |
| Location | Right paraumbilical |
| Associated anomalies | Rare (mostly intestinal — atresia ~10–15%) |
| Bowel appearance | Thickened, matted, "peel" due to chemical peritonitis from amniotic fluid exposure |
| Maternal associations | Young mothers, low socioeconomic status |
Prenatal Management
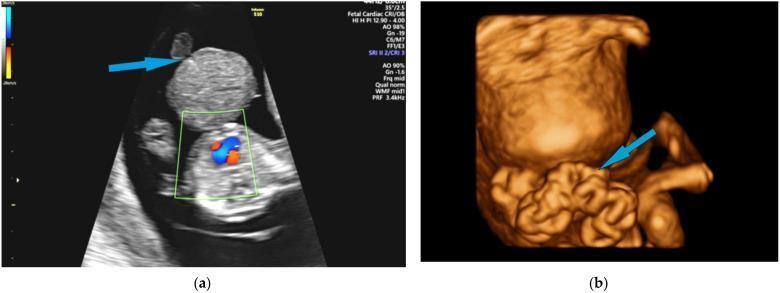
- Diagnosed on antenatal ultrasound (typically 18–20 weeks)
- Serial ultrasound to monitor bowel and fetal growth
- Delivery at a tertiary centre with neonatal surgical facilities
- Timing: typically 37–38 weeks (or earlier if bowel compromise); caesarean section not mandatory
Postnatal Immediate Care
- Wrap exposed bowel in warm saline-soaked gauze then cling wrap/bowel bag to prevent heat and fluid loss
- Nasogastric decompression
- IV fluid resuscitation (significant third-space losses)
- IV antibiotics (broad-spectrum)
- Keep neonate warm; nurse on side to prevent mesenteric tension
Surgical Repair
Primary (Immediate) Closure
- If the abdominal cavity can accommodate bowel without raising intra-abdominal pressure (IAP)
- Performed in the NICU or OR
- Sutureless/umbilical cord closure techniques increasingly used
Staged Closure with Silo
- Used when primary closure would cause abdominal compartment syndrome (IAP >20 mmHg)
- Spring-loaded silo placed at bedside in NICU without anaesthesia
- Bowel gradually reduced over 5–10 days by gravity
- Formal fascia closure once bowel fully reduced
Postoperative Issues
- Prolonged ileus (weeks) — TPN required until gut function returns
- Risk of short bowel syndrome if intestinal atresia/ischaemia present
- Necrotising enterocolitis
4. Omphalocele (Exomphalos)
Definition
A midline abdominal wall defect at the umbilicus where abdominal contents herniate into the base of the umbilical cord and are covered by a sac (amnion + peritoneum).
Key Distinguishing Features
| Feature | Omphalocele |
|---|
| Sac | Present (amnion-peritoneal membrane) |
| Location | Central / umbilical |
| Contents | Bowel, liver (in large defects), stomach |
| Associated anomalies | Very common (50–70%) — cardiac, chromosomal (Trisomy 13, 18, Beckwith-Wiedemann syndrome) |
| Bowel appearance | Normal (protected by sac) |
Classification
| Type | Defect Size | Key Feature |
|---|
| Minor / Small | <5 cm | Bowel only; primary repair often possible |
| Major / Giant | >5 cm or contains liver | Complex staged repair needed |
Associated Syndromes
- Beckwith-Wiedemann Syndrome (macroglossia, gigantism, hypoglycaemia)
- Pentalogy of Cantrell (cardiac + diaphragmatic + sternal + pericardial defects + omphalocele)
- OEIS complex (Omphalocele, Exstrophy, Imperforate anus, Spinal defects)
- Chromosomal anomalies (Trisomy 13/18): thorough workup before surgery
Prenatal Management
- Antenatal diagnosis on ultrasound (often earlier than gastroschisis)
- Fetal echocardiography and chromosomal analysis (amniocentesis) essential
- Multidisciplinary counselling
Postnatal Immediate Care
- Do NOT rupture the sac — it protects the viscera
- Keep sac moist and protected
- IV access, nasogastric tube, IV fluids
- Thorough assessment for associated anomalies (echo, renal US, genetics)
- Treat hypoglycaemia (Beckwith-Wiedemann)
Surgical Repair
Small Omphalocele — Primary Repair
- Sac excised
- Viscera reduced and fascia primarily closed
- Performed once neonate is stabilised
Giant Omphalocele — Staged Approaches
| Approach | Description |
|---|
| Staged fascial/skin closure | Gradual stretching of abdominal wall over weeks |
| "Paint and wait" (conservative) | Apply escharotic agents (silver sulfadiazine, betadine) to sac → scar tissue granulates → delayed surgical repair months later |
| Tissue expanders | Slowly enlarge abdominal domain before definitive repair |
| Component separation | Releases oblique muscles to achieve tension-free midline closure |
Prognosis
- Gastroschisis: generally good survival (>90%) if no major atresia; bowel function recovery may take weeks
- Omphalocele: prognosis driven by associated anomalies — isolated omphalocele has good outcomes; Trisomy 13/18 carries poor prognosis
Quick Comparison: Gastroschisis vs. Omphalocele
| Feature | Gastroschisis | Omphalocele |
|---|
| Sac | Absent | Present |
| Location | Right of umbilicus | At umbilicus |
| Bowel appearance | Matted, thickened | Normal |
| Associated anomalies | Rare | Common (50–70%) |
| Chromosomal anomalies | Uncommon | Common (Trisomy 13, 18) |
| Maternal age | Young | Any |
| Immediate priority | Wrap bowel, fluid resus | Protect sac, assess anomalies |
| Repair strategy | Primary or silo | Primary or staged/"paint & wait" |
| Prognosis driver | Bowel viability | Associated anomalies |
Sources: Bailey and Love's Short Practice of Surgery, 28th Edition (pp. 1089, 1094); supplemented with standard pediatric and general surgery knowledge.