A 17 year old boy texted me these saying he got this skin lesion for the last 1 month.Went to a Medical complex received some antibiotics (augmintin) slightly recovered but no benefit.Then went to some another Doctor he asked to perform the LD antibodies test which came out to be -ve but the doctor denied and said repeat the test...can you tell me your diagnosis and explain that topic?
Reading File
Finding Sources
Searching PubMed
"cutaneous leishmaniasis" AND diagnosis
Searching Images
cutaneous leishmaniasis skin ulcer
Reading File
Reading File
Reading File
Loading Image
Reading File
Reading File
Loading Image
The textbook image from Fitzpatrick's (Old World CL, "moist type") is virtually identical to this patient's lesion. I now have everything needed for a comprehensive answer.
Diagnosis: Cutaneous Leishmaniasis (CL) — Old World type ("Oriental Sore" / "Lahore Sore" / "Kandahar Sore")
The clinical picture is highly characteristic. Compare this patient's lesion with the textbook image from Fitzpatrick's Dermatology below:
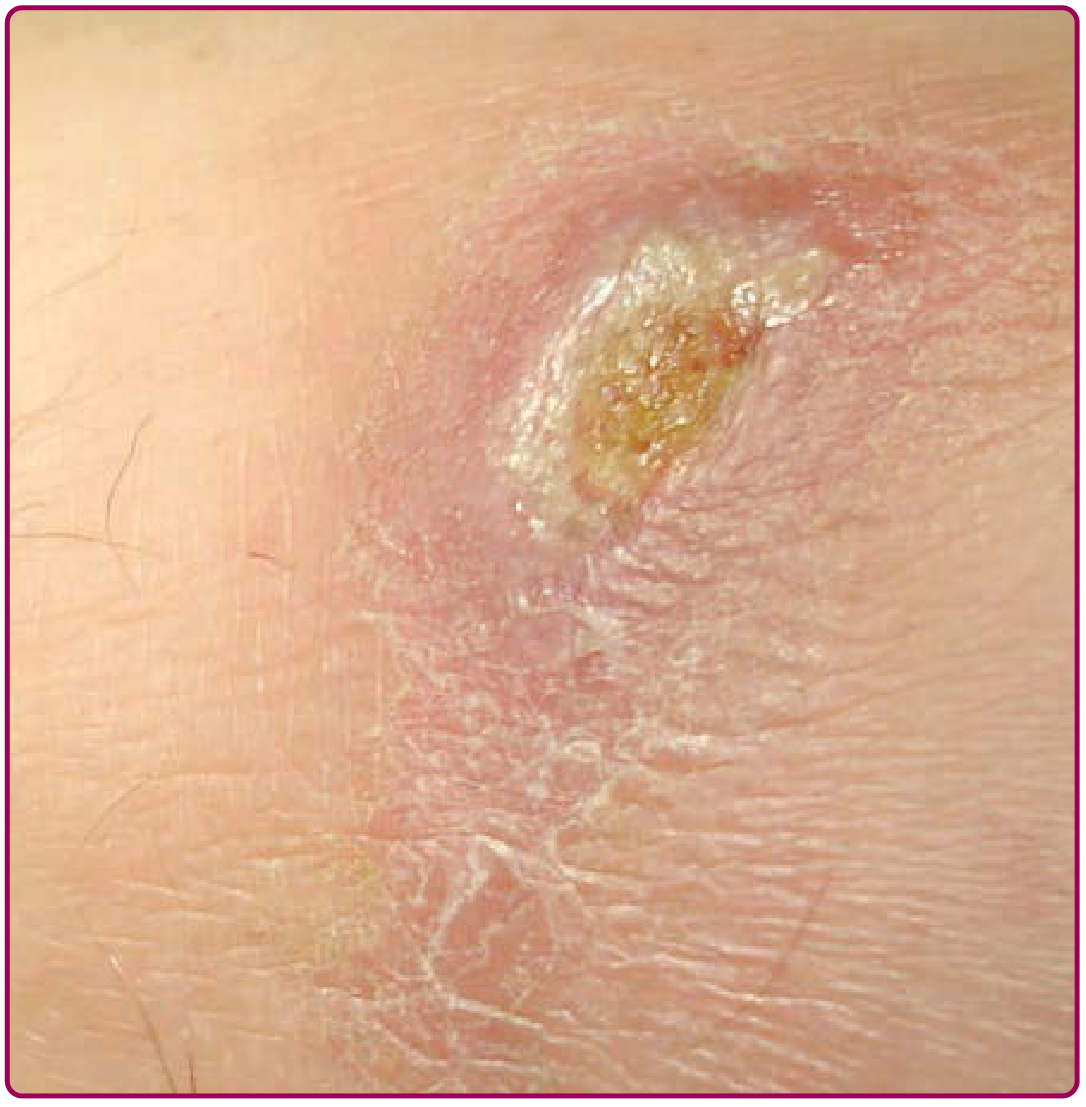
Patient's lesion:
(Provided in your images — single, well-defined ulcerative plaque on the dorsum of the wrist/hand with a granular red base, raised/rolled indurated border, and surrounding scale-crusting)
Textbook reference image (Fitzpatrick's — Old World LCL, moist type on the arm):
The two lesions are virtually identical.
Why This Diagnosis Fits
| Feature | This Patient | Classic CL |
|---|---|---|
| Age | 17-year-old male | Any age; common in children/young adults |
| Duration | ~1 month | Weeks to months |
| Location | Dorsum of hand/wrist (exposed area) | Exposed skin — face, hands, limbs |
| Morphology | Ulcer with granular red base, raised rolled border, crusting | "Volcanic" crateriform ulcer, rolled margin, necrotic/crusted base |
| No response to antibiotics | Augmentin gave no benefit | CL is parasitic — antibiotics are ineffective |
| Geography | Pakistan (the lab is from a KPK/Peshawar-region facility) | Pakistan is an endemic zone — "Lahore sore," "Kandahar sore" are historical names for CL in this exact region |
What is Cutaneous Leishmaniasis?
The Parasite
Leishmaniasis is caused by obligate intracellular protozoan parasites of the genus Leishmania. In Pakistan/Afghanistan/KPK, the main species are L. tropica (dry/urban type) and L. major (moist/rural type). The parasite is transmitted by the bite of a female sandfly (Phlebotomus species in the Old World).
Life Cycle
The sandfly injects promastigotes (flagellated form) into the skin → macrophages engulf them → promastigotes transform into amastigotes (non-flagellated, oval/round, ~2–4 µm) = LD bodies (Leishman-Donovan bodies) → multiply inside macrophages → rupture and infect more cells → trigger granulomatous skin reaction.
Clinical Progression
- Papule at bite site (days to weeks after bite)
- Enlarges → nodule
- Nodule ulcerates → classic "volcano" ulcer: painless, crateriform, with a raised/rolled indurated border and a crusted or granulating base
- Most Old World lesions heal spontaneously in 2–15 months, leaving a scar
About the LD Bodies Test and Why It Was Negative
The lab report shows: "Smear for LD Bodies — NO LD Bodies Seen"
The referring doctor was absolutely right to repeat the test. Here is why a negative result does NOT rule out leishmaniasis:
What the Test Is
A slit-skin smear (or aspirate from the active edge of the lesion) is stained with Giemsa and examined for amastigotes (LD bodies) inside macrophages. These appear as small oval structures with a nucleus and a rod-shaped kinetoplast ("double dot").
Why False Negatives Are Common
- Sensitivity of smear microscopy is only 20–60% in cutaneous leishmaniasis — significantly lower than in visceral leishmaniasis
- The number of parasites in the lesion is often low, especially in:
- Older, more chronic lesions (>3 weeks) — the immune response clears parasites from the periphery
- L. tropica infections (dry type) — fewer organisms than L. major
- Lesions that have started healing (even partially, as with this patient after some antibiotic use causing secondary infection treatment)
- The smear was taken from blood (the report says "Specimen: BLOOD") — this is incorrect for cutaneous leishmaniasis. The sample should be taken from the active raised border of the skin lesion by slit-skin smear or aspiration, NOT from peripheral blood. Peripheral blood smear has essentially zero yield for cutaneous leishmaniasis (LD bodies in blood are a feature of visceral leishmaniasis/kala-azar, not cutaneous)
This is the critical point: The test was performed on the wrong specimen. For cutaneous leishmaniasis, the smear must be from a scraping or slit of the lesion's indurated edge — not blood.
Recommended Diagnostic Approach
| Test | Notes |
|---|---|
| Slit-skin smear from lesion edge (Giemsa stain) | Gold standard; must be taken from the active border, not the necrotic center or blood |
| Skin biopsy (histopathology + Giemsa) | Higher sensitivity than smear; shows granulomatous infiltrate + amastigotes |
| PCR (from biopsy or swab) | Most sensitive (~95%); identifies species — important for treatment decisions |
| Culture (NNN medium) | Grows promastigotes; confirms diagnosis but takes weeks |
| Montenegro skin test (Leishmanin test) | Positive in >90% of CL; indicates delayed hypersensitivity; remains positive for life |
| Serology (anti-Leishmania antibodies) | Low sensitivity in CL (better in visceral form); not reliable for cutaneous disease |
Treatment
Per Harrison's Principles of Internal Medicine (22nd ed.) and Fitzpatrick's Dermatology:
- Pentavalent antimonials (Sodium stibogluconate / Meglumine antimoniate) — first-line drug: 20 mg/kg/day IM or IV for 20 days
- Miltefosine (oral): 2.5 mg/kg/day for 28 days — increasingly preferred; effective against L. major
- Intralesional antimonials: For small single lesions
- Fluconazole (oral): 200 mg/day × 6 weeks — shown to achieve 79% cure in L. major (vs. 34% placebo)
- Topical paromomycin: For small, uncomplicated lesions
- Systemic treatment is required for: lesions on face/hands/joints, large ulcers, multiple lesions, lymphatic spread, or immunocompromised patients
⚠️ Augmentin (amoxicillin-clavulanate) has no activity against Leishmania. Any apparent improvement was likely due to treating secondary bacterial superinfection of the ulcer, not the underlying cause.
Summary for the Attending Doctor
This 17-year-old from an endemic region (KPK/Pakistan) with a 1-month painless ulcerative skin lesion on an exposed area, non-responsive to antibiotics, has a clinical presentation essentially pathognomonic for Old World Cutaneous Leishmaniasis (L. tropica or L. major).
The negative LD body smear should be disregarded as it was performed on peripheral blood (wrong specimen). A slit-skin smear from the lesion's active border or skin biopsy should be performed. PCR is the most sensitive confirmatory test if available. Treatment with pentavalent antimonials or oral miltefosine should be initiated.
Sources: Fitzpatrick's Dermatology (9th ed.), Vol. 1–2, p. 3258; Harrison's Principles of Internal Medicine (22nd ed., 2025), p. 1830; Andrews' Diseases of the Skin (Clinical Dermatology), p. 493
Yes and the kid also says i was bitten by something a mosquito or something else which was itching so after rubbing it repeatedly it transformed into this.
This actually strongly reinforces the diagnosis of Cutaneous Leishmaniasis. Here is why:
The "Insect Bite" History is Classic for CL
The boy is absolutely correct — it was an insect bite. Just not a mosquito.
The Culprit: The Sandfly (Phlebotomus species)
| Feature | Details |
|---|---|
| Appearance | Tiny (1–3 mm), yellowish, hairy — easily mistaken for a mosquito or gnat |
| Bite sensation | Causes an intensely itchy papule — the itch is often more severe than a mosquito bite |
| Time of activity | Dusk to dawn, like mosquitoes — often not noticed |
| Common in KPK/Pakistan | Phlebotomus sergenti (vector for L. tropica) and P. papatasi (vector for L. major) are highly prevalent in this region |
The Exact Sequence of Events in CL
Sandfly bite (itchy papule)
↓
Child rubs/scratches repeatedly ← THIS IS WHAT THE BOY DESCRIBED
↓
Inoculated promastigotes taken up by skin macrophages
↓
Transforms into amastigotes (LD bodies) → multiply
↓
Papule → Nodule → Ulcer (over weeks to months)
The rubbing/scratching did not cause the lesion — the sandfly's saliva had already injected Leishmania promastigotes into the dermis at the moment of the bite. The scratching merely:
- Spread the inoculum slightly in the skin
- Traumatized the initial papule, potentially accelerating ulceration
- Introduced secondary bacteria (which is why Augmentin had some partial effect — it treated the secondary bacterial infection on top of the Leishmania ulcer, not the parasite itself)
Why the Initial Bite Was "Itchy"
When the sandfly feeds, it injects saliva containing vasodilators and immunomodulatory molecules that:
- Cause local histamine-mediated itch (hence the intense itching)
- Simultaneously suppress the local immune response — this is what helps Leishmania promastigotes survive and establish infection
This is why children in endemic areas often present saying "I was bitten by something that itched a lot, and then it became a sore."
Bottom Line
The history of "bitten by an insect → intense itch → rubbed repeatedly → slowly turned into a non-healing sore" is the textbook presentation of cutaneous leishmaniasis in Pakistan/KPK. It is so characteristic that in endemic regions, this history alone — combined with the visual appearance of the lesion — is considered sufficient grounds to start treatment while confirmatory tests are arranged.
The next step remains the same:
- Slit-skin smear from the lesion's active raised border (NOT blood)
- Refer to a dermatologist or infectious disease specialist with experience in leishmaniasis
- Treatment with sodium stibogluconate (pentavalent antimonial) or oral miltefosine as prescribed by the treating physician
This is a shared conversation. Sign in to Orris to start your own chat.